What’s Up With Kevin is a “hidden” page I started on this blog in August of 2011 when Kevin was diagnosed with Autoimmune Hepatitis (AIH). (Simply put: his immune system is attacking his liver and causing inflammation. Hepatitis means inflammation of the liver.) He has had rough Freshmen years. He missed the entire first six weeks of his Freshman year in high school recovering from the emergency surgery that led to the AIH diagnosis.
He had to unenroll February 2016 and miss the rest of his second semester of his Freshman year at Crown College in Powell, Tennessee, near Knoxville, because of health complications stemming from AIH. That semester he was diagnosed with a bile duct disease called Primary Sclerosing Cholangitis. “Primary sclerosing (skluh-ROHS-ing) cholangitis (koh-lan-JIE-tis) is a disease of the bile ducts, which carry the digestive liquid bile from your liver to your small intestine. In primary sclerosing cholangitis, inflammation causes scars within the bile ducts. These scars make the ducts hard and narrow and gradually cause serious liver damage. In most people with primary sclerosing cholangitis, the disease progresses slowly and can lead to liver failure, repeated infections, and tumors of the bile duct or liver. Liver transplant is the only known cure for primary sclerosing cholangitis.” (I Googled it and pasted the least wordy definition this one from the MayoClinic page.)
He began the process we thought would be further down the road: He was listed and waited for a liver transplant from August of 2016 to September of 2017. He was listed for transplant in August of 2016 in Houston. He started the process of being dual listed at Ochsner Medical Center in New Orleans in May 2017. Kevin was evaluated there July 6-7, 2017, in New Orleans, Louisiana, and officially dual listed July 12, 2017!
He was transplanted Wednesday, September 6, 2017, at Ochsner Medical Center, New Orleans!
Kevin “desires” to return to and continue his Pastoral Studies degree. (See helicopter doctor post below) He was able to take online classes through Crown during the Spring semester of 2017. It was a wonderful thing to see him listening to lectures online and reading and studying. Even sometimes on his worst days I saw him completing homework and reading assignments. We continue to praise Him that he found favor with the transplant team and was given an offer for a liver. This was a difficult thing to pray for because we knew a donor must lose their life to save Kevin’s. We trust Him because only He can orchestrate something this beautiful. We prayed faithfully that he would find favor with the transplant team and be given an offer in His time with His perfect will. I am so thankful for all who prayed with me that Kevin would continue to be strengthened, settled, and established through this entire process and healed in His time! We will give Him glory and praise, “For ye are our glory and joy.” 1 Thessalonians 2:20
As I update this paragraph he is packing to return to Crown! He is enrolled for the Fall semester of 2018 and will be studying pastoral ministries. My prayer for Kevin as he returns is from 2 Chronicles 16:9 that He would find Kevin strong and worthy to be used of Him. And that Kevin would be diligent in his study and walk with the Lord and day to day life, and that his testimony would stay above reproach. From Ps. 1:2 I ask that Kevin would delight in His law as he meditates day and night in it. I ask from Daniel 9:22 that He would give Kevin skill and understanding in each of his classes. From Lev. 8:11-12; 30 and Jeremiah 1:5 I am praying that Kevin would be sanctified — set apart for His service. I also beg Him for protection for Kevin as he drives on those winding and narrow Tennessee roads from his dorm to the school.
So, if you have found your way to this page then you must really care for my son Kevin. I wanted to leave the paragraphs above as a way to explain what is going on specifically. All the stuff below this is the somewhat detailed daily and or weekly updates I post when I have time. It is our medical memory if you will. (It has been a great tool especially keeping up with tests, labs, medicine dosages, and procedures!)

Tuesday March 31, 2020 Zoom Chat with Dr. Galati and Katie
Discussed changing our background from our kitchen to someplace fabulous (lol) then labs from Friday at Quest in the Woodlands at Methodist. Sounded like most of them were trending down.
Alk Phos 193 down from 220
BILI 1.2 was 1.1 (he’s not going to have a fit about that)
AST 26 down from 95
ALT 112 down from 256
He recommended to possibly not do the summer camp thing Kevin was applying to do at Lake Texoma and honestly who even knows what the next step is other than dinner tonight. After next labs and zoom chat possible 2 weeks then longer between labs.
He was messaging Dr. Nguyen on how long for the stent to stay placed. Dr. Galati texted this to Kevin after the call ended:
Update, he placed a metal stent, rather than the typical plastic stent, these are more durable and have a longer lifespan so six months seems correct.
Labs on Monday then another follow up Zoom chat later that week.
3/20/20 Kirby ER to 1009 Dunn Tower Houston Methodist Hospital
8:30 am after emailing some one on Kevin’s team late last night these symptoms we went ahead and called Dr. Galati’s office once they opened. Symptoms: yellow eyes in the corners (Caleigh noticed yesterday when they tried to swim) pale colored stool, itchy abdomen. I call it three strikes you’re in.
9:30 am Anthony the NP called us on a conference consult. He asked all the questions. He definitely wants labs but said hold off until he hears from Dr. Galati.
10:00 am ish heard back from Anthony that Dr. Galati wants him to go to the Kirby ER.
All the while copying and keeping his new coordinator in the loop Tasha Murray
Noon: Made it to Kirby ER. They masked Kev up. They didn’t mask me. I’m just a mom. Hoping to get checked and outta here ….

12:20 ER Doctor just did his quick check. He said his eyes look a little jaundiced. Gonna run some tests and call the liver people.
1:30 The ER nurse gave us a quick update. His liver enzymes are elevated. Last labs they see are Jan. I have March 3 ones. (Both were very normal ranges)
BILI was .4 now 5.5
AST was 19 now 134
ALT was 21 now 164
Waiting for the doctor to come back in.
1:50 The ER doctor just came in. He talked to Galati. They are trying to get him admitted to Methodist to see what is going on.
2:45 The ambulance team arrived to take Kevin to HMH. I went ahead and drove my car so it would be at the hospital.
3:00 Its 1009 west Dunn tower. I walked in lobby by where we normally pay for valet and there is a queue. A lady in a helmet mask takes your temp then you step over and get asked the routine questions. They gave me a wrist band and I was good. We are waiting on the PCA to get vitals. Met his nurse Esther.
4:00 nurse Esther and PCA Evelyn checking him all in.
6:00 they took him for an ultrasound
He did get to eat! Ordered himself a heart healthy meal.
7:00 shift change. Nurse is now Diane and PCA is Pacina. They gave all his meds.
Kevin worked on course work most of the night. Pretty uneventful information wise. We did get a pretty happening FaceTime call from Bailey. She showed us her new motorcycle trick. And sang like aerial. And told us how mean Ursula was taking the little mermaids voice.
3/21/20 Saturday
9:45 He woke up with a migraine. Bummer. The normal migraine medication isn’t in the system. So they can’t give it to him. So we are waiting on the team to round. Earlier the night shift nurse called the doctor. The doctor said we will take care of that when we round. 😭😠😳🤯😱
My frustration with the hospital continues. Love. Hate.
He’s had the headache since early hours of the morning. Night shift is who called. Am shift said she will see what time they might round. 😶
My big brother Steve sends me really encouraging scripture filled texts every day. Just got this one and I cut out most of it but the ending prayer is exactly what I needed:
“Happy Happy Saturday Beth
Good morning Father, thank you for this NEW DAY as we rise please let us be filled with Your spirit. Wherever we go, let us spread love, joy, peace, goodness, and faithfulness.
– Trials Are Part Of Our Development…
In a way, this is what James is describing in James 1:2-4, “Consider it pure joy, my brothers and sisters, whenever you face trials of many kinds, because you know that the testing of your faith produces perseverance. Let perseverance finish its work so that you may be mature and complete, not lacking anything.”
Dear Lord, You are always giving us the opportunity to face challenges that improve our skills to serve you. Help us see these challenges as the learning and development that they are, and not irritants for us to complain about.
Be good to yourself today Beth”
9:50 I’m listing out the times to keep myself straight. But also it’s such a blessing because before I could finish updating my brother’s prayer a friend texted and said remind them every twenty minutes. I was about to step out to start that “reminding” when Sarah today’s nurse walked in with a paper asking for the specific medications and dosages. Megan who is the NP for the liver team is on for this weekend and our nurse contacted her. Such a praise!
10:30 The nurse gave Fioricet for headache! Did blood cultures. And read us the following labs:
Yesterday’s then today’s
ALT 161 to 193
AST 134 to 154
Total Bili 5.5 to 6.2
Still waiting on Megan who is the NP for the liver team to round.
11:00 Kevin did this update on what the liver team NP said:
Ok. The NP just came in with a rough plan.
Wait on the cultures to see what they say.
Talk to the GI doctor most likely do an ERCP (just another scope to check out the bile ducts)
Depending on all those results maybe do a biopsy of the liver to see if there’s any rejection
Back to me. When she said ERCP we said we were familiar. And mentioned Dr. Dang Nguyen and when she mentioned who was on the floor today for the liver team she said Dr. Saharia and we were happy again because we know him too! And better yet. They KNOW Kevin! She said the ultrasound looked fine. The plan is if the ERCP can be done this weekend they will order it. If not it will be Monday.
So they are looking at several possibilities: blockage, rejection, or recent medication. (Ruling our medication maybe because he’s had good labs since the February pneumonia)
12:00 We finally got to meet Christina who is with Dr. Galati’s Liver Specialist of Texas private practice. She has talked to us over the phone and got Kevin through one of the TN ER trips. She said she spoke with Dr. Galati this morning (my Stitch “bad tank” just went to straight happy! I told Kevin while I’m not mad I’m just wanting people to know we are here. Well. I know they know we are here but I’m experiencing a sense of urgency and it seems like this place is on Saturday slow mode. But now I’m Happy!) [also just coming off Disney world so hence the Stitch reference]
•she said they would like to do the less invasive MRCP imaging today (non fasting)
•they will speak with Dr. Nguyen (ERCP) to see if he agrees
•she said this could be sludge or stones that have built up because liver transplant patients do not have a gall bladder.
She explained it like this. With his Alk Phos (247 yesterday to 261 today) and and liver enzymes elevated she said that equals or points to his bile ducts. Which now that he’s jaundiced even more points to bile ducts. And with no gall bladder your body still can make stones. So an MRCP would show that image. And ERCP will actually be done to go in and clean out the sludge and stones and place a stent. If needed.
12:30 the PCA came in and said they are now monitoring his blood sugar.
2:00 Dr. Rajjman from the gastroenterologist team with Dr. Dang Nguyen stopped in. He told us Dr. Nguyen was his fellow. He said he is the old guy. I’m like. We will take the old guy. Most likely ERCP tomorrow…based on MRI/MRCP findings. He also said alot of other stuff and when I tried to take notes he wouldn’t let me because he said he didn’t want me googling it!
After he left the nurse was in drawing more labs. And Kevin’s phone rang. It was Hoy the NP from the diabetes team. They are giving him a huge dose of steroids and will monitor his blood sugar. Based on his numbers he may it may not need insulin. She said exposure to long term steroid can cause diabetes. They will be checking his levels 4 times a day.
5:00 He’s not eating before his MRCP scheduled for later tonight.
7:25 They took him for his MRI/MRCP
3/22/20 Sunday
8:00 the nurse doesn’t see Kevin on the schedule. She will confirm with his team if the procedure is today. She will get back with us in an hour. She wants him to eat if he isn’t having it.
There was a bit of confusion and miscommunication this morning. We honestly do not know how they keep it all straight, but are very thankful that no matter what, all the teams are doing what they think is best for Kevin. For now, today looks like it went from fasting and a procedure to being able to eat and the procedure will be tomorrow. So, he will be NPO after midnight tonight.
Kevin and I enjoyed listening to services today on line! Also this computer will not connect to the internet…I asked the nurses. They said the service here can be wonky.
3/23/2020 Monday
8:30 they came and got Kevin for the ERCP. Once in Jones Tower they prepped him. He signed consents. They had to do a new IV. The other was in his arm from ER. The anesthesiologist prefers a different placement for this procedure. Everyone always comments what a tough guy Kev is.
9:35 They took him back to start the ERCP procedure.
10:15 Met w Dr. Nguyen who gave me the best news! Kevin did great and he was able to place a stent. He said this was very common. He said Kevin looked great! Hadn’t seen him in almost three years. He showed me the print out. (He always shows me this either bedside or waiting room side. Kevin told me yesterday I could stay in the room and didn’t have to go to this procedure. I was like…NO. I mean an xray or ultrasound sure. Go on and have fun. I will stay behind. But for a Dr. Dang Nguyen ERCP…he always gives a quick talk. He’s the best! Kevin is out during this too so what does he even know) And he showed me on the print out exactly where the old duct was connected to the new duct where the narrowing was and where he placed a stent. Very flexible covered stent… He explained that this will stay in place for 6 months and 85% of cases will not need another procedure once the stent is removed. There is a risk that it migrates or forms stones or even food can get in there…but between now and then if jaundice or fever that would be the sign to check back in. The doctor said he really needed this procedure and that the MRCP really showed that stricture.
10:30 pain med. Kev is very uncomfortable in recovery. gave second dose a bit later
10:52 gave delodid for pain. He was at a 7 before. Then it stayed same after two doses.
12:25 nurses on floor gave tramadol. He’s still at a7 We are back on the floor. yikes
1:30 Xray came to the room. He’s been resting before and after finally. This did turn out fine. All looked good placement wise and all according to this.
Pain still same at 1:50. Next available is at 6:20 😱
4:55 thankfully they were able to bring another type of pain relief for Kevin before 6:20. Someone’s praying. Poor guy. His pain level has been at a 7 basically all day.
7:00 This has been a rough day. All I can say is people started out the day saying what a tough kid Kev is and I’m echoing it as his mom hours later saying I don’t know how he stands it. I know it will only get better with time and rest but goodness…this one was tough. I told friends that I did keep my mouth closed but in the recovery after loads and loads of IV pain med was given I was ready to ask what is wrong with his IV and where do you think all that med is going cause he isn’t feeling it so it must be just connected wrong. Glad I didn’t say anything but goodness…poor Kev. I treated myself for suffering so by ordering my first uber eats to the front of the hospital from Zoe’s kitchen. Kevin hates hummus and cauliflower rice and since I’d consumed that last of the snacks in my back pack from Disney I had for line distractions for the girls…I needed real food. Now had I ordered Papasitos Fajitas that would just be mean…
3/24/2020 Tuesday
He is still in some pain. All day yesterday he was at a 7 even though the faces I saw I would put it as a 10. But today he’s a 6 to 5. So we will take it.
8:30 Dr. Dang Nguyen was in. He talked to us for a while. He performed the procedure yesterday. He explained that in young patients it is more painful. He said even during the procedure when he’s opening the duct and stretching it they jump or move at that time. So he said it is like a stretching that eventually he will get use to. He said again how good it was to see Kevin doing so well. He told us a story of his youngest patient getting transplanted at 17 and is now graduating from college and somewhere in there he mentioned he’s been seeing him since he was little. He treats him for colitis. We threw in that Kevin has been recently diagnosed with that! He said normally in patients with PSC colitis goes hand in hand. Usually it’s found before PSC. I told him Dr. Galati said the exact same thing! We told him the Med they started Kevin on and how long he dealt with “stomach issues” and he said it’s normal. It takes a while to determine and that medication is the first level. He also put his hand out and was like he may know 5 people ever that are this young that has the things Kevin is dealing with. He also commented on how good Kevin’s labs look. He said normally after a procedure they bump up from the contrast in there. So. He’s happy with Kevin’s outcome. Wants him to move to a Full liquid to soft diet.
9:45 Pain level is at a 2! The soft breakfast arrived
Between 10 and 11:30 the transplant team and the galati team came by. We didn’t know either of the transplant team members but it was good to meet them since they all help make decisions on Kevin. They did switch him to cellcept from zortress out of an abundance of caution temporarily because a procedure was done. Just like they did when he had his appendectomy. (As I am typing this the pharmacy hopped in with a refill of it from walgreens! They said it was a zero copay and knew we were concerned about our mail order for the antirejection meds getting him some for when he is discharged…so that’s taken care of! And he gets a break from peeling his zortress every day twice a day and Keith says he gets a break from picking up all those peelings! Lol
They ordered a few more blood tests to rule out any causes for pain other than procedure. Christiana from Galati’s team gave us good information too. She said the xray showed no perforation or puncture and that the stent was in place. His alk Phos and Bili are down but the AST and the ALT are still up. She said this could be normal after a procedure with the liver…
Overall they agreed to do what Kevin felt best on discharging today or tomorrow. Since he is still in pain, it is lower and since they want to see those other liver numbers once more it looks like discharge day is tomorrow. Pending any sudden changes.
3/25/20 Wednesday
Asking myself now why did I write: pending any sudden changes? Last night starting around 10 pm Kevin started hurting. He had just had his pain meds at 9 and just prior to this he had to ask for the other pain med to try to make it to the one that works and migraine med. He was in a heaping mess. Somewhere around 10 I stepped out to the nurse. She said let’s give it time. I stepped out again and she called Dr. Nguyen’s office. She said the lady doctor on call for that team said she didn’t know Kevin and that she wasn’t comfortable giving anything else. Meanwhile poor Kevin was hurting. I massaged and rubbed his head and back…prayed and read scripture aloud. All the while the nurse brought in a heating pad. Just crazy stuff here. I think the station called her back maybe she didn’t put in an order. She was struggling to put it together anyway. This is not your normal heating pad. It looks like it requires NASA astronaut training to even plug up! While she was gone doing all that Kevin wasn’t any better and his pain was to a 9. Worse than after the procedure. I’m thinking something else is going on!?!? No one is in the halls. Finally, our PCA stepped in the hall and I said can you please call the lady doctor back and make her call the doctor who knows Kevin! The nurse found us and she said she had a call into the transplant team. I said we just met them today and honestly, I don’t know them and they don’t know us. I asked her if they were young and new? None of it mattered because by 11:30 they approved a shot of delaudid (correct spelling. Finally looked it up. I’ve been spelling it dilodded…the dictionary doesn’t know either so who cares!) By 1 am he was waking me again to help with his head. At 3 the same. Finally, we must have both fallen back asleep. At one point I took a picture of the light above his door. It was red the entire time. Shows how much that system works. They were in and out helping but never touched that light box on the wall behind the door to change it. Good enough too cause it was a RED LIGHT NIGHT. Awful.
Our nurse was a trooper! I don’t want to slant in my observation of Kevin’s pain that she wasn’t doing anything. Once he finally settled and slept after the pain dose to the IV I was sitting in the chair and just couldn’t hold it in anymore. Watching Kevin silently and sometimes not so silently suffer and being able to do nothing just takes it out of you. I was silently crying and she came over and threw her gloves away and hugged me. I’m not even the one who needs the hug but I took it for Kevin…
It’s 8:30 now and who knows. He’s feeling a little better. Resting. Ordered breakfast cause they knock on that door to get that order not knowing how your night was.
8:45 Dr. Nguyen was in. We told him about the horrible night. He did say the transplant team always manages the pain meds. And he is starting him on an anti-spasmodic. He examined him and pressed around the abdomen. He said it’s soft and no way would Kevin allow or tolerate that pressing if there was something wrong. He said it does take time. I asked should we have stayed on a clear diet he said no…
9:00 He is still at a 5-6 and cannot have norco until noon. Nurse gave normal meds and tramadol because maybe it will help some.
9:50 Just gave him Bentyl (or dicyclomine) it’s the antispasmodic dr Nguyen ordered after seeing Kevin this morning and hearing about the bad painful night. The nurse said let her know if his pain worsens.
10:00 The endo np or doctor called kevin on his cell…social distancing at it’s best…she’s concerned about his levels. We talked through all that has happened and she said she would look at it again tomorrow before adding something to take short term. She said the pain could play a role in it.
10:45 Megan the NP from the Transplant team said he’s going home. Horror face from us only because of the horrible night. But, she said she doesn’t want him here in all the corona craze (my phrase) just to get pain meds every 6 hours. Got it. She’s trying him on a Tylenol 3 and seeing how that works and will send him home with whichever works best for him. Labs Friday. Taper the prednisone orders will be in discharge papers. He’s always at 5 mg but they increased it for this stay along with that heavy IV dose Saturday. He will be tapered back to normal soon. She is going to talk to the endo lady and let her know it was most likely because of the increased steroid that his blood sugar levels were increased as well. The cellcept antireject med will also come from Tasha his coordinator as to know when to switch back. Aslo labs again April 6.
If he needs to be seen for pain or whatever to call first. Call. They will telemed or conference call. No just showing up at our beloved Kirby ER we learned way back in the day from Jane (our first and most beloved transplant coordinator!)
11:00 Christian Galati NP came in next. She is going to talk to the above too because Kevin has not felt like eating this morning. She doesn’t want him going home and vomiting anything he eats. He wants him to eat and ordered those good old “boost” shakes. If it’s what I’m thinking after trying one they just kept stacking up in the corner of the room until discharge… She is fine with labs Friday and a telemed call next week. All his liver numbers look good and are down. I asked even ALT and AST because those were the final hold outs! She said yes…even those. That’s good. She listened to him too. Said his color looks back to normal almost no yellow in the eyes. If we get to go home today it will be later…
11:30 Abby our nurse just gave him Tylenol 3. She wants to know in an hour what his pain level is. He’s a 5 right now. She wants to figure out which one helps him to be more comfortable. She also said Luze the endo lady wants to send him home with a sliding kit…(?) insulin stuff. I said did she hear from transplant because they didn’t seem to be worried at all about this. She is going to check. Before she educates Kevin on it she said they at least need to see if they are all on the same page. Agreed.
1:30 The Tylenol 3 worked. He ate lunch. The pharmacist stopped by with updated med list. We are getting discharged today!
Dr. Galati 3:30 March 2, 2020
Dr. Galati wanted to see Kevin. We flew him home for this quick visit. Funny thing. Kevin was the one talking to him. He said the doctor said to call his office and get them to schedule you Monday afternoon. When i asked Kevin what time Monday on Friday night once we picked him up from the airport he said… oh. I forgot. We were suppose to call. K. E. V. I. N. !!! That makes me the bad guy Monday morning when I call to ask what time. 😬 It all worked out but no one knows Kevin there anymore. But they do now. 😂
•Dr. Galati wants drug level labs Tuesday morning for Antirejection medication.
•A malaise
•Iron
Wild card how you feeling
Could have been antibiotics
Keep gloves on! Try not to touch surfaces
Labs in the am
(Seat guru for airline tickets)
BVI in May bring a basin and three sets of medications 😂
2/26/20 Kevin Called 1:00 am Wednesday
Sharp pain in my the left side of my back and real bad discomfort in my abdomen
(He finished his two antibiotics yesterday from last weeks stay of pneumonia Levoquin
Clindamycin —Levofloxazen)
We called OPC for on call transplant coordinator. Was on hold. So we called Texas Liver Specialist after hours. Left a message.
1:30 His RA Phillip is driving him to the ER
4:20 Well you know my luck. A code happened shortly after I got here and the dr checked me out. So I just now got something for pain.
4:45 I just had a cat scan. And they did an X-ray and they said the pneumonia looks cleared up
5:00 My white blood cells are up to 11 something right now (all last time they were 6 then low of 3s)
6:45 Kristina NP from Texas Liver Specialist Dr. Galati’s office called. She’s going to speak to the team this morning. Dr. Galati was already wanting to see Kevin in March from the colitis diagnosis so I asked her to try to find out what that appointment needs to be. Just an exam or another scope.
9:00 Dr. Galati called. He wants one of us to text him tomorrow at 11:30 with a Kevin status update. Wake up. Eat. Start your day. If your in cloud nine he wants to know. If you feel like crap. He wants to know. He did say that antibiotic would give anyone colitis!
We discussed dates to see him. He’s still in the decision making about colitis. He may kick Kevin upstairs to the colitis expert.
10:00 am Email from Tamieka
Good Morning,
The Transplant Emergency Line is still 713-441-5451, my apologies if you didn’t receive a return call. In addition, it is common for Antibiotics to cause GI Upset, as it kills ” Good Bacteria” in the gut in addition to the bad bacteria causing the infection. He can add a Probiotic to help restore Homeostasis & reduce Abdominal discomfort or Diarrhea. I will refer you to Tasha for any further intervention as needed. Glad to hear he is feeling better, make sure he is taking a stool softener with the Oxy to prevent constipation & he needs to start weaning himself off after 72hrs because those pills are highly addictive.
2/16/20- 2/19/20 Tenova Hospital Stay Powell TN
Kevin was admitted to Tenova Hospital in Powell TN Sunday Feb 16, 2020
Discharged Wed February 19, 2020
He went to CVS minute clinic w fever of 101.3 and they sent him over to the ER. They did a chest x ray and a CT scan and are treating him with antibiotics for possible pneumonia. They also started Tamiflu on him because they just cannot find the cause of the fever. In an abundance of caution as a liver transplant patient they spoke with his Houston doctor twice today and decided to keep him overnight for observation as well as discussed the best treatment plan.
Keith, Caleigh and I were already here for the long weekend for my uncle’s funeral, but after spending the day at the hospital with Kevin —it is clear that he is surrounded by the most caring people at Crown College. We praise Him for each staff member and friend that stopped by to pray over him today.
Please pray that the team here will find the most effective treatment plan for Kevin and that he would heal quickly, and for us as we fly back Monday night to Houston.
Monday 17th :
We are leaving for the airport. They just got him moved up to a room on the floor. Been in the ER room since yesterday morning. Pretty. Scary. Curtain for door. Germs everywhere. Shared bathroom. BEST NURSE THIS MORNING. She said. I’m calling Pam. Her floor supervisor. Got him moved. It’s ALWAYS the nurses. 💚 I’m a crying mess. But Melissa is gonna check on him after she gets off work and tomorrow. Not to mention all the floods of Crown people who hop in. The floor people are fabulous. He has dinner and breakfast ordered. Getting IV meds and Much Much needed rest.
Me Keith and Caleigh attended chapel this morning. Caleigh toured the school after. We are praying for His will for her college choice.
Tuesday 18th: Dr. Korey the ER doctor called me all the time. He was the best. He’d talk to Dr. Galati, then Kevin then me. He made sure I was in the loop and stepped us through exactly what he was doing. Melissa was able to get away and stay with Kevin.
Wednesday 19th: Kevin was discharged and given a note to recover in his dorm for 5 days. He drove himself there so he drove himself back to the dorm.
February 3, 2020 Dr. Galati phone call: It’s Not GVHD
Dr. Galati just called. He said straight up it’s Colitis. He said we’ve been waiting for this shoe to drop. It’s a pretty good case of colitis. He wants to see Kevin late March and wants me to text him some loose dates that he would be available. Maybe soon a limited colonoscopy or a sigmoidoscopy. He also wants to get a feel for Kevin’s weight. He mentioned all along he was thinking it was PSC w Colitis. While this didn’t come out of the blue he has been dealing with this for a while now. Actually since about March of 2019. This has been PRESSING. That’s all I can say. While it’s difficult to say we are so thankful it’s colitis … we are because it’s not the GVHD (Graft Versus Host Disease) crazy out there aggressive rejection. We are praising Him for answered prayers! So far we have texted him that Kevin’s best dates are Mondays so either March 23 or 30. Waiting to hear back from him plus we probably need to ask what kind of appointment.
January 22, 2020 Update from Dr. Le
Good news for Kevin from Dr. Le! They just called! She showed the ultrasound images to Dr. Sternbergh of New Orleans and he agrees with her that nothing needs to be done. Follow up in one year again for ultrasound. Call two months before especially if United Health is still at odds with Methodist. (They were on my list to check today too!)
January 20-21, 2020
The saga of the slides. You really never want to hear your doctor’s office say “I didn’t know about the slides” when for twenty plus days we thought said slides were being looked at for a second opinion. Somehow things slipped. I questioned had I not called to check when would they have ever known to do it!?! I told Keith the doctor’s office needs a whack a mole type system. The patients need to pop up so the “staff” can remember to follow up with what they told them they would do. It was like news to them! Well. I’m sorry. But you tell me there’s a random weird chance that Kevin could be in a weird form of aggressive rejection and you are sending biopsy slides to get another opinion then get it done! Or at least act like you knew! The office called back three times one day and I could not hear the connection. So I called them back. I repeatedly tried all day. Leaving voice messages to anyone they transferred me to. Finally sent an email to Marie. She called bright and early the next morning only to let me know nothing has happened and it was her trying to reach me yesterday. I said we have other ways to be reached. Home phone. Email. I can’t even put into words the amount of frustration this brought me. As my family would say: she’s an angry elf. Efficiency. I’m thinking it’s not too much to ask. Just present efficiency and this mole will be whacked right back down. The different people I spoke to treated me like I use to treat people when I worked retail and they came to check on their order. “It’s in the finishing process.” Only, this isn’t retail! And I wasn’t buying it. One lady commented so vaguely: well I’m sure they were calling about the medication. I said that was three weeks ago. What would they need to tell us!? And another commented it looks like the form was sent to whomever it was being sent to so we will know something soon. I said. Ummm. I’m gonna need more details than that. Dr. Galati himself gave us more specifics than that. He was wanting to send them to HMH MDA… so which place has them?
January 9, 2020
Kevin heads back to Crown for Spring semester! For the record this will actually be his very first Spring Semester at Crown. His Freshman year he came home in February with liver failure and then after transplant he spent that first Spring semester abroad—at Crown Hall in England.
January 8, 2020 medication update
Kevin’s new medication is called Sulfasalazine 500 mg tablet. He takes 1 tablet 4 times a day. Start day is today. CVS gave him a 90 day supply. He had one week of Asacol or generic Mesalamine 800 mg tablet he took 1 tablet 3 times a day until we could get the insurance to approve an acceptable one for the new diagnosis of colitis.
January 8, 2020 Dr. Le phone call
Dr. Le called tonight. It’s incredible that she called us at home so late to tell us that she looked at the ct scan images and she doesn’t think he needs a procedure. It was not occluded. It was patent. She reminded us that Kevin is her only hepatic stent and that HMH in Houston doesn’t do many of those. He’s her only one. Ochsner does way more liver transplants and she saw them more frequently when she was there. She’s seeing Kevin’s NOLA doctor tomorrow and will hand him off the images. She said he never forgets a patient. He’s going to most likely get back to us next week after their conference they are at together. But for now it’s looking like hepatic stent wise. He’s good. Our insurance is extended officially until April so if he needs one it can be here in Houston or Nola. Such a praise for now! Kevin said welp. We just have really good doctors. Amen!
Jan 3, 2020 I sent this email to our Houston Methodist Hospital (HMH) Coordinator Tamieka
Good morning,
Kevin update about recent colonoscopy showing some form of colitis plus a crazy Graft Versus Host Disease and yesterday’s ultrasound at cardiology showing possible stenosis. (And a scar pic. Always a pic!)
•he had a colonoscopy Dec. 17, 2019, by Dr. Galati’s private office. Bedside Dr. Galati said it looks like it’s under the colitis umbrella. Path results this week confirmed just that plus a crazy way out there possibility (😱) Dr. Galati called us. Kevin and I were both able to listen and ask questions. Love that doctor! He said it’s definitely colitis and called in a medication for that. (Insurance doesn’t cover it so we bought a week’s worth to get through the new year holiday this week and to touch base w correct people)
Who do we get this medication from now? His office. You Tamieka? First set came from his office so them?
•the other way out there possibility he worded it like this. The pathologist asked him if there was a chance this kid could have Graft Versus Host Disease? Dr. G asked if we had heard of that. We replied we don’t even know what you are saying. (I’m sure if I dug out the two transplant notebooks it might be in there?) anyway. I love his response. He told the pathologist thank you very much but I’m a logical guy. You can’t go giving this kid two diseases. He said we are not giving him the disease of the week. (Lol) But since it’s in the report he’s going ahead and sending it over to HMH pathology and MD Anderson and maybe one other for their opinions. Dr. G said it’s going to be a wait and see kind of thing. IF the colitis medication works then we have our answer. He has been having diarrhea since March of 2019. We have done all the things to keep from scoping but even this summer Dr. G said he needed a scope. This was just first available time and I’m kicking myself for not getting it done sooner. Kevin never tells us all the things. He’s even been waking at night with symptoms. I’m like. Kevin! That’s information we needed to know months ago…
•yesterday’s ultrasound at Dr. Linda Le (Lay) office in Smith tower. She saw possible stenosis. She wants a CT scan today to decide if a procedure needs to be done. She trained under Dr. Sternbergh at Oschner who placed this hepatic stent 6 weeks after transplant. After we saw him for a follow up he told us we could use her since she’s closer than New Orleans. Now thanks to Methodist and United Health Care our insurance Dr. Le said she would not let us pay out of pocket like we were willing to. She found a place near us called Herman Imaging and we are scheduled for 2:00 today for a CT scan. Kevin will then drive the images to her office because she is seeing Dr. Sternburgh next week at a conference. IF he needs a procedure to clean out or replace it Oschner is in network and it’s half way to his school in Knoxville so that was her plan.
•Dr. Galati and y’all i don’t think know this last ultrasound information. How do we relay it to him? Through y’all? We did fill out the transplant extension. We don’t know if it’s approved. I know it’s a lot of information. And I know as of two days ago y’all aren’t even in our plan. (All the tears. All. Of them!) But Dr. Galati said we would cobble something together. Lol. His private office is in our plan. Dr. Le is through April. I’m sire y’all are getting this exact situation times a thousand!
January 3, 2020 Imaging at Memorial Herman because fight between HMH and UHC insurance
Kevin’s CT scan at Memorial Herman Imaging center based on yesterday’s ultrasound report of possible stenosis in his hepatic artery. Bonus. This facility is 11 minutes from our house. What!?! Not an hour and a half in traffic!?! Kevin is leaving from here probably first for food then second to Smith Tower! Finally he gets to drive through all that traffic while I finish my day in the spring area running errands. He plans to stop at TIFF’s treats and grab some cookies for Main 7 HMH. I Love that it was his idea. He loves those people on that floor! It’s Friday so hopefully we will know something by Monday. I’ve lined up dental and vision and trying for chiropractic next (anything to try to help w migraine) The eye exam is due to crazy glasses mix up. He wore new script glasses all semester. We had to mail them to him. But they caused him to see multiple lights in classes and church and while driving at night he would see multiple cars headed towards him! Crazy! This is information we need to know! He goes back to school next week so most of this will not be resolved before he leaves but it will all work out.
January 3, 2020 Kevin’s Yearly Ultrasound to Check his Hepatic Stent With Dr. Le
6 weeks after transplant the flow between arteries wasn’t good enough so Ochsner had us see their cardiologist Dr. Sternbergh and he placed a stent. We followed up with him for the first 6 month check up but he recommended Dr. Linda Le (pronounced Lay) in the medical center in Texas Smith Tower. So we’ve been seeing her now. This is the second time. Last year was smooth sailing. All looked fine. This one however she said there looks like a possible stenosis. Blockage. Because she is covered until April with our insurance, we were fine seeing her. But since she saw what looked like a blockage, she didn’t want to do the CT scan there because it isn’t covered. We tried to do the out of pocket thing. I was like thinking to myself we can max that out right here and now and stick it to United Health the rest of the year. But she wouldn’t let us. So she had to have her people find an imaging place for us to schedule a CT scan. The plan is to get the CT scan. Get the images to her ASAP. She sees Dr. Sternbergh next week at a conference. IF A PROCEDURE is needed to clean out the stent it would have to be where our insurance covers it and since she cannot do it, she’s sending us or wants to send us back to Ochsner. It’s kind of on the way to Crown. Who knows if all this will get resolved before he has to be back at school by Jan 10. Oh. Wait. I do know. He. Knows. He is with us. Ever since the phone call about the aggressive rejection disease that one pathologist saw might look like GVHD I was just already doing my normal Sunday School prep now that it’s my turn again. We left off praising Him through the Bible in Haggai. And sure enough when I circled praises for Him back in the day in that short book twice I praised Him for being with us. I use this analogy. So many times we have been close to the edge of the cliff. Just ready to tumble off. But then the tests or opinions will change and it will all be a non event. While we’ve seen many cliffs we cannot tumble down without landing on His strong and mighty hands. And one sweet friend of Kevin’s we met along they way sent us by means of a thank you a hand lettered framed picture of Kevin’s bracelet verse. Isaiah 40:31. It was the very day we got the call later about his crazy scopes report. Caleigh was with me when I opened it and I had tears. I don’t even know if she knew it was his bracelet verse. Just such a vivid whisper that He. Is. With. Us!!!

December 31, 2019 New Medicine for Colitis
Yesterday after the call from Dr. Galati he said to send a text tomorrow (New Year’s Eve) in case he runs into a snag to be sure he gets going on Kevin’s medication. He went home last night and studied Kevin’s current list of medications to decide which one.
They got one called in named Asacol generic Mesalamine and it’s 1500 dollars for 30 days. Keith was at CVS and they worked up a plan to just fill 7 days worth. I texted Dr. G only for him to reply ugggh. So he has started those meds and we will wait. Now that our insurance United Health Care didn’t reach an agreement with HMH he also added we will cobble something together. Our coordinators are our lifeline. I don’t want another coordinator! That’s who we would reach out to for information about this exact thing.
December 30, 2019 Pathology Results from Scope …
Keith said wait a week and text pretty much the same thing. Smiles. This time I waited a couple more minutes 😂
12:10
“Good afternoon Dr. Galati. This is Beth Troutman—Kevin’s mom. Checking in on possible pathology results from his colonoscopy on the 17th.”
Reply:
“Yes…checking
Beth…sorry for the delay. Just got the report now and spoke w the pathologist. I’ll call shortly.”
The phone call came after his day ended. Cannot tell you how much we love this doctor! I carried around my phone and paper for the ready. So glad of God’s timing! Kevin was actually finally with me. We were all home to listen. Basically, he said it is colitis for sure and leaning towards ulcerative colitis. He’s known all along it had to be colitis and wondered who missed this colitis on Kevin!? But even his last scope before transplant he thought where’s the colitis and never got it.
The second thing is a wait and see and a most likely stinking hopefully NOT. And it’s Host Verses Graft Disease. That’s a scary term for transplant patients. Aggressive. Rejection. Especially seen in bone marrow transplant patients of which Kevin is a liver transplant patient. BUT. Since a pathologist spotted what looks like that then dr g is sending it along to more eyes to see. If the meds he started this week for colitis work that’s a really good sign. So. We wait and see.
December 20, 2019 Text to Dr. Galati
Exact text sent to Dr G worded by mr few words Keith so as not to abuse my privilege(!) oh. He said text around noon. Literal me…
12:08
“Good afternoon Dr. Galati. This is Beth Troutman—Kevin’s mom. Checking in on possible pathology results from Tuesday’s colonoscopy.”
No news meant no news. Even though I like a response. I’m told I’m old and nothing said means nothing.
December 17, 2019 Colonoscopy 6:30 am 15th floor Baylor Clinic Something like International Endoscopy Center
•first yesterday’s prep day was awful started out not so bad but by the end of the night he could not drink much of the second stuff and pretty much vomited what he did sip. Yuck. Add a migraine and hunger and it’s a horrible terrible no good very bad day. Through in more horrible.
•Dr. Galati did the procedure and talked bedside to us afterward. He took 6 at least biopsies. He threw out there that he feels like it’s under the colitis umbrella. He said to text him Friday (see? approachable!) to remind him to look for pathology results. It’s Christmas week so Friday may be too early. There’s just a lot of funny stuff in these visits that make everything a little less stressful but Kevin already tells me I put too much detail so will skip it but if you ask me in person oh I will share! Lol We took him to a place off the Grand Parkway for breakfast called The Toasted Yolk.
December 2-9, 2019 Trying to call and schedule Kevin’s Colonoscopy with Dr. Galati through his private office
•it was finally time to get this scheduled. I encountered a sad thing. When I called his private office there was no Lexi Phoung Erin Samantha Araceli … this is gonna sound like we are all that and a bag of chips but no one knew Kevin. 😱 One gal actually told me we needed an office visit because we hadn’t been seen since 2016-17! I’m like well he’s a transplant patient and he is seen in the OPC by Galati and his coordinator. I said all of the below posts stuff. Galati wants him scoped. Tamieka wants him scoped. Only gettting it scheduled I finally had to play the mom card. I called weeks before he was coming home for break so we could get this process started. No matter what my screen saver says. Time is NOT on our side! Lol! I gave them one week plus to get back to me. Then made contact again. They said there isn’t an opening until February! I was like why didn’t you tell me that last week. This is just the scheduler I’m talking to. I know that’s a high turn over position. So. I dropped the card. I said look. I have Dr. Galati’s cell phone number. I can text him myself or like he said back when he saw Kevin last: call one of my girls. Call my office. Let’s get him scoped. He’s the most amazing approachable doctor! The scheduler sent me through to the next level and before the day was over Kevin had this appointment. I have no idea what it’s like from their side and maybe one day I will see it but for now I’m still recording things for the book we need to write about the other side of the door. It does sound rough but when we go pretty much low key until we need high maintenance then that’s the way it has to be. I just KNEW we could not postpone this any longer! Scope will be dec 17 at same place in medical center. On main. Across from where tiff had her girls. Yeah. Keith will love those directions!
November 16, 2019 Labs, Stupid Mail Order Pharm and it Appears HMH and United are in a Throw Down of a Lifetime
•Labs at University of Tennessee Knoxville LabCorp (great labs again!) Patient portal has all these organized. I hope it stays backed up for life!
•many many many emails back and forth to Tamieka over mail order antirejection medication refills. We usually get a call from their system reminding us to order. I go online and click refill. Love the online option especially since some encounters with the phone pharmacy techs have been … insane challenging infuriating (fill in the blank) This last time was such an ordeal. It takes all the life out of me to fight them and it just should not be so! It’s exhausting on our part when “they” don’t see what they should see to make the reorder happen. Woe is me when the script expires and we have to make contact for another refill. But I love his coordinator! She goes to battle with us! Gets put on hold and has complete idiots to deal with and she is an RN for HMH! Praise Praise Praise this time around we got a 90 day supply!!!! Now if I can train my body to not stop in it’s tracks every month before the 7th I’m good! That jolt to my system of: did we order the antirejection meds!!!??? Is a whopper! Lol
•our insurance and HMH are in contract negotiations. It’s pretty bad when I’m checking Cals snap chat story that there’s a story from one or the other of these two getting information out there to let patients and insured know to contact someone to let them know how we feel. All the social media outlets have random articles and arguments. I asked Tamieka about it and she thinks they will come to an agreement by the years end or if not transplant patients get an extension. Ok. For now.
9-6-17 to 9-6-19 Two Years Today!
Kevin is 2 years today! (Bailey was a year this past June) We are thankful for the donors and their families. We pray for them and think of them so often and even though we do not know them we cannot forget their great gift of life. Bailey never forgets. She does the same thing for each person in our family. For Cole it’s the blub blub of her finger over her lips; for Caleigh it’s “more more anna” which means get in there and play Frozen on that piano so she can dance and twirl in the living room! With Kevin she just walks up and stands or sits as soon as she sees him and lifts her shirt…preciously pointing to her scar. So he joins her. They are forever and ever Scar Buddies. And we are forever and ever thankful for the scars. Each time I see them or think of them I am so so thankful for the donor and family behind that scar.


Scar Buddies 
August 6, 2019 Kevin Headed Back From Canada Needs Labs or Possible Scope?
Contacted Tamieka on Kevin’s way back to Texas. Same stomach issues. She was off getting “hitched” as she put it! So happy for her!!! Anyway. She said: “Let’s wait to see how labs look, because if Magnesium is too high, that could be the culprit. Just want to make sure we can adjust medications first to resolve these complaints. In the event that this is not an option, I would suggest the scope to be on the safe side.” In a previous email she said to contact Dr. Galati’s Private office for scopes. His labs did look great! It’s such an amazing thing to study the numbers and she them in between the normal ranges. Thank you Lord for taking care of Kevin!
May 15, 2019 HMH (Houston Methodist Hospital) OPC (OutPatient Center) Clinic Visit with Dr. Galati
Clinic appointment with Dr. Galati and current coordinator rounding. (We missed Tameika this go round) Maybe Jamie (?). For the most part it was a quick visit. Kevin was loaded up to start his drive to Canada for the summer where he was to serve. The main problem was working out what to do with his continued “stomach issues” he wasn’t over with since his bout with food poisoning over in England. Dr. Galati wanted to scope him but there wasn’t time. So they ended up having him leave a stool sample and were prepared to call in something along the way if he needed it. Turned out nothing was found so Kevin served an entire summer in North Bay Ontario. We invited ourselves to see him here too. This time we made most of the journey by Amtrak train! From San Antonio to Buffalo then by car the rest of the way. We ended up meeting his crew at Niagara Falls and after touring there followed them into North Bay. On his way back home at summer’s end he was able to catch a couple of baseball games checking off stadium visits on his journey back to Texas. He still struggles with migraines and the same stomach issues. We’ve been in contact with his coordinator several times. Too much magnesium. Not enough magnesium. BRAT diet. All have been tried.
January 13, 2019 Email from Crown Hall for a place for Kevin to get labs
Dear Mrs Troutman,
Thank you for your email. I believe Mark McElreath was going to be in touch with you regarding further details.
I told him I would send you the details of the nearest medical centres to where he will be living. These are listed below. They will need Kevin’s records from the States which you have obtained. For Data Protection (which is heavily regulated here) Kevin would need to contact them personally or a professional on his behalf.
We have spoken to an NHS nurse and she would be happy to help explain the National Health Service functionings if Kevin has questions about differences.
Benjamin Galyen who lives on the Crown Hall property would be happy to help with arranging transportation with Kevin.
Every blessing,
Lareina Kiser
The Spa Medical Practice
Droitwich Health Centre, Ombersley St, Droitwich Spa WR9 8RD
Phone Number: 01905 772389
Worcester Royal Hospital
Charles Hastings Way, Worcester WR5 1DD Phone Number: 01905 763333
Tuesday Jan 8, 2019 The Semester Abroad in a Paragraph!
Kevin flies to England to study and serve for the Spring Semester. He was able to get labs over there a couple of times. Maybe three times total. We got results from ONE. He said they basically said we will let you know if there’s a problem. (!) He had about three rough weeks in all in the semester total. A couple of typical things and one horrible case of food poisoning. What I love is that we never knew until after the fact. That kid! 6 hours ahead time wise made for calculated conversations but he didn’t let us know everything during those calls. We learned our mail order pharmacy our insurance company uses for his anti rejection meds doesn’t mail the monthly medications overseas! They said they would mail them wherever he was. They lied. And I let them know. We had to mail one month to him. It was insanely expensive and stayed in customs for almost three weeks. We were about to tap Cole to head to England as courier when it finally was delivered. We didn’t send him with a semester supply because they said they mailed them! They sent us a three month supply so we hand carried them over Spring Break. We had a great time inviting ourselves to visit him and deliver meds! He had just finished the horrible week of being sick and I had to just keep telling myself that was all…he was really thin but who wouldn’t be after that. Poor kid. He is the toughest thing!
January 3, 2019 Follow up with Dr. Linda Le Cardiologist 8 am ultrasound 9:10 appt OPC 2nd floor fast after midnight & Dr. Escudier follow up 11:40 Green Park One
Follow up w ultrasound. All looks great. Now we can follow up in a year. Jan 2020 unless there are any problems.
Dec. 19, 2018 RESCHEDULED follow up with Dr. Galati OPC 10:00 am
Dec. 1, 2018 Labs Knoxville at LabCorp University of Tennessee Medical Center
Nov. 21, 2018 Follow Up with Dr. Galati OPC 10 am CANCELLED
This was cancelled and rescheduled for 12/19/18 with them in OPC. We need to check to see if they need labs before this visit.
Nov. 17, 2018 Labs Knoxville at LabCorp University of Tennessee Medical Center
Kevin said today’s lab lady was extremely slow!
Nov. 3, 2018 Labs Knoxville at LabCorp University of Tennessee Medical Center
He borrowed a friend’s car to get to these labs since his truck battery decided to die. He was thinking about last labs and the tac level and there is a chance with the pill box that all meds are in am and pm and he’s suppose to take all meds except the tac and zortress before labs so he said maybe one of those tiny tac pills did get taken accidentally which made that number so high last week. Kevin is back to baseline from these labs! Katie said labs every two weeks for this month then back to every month. (We need to find the name of the lab place in England from our insurance company…)
October 27, 2018 Labs Knoxville at LabCorp University of Tennessee Medical Center
10/31 Katie emailed: Beth I am concern with Kevin’s labs. He did not take his Prograf prior to labs on Saturday correct? His number has jumped up to 10.9 from 5.8 without a dose change. If not I am not sure why his numbers have been all over the place since going to school. Maybe he has added something to his diet. Or maybe the timing of the medications, or his lab times on Saturday. Can you have him call me if he gets some time so we can review. He will need to hold tonight’s dose and then decrease back down to 3mg twice daily. Continue with weekly labs. My desk number is 713-441-9819.
Kevin was able to reach her and I think he said the same thing skip the next tac dose but the med might have been 3 am and 3.5 pm but will confirm with Kevin…
October 20, 2018 Labs Knoxville at LabCorp University of Tennessee Medical Center
10/23 Katie emailed: I am still waiting on the Prograf and Everolimus levels but I wanted to let you know the liver numbers are coming down still, which is exactly what we want. I will be in touch once the last 2 levels come in.
10/24 Katie emailed:
Everything is looking good the Prograf is a good level. However the Zortress is still a little low considering the recent spike. Please increase Zortress to 2.5mg in the morning and evening. Let me know if you have any questions.
October 13, 2018 Labs Knoxbille at LabCorp University of Tennessee Medical Center
10/17 Katie called me and said the lab didn’t run the TAC level. Inconceivable since that is pretty much the reason for labs. And it was on the order Kevin printed and carried in with him! I spoke with Kevin and he said this place even though it’s at the University of Tennessee Medical Center LabCorp here isn’t as advanced as the one we went to back in the day in Tomball, Texas! He said they hand write the tests on the labels…hand write. I told him to triple check the order with them and don’t leave that office until he knows the tests he’s there for are ordered.
October 6, 2018 Labs Knoxville at LabCorp University of Tennessee Medical Center
10/11 Katie replied to labs:
I went over Kevin’s labs and a few of his enzymes’ are up. His Prograf level dropped drastically, most likely this is the culprit. I am going to increase his Prograf to 3mg in the morning and 4 mg in the evening and also go up on the Everolimus. Please increase the night dose of Everolimus to 2.5mg . We will need labs weekly for a bit to make sure they are coming down.
Kevin can you go this Saturday for me? I won’t see the increase in the Zortress but I will in the Prograf. Please also plan on labs probably the following 2 Saturdays maybe only one.
September 1, 2018 First Labs Scheduled in Knoxville at LabCorp University of Tennessee Medical Center
Katie was out of office from 8/22 to 9/10 when she returned she sent this: I see that his alkaline phos is slightly elevated but it is not a level for cause for concern. It can be elevated for a lot of reasons, we will just keep an eye on it. If it continues to rise then we may make some interventions. His Zortress is just slightly low. We run it 3-6 after a year out. It being a little low could be why the phos is up. I do not feel comfortable adjusting medications using labs that are over 2 weeks old so I think we should just wait for the next labs.
Tameika responded for her that his liver function tests were withing his baseline range and Tac is 6.6 and Everolimus is 2.8
Kevin’s had headaches and missed class from them about 2 or 3 times
August 13, 2018 Registration and PCP in Powell Visit
Registration went great! We also went to meet with his new PCP who is in Powel and was very understanding and thorough. He didn’t even have him do labs since he just had huge ones last week so Katie faxed them over to Dr. Brakebill’s office. He gave us each his card and said call with any concerns. We found a hole in the wall pizza place for lunch then it was time to say goodbye…that is when a couple of tears streamed down. But he will do fine and really we are all just so happy for Kevin!
August 9-10, 2018 Leave for Crown!
It’s dorm move in time! And I’m HAPPY for Kevin!!! I told a friend I did cry after seeing Caleigh hug Kevin good by this morning but only a tiny bit because I’m trying to be H. T. tough! She replied: you will never be that tough! lol! Kevin is just ready! It is just an amazing fun thing to be in this plane today. Once we got to the Big House Friday Dr. Evans who helped tremendously when Kevin was falling apart here back in spring of 2016 came straight to us and shook our hands and said he KNEW this day would come and he’s prayed for this day for Kevin! We got this same reaction from Pastor Sexton and anyone we ran into that knew us from Pastor Pope and from Kevin’s short time here before. Such a blessing!
August 8, 2018 Last Pentamodine Treatment West Pavilion Tower 11th floor
Kevin did these every month since he was hospitalized last December having such a low white count. Instead of taking Bactrim everyday they went this route. It was outpatient and very hard to find the first time but once we found it we could almost get back to it every month! One of those park at the OPC and dog leg your way to Smith Tower then go up the to 3rd floor and walk up a weird hidden ramp type bridge to the 4th floor of West Tower and take the elevator to the 11th floor! It was a quick outpatient visit each month. The respiratory therapist would set him up in the “tent” and I would read a book in the waiting room just outside.
Almost every single time we are near Main 7 Kevin says want to go say Hi to Main 7…so we hop over and usually we get who we get. Over the year we have gotten to visit several times and every time we see someone new who remembers Kevin from “his time spent on this floor!” They usually have a fit and cannot get over how good he looks! He is lectured by the nurses more than a mom would especially knowing he’s returning to Crown. They are like: WASH YOUR HANDS! Eat right! Stay at this weight! They love Kevin! They also tell him always come back and say hi:) And when there is a chance they want him to hop in the rooms to encourage patients waiting for a transplant. Kevin had this when we were waiting and it truly was an encouragement seeing someone on the other side of it!
Earlier this morning Kevin saw his new PCP Dr. Lee at Capstone Family Clinic. No more Dr. Pope:( He kept him through the transplant and until he turned 21. She did a follow up from an ear infection/rip he was seen by her a week or so ago. All things are healed up and clear! This was wonderful news too.
August 2, 2018 Yearly Clinic Visit
One of the highlights of this visit was in the waiting room before getting called back. Kevin leaned over and asked had I emailed Jane (pretransplant coordinator) to let her know we were on the floor. I hadn’t but did it right that second and in no time she replied “I’m on my way!” We got to catch up with her! She is just the best and really did so much not only to get us to New Orleans in an expedited way once we decided to be on that path but the entire year and a half of hospital stays and in between stays she was the voice on the other end of the phone encouraging us and teaching us so much. She lectured him too: wash your hands! We will always keep in touch with her and she wants a picture of Kevin in front of his dorm.
In clinic we saw Katie our newly trained Post Transplant coordinator. So thankful for the couple of pretransplant coordinators who stepped in to fill Debbie’s shoes until they could train one. We saw the NP we saw in the hospital during the “antibiotic only appendicitis” and it was good to catch her up on Kevin. She said so we don’t need to meet to decide when to take it out like she mentioned during the hospital stay back then. They gave us copies of the ultrasounds, x-rays, and bone density scans. Everything was “unremarkable” which is a good word to hear!
Labs can now be done every month!!!!! We found a lab in Knoxville that is open on Saturdays so Kevin won’t have to miss class. We also have a PCP there and found a CVS. They were happy to see Kevin and so glad he was getting to return to college. Katie already made his follow up appointment with her and Dr. Galati in the OPC for the Wednesday before Thanksgiving. So he is now officially turned over from the surgeons to the hepatologist.
A fun thing he got to do after this visit was head to the airport with Cole to fly to Vegas and see the Sargents! So happy that he got a redo on a vacation and on top of that some fun brother time before heading to college.
July 31, 2018 Follow up with Dr. Escudier oncology
Follow up from pathology report and in general for keeping an eye on Kevin closely due to immune suppression as well as his autoimmune disorders pretransplant. She evaluated him. His spleen measured smaller to her from her notes from previous exam. She questioned him and wants to see him in 6 months. She will look at all the scans from yesterday and the labs.
She has a nephew who when he was 12 had a liver transplant. He’s 40 now and about to have a child graduate from high school. She told us before about him but today I asked what at age 12 caused his need for a transplant. She said he was born with biliary atresia… they told them back in the day it may not last long. They didn’t expect it to last 12 years she said but it did. I told her about Bailey…how amazing!
We also heard from Katie in the portal about yesterday’s 11 vials of blood drawn: she said labs look good see us Thursday.
July 30, 2018 Yearly Scans labs and ultrasound
9 am Labs 11 vials 9:30 Bone density scan 10:00 Abdomen Complete Ultrasound 10:30 Abdominal Doppler Ultrasound 11:30 Chest X-Ray
They call this the yearly scans and it’s a tiny bit early for since he leaves for college this is when they said do it!
July 26, 2018 Kevin sees new PCP Dr. Lee at Capstone
Kevin has had two days of ear pain so we are getting him in. He is now needing a new PCP for home and Powell. Dr. Pope only sees them through 21…bummer. We just missed it. Anyway we got the newest doctor who just started this week and we liked her. She did say he had a rip in his left ear drum with fluid build up. She put him on antibiotics. Also no going underwater for about 6 weeks until it is completely healed and she said to wear an earplug in the shower to which Kevin told me later…yeah I’m not doing that. And can he just quit popping up something randomly normal for the summer!
July 16-22 Vacation to the Ozarks and Kevin overloaded on Mag!
We made the trip to the Ozarks stopping in Eureka Springs to see The Great Passion Play and hide away in a cabin. Kevin ended up having a reaction to an increased dose of magnesium he was put on at last Thursday’s clinic visit. (they dc cellcept so now only on 2 antirejection meds: Prograff (Tac) and Zortress (Everolimus) Who knew that would cause a not so fun vacation for him. I kept thinking maybe the antirejection meds changing needed to be balanced out but then found a forum and could read random strangers experience…I googled LT with upset stomach and found lots of comments on one forum about the culprit is magnesium! Love transparent strangers telling all! Sometimes it can be helpful! Once we figured out the cause of the upset stomach we held the magnesium then was able to pick up a slow release mag. We also went to Branson at stayed at a cabin there. We saw Samson which was amazing but the Shepherd of the Hills play we were scheduled to see was cancelled as we were walking out the door because of unexpected weather. (this was the night and time of the tragic duckboat sinking in Branson…so very sad for all those families involved. Keeping them in our thoughts and prayers) We were able to sneak into Shreveport Bossier area for one day on the way home to see family and get our Johnny’s pizza fix!
June 24-30, 2018 Kevin Chaperoned Teen Camp at Indian Creek plus saw Noah’s Ark Exhibit at the Creations Science Museum
Kevin got to go along to this camp with Caleigh and our church teens to serve as a counselor. He was so excited to do so. I was excited the appendix was out in time for him to do so! He also turned 21 at camp doing what he loves to do!
Kevin appendectomy June 14-16 details
That’s right…I said appendectomy! He is that rare recurrence. He was hospitalized for this just a week before but they opted for antibiotics to treat him. I wish it would have worked but am somewhat relieved that it’s now DONE and DONE. And in true Kevin fashion he waited for this recurrence for late at night. Like midnight late! We called the on call coordinator just to tell them we were headed down and that helps let the ER know they know. Below is lazy me just pasting my updates to Keith. We were soooo tired. Painfully TIRED! (Bailey was transplanted on June 12 so we were B1 tunneling to them too!)
Text updates to Keith:
Thursday late night to ER
12:41 am early Friday morning
Got in ER. Charge nurse was notified we were coming by on call coordinator. So she got right to him. Put him in exam room 10. Grabbed a Dr. on way in. (He looks like Jonathan Pope) Dr. Boshkey. He examines him and said he’s clinically presenting with appendicitis. He’s gonna call Dr. Saharia before doing a CT scan cause he’s 20 and wants to minimize radiation exposure. So. Labs are being drawn now.
1:11 am
Dr B came in and said he spoke to Dr. Lunsford the attending for Saharia. They want a CT scan w contrast to check for perforation… he went ahead and has admitted him upstairs in a room but not until after the CT scan. *we never got in said room…stayed all night in ER until surgery…
1:23 am he’s at a 6 for pain
Finished the contrast
It was nasty
He’s probably gonna ask for pain meds
(Let me know what they see)
I will
1:55 am he got morphine for pain. Number at a 7
(Poor guy!!)
So. Glad. We. Came.
2:30 am they took him back for CT. I was asleep sitting up and she went to get me a recliner. *praising Him for the ER nurse who took care of this mama too
From Keith: Text if you hear anything… I have sound turned up, so I am going to get a nap
6:31am
(How is Kev?)
6:48am
We are still in ER. Fell asleep. He’s sleeping. We are waiting on a room upstairs. I’m in a recliner.
8:00am
He’s having surgery in about two hours
12:19 pm
Nurse stopped by. Next is anesthesia then they take him back
The surgeon Dr. Lunsford was great! She actually was able to perform it laparoscopically which was a huge praise! He went in late Thursday night. Surgery early afternoon Friday and he was released the next day on Saturday!
June 14, 2018 Follow Up with Dr. Le from the Ultrasound CANCELLED
Cancelled and rescheduled because now Kevin is having surgery! Appendectomy…he just wants to one up Bailey in that scar department!
June 12, 2018 Bailey Transplant Surgery and Kevin Hepatic Ultrasound
Crazy. I remember getting to the waiting room for Bailey so early in the morning and of all things Kevin and I had to step out to go to one of his appointment down the street. He was having a image of his hepatic stent. First time follow up with Dr. Le who the NOLA doctor recommended for us to see to save a trip to New Orleans. Sweet Bailey. Getting her precious gift of life!
The Approach to Appendicitis In Kevin: Antibiotic is the new Appendectomy! Who knew!?! No. One. Ever! (May 30-June 7, 2018 Details below)
Wednesday May 30, 2018
Kevin presented with pain and nausea in his right side. He said it came on about the time he was hanging door flyers for VBS during outreach but it wasn’t too bad. He powered though the rest of the day and evening attending church and driving himself home. He thought maybe if he had a bowel movement it might help but came downstairs just doubled over! It was awful. It was 10:30 pm. We left his good pain meds and nausea meds in Vegas over spring break and hadn’t had them replaced yet. So I called the on call coordinator. He was wonderful. Most pharmacy’s near us that use to be 24 hour now close at midnight. Thankfully he was able to get it to one near us just in time otherwise I would have been driving far away for it. So we got him his nausea meds but the night was rough! He kept waking me just like pre-transplant days. And we had no pain meds except the one Dr. Galati said never take that New Orleans had him on. But at 1 in the morning he got that! I’m writing this in hindsight but sure wish we just would have gone straight to the Kirby/59 ER. In my mind I thought it was a reaction to his anti Rejection meds. He’s had one episode of that before when they added back cellcept at a high dosage. We found out two days later it was actually appendicitis so below will be the play by play of that hospital stay. Sometimes I text updated. Sometimes I emailed. Occasionally I started a note. Combining all that for my medical memory now because this has tuned out to be quite the ordeal! They wanted to approach it conservatively especially since he’s still under a year of transplant. It was almost too much for me at some points because we had never heard of this approach. We just assumed he would get in. Get that thing out. Go home.
Thursday May 31, 2018
Clinic with Tamieka and Dr. Saharia.
Kevin can DC cellcept. He started Zortress May 15 and they wanted to wait to pull cellcept to make sure the other two were in therapeutic range.
He showed/pointed to where he was feeling the flank right side pain. We described the horrible previous night. He added a UA to his labs. Wanted him to add stool softener as well. Dr. Saharia ordered a CT scan for tomorrow because he wanted Kevin to have a bowel movement before imaging. They were thinking possible kidney stone. They sent tramadol for pain to the Scurlock tower walgreens. If zofran doesn’t help with the nausea they can send Reglan. They said a heating pad can be used for help with constipation. Later I read not to use it if appendicitis was suspected! Oh well…since they actually thought it could be a kidney stone they called in that stuff to help with that.
The elevator ride from the 26th floor of the Out Patient Center to the lobby was awful! Kevin was not doing well. He needed to take his morning meds. And he needed to eat before doing so. But he didn’t think he could make himself do either. Kevin couldn’t walk after appt. and was getting more nauseous. I tried to get a wheel chair, and the valet guy wouldn’t let me. So then I looked up and there was the old man driving the courtesy golf cart along the bridge between all the towers down there. I asked the man if he could help get Kevin to the Marriott because Kev was just doubled over asleepish in the lobby. By the way. Get the Marriott app! I’ve had it. Looked up room availability and pricing. I was able to tell her when she said they could offer a medical discount that my Marriott reward rate was cheaper than that. Praise the Lord they let us in early! It was 10 am. Kevin needed a place to rest. It actually was another horrible day. He couldn’t even lift his right leg into the bed. I had to do it for him. Looking back his white count was the highest on this day. Tramadol didn’t help.
Tiffany was so concerned about possible bowel obstruction she slipped over to listen to them using Bailey’s stethoscope. Bailey at this point is in Texas Children’s hospital waiting for a liver. Admitted April 12.
Sent this as a prayer today request for Kevin to church:
Please be in prayer for Kevin. He experienced pain and nausea late last night. The surgeon at his routine transplant clinic visit today suspects a possible kidney stone. He will have a CT scan tomorrow. Praying for comfort and His healing mercy for Kevin.
Friday June 1, 2018
We stayed the night at the Marriott and checked out and went straight to the CT scan. It was a 2:30 appointment but we got there early. So glad because they took him back early too! We got a call from Tamieka his coordinator at 2:40 saying the scan shows he has appendicitis and give her 30-45 minutes to direct admit him to Methodist. And also. Don’t eat or drink anything.
Sent this to the prayer chain:
Update and continued prayer for Kevin. He has appendicitis. They are admitting him. Please pray for relief from pain and nausea now that they have the reason. I sent this to Kevin as he went back in the CT scan “Praying He REVEALS what He already knows is wrong so they can see it!” Love how He answered that prayer! Hate that he has this.
Admission Lobby around 4 and Pastor Pope found us to pray with us before Kevin was admitted in case it was a quick surgery. He was on his way south of town to speak at a graduation. He also had to hunt down Bailey she went with Tiffany to the lobby to meet a friend for coffee. I told pastor it was a praying in the lobby kind of day!
In Dunn 411 after 5:30 or so
They haven’t said much. We’ve been the ones telling them everything. #Shift.Change.Admission.
They nurse hung the IV meds. Zosyn antibiotic. Kevin doesn’t have an IV yet. The respiratory therapist came w ultrasound to get “blood gases.” We are like. Ok. We have no idea even to this day what they ran that for. But the day shift nurse stepped away so they could do that so his IV never got placed until later. It was so close to shift changing so who could blame them!
Meanwhile I googled “how do you get appendicitis.” Learned that the heating pad the dr ordered yesterday to help with pain and possible bowel movement could cause an inflamed appendix to rupture. Yikes!
Nicole was our night shift nurse. She seemed tired when she came in. First impression. The IV was a drama too. She first tried to place it on his wrist. She was leaving to get the scissors to cut off his newly placed hospital ID bracelet when I got the “look” from Kevin. So when she got back in I said please don’t put the IV there. Kevin said he’s had them there before and they hurt. Plus it’s just in a weird place. I pointed to the forearm where he’s had them before. Then after a while I saw she was trying to put it in the bend of the elbow! Kevin for sure glanced over at me. At which time I hopped into action for the one and only job I’ve ever been given at this time and that’s IV placement advocate! She looked and said she couldn’t put it there because the veins are too short and it would blow or something like that. So she never cut the wrist band off and placed the IV there all the while it was in the way and she bloodied it. So she had to cut it off and he went about a day without the ever important ID bracelet to scan She made us anxious. But I kept thinking of all the new nurses I know and decided to just go easy on her! It could be Olivia.
Saturday June 2, 2018
They have IV antibiotics hanging. No machine. No beep. It just hangs to infuse. I guess that’s a thing. But they never disconnected it all night. I could be getting Bailey’s heplock incident mixed in here but I’m thinking when the medicine is done you cap the IV. So it made me nervous just seeing it hanging there.
8:30-9 ish
Text to Ruth and maybe others if anyone was asking at his time!:
“I feel like I am about to hyperventilate. Kevin said I sounded ticked to the nurse. Well. They didn’t have his current anti reject meds correct. At 9 am. Even though last night less than 12 hours ago they did. No one reconciled the meds like we have done for all 20 hospital stays. I have my list. Ready. So this morning’s nurse felt my panic I know. (She had Kev in dec) and asked if anyone reconciled them with us. I told her no. Last night’s nurse said the doctor does that. 😡 I also pointed out to her the hanging IV antibiotic bag and told her I’ve been asking all my nurse contacts why it’s hung this way. I did not tell her You said they are all just being lazy. Lynsey (morning shift nurse) said they had 10 admissions last night! My comment in my head is. Oh. Well. Your a hospital. Deal with it. Isn’t that what you do. If you have a thousand beds there’s a possibility you will get a thousand patients.
But she said that about all the admissions while DISCONNECTING and flushing his IV 😊 So I kept my thoughts to myself.
I told her I was a little panicked about his appendicitis. He presented Wednesday. They were misguided at clinic for two days thinking it was a stone. She tried to call a dr to figure out why they changed prograff to .5 when it’s 3.5 two times a day. I honestly think they don’t know how to look at the screens. But “they” only sent point 5 prograff. (These are Antirejection meds in a liver floor you don’t just change dosages) She hopped out again and back in and said. Good thing. The Liver surgeon and NP are about to come in. And maybe they held off anti rejects for a reason. So I’m fine if they tell me the reason. He’s just so new to the new added anti reject med. And Thursday they dc one of them.
You get my text rant. Kevin already said I was mean. I’m not meaning to be. I’m nervous. Haven’t seen a single dr. I probably googled too much about liver patients and appendicitis! All the things I know not to do 😂😂😂”
11:00 the nurse brought the current and correct amount of anti rejection medication! He missed a dose on Thursday morning because he was so nauseous and in pain. We told the coordinators cause that’s what you have to do. So to completely miss another does just made me crazy. I kept telling them we have his medications. Can we just please give them. They said no. Praise praise they got this straight.
noon
Surgeon for transplant just came in w NP. Dr. Mobley and Natalie. But I had to tell the nurse that we hadn’t seen a dr yet. She said they were “about to come in” at 9. It’s noon. I’m telling you I was in panic because all I ever knew was in appendicitis the appendix comes out! Anytime I asked the nurses to check the surgery schedule they would and say classic nurse response: there are no orders.
So much to take in after from Dr. Mobley transplant surgeon with Natalie transplant NP liver team
They are going old school. Not really considering rushing it out. They will re-evaluate tomorrow. If he’s still tender they will probably remove. So he stays NPO. She said data shows now they shouldn’t do the removal but treat w antibiotics. I was like I feel like he’s a ticking time bomb. We left clinic Thursday and had to grab the golf cart man to get us to the Marriott. So she was aware of when he presented. She seemed laid back. I told her he goes back to college in 10 weeks not that she can control any of this but after two years of liver stuff I would hate for him to be set back because of appendicitis. She said they don’t even remove it if it ruptured. They drain and treat w antibiotics. They are for sure not worried about perforation either because then they would drain and he’s already on antibiotics. I told her about Debbie my sis in law she is going this route. Her doc in Louisiana said of the 6 people he’s treated slowly they have all needed an appendectomy. She feels like a time bomb too.
I also told her we are hearing everyone’s stories of appendicitis. And they all had them removed.
***me. And now it’s different. So…great. We get to be guinea pigs. I’m not that much more comforted but Kevin is resting and I don’t want to hype on him. But great day. I mean I don’t do change. If this is what “they” do then ok. But it’s contrary to anything anyone I know knows. But. What do I know. And apparently what does anyone I know know😂
Praying praying praying for wisdom and great clarity for the decisions that this team of doctors will make for Kevin. Great quote I read this am in Mathew Henry commentary “That which we take to be a dark cloud, is to God clear as crystal, through which he looks upon all the inhabitants of the earth.” To distract myself from this I am rereading Ezekiel😂🤭🤔 because I can’t understand appendicitis or that book! But was truly blessed by the explanation of the first few chapters… and I’m determined to understand it! I got nothing but time either 😊
8:00 pm Tiffany sent what Bailey’s liver doctors said. Dr. Sonny Harpavat and Dr. Goss said get it out. Of course prefacing with they haven’t seen Kevin nor his scans.
Sunday
6:30 am text to Tiff and CALL to Keith:::
Just reported the nurse we’ve had for the last two nights. I’m just DONE with her. She could not program the IV pole. She pressed and pressed for 30 minutes. I sat up and said seems like something is wrong. She was all Jamaican, no, it does this sometimes. It sometimes gives a problem. So then I said maybe we need to get someone in here to help. She said she would. Headed to, then it started beeping again. So she came back and pressed and beeped. I sat up. Mouthed to Kevin that I was done. Grabbed my phone and glasses to see the board so she went and got someone. Another regular nurse. I changed clothes. Then went in the hall looking for the charge nurse. I told her that I don’t know what it is but I don’t think she knows what she’s doing. I said we’ve had her two nights and if she comes back a third night we CANNOT have her. I asked how long she’s been here. I said we’ve had soooooo many nurses from pre transplant to now especially on main 7 and never have we had something like this. (I should have mentioned first night IV placement saga but didn’t) I came down stairs for coffee and to take deep breaths. I know she must have been in her patients room down beside us because after our PCA woke us at 5 am — the IV pole down from us was incessant. Which everyone on our hall must have been thinking about our room!
Silence the sucker!
All I ask is for a nurse with confidence, courtesy, and common sense!
I know it could be funny. But not at 5 am! The first night I was all it could be Olivia. I’ll be nice. She couldn’t even scan the medicines in. Ever. It was insane the amount of time each pill label thingie took her. First impression was she was tired coming on Friday at 7pm! She just seemed tired. Sluggish. Lazy? And she never talked! Like tell us! Say I don’t know why this machine is being so dumb. Apologize. She was all internal. Wrong messages being sent! I kept thinking she doesn’t know what she’s doing. Kevin told me later that after she drew labs she put the bandaid just randomly on his arm. NOT even where she drew labs!:0
Monday
Dr. B on Transplant surgery team
One of the transplant surgeons came in. He said more information but similar to what everyone else has been saying. He is looking at the CT scan in about an hour and with liver transplant patients they just want to be careful. His liver is settling back down according to the labs. Some of them were elevated. Today is more settling. If CT shows an abscess they place a drain to remove all of that. If it shows it’s responding better they let him sit for a while. Sometimes even taking it out at a later date. (? That was new to me)
I’m so jumbled up with all the information. But he did seem to explain more details. Should have recorded him. Didn’t know him or his sidekick. So at first I thought it might be the surgeon who takes out appendixes coming for consent! Cause I’m still on that boat!
I asked will they do surgery today? He said probably not. But keep him NPO until after seeing scan. He may be able to drink some things. If it’s emergency surgery he would have to be spiking a fever etc. so we are not there yet.
Encouragement to myself!
“thou shalt cover thy face, that thou see not the ground:” Ez12:6 I know it’s totally taken out of context and even the middle of this verse but… it’s where I feel we are. We are trusting Him with our faces covered and not even looking where we step. I have been in and out of Ezekiel. I thought why not sit during hospital time and read it slowly also checking chapter by chapter commentaries. So that’s where I was…
This was an issue going back and forth in my head. I wasn’t completely mental but told myself look: Kevin has eyes everywhere on him. So reach out to them. It’s not like I’m telling on the Dunn 4th floor staff. I’m just getting opinions of the people who know Kevin. So I sent all his coordinators an email explaining Kevin’s current situation.
I have heard back from Nancy the NOLA (New Orleans) coordinator. She is passing info along. I also heard back from Tamieka the coordinator who admitted him. (Houston post transplant coordinator)
She emailed this:
“Just think with everything else he has going on with his elevated liver enzymes, the last thing they want to do is take him back to the OR. Also, I know that everyone is just trying to be helpful in giving you their stories with appendicitis, but if there is one thing I’ve learned in transplant is that Everyone has a unique & different experience….whether it be in recovery or to the meds or etc. Let’s just focus on Kevin & how he responds to the current treatment of IV antibiotics. Hopefully he won’t need, if so, we will cross that bridge when we get there. Such a blessing to hear about Bailey’s exception points. I am still praying for your little princess.
Thank you so much for the updates, don’t hesitate to email or call if you need any. Ttyl”
10:45
Ok. Agnes our Day shift nurse came in and I asked who were those people just in. Dr. B was like the team resident/fellow and sidekick was Kim the NP. She asked her about Kevin and they told her to call Dr. Saharia. He said the scan looks like it’s improving:) So he can be on a regular post transplant diet and they are taking it conservatively. Things happenin kind of quickly today…praise God!
11:00 Bummer of all bummers the nurse just hopped in and said she misunderstood the order and said he’s on a liquid diet. And tried to make it sound exciting like he can drink all the juice he wants! I’ve never seen Kevin so bummed. He doesn’t want to go through this again, and he’s not happy about all liquid😂 He’s asleep…and I’m trying not to cry and cry.
New Orleans Nancy replied three times. Once with Dr Tyson (Nola version of galati) is on vacation. Next with Dr Sonnier (actually did Kevin’s Transplant) said it’s hard to really know without seeing him or the scans. He said transfer could be an option. Then 15 minutes later, All the doctor’s think the appendix should come out…
So. There’s that.
For days I’ve told people that I feel like a firefly trapped in a mason jar. All flying around and trying to be His light all the while smacking into all sides of that clear jar trying to MAKE my own way out. My kids hate it when I speak in analogies. But it paints the picture!
Absolutely putting this case before Him! To operate or not to operate! Who to trust! I don’t even want to make the decision!
Kelly H sent me all the versions of Job 5:8 and it is what we have been doing! Perfect timing.
“But if I were you, I would appeal to God; I would lay my causes before Him.” NIV
“I would seek unto God, and unto God would I commit my cause:” Job 5:8 KJV
“”As for me, I would seek God, and to God would I commit my cause,” Job 5:8 ESV
“”If I were you, I would go to God and present my case to him.” Job 5:8 NLT
“”But as for me, I would seek God, And I would place my cause before God;”
Job 5:8 NASB
Tuesday
Met Dr. Saharia in the hall. I went for ice. 8:30 am. And came back from 5 doors down with the cleaning lady cart blocking the door and the surgeon in the hall. So he spoke with me holding two tiny complimentary cups of ice. He asked about his pain and nausea levels. I told him he walked around the unit once then needed to stop. He is concerned with Kevin’s normal transplant meds. His creatinine was elevated. He is needing to change his antibiotics. Possibly dosage levels.
He is truly thinking and so many things are on the, my words, his don’t do surgery list. One is the Antirejection med Zortress that Kevin switched over to on May 15. Last Thursday cellcept was discontinued. (I actually thought he was dealing with a reaction to that because he has before. This time completely different area for pain) It hinders healing. It’s one of the reasons they don’t start it right after transplant but give time to heal. Another is because of Kevin’s history with auto immune issues. Several things there to take into account. (Fissures? I’m telling you we were in the hall.) Another reason is an increase risk in damaging the cecum where the appendix is attached. It’s best done at first presentation. He said Kevin was having symptoms already when he came in. It sounded like it just wouldn’t be good for Kevin to go in. Also he said his white count is better. It’s improving. Along with the CT scan showing the appendicitis is improving from Friday’s scan to today’s scan is another plus that the antibiotic treatment working and no need to perform the surgery.
Today after speaking with him after he came in and evaluated Kevin he said he thinks he’s doing better. He pressed and checked. I point blank asked him: so are we still considering surgery at this point and he said no. I asked if it were his kid in the bed what would he do: he said, treat with antibiotics. He said appendicitis can be treated with antibiotics. Kevin is actually responding to this treatment now. And I have to say, like I told Kevin for today, I have a tiny bit of comfort and peace about that but what I don’t have peace about is something we both know they cannot guarantee and that is recurrence. The manager last night gave me two research articles on antibiotics vs surgery, and it’s interesting, but “at the end of the day” and I quote researcher Dr. David R. Flum: “It remains to be determined whether benefits of potentially avoiding an operation with the antibiotics first approach are outweighed by the burden to the patient related to future appendicitis episodes, more days of antibiotic therapy, lingering symptoms, and uncertainties that may affect quality of life.” That last phrase should be all caps. (He used a similar phrase in the paper earlier, “anxiety about future episodes of abdominal pain”)
The key take away from reading the papers to me was this phrase: all the studies excluded patients with compromised immune function. Kevin is compromised. And the entire research once that guy summed it up said IT REMAINS TO BE SEEN! Aka : got no answers.
We have been praying. One verse I sent out earlier was in Ezekiels and repetitious but we are still there. I know it may seem out of context too but still so fitting for us now. Basically blind faith…”thou shalt cover thy face, that thou see not the ground:” Ez12:6 We are trusting Him with our faces covered and not even looking where we step.
I have that tiny peace because Dr. Saharia is the eyes on Kevin now. I trust his thought process. He knows transplant patients. He knows immune compromised patients. His patients all are. And on top of that he knows Kevin who has underlying autoimmune issues which led him to transplant. I told a friend who called while I was writing this update that today at 9:41am on Tuesday I have a smidge of comfort and peace. A great friend sent this verse from Job 5:8 “I would seek unto God, and unto God would I commit my cause:” and followed up later with trust your gut and your heart.
•Oral Doxycycline when they dc vancomycin yesterday. Creatinine was creeping up so the pulled it.
11:45 Samantha came in from Dr. Galati’s office! She found us because Kevin popped up on one of her lists she checks. Not often but she saw it last night. She said they would be rounding later tonight. After 5…
6:30 pm Dr. Galati and Samantha came in! It was so so so good to see Dr. Galati. I’m telling you it was an answer to prayer having someone whose known Kevin from the beginning and before transplant. He examined him thoroughly. I joked with him about searching his websites for articles or research about liver transplant patients with appendicitis and I couldn’t find one. He said that’s because there are none! He would say my first thought is get it out but then he started thinking and thinking and said I don’t know. He is calling Dr. Saharia tonight. He said together they would come up with a plan. He definitely agreed that the anti-rejection medication Kevin is on everolimus would need to be switched to cellcept. What they need to determine is how long before that medication is out of his system. How long should they let the appendix cool off/settle down. We said we want what we know you cannot guarantee and that is recurrence. And if there’s a recurrence we need a plan. He totally agreed. He said he would be back to talk tomorrow.
Tuesday June 6, 2018 9 month transplant anniversary!
7:30 Dr. Galati woke us up! (Nurse Rhey said later she pointed to our room and said let them sleep to everyone trying to hop in before them😇)
He had a long conversation with Dr. Saharia last night. Dr. G has actually never had one of his patients have appendicitis. Other hepatologists on this floor have. He has zero experience with it. So he listened to Dr. S. And he quoted the research and Dr. G was surprised that the chance of recurrence is 5-10% also the guideline for taking it out after it settles down is very involved. No great details but you just could tell it was complicated. They were glad he didn’t get it out at some random emergency room because of the anti rejection med he takes Zortress (everolimus) would have totally hindered healing. Dr. G said the final words were once he gets over this take it out. But he would leave it to Dr. S to define when he’s “over it!” He also wants him to add miralax today for a while to be sure he’s cleaned out. He’s still tender and he said cleaning it all out can help with that.
I had 4 of his books. I bought one for each of my kids. So he said last night he would be back today to sign them and he did! He brought his pen and signed away! He asked what stood out to me in the book. And i said right off the bat when i was reading it I even hollered this out loud to my household that he watched movies of surgeries when he was 5 years old! He went into great detail about these movies and how even when he would show them to the kids on the street! Just so funny! I also reminded him how very blown away we were with the 2 g sodium 40 g fiber diet and told him Ithought his office sent us a bad cut and paste!
8:10 Dr. S said the removing of the appendix later is still an option. But he hates to do that if it’s not infected. Plan for the next time IF there’s a next time is one day of antibiotic remove it the next day. Also he said sometimes taking it out when it’s inflamed it gets complicated because it’s hard to even find it. One time he had to abort the surgery on a patient because he couldn’t find it from the inflammation and didn’t want to cut too much. Treated w antibiotics. They have been worried about his kidney function because his creatinine has been high. But Dr. S said it’s trending down.
I will say I was dreaming Kevin needed a kidney transplant when Dr. Galati woke us up!
Also. Saharia says he can go home tomorrow!
May 15, 2018 From Tamieka after labs on 5/14/18
She said no need to come to clinic this Thursday but after up and down and up and down for the last 6 weeks it seems and with starting a new medication I said I would like for someone to lay eyes on Kevin. Especially since he’s starting a new medication. So we are keeping the clinic. We will see whoever!
“Hi Mrs. Troutman-
Spoke with Dr. Ghobrial today about Kevin’s labs on yesterday. He is pleased with the findings thus far. His levels are trending down appropriately. I was told to cancel his clinic appointment for Thursday and recheck labs only. He wants to continue to monitor him before electing to do any procedures. Believe it or not, he wants to try Zortress (Everolimus) for him. I reminded him of our previous conversation when you were told the medication was contraindicated for his diagnosis, to which both he & the Transplant Pharmacist had no knowledge of. I was told there was no recent literature or statistical data that they were aware of to support that claim.
Long story short, we will Initiate Zortress & recheck labs on Thursday. I know that you already have the medication, so please have him take 1mg (2tabs) twice a day, starting with his night dose. We will recheck labs on Thursday, to include Zortress level. If it is at a therapeutic range we will STOP the Cellcept. But he will not need to come to clinic.
I know that is A LOT to take in, so email me with any questions or concerns. I will schedule his appointment for labs now.”
May 14, 2018
This lab needed to be redrawn. I asked what was it for. And got this explanation from Tamieka:
The IKNOW Viracor is a serology that helps us determine his sensitivities too his immunosuppressive therapy. It helps us determine if the medications are adequately suppressing the cells that influence rejection or not.
May 9, 2018
Tamieka called. She said she read up on Kevin’s donor because his BILI is elevated. I think 1.4 from .7 she didn’t know about all Tamara knows from the abscess and sore throat and cough from Monday. At first she said Dr. Ghobrial wanted an Ercp. Then I filled her in on the permanent stent. Gave her Nancy’s number at Ochsner to get questions from. She was asking did we do high risk blood panels. I told her I’m not where I can see my notes. I was driving to tx ch. Then Dr. Gohbrial actually called her while she was on the phone with me. He wanted her in his office. They spoke of Kevin and then sent this in an email.
“Just spoke with Dr. Ghobrial about everything & he agreed to wait til Monday [5/14/18] to see how his labs trend & he wants to see him in clinic on next week.”
I had pulled over between parking garages because I couldn’t believe all i was hearing. Just last week his labs were fine.
May 7, 2018
From Tamara after Kevin saw Dr. Pope about an abscess spot on his thigh.
“I saw Dr. Saharia and told him all the *scenario and he believes we need to decrease Cellcept to 500mg twice a day until next lab draw on Monday. He agrees that the infections are probably what is causing the increase in LFTs.” Dr. Pope put Kevin on Bactrim to cover this. They were fine with that choice.
*”Scenario” mentioned above: Kevin was having a sore throat and cough along with the random spot/abscess on his thigh. So we just went in. Nothing to worry about on the throat and cough. Just safe OTC for that. He drained the abscess. Cultured it.
May 3, 2018 Email to Tamara
“Tamieka reached out yesterday and needed to update his flow chart. She had just a few questions like dates of prednisone increase etc. She wanted labs next week to check his Alk Phos. She’s not too concerned about it but wanted to do that.
So she scheduled one for Monday. I haven’t checked the portal but that is what her intentions were. She said Dr. Ghobrial likes top facts from the flow chart and she would be ready for him on Tuesday when she saw Dr. Ghobrial. (I’m sure I’m not spelling that correctly!)
And above all she knows you are getting his labs and didn’t want to step on your toes. We appreciate all the eyes on Kevin. We made his dorm deposit today.”
May 2, 2018
Tamieka conversation for 30 minutes.
She said all his labs look great except alk phos and it was up from 120 to like 161 and Dr. Ghobrial didn’t even want to be bothered by it unless it was in the 500’s. She mentioned so much. I had questions that she answered. She and Tamara are keeping an eye on Kevin especially since we lost Debbie. So it can get confusing. But Tamieka is a coordinator and Tamara is stepping in as one but works transplant recovery. Sometimes they have an overlap in information and I’m figuring out they don’t cc one another so I probably should. She did mention Kevin has two of the most difficult things preteansplant to treat post transplant. He won’t be the normal off most meds by a year but it won’t be too long before he is. She said I could call in Tuesday or Wednesday’s to go over labs with her if I wanted to. He is back getting labs every week. They email the changes for his medication and I try to copy it over here. It is a lot to keep up with!
April 5, 2017 Could Maybe be Looking at a possible Mild rejection (Kevin will be 7 months post transplant tomorrow!)
|And…who knew I did write last clinic’s update! Been carrying around the notes to do it sometime and looked and it’s already written!|
Labs and clinic day:
While Bailey is boasting a zero BILI dodging a possible procedure last week, Kevin is maybe starting to have a mild “rejection.” Dr. Saharia mentioned that word today at the routine lab and clinic visit at the Out Patient Center in the medical center. His LFTs (liver function tests) have been creeping slowly back up and today’s labs—they were doubled. So, there was discussion back and forth, but they want Kevin to increase all three agents he’s on: prograff from 2.5 mg twice a day to 3 mg twice a day and cellcept from 750 mg twice a day to 1000 mg twice a day and prednisone from 5 mg once a day to 40 mg once a day. (Steroid will decrease starting Monday after labs if they are lower) Just normal anti rejection medication gives him a migraine about once a week. Increasing meds will most likely add to that. Praying it doesn’t! The surgeon Dr. Saharia said he will just have to take the headaches and he’s glad he has effective migraine meds.
Since Saharia mentioned the word rejection he said not that this is happening but the lfts are slowly trending up. So labs every Monday. Clinic in 2 weeks or sooner if things don’t trend down.
We saw Tameka today but Tamara emailed us and said not to leave the 26th floor until she saw us. We got called back super early! And we had Bailey. We were prepared to wait for hours!
From Tamara: (for my records)
“I spoke with Saharia and he agrees we should increase Cellcept first and then the Prograf. So increase cellcept to 1000mg twice a day and we will see labs on Monday.”
And in no time she sent this:
“Ok don’t kill me, but I was not looking at this mornign’s labs. His labs from today have double so unfortunately we do need to increase prograf. Ughh, tell him Im sorry but increase to 3mg twice a day. Also Im going to call in prednisone for him to CVs on Spring Cypress. Have him take 40 mg everyday starting tomorrow. We will reduce on Monday if labs come down. This will be a good test to see if the prograf is indeed the culprit.
My apologies again,
Tamara Merriwether MSN, RN, CCTC”
We had a fun day with Bailey all day too! Even took her to the zoo. So we got in late tonight.
To do:
Dr. Linda Le cardiologist schedule appt
Dr. Susan Escudier schedule a follow up based on pathology report and Dr. Carter Davis NOLA advise.
We have a contact to help with insurance questions at the 26th floor. She gave me a pink sticky note with her contact info. We need to send heart cath mess to her and check if optim is being billed correctly. We should owe nothing because transplant is covers 100%
April 1, 2018 Easter!
Kevin was awake all night. He had the “vomit virus:0” He needed nausea meds several times and vomited with horrible painful nausea. He said the nausea hurt. He was miserable. But he made it through the entire day without an episode and did not need hospitalization for hydration! Tamara responded quickly for him to hold cellcept and prograff for a couple of days and she said to be careful because this virus was exremely contagious.
March 8, 2018
Clinic and labs
It’s been a terrible. Horrible. No. Good. Very. Bad. Day! Kevin had the worst night. We had clinic and labs already planned but he was in pain and having horrible nausea all night so he said he wasn’t going! I’m like oh your going! We have to. With spring break plans around the corner not to mention a 6 month old liver that could be in rejection we just had to go. He said he’d rather go to the ER than sit in the clinic. I don’t get that. That’s crazy talk! Finally at 5 am the nausea meds worked. He got a little rest before having to head down. He was still in right side pain and tired. We didn’t get to see the new coordinator and for a couple of hours we thought we were coordinator less again but it was a mix up. They are all still trying to cover for Debbie. We saw Jamie and she had a surgeon Dr. Saharia come in. We know him! He was SURE the culprit was adjusting to the increased dose of his cellcept. The highest dose they want an autoimmune patient on is 1500 mg twice a day. We had been doing only 1500 mg a day until a night and a half ago. Then they said all should be well as long as the labs look good. The labs we found out late afternoon looked good. Tamara said they were a little elevated but nothing to worry about. She will remain our coordinator. She actually works recovery but said she could handle Kevin. Whew!
I had HUGE phone issues and ended up without a phone all day which added to the terrible awful. And I have been in the iTunes hole for too long all day and night thinking I almost have it only to start all over again so many times. Somehow I even encrypted myself out of my fresh back up! Then after hours and almost completely done my stupid old iPhone that kept having a black screen decided to pop up a message that said hold this up to the new phone to synchronize it! I’m telling you I could have thrown it at the wall! It is a lesson on patience and I know so many people struggling with real other issues beside Kevin that I just plugged along. Sucked Keith in part of the journey to recover the phone! Cole got a break even though we could have used his hac- king skills on that encrypting thing! We say it every time! We need to pay more attention to this stuff!
Anyway, earlier Kevin and I both went straight mentally wise to the only thing we knew to do with pain and nausea. Lots of praying! Pain meds and nausea meds and I’m sure I have my lip chewed off. I was wishing I could get the word out but this time God just used me and the few who got through!
I also know how happy I’ve been all week thinking about and preparing a lesson to start back teaching Sunday school. And it dawned on me that every time I get ready to sit in that chair someone lately goes in the hospital! I just knew we were going to be admitted. Those symptoms don’t have many other options. But today they did! Cellcept! Who knew!?! Poor Kevin. He will know how much his body can tolerate it for sure and we know it does not tolerate 1500 mg twice a day. He is to rest. Drink plenty. Stop cellcept for three days. Start back gradual and increase. Labs again Monday the 19th. And I mentioned our spring break plans to her: Vegas! She laughed! Just where a liver needs to be! I said oh no! We are straight up Baptist. No gambling. No drinking! We are in it for the shows and restaurants from the cooking shows we watched for two years in the hospital! And day trips! When Kevin heard me mention we had until 3 to cancel our hotel today without being charged he said he could sit in any room! So that helped us have peace to keep our plans.
Kevin has been getting much needed rest all day. After being doubled over with nausea all night I am just letting him sleep and eat the BRAT diet. Only we also threw in a baked potato!
Praising God we are home and my iPhone is restored on this new phone!
Feb 28. 2018
Tamara called. Our new coordinator.
He should be on three “agents” for anti rejection. Prograff, Cellcept, and Presnisone. Three because he’s autoimmune. His ALT is elevated but she said not too much. It’s 74. Tac is 3.8 from 4.3. I told her we aren’t on cellcept. Dr. Saharia stopped that in the hospital. (In December!) Debbie (last coordinator currently on extended leave) said start zortress. And we have it. 6 boxes of it and Tamara said he will never be on that. Ok. Anyway. She will email later after talking to me and hearing from Dr. Saharia if he wants him back on Cellcept. Alk phosphates were 170 she said was fine. I told her about the issues we’ve had and forwarded her the thread. I told her one thing we need changed is his transplant date. We’ve told everyone and it’s still in as when he went in to the hospital in dec for low counts as transplant date. I told her not 12-4-17 but 9-6-17! She did a gasp! And sent an email as we were talking to get that corrected! Yes! We already love her! She also said he isn’t scheduled for another clinic visit because he’s on every two months now but she said let’s get him in next week just to lay eyes on him. This makes me so happy. I told her he is returning to college in 5 months so that gives them time to level things out. I also mentioned his horrible migraines. This week he had three straight. It’s bad when he calls me to come massage his head in the night:(
We also left church early because he was hot and nauseous. It turned out fine. He needed to sit still and eat. Whew! I never like those two symptoms together!!!
She emailed this:
Hello,
Just spoke to Dr. Saharia and yes he needs to restart Cellcept. Start him at 1500 mg or 3 tabs twice a day. He is to have labs and clinic on Thursday 3/8 to see how is he doing. Hold his prograf dose tonight to see if it helps his migraine.
Let me know that you got this. Soon.
Tamara Merriwether RN, MSN, CCRN
Post-Transplant Liver Coordinator
JC Walters Transplant Center
Houston Methodist Hospital
6565 Fannin Ste. 1201
Houston, TX 77030
Main: 713-441-5451
Fax: 713-791-5045
Feb 23, 2018
Discovered Debbie went on an extended leave. Thank you to Rolita who is our neighborhood Liver transplant buddy! She messaged me and asked if I knew Debbie was on an extended leave. I replied no but today was the day someone at HMH was going to hear from me! We’ve sent several emails and all in the same thread as she requests with no answer. So our back is covered. She gave me her assistant’s info! I had it but wasn’t sure I ever used it and would have found it in time but it was so good to just have it so I could immediately call her. She actually answered too! Praise! She said Debbie would be back and all but for now she would get Kevin’s info where it needed to be. Before Rolita sent me the contact I already forwarded (borderline tattle tailed) the entire thread since we started with Debbie to Jane. (Pre transplant coordinator with Galati) I prefaced it with I am trying to contact Debbie’s assistant but until then here is what’s happening with Kevin. Jane replied in a NANOSECOND! She said anything for me and Kevin! We love her soooooo much! She said she would print out the emails and take it to Tamara’s (post coordinator too) desk. She said if she could she would hand lick Tamara for us! That’s good to know. Aracelli answered my call so we were doubly covered after not being covered. She scheduled labs for Monday. I told her no one has actually gotten back with us from the last labs. So she peeked at them and not sure what she is allowed to know or handle so I just said I was concerned his Tac level was not in the therapeutic range and that we’ve had a second anti rejection med that he hasn’t started because we are waiting for instruction. I mentioned we are fine not starting it I’m not trying to push it. I actually don’t know much on this side yet and we are counting on them. She said his level was low and they like it higher and I guess that’s why she scheduled Monday labs.
Feb 20, 2018
New Orleans Vascular Follow Up Ultrasound and Appointment with Dr. Sternbergh
Monday through Wednesday of this week we were in New Orleans for this ultrasound and follow up. It went great. He said things could not look better! He said time the next visit with leaving for College or even see if we can see his trainee who is at Methodist (Linda Lay?) now instead of making the trip back. We wouldn’t mind the trip. We kind of enjoyed eating our way through New Orleans those three days! My favorite latte was at district donuts so we hit that place every morning for coffee. And of course beignets on the way out. We got to take Pastor Jackson and his wife out to eat too. They said how good Kevin looked! They truly only saw him at his absolute yellowest! We sound so old talking about how good his color is! Pasting the ultrasound report below from the patient portal just for us to reference. They gave us a cd but I need to check and see if anything is on it. Last time we did that nothing was.
Kevin M. Troutman
US LIVER TRANSPLANT POST – Details
Study Result
Impression
Low normal hepatic allograft arterial resistive indices, slightly improved in comparison to prior examination. No definite hepatic artery stenosis on this exam. Continued surveillance is advised. Otherwise satisfactory liver allograft Doppler evaluation.
______________________________________
Electronically signed by resident: MUSTAFA ALHASAN MD
Date: 02/20/18
Time: 09:59
As the supervising and teaching physician, I personally reviewed the images and resident’s interpretation and I agree with the findings.
Electronically signed by: STEPHEN JOHNSON MD
Date: 02/20/18
Time: 10:03
Narrative
Time of Procedure: 02/20/18 09:15:00
Accession # 27496368
Technique: Limited abdominal ultrasound of the transplant liver with Doppler evaluation.
Comparison: Ultrasound liver transplants 10/31/2017.
Findings:
Patient is status post orthotopic liver transplant6 months ago. Liver allograft is normal in size. The liver demonstrates homogeneous echotexture. No focal hepatic lesions are seen.
The common duct is not dilated, measuring 5 mm. No dilated intrahepatic radicles are seen.
Color flow and spectral waveform analysis was performed. The main portal vein, right portal vein, left portal vein, middle hepatic vein, right hepatic vein, left hepatic vein, SMV, and IVC are patent with proper directional flow.
The patient is status post proper hepatic artery stent placement. Anastomosis site of the main hepatic artery demonstrates a peak systolic velocity 242 cm/sec.
Main hepatic artery demonstrates resistive index 0.55 with normal waveform.
Left hepatic artery shows resistive index 0.61 with normal waveform.
Anterior branch of the right hepatic artery demonstrates resistive index 0.54 with normal waveform.
Posterior branch of the right hepatic artery demonstrates resistive index 0.46 with normal waveform.
Component Results
There is no component information for this result.
General Information
Feb 8, 2018 Kevin medication update
Hi Beth.
Labs look good. Here are the changes that I would like to make:
1. Decrease Prograf to 2.5 am and pm. Start tonight.
2. Prednisone 5 mg is back on the list.
3. Magnesium 1 tab 2 times a day.
4. Repeat labs next week to check the level.
TY
Debbie
We are waiting for her to give instructions on zortress. Kevin remembers her saying wait for her instructions. So it arrived in the mail today so we will wait!
February 6, 2018 5 Months Today
Kevin is 5 Months post transplant today. And, he steps into “interning” at our church. Last week’s labs were in the portal yesterday but I never checked them until this morning. (We had Bailey for 9 days while Tiffany and Grant were in Jamaica and they got back yesterday! We miss her so much! I found a pair of her sockies she left on my bed and we’ve all been walking around smelling them! They smell like Pudge! Cals said they should make a perfume that smells like her and call it Pudge!) Anyway, so this morning I looked at the labs. You would never know the LFT’s (Liver function tests) were a transplant patient! They look amazing! All within normal range. We contacted Crown College as well in this last week and they sent a “re-enrollment” application for the fall. We are praying about the perfect dorm to meet his needs. All the while that donor family who we have yet to hear back from is really who is completely on my heart and mind this morning. (And every day that goes by too…) Thankful Beyond Words.
Feb 2, 2018 Kevin clinic update
We went to the clinic and labs yesterday Feb 1. We had Bailey. They actually didn’t have him an appointment even though they told us last month to come. I told them we are doing our part keeping appointments and they needed to do theirs remembering to schedule them. Really that last month’s clinic visit we felt like they were trying to back up out of the room as soon as they were in the room! Kevin felt the exact same way. We told the ladies at the front desk too.
(Our regular coordinator was caught with a fresh transplant so we had a back up and she seemed like a new and in training one. She was beautiful and nice but didn’t dot all the i’s or cross the t’s like Debbie does) Poor Bailey. We waited 3 hours on the 26th floor. I also had emailed at least twice with no reply all month. No news is good news unless you have questions and unless they say we are adding another anti-rejection medication and never tell you when. I would say it was a terrible horrible no good very bad day except we had Bailey and she makes all things happy even if she had a blow out once we finally got in the room and lost her precious pearl baby earring. Well. I’m not giving up looking but for now it’s gone! But I can replace it. In my jewelry box is all the single earrings my girls lost! Now they have a purpose!
So today I sent a follow up email that said we are waiting to see what the levels are 🙂
Here’s the reply so we remember what to do and when.
Hi Beth and Kevin!
The Prograf level is still accurate if it is a little over 12 hours.
Here is the plan:
1. Decrease Prograf to 3.5 mg in the morning and 3.5 mg in the evening. Start tonight.
2. Start Magnesium oxide 400 mg. Take 1 in the morning and 1 in the evening. You can get this over the counter.
Some insurance will cover it so I sent over a prescription to CVS.
Liver enzymes look great. No other changes. We are waiting to see if the Zortress gets approved.
I have made the medication adjustments on MyChart so that everything is up to date.
Return to clinic in April.
Labs next Tuesday at the Woodlands so that I can recheck his Prograf level. You have standing orders there.
Please respond to this email so that I know you received it. If you have any additional questions,
let me know.
TY
Debbie
We didn’t have the .5 prograff. Briova is mail order so that won’t work to change today. But CVS can refill if we pay cash and the price Briova charges every time we reorder his meds is 67. CVS said insurance denied it of course so we would have to use Briova but I told her the fee they charge. CVS was 120 but they had a coupon for us and it ended up being $3 less so we can just get it today and would have paid that anyway but would have been hours on the phone and waited for mail delivery.
The insane part of transplant medication and when they change the strength often can not really be effectively done mail order. Just a tiny bit of stress. But, It’s all good!
January 4, 2018 OPC Clinic Visit, Labs, and Tent Treatment
Debbie had another patient in another room who was recently transplanted so this clinic visit was disheveled. But we had our list of questions and were determined to get through them all! My list of questions:
Transplant date? they have it in their system as 12/4/17 which was when he went into the hospital for fever and low wbc and he was almost 3 months transplanted then so we asked them to change it to 9/6/17
Estimated GFR? This is one of the labs they check every time and we have no idea what its for and if we should pay attention to it. She said its all about the kidney function and that honestly they pay more attention to the BUNN (?) and Creatine (my phone blog app still will not open this page so I’m on my pc and it doesn’t like any of these words I’m trying to spell!) Which they said based on his last lab he needs to drink lots of water because it’s borderline…water water water
CMV last return was negative. Don’t know that I will ever completely understand this one. He was positive and the donor was; yet, the last test for this populated in the portal said negative. So I’m thankful he doesn’t have this now! They say it’s horrible for a transplant patient and normal untransplanted people can just walk around fine with it.
Where is the TENT treatment today!? The calendar even says HMH WP11 INF SR 3 and they just tried to somewhat tell us but then said ask the security guard because they only know the back way that we cannot take. Or something like that! So we had a wilderness wandering after but found it in time! We had time for lunch then I asked Kevin if he wanted to go to Main 7 which was the floor he was on 15 times and those people are like family. He said sure so we hopped up there! Everyone was so happy to see Kevin!!!! The first person we ran into was Dr. Seelbach…he said how great Kevin looked and that he wished more patients came back because they only see them at their sickest! We headed to the nurses desk and were just overrun with great people and smiles! The cpa’s who changed sheets and took stats were even wheeling their machines by to smile and wave! I saw several wiping tears! Such an amazing floor of folks! They even asked by name about Bailey (who was having her own issues starting this very day…see Tiff’s blog the Dailey Baileyyy for that update)
Next Visit? The next visit is next month with labs every other week! Huge Praise! Kevin wasted no time in getting away from me either since later when Cole was heading back to college for the spring semester and Kevin was in an off week for labs I was like you could probably go with him! I’ve never seen Kevin pack and shower so fast! I doubled over in the kitchen crying at that too! He was just too happy to leave me! But it was a great thing to cry for him being normal! They had a great week and I withheld all attempts of momming up their week and left them alone!
Billing? There is still the insane issue of Keith being billed for Kevin’s right heart cath back on 10/12/16! Kevin had to have it for them to list him yet they put it on Keith! We told them then it wasn’t Keith and we told our insurance. Well the hospital billed the insurance and the insurance paid it! We are beside ourselves and thought we were done until the red letters from debt collectors arrive in the mail this new year! I was ready to go toe to toe but they gave us a name Sue Weber and we know her and she knows us so we will calm down for a minute until we hear what she says. But only for a minute! They are the ones committing insurance fraud and we are being chased by debt collectors!
December 21, 2017 OPC and Clinic Visit and Labs
Cole took Kevin to this visit because I was sick! Since we most likely gave Kevin what he got to be hospitalized this time I did not come out of my room and didn’t want to be in the car with Kevin driving an hour down and an hour back! So Cole took him and it’s already January 17th as I’m updating this page and have no memory of what they said Debbie said other than things look great and labs next week! I know when I saw the labs later in the portal and hollered them out Cole said something like that’s what the clinic visit sounded like! WBC is this Tac level is this LFTs are this…he has like the same 5 labs drawn so some of us get use to those numbers. I was so thankful Cole could do this for Kevin! and me!
December 14, 2017 OPC (HMH Outpatient Clinic) Clinic Visit and Labs
This was Kevin’s first visit after hospitalized last week for neutropenia. (low white count plus fever) We saw the new coordinator Debbie and a female surgeon or “provider” who was in the clinic. She changed his aspirin to a coated one, refilled his ergo vitamin he takes every Saturday, made his “tent” treatments for the year once a month, and has him on prednisone since he is off cellcept. He’s off bactrim and the tent treatments replace this. HIs WBC was great. I think she said a 5. He is NOT anemic and she said don’t let anyone tell us he is but they make it look like he is with all the meds. His prograf level was 7.3 We asked about sailing. Sand is ok but she doesn’t want him in the OCEAN! He can travel but for the first year be careful and check with them. He can get in a pool now just not the ocean water because of all the bacteria. Keith’s sailing trip with the boys will have to be postponed for at least a year. She wants him walking 20 minutes a day with no core. She said pretend you don’t have a core because if you use it you could get an incisional hernia and that would look like an alien baby on the scar line:)
Admitted to Houston Methodist Dec 2- 6, 2017 for fever of 102 and low white count
*** the iphone blog app hasn’t worked for me for two weeks. I’ve been keeping notes and will try to use my pc to upload them. Kind of afraid of that site on the PC because I’ve pretty much only done the app. It already said “there’s an easier page editor. Switch now!” So do I click it and hope it all stays! Oh if i were truly a blogger! Cole can’t get home soon enough for semester break!
December 6, 2017 The Much Much Better Morning!
I sent this quick update to our church prayer chain:
The nurse just gave us a report. The white count did go up this morning! It’s a 1.1 from .7!!!! (Crazy to be excited about a high still low white count!) He is having no pain right now! They were allowed to give tramadol with Benadryl and that helped! Ruth Stayte (from Florida) actually texted me about the antihistamine tip and I showed the nurse and she asked the doctor and he said yes! Praise Him for Great timing and wonderful guidance!!! Waiting to hear from the team if he stays or goes home today. Thank you for your prayers and concern for us!!! Pastor sent us this verse and it’s perfect:
Isaiah 38:5b, “…Thus saith the LORD, the God…I have heard thy prayer, I have seen thy tears…”.
Very thankful!
9:30 Dr. Saharia said Kevin needs one more shot today and then can be released to go home! He said he just needs to be home! Especially now that all those tests have been seen and are negative…everything is ruled out that they were concerned with. He does have that parainfluenza and is really recovering fine. Hardly any symptoms just those side effects from the shots. Recovery Chair here he comes!
December 5, 2017 The Horrible. Terrible. Awful Evening!
So far the nurse mentioned in way as a bummer that his wbc was even lower than two days ago. They are .73 yesterday .9 Sunday .8. This was earlier like around 8 am. I got ready. Used my wipes to clean the surfaces of the room and leave a nice citrus smell. And it’s like 10 and up until this very point only a box of masks was on the outside ledge of the door and a hand written sign that said wear a mask for neutropenic conditions. Just now. Someone opened the door to “hang” what I know is that next level thing which holds gowns and masks and gloves. Nothing said to me. Just an attendant. Maybe I should peek out there.
At 6 ish the nurse gave Tylenol for 99.8
I only know fever part from the front door report given to us between nurses at shift change and because we were awake! I kind of looked over at Kevin because it was a shock to me. I mean he was awake and looking at his phone. But I missed that dose and am in the room! Lol! Must have been sleeping good … and the door drama was just that. Drama. The actual door hanger was finally delivered from the other day so no more make shift signs and boxes. It’s an organized box holder that the container store would marvel at.
The NP Kimberly came in. He can’t go home. They think and are checking for a possible secondary cause along with parainfluenza. She said it could be cmv but they aren’t sure. Waiting on that result. It takes a few days. So. Kev was + for cmv and donor was too and I asked once he’s had it can he get it again. She said yes. But who knows. For now. Stay put. And it’s critical to the young and transplant patients. Like we are where we need to be. It’s good that he isn’t out and not realizing he has this because it seems to me that the symptoms can kind of go unnoticed until it reaches a critical point. They explained it like how you can get mono (ebv) and not know you even ever had it. Also I’m reminded of our hospital cycle. It starts out all hype and what!?! Then finally settles down. So I’m not jumping or nearing the edge over what could this be. Because we are right where we need to be for whatever it decides to be. Pep talking myself!
Around 4 he was trying to nap and he just couldn’t. His bones were hurting. So the nurse gave Tylenol. He’s just been quiet today. He watched PSG get beat:( That could cause bone ache but also those shots to help boost white counts. He had his third one today.
Samantha NP from Dr. Galati stopped in but I missed her because I was down delivering our dirty laundry to Tiff & Bailey “drive by all things needed at our service!” Babies can’t be on this floor. No one probably would want to be so drive by is the way to go. Good thing she’s in midtown!
They tented Kevin for a Pentamidine Treatment. I asked the tech all kinds of questions and really wasn’t completely satisfied with his responses. He said Kevin had this before. I asked when? And he just didn’t answer. But I had to leave so I went ahead and grabbed dinner in the cafeteria. I could have cried down there and was close but got some perfectly timed texts and verses and closed the google window I had opened. (!) The new coordinator yesterday said DONT USE DR GOOGLE WEB MD NONE OF THOSE! Lol! She said email her anytime.
I got back up to the floor and asked who ordered it and what is it used for to our nurse:) (Tabitha) And the nurse just explained it really well! Then confirmed it with her charge nurse. Liver team ordered it. So they had to stop the antifungal meds (Valcyte) cause those make his counts low. But they want the effects of those without making the counts low so this tent thing is once a month treatment! And fights preventatively stuff like pneumonia etc Light. Bulb. Whew. And I’m pretty sure Debbie mentioned this in the whirlwind green binder talk yesterday but new words don’t stick. And when she said inhaler I imagined an albuterol hand held one. Not the bubble boy tent!
The entire rest of the day was what I call stress on a stick or absolutely horrible. Terrible. Awful. But by 11 pm we both went to bed! Basically his body was twitching from pain from those neupogen shots to increase wbc. Add flu and you just don’t know what is the culprit. Dismiss and say he’s achy from flu but as he asked me to massage his back he just was warm to the touch plus could not find a comfortable position. And absolute real sharp pounding bone wrenching pain. He was suffering silently. Before shift change the nurse did give him Tylenol to try to help with it and after shift change it just heightened. We did get the same nurse from the night before so she knew us a little. Kevin did let me go find her to ask her to call for something. And it was early enough that we wouldn’t be waking any NP or doctors. I say early it was 8 to 9 ish. The NP she called wasn’t comfortable ordering anything because of how newly transplanted he is. Everything we knew before transplant is off the list kind of for pain management. And in my head I don’t even think I was wanting pain meds for him just wanted to let them know what was happening and is this normal and what could help. I’m thinking chicken noodle soup treatments! But he didn’t even eat his dinner. One bite was all. It was bad. I knew all day he just wasn’t himself and it just got worse. So there was a moment when I’m praying and crying in the corner and the nurse walked in and gave me a hug! I told her she just caught me at a bad time. And hey! It’s all happening to Kevin! She kept us informed every step of the way. She was texting and calling the doctor. Finally she reached him. He was in the operating room. But he took the call. God’s beautiful timing to because I was reaching out to Ruth and she had just sent this text “What about this? “Neupogen helps the body make more white blood cells by stimulating the immune system, which also creates histamines. So your doctor also may recommend an antihistamine such as Claritin (chemical name: loratadine) – NOT Claritin-D – to ease bone pain caused by Neupogen.” And the nurse was able to ask the doctor if along with pain med could he take an antihistamine. And he did! So Kevin was given tramadol then Benadryl and we dropped in bed. In the middle of this wonderful Rebekah Pool had Tiff’s treats delivered! How sweet was that timing! So we stress ate cookies waiting for the orders. And by we I mean me. But there were enough to share so we could offer them to the staff as they came through with updates! It was the sweetest worst time ever! Lol!
I sent this prayer request to the church prayer ladies and to our pastors:
Prayer Request for Kevin Troutman.
He’s been in Methodist Hospital since Saturday. Fever and “parainfluenza” are the official diagnosis with a very low white blood cell count. The shots they gave over the last three days to help increase the counts are now affecting him. He is in pain and not really eating well, and we are asking for prayer over his entire body that everything would settle down. Praisefully he isn’t showing signs of rejection but because of the delicate low counts he is isolated and being treated with great caution. And in pain:(
These verses came to my heart to intercede for Kevin. Please ask for His guidance and way since we don’t know what to do.
“I will instruct thee and teach thee in the way which thou shalt go: I will guide thee with mine eye.” Psalms 32:8
“O our God, wilt thou not judge them? for we have no might against this great company that cometh against us; neither know we what to do: but our eyes are upon thee.”
2 Chronicles 20:12
God Bless You and Thank You,
Beth & Keith
I am writing this at 6:30 am Wednesday and we both slept straight through the night! Very much praising the Lord for Great sleep and great Care over Kevin! His timing is perfect. Poor Grant tried to deliver our clean clothes downstairs after his basketball playing Tuesday night and I cried to him saying it just wasn’t a good time to leave. Kevin looked at me like go but I couldn’t. And sure enough the text from Ruth came right after and then the nurse walked in and I was reading it to her and she even had to read it herself! He kept me in the room to show that. He guided and showed us the way exactly like we asked!
Also in all of this crazy the portal updates every night for us with the day’s tests that are back. And the cmv and ebv test returns populated the portal. So in all the crazy I asked the nurse to see if it meant nothing detected like it said or was there another report they are waiting for. She said after checking later it looked legit! Can’t wait to ask the team this later. To me that means no cmv or ebv going on. Will wait for absolute doctor official though!
Dec 4, 2017 Monday
Kevin ran a fever last night. So we will see what the numbers look like. He does have a sore throat but is up eating breakfast. I walked down to the Starbucks in the lobby because it’s open later today and got him so good hot tea!
Dr. Saharia popped in. (I said hi from my dad to him!) His white count went from .8 to .99 so another neupogean shot today and one tomorrow. |operative word there: tomorrow| bummer… he did run fever last night so we didn’t have the highest of hopes. He’s showering. Ate breakfast. Little sore throat. They aren’t worried about anything but the counts.
We met a new coordinator. She hopped in. Educated us with a new Methodist Binder. She is the post Liver coordinator. He will have labs on Mondays at Woodlands Methodist and labs and clinic visit on Thursday’s at Fannin Methodist. It was a whirlwind but very informative. Very similar information compared to Ochsner. I already read the entire notebook. I told Kevin he could next. I was waiting to hear his classic two year old reply: “I said no mama!” Can you believe he lived to this day telling me that! Lol! We quote it all the time. If anyone can get away with it it would be Kev! Cute enough to stop strangers in their tracks when he displayed his poochy lip! Anyway. Tiffany brought dinner to the lobby! Great escape! I got a break from wearing the mask and Kevin got to wear one! We are loving the transplant floor. Each person who walks in that door is just born to bless. Goodness are they called for what they do! I know I didn’t think I could enter a hospital again and I wanted to be done and then I get here and see how well they treat Kevin and see how well he takes everything and how much right now he needs this place, and I am right back to making the most of it and completely thankful!
Dec 3, 2017 Sunday
Dr. Galati and Samantha NP rotated through. He called me out. Said I needed a mask on! Ultrasound looked good. The white count is low and could be from this Virus or from the medications. Dr. Saharia wants cellcept stopped. Ruling out other infections and watching cultures. If all looks good white count wise he’s for Kevin recovering at home as long as he eats and drinks plenty of fluids. So as early as tomorrow.
No Visitors he’s neutropenic which means his white count is even lower that it was yesterday and that was low.
He ran fever last night.
NP for transplants was just in. Janine Hyden. She gave me her card. She was great. Informative! She said we will get a post transplant coordinator. Also gave me the number for after hours.
713-441-5451
Bummer is his white count is lower. It’s .8 so no visitors.
Checking for cmv and evb because of low count. And holding cellcept and Valcyte and Bactrim.
Neutropenic so gowns and masks on those coming in. Mask on us if we go in the hall
Doppler looked good. So ultrasound from yesterday was fine. Need to 100% ask one of the doctors if the flow looked good.
Kevin asked to shower so that’s a good sign.
They drew more blood to test for cmv and Evb
***My app for my blog hasn’t worked for two weeks now! Cole checked it on the pc and it’s fine only I didn’t grab mine. He said give it a few weeks for them to get the bugs out of the latest update. The blog app going down was perfect timing. At least I got to update the most important part of transplant!
Dec 2, 2017 Saturday
10:30 pm 99.7 and freezing Even though the room was hot. So he’s creeping up again on the temp. He also has a headache. Only Tylenol since the ordered aren’t in. I’ve rubbed his head several times. Poor guy. Nurse also hung zosyn antibiotic. Earlier a second antibiotic was ordered and the NP said that Dr. Galati shot that one down.
7:00 in Dunn 409 no meds ordered but I brought Home meds and the nurse said the orders were to take home meds but only prograff. Glad I brought them:) I asked about that later now that he’s post transplant so we bring Home meds with us and basically she said no but it’s what they did today.
6:00 I asked for food for Kevin. Keith said something about a tray being ordered. He’s had no food and is finally hungry. Waiting on transport so by the time he gets to his room the service will be closed. The nurse came in and we couldn’t understand her. I said two hours ago they said they could order him a tray. She said she could get him a sandwich. So we were like yes. Bring food.
5:00 The NP and pharmacist came through. NP was from infectious disease I think. They were screening for sepsis. Tiff says all the hospitals check for that. The pharmacist went over meds. We had the blue card which makes that so easy.
4:00 Me and Cal made it with packed bags. All the info is from text messages from Keith! He did good.
3:45 Kev just went to ultrasound. I am waiting in room
3:30 Bro. Pope just left
3:00 Galati just came back:
-Will admit under transplant surgeon Saharia(sp?)
-He is on call this weekend
-He and Samantha will be by later
-Blood work not out of ordinary
-White blood count a little low, but could just be meds
-I told him that will not be a good enough answer for you… he said just chalk it up to high fever something….:)
2:30 Dr. Galati just came in :). He is checking labs now
1:15 Chest X-ray… of course… following protocol 🙂
Or just paying out the machine 🙂
1:00 They got him in an evaluation room now… looks like they fast tracked him ahead of all the others, even a chest pain lady…We are in ER exam room #41
12:30 checked in with triage and waiting
11:30 Keith spoke with on call coordinator and that guy said get to the ER. BTW the temp to call with is 100.4. Anything over that they want to know.
10:00 am 100.4 Keith searched the house for the transplant notebook from last year! We have all things Ochsner and all things Galati here but no after hours call number. I told him what quadrant of the house to look in and it’s called no man’s land. In the study. He found a couple of binders! One had Houston Methodist Transplant Center and he made the call. And asked for the on call coordinator to call him back.
8:30am Fever 99.5 not feeling well. Ate half a piece of toast. Took meds. Went to bed last night with fioricet headache meds.
Nov 30, 2017 Thursday
spoke with Dr. Galati. He would like to increase the Cellcept to 1000 mg AM and 1000mg PM. Do you need a new prescription, or double up on the meds you have?
Labs all look good!
November 15, 2017
Dr. Galati & Jane This is the first Houston visit
We found out Jane will still be our coordinator in Houston! We had a great visit. Jane cried at least twice seeing Kevin! Dr. Galati examined Kevin and asked questions that didn’t require “good” from Kevin! I didn’t record this one so I’m going on memory and my notes. Not to mention how many times I’ve tried to update and my blog page is being so persnickety.
About the stent he thinks it’s a good idea to keep the follow up appointment with the Ochsner doctor who performed it all the while pouting out how important the hepatic artery is. It’s the life blood to the liver! If flow isn’t good he could get schlerosing cholangitis. And not the kind he just battled. He said he got that the good old fashioned way: primary schlerosing cholangitis. But secondary schlerosing cholangitis from low flow through that artery and in turn the liver and that is all I’m writing here. Never want to think about that again! The images didn’t actually come so he couldn’t see what we thought we were picking up the day we grabbed medical records. If he could have seen how open it is maybe he wouldn’t have looked so concerned… No wonder it only took 15 minutes to get those before we left New Orleans. I don’t think anything much “film” wise was on there. But Jane said she would get them! She said she is tight with Ochsner now! She’s so wonderful! We are so thankful for this team! He was ready to send Kevin that moment for an ultrasound. But he will get one in the next month to set a baseline.
Labs in two weeks.
Dr. Galati gave Kevin a routine to work up to and encouraged exercise like walking 30 minutes two times a day. In a month or so he can add weights to the walk like small hand ones. Then lead up to a ten pound one in a back pack to walk with. He called it something like a slow roll out of the two year sick crawl. He wants him to take his time.
We mentioned the back left side pain Kevin was having and it didn’t hardly register with him. He chalked it up to recovery stuff. My words. He saw the blue card to see his medications and when he saw the pain med listed he said don’t take that! He said start with Tylenol. Kevin hasn’t had pain in weeks except for those “growing” pains from all things settling down in there. Most people I read after said it felt like a bomb went off inside and scar tissues would just pop and adjust as they stretched and got more mobile. Keith told me not to google it. But I did. I had to know what they Transplant community said about back left side pain. We also had him out of his routine. Packing. Moving. The drive back to Houston!
Keith is wanting to plan a trip for the boys for the end of May and Jane said as long as Kevin is doing well to go for it!
Thursday November 9, 2017
2 months and 3 days since transplant.
3 months and 16 days since we left Houston.
We were officially released today from Ochsner to HMH! (Houston Methodist Hospital) The day we’ve waited for is today! And I woke up thinking now how can I ask what I already asked on Monday without saying the same thing: so when are we released? What has to happen before we are released? What’s the timeline here? So today I sent a note in the portal with this: what is next? We had labs twice this week and an appointment in Houston for Wednesday that I can cancel if needed. And I got a call from Nancy!!! She said Dr. Tyson was just waiting to speak to Dr. Galati. And that she has called all week. I said I can call and let someone know if that would help?:) We basically put out an APB on that guy. Dr. Tyson even left her cell phone for him to call on. Whew! (Now if I could only know what they said!)
Keith, Cole and Caleigh were trying to decide if they were coming this weekend. Caleigh is done with marching band so no more leaving Houston at 7 pm for a 6 hour drive! Keith said they would come either way. So that was the best. I think I needed to hear that! We’ve had the best trickle of company, calls, texts, cards, packages, and have lived for each moment! It’s filled our days! When Nancy called and said that the two doctors have spoken and we are free I was like well what do we do? Do we need y’all to sign something!?! She explained how to get the “films” and then said she was off tomorrow but she can be reached always in the portal!
Keith and I had already been talking and I called him first because Kevin had fallen asleep after morning meds and when he answered I couldn’t even get the words out. He went straight to what is wrong and thought something terrible had happened. No. The complete opposite. Something Wonderful Has Happened! I cried and cried through telling him that we are released. The BEST was telling Kevin! I was a new creature by then! You can guess the look on his face: gentle quiet yet priceless expression of perhaps Christmas morning anticipation. Happy. He was up and showered and we were out the door for medical records!
I cannot even begin to tell you the simplification of the film retrieval. I was thinking back too much on that medical records floor in Scurlock tower and let fear and trepidation take over me! There was a bad lady in there one time. I’m sure I blogged about it! We went up to the second floor at Ochsner and into the waiting room and there was a phone on the wall. You pick it up. It rings the records. They get your name and info. Then she said there is a clip board with Medical release to fill out and she would be out in 15 minutes! We were willing to come back tomorrow because Kevin left his wallet. She asked if I was his mom. I said yes but he’s twenty. She said that’s fine! She would have me sign the release. We barely had time to buy TShirts! Oh yes. We ain’t leaving this place without the T-SHIRT!
We bought Great TShirts: “Donate Dat” “Donate Life It’s Always in Season” “Transplant Dat” “Team Ochsner” We went back up to the second floor and in no time a lady came out with our cd.
And that was it.
It was wonderful and emotional all wrapped up together. I mean. How do you just walk away from the place that gave us through His Great leading new life for Kevin. I don’t even have words.
Ok well I have a few words! You can’t just walk away. We never really will. This place is forever in our hearts and being. We can hear Ochsner. Literally when you enter the atrium there is a terrific friendly welcoming lady. Always welcoming. Always happy. Everyday. Always the same. Happy. Welcoming! The place from the first day that welcomed us with God’s rainbow over it. The very first day we had appointments for Kevin to be evaluated the rainbow was over the hospital. I took pictures! And I don’t even need pictures because it’s etched in my mind! Matter of fact the pictures don’t do it justice because of all the raindrops on the windshield. Each greeter, cafeteria and coffee staff, administrator, NP, nurse, surgeon, doctor we are forever grateful for. Just forever thankful. They chose this life of all things medical and are embedded in it from parking to bedside! And how do you just walk away. And to know that a precious donor family chose to donate their loved ones organs. To donate life. I stand in awe. Absolute awe. (Not to mention also in shivering tears) A liver was brought into this facility. Arrived on September 6 and made its way to the second floor operating room and into my son by His guiding wonderful hands and through poured out wisdom and knowledge and into two amazing sets of surgeon’s hands: Dr. Sonnier and Dr. Carmody. “I will praise thee; for I am fearfully and wonderfully made: marvellous are thy works; and that my soul knoweth right well.” Psalms 139:14
We are so thankful. We thank God with JOY for Ochsner Medical. “I thank my God upon every remembrance of you, Always in every prayer of mine for you all making request with joy,” I have prayer cards. I think I’ve called them my Jericho cards before when I passed them out in Sunday School back in the day and wanted my ladies prayer requests and even said if you don’t write something I will make something up! I meant will find a verse to pray for you! And that verse in Philippians is like a bright shining illumination of happiness and joy. I was praying through my cards during Kevin’s surgery and wrote 9-6-17 in my chicken scratch on the top. And now I might just know what Bro. White meant when he would say: now someone hold my mules! When I get to that prayer card each day and see that chicken scratch date it stops my heart all the while infusing it with absolute joy unspeakable! My heart has a happy fit! So we will pack and walk away from New Orleans this weekend but will thank Him everyday in our walk with Him for all it has meant to us! It will be impossible not to.
November 6, 2017 Monday
Labs this morning. Dr. Tyson said last week: labs Monday. Only we never saw an appointment scheduled for them and Saturday when we realized it, messaged Nancy. We went in by faith because it’s what we know to do and sure enough Nancy thought she put the order in but it wasn’t there. It was a quick fix and almost no wait time but in that waiting room I heard and eyed 3 different people coughing! We couldn’t get out of there fast enough! He already picked up one virus so far this recovery and was hospitalized for it and ain’t no way we want to go through that again. I stopped short of interviewing each cougher once Kevin slipped back for labs but desperately wanted to. One woman sucked on an inhaler after so I’m thinking she was not contagious. But the other two??? We are waiting on a timeline. They should call with his Tac level or at least populate the portal with the lab results and I will follow with a call or message about what’s next. Keith and Cole are ready to come this weekend or the next and help load the heavy stuff.
As I was typing the above I had this message in the test results:
“Decrease cellcept to 500mg twice a day as WBC count trending down and increase tacro to 4mg in morn and 3mg in evening. Repeat labs Wednesday.” Those were actually reviewed by Dr. Tyson and it was last weeks labs she made the note on today. So we will still have new results from this morning. They did prepare us for this medication change up! The Hepatology doctor handles it a little bit different than the surgeons. So glad for the cellcept decrease. Both cellcept and tacro are antirejection meds. Cellcept was 4 pills both am and pm. So. Huge decrease! Those capsules are 250 mg each. Tacro (same as prograff) are only 1 mg capsules each. I don’t do numbers. Even the easy ones stump me! Lol!
So I’m thinking Dr. Tyson just wants Kevin’s labs stable before handing us off. I know we have an appointment on the books in Houston for next Wednesday the 15th but that doesn’t mean we will be released. It may mean things will just have to wait another week. But what do I know. I know by this Wednesday Caleigh will have completed her entire marching band season. And I missed it all 😦 Harvey changed so much of it but other than Keith and my great friend Shawn who videoed it for me I would have missed it completely! Keith’s video was good but Shawn’s was perfect! I told Keith she zoomed in on Caleigh’s section! I had no idea where she was. I’m not musically inclined. They are all so tiny on the field! We got to see Shawn again yesterday and cross off something on our NOLA bucket list: cross the Lake Ponchartrain Causeway and actually see that gigantic lake! It gets us out of the apartment and free from coughers! That thing is 25 miles across! We finally did it! We met up with Shawn on her way back from the beach! One crazy question about that causeway we are curious because crossing from NOLA to Mandeville it was free. Returning we had to have a tag (which we have a Texas ez tag) but had to pay $5. Which is fine. But why only one way:) We never did it before transplant because of the obvious. If we were to get the call we sometimes had to be 10 to 30 minutes away. It felt great to have that freedom. It’s weird but after living so long with phone charged and on loud and ready to go I have to remind myself we are done with that! Praise God for such a wonderful blessing!
3:30 pm Nancy called to go over what medication changes. I reminded her those were from labs on 11/2 and not today’s labs 11/6. She said she would point that out to Dr. Tyson. She said she is meticulous and the key word with her is “trending!” She wants to speak to Dr. Galati herself and make sure he is ready and willing for this transfer. I asked about a timeline and she is getting with her.
November 2, 2017
Astros Won The World Series! Now we can sleep!
Today was labs and Dr. Tyson. She’s wonderful! She was SOOOO happy to see Kevin. She welcomed him to the “other side!” She said see I told you I thought we could help you! And that she did. We met her at evaluation in July and the last time we saw her was Aug 31 before the transplant. (My first impression at evaluation was how very aggressive she was. Because she said then to like stop taking all meds! Then he would be sick enough for transplant! I was horrified! But it made sense. But then I was horrified because I knew what that meant for Kevin) She went over the list of medications and when we will stop some and which ones are for life. Basically the anti rejection meds and the aspirin are for life. 2 antirejection because of his autoimmune issues. Dosage on anti rejection will change after 6 months to a year. (Cellcept drop to 500 from 1000 by then) She wants his Tac level at 8 for 6 months to a year to stay on top of the autoimmune stuff. (Last labs it had dropped to 3) He will finish Bactrim March 5. Valcyte Dec 5. Urso is for now while his bilirubin is just a tiny bit elevated. I’m talking tenths. Not like pretransplant days! Plavix for one month and with that continue Pepcid while taking Plavix. It was for while on steroid too. Vitamin D and Aquadeks continue while his system is adjusting but should be able to roll off those and they will recheck those before taking him off.
The ultrasound Tuesday said there was still moderate ascites and she said she didn’t believe it after examining him. She’s not too worried about it and won’t put him back on lasix because she feels it will work itself out normally. She asked if he was feeling it like hard to breath and such. He hasn’t noticed any but we have been so tired getting those Astros this victory! She reminded us that the Saints Won the super bowl after Katrina!
Vascular. While that doctor on Tuesday said follow up in 3 months he told us it could be done in Houston. But then yesterday our portal populated an appointment for Jan 30. So she is going to see if that was just the coordinator reading the notes or if he changed his mind. We can make it work if we have to by hopping over.
We discussed his blood pressure. The transplant notebook says anything below 130/90 is a good read. He’s been above that lately. I mean it could be those Stros but she said ultimately with prograff increasing and his body adjusting to anti rejection meds for now keep watching this. 140/90 is fine but if it’s over we need to communicate because she may add something to help.
The pathology report. The team meets every Thursday and while we started this topic Nancy peeked in and said “they” want him to see hematology and get a pet Scan. Dr. Tyson had just said that same thing. While they can’t confirm anything she feels since it’s been a while and because of how many infections he had between last year’s bone marrow biopsy and transplant it would help to keep an eye on this. She thinks have this done in Houston so that center can keep the close eye on it. It depends on how quickly it can be scheduled. So that part could happen here if it’s soon. Otherwise she asked for Dr. Galati’s number and will call him and get his thoughts on hematology and transferring Kevin back to his care and when. (!) I told her we had a tentative appointment on Nov 15 and it could be moved. They are flexible.
For now labs on Monday. We hugged her and thanked her because we are so thankful for all she did and this entire Ochsner staff. We may or may not see her again but she said she wants to hear from Kevin along the way for him to drop them a note. She also pushed Tulane and then they could really keep an eye on him! Lol! I’m sure Nancy will be calling to tie up these loose ends. I think I wanted to hear a date when we can move home today but I’m sure we will know once all the teams here and in Houston have communicated and are ready for hand off. Kevin was wearing “His Grace His Love His Church” T-shirt and she saw that and said God is Good All The Time! Yes He Is!
11:50 Michelle a nurse for Ochsner called and already has Kevin a hematology appointment for today at 1:40 with Dr. Carter Davis. That works!
1:40 Dr. Carter hematology. Pasting the text to Keith:
The hematology doctor was excellent. He explained the pathology clearly. He said he’s not surprised by the lymphocytes in the old liver pathology report because of Kevin’s AIH. Also the pathology of old liver those lymphocytes are not “clone” cells which would be the case if it were lymphoma or cancer blood cells. Because they were all different ones that equals not cancer. He could reassure us also based on the ct scans he’s had. He read over Kevin’s case and seemed very familiar with it for this short of notice. He will report to the liver team that the pathology report has nothing that bothers him. The final test came back Oct 30. One test result that didn’t come back the T cell something didn’t even need to be looked at. However, he did caution us on PTLD. Post. Transplant. Lymphoproliferative. Disorder. While very rare, because of the immunosuppressant meds he takes can in rare cases cause that and somehow that’s related to Epstein Barre and that can cause lymphoma. All this is my words. Can’t fight infections so you get that. Almost everyone has had it. Symptoms tired. Unexplained weight loss. Enlarged lymph nodes. He was reassured and wanted to reassure us. The word of the word of the visit. Reassured. He wanted to be sure we understood because he was worried that we were worried because we were sent to the cancer building in one day! But. We knew why we were going to the cancer building. We’ve been to the cancer building in Houston to see that hematologist. And. We wanted answers to the “concerning” pathology report. So all in all a huge relief!
Tuesday October 31, 2017
7:15 am ultrasound
9:15 vascular follow up
Dr. Sternbergh was completely pleased with the ultrasound. He said it’s really what he expected and that 2 out of 3 things were just excellent. He didn’t go into detail about that third one because I think it was complicated but still good. He isn’t expecting any problems. He will pass this on to the Hepatology team and said follow up in Houston with an ultrasound in 3 months. I asked him to show Kevin the images he showed us after the procedure last week. I knew I couldn’t do it justice describing it to Kevin. Absolutely amazing. He has him on plavix for one month along with aspirin. He said most likely continue baby aspirin for life. He was already on that since day one of transplant. I have a list of medications to ask when to stop taking what. But that’s for Thursday.
Monday October 30
Fasting labs this morning and Nancy called later that his Tac level is low. It’s 3.5 so we are adding prograf. From 2 and 2 am and pm to 3 and 3 am and pm. We changed the blue card. She said labs again Thursday plus that’s the day we see Dr. Tyson hepatologist. (For the record the iPhone never recognizes that doctor term. It makes me insane. We’ve seen Hepatology for 6 years. When will it learn!)
Also we need to call Briova. They left a message on our home phone. The insurance mail order pharmacy company we use for the anti rejection meds. Keith needs many prayers for dealing with the travel department of our insurance. He spent an entire day in frustration with them. They “lost” one claim for reimbursement and denied another. Only they never reached out to tell us of either. They had the original copies so we got those replaced and are starting again. They will not accept a fax and will not give us an email. All I can say is they better be glad they get Keith. When we get released from here and if we are still getting the run around I will find the travel department and walk in with the documents wherever they are located! Have time. Will travel. If they approved all of this before we even considered coming here and they know we are here and have already reimbursed the three day evaluation stay I have no idea why they seem to be deflecting the rest of the monthly reimbursements. I have said it over and over I just want to know how stuff works. Behind the scenes. From hospital administration and “waiting for a bed” to insurance claims! There has to be a common sense approach.
October 27, 2017
Kevin is doing great from the procedure Monday! He never even needed pain meds! He’s probably like meh. I’ve had worse! So we basically stayed low until yesterday. We “drove” to a place to walk! Kevin was like so we are driving to walk. Well. Yes. I’ve been wanting to walk the Mississippi Levee. I could see people on it from every window view we had when in the hospital. I told Kevin then we are gonna walk that Levee someday. Someday yesterday! (Parked close to the Huey P Long Bridge and walked to it and back to the car. Just enough for Kevin!) We are also finally connecting our little area with the rest of the place. Like who knew I’ve been driving to Kenner! The airport is in Kenner! We live 10 minutes from that. People say they landed. We leave the apartment just in time for them to be curbside! The River Road that runs behind the hospital also took us the “back way” to the French Quarter yesterday. We had nothing but time on a beautiful fall day so we went out! Magazine Street is basically 6 miles of Old Town Spring btw! We actually had seen some paintings before on a trip down there in Jackson Square where the artists dwell around the rod iron fence and thought we might get one to remember our time here. Well. Yesterday we didn’t find anything but the weird ones. And a $575 tuba one. So. Maybe another day.
Keith and Caleigh took in Klein Cain’s spring drama last night. It was daddy daughter date night. Dinner and the theatre! Even spelled “re” on their website to get tickets. He said the play bill is in a link. They don’t hand them out anymore. Wat!? (Really people! Does everything require a link! One of these days that World Wide Web is gonna fall out of the sky! I can see it now: what part are you playing to clean up the web! Politicians will run on this platform one day. Mark my words! It’s got to be getting close to a point of NO MORE! The Web is Full) And most parents just dropped off their kids because he said when they walked out there was what looked like a carpool line for pick up! Well. We aren’t those parents! Kevin and I always loved seeing those productions! He didn’t even know about it until Caleigh came in and said they got to see a sneak peek in class and they HAD to go because she HAD to see how it ended!
Keith is hosting several of Caleigh’s friends again tonight. This time they are getting costumes ready for tomorrow’s Fall Festival at our church. The girls are all pieces of fruit. Me personally thinks Keith is a basket case for letting Caleigh talk him into this so he can be the “basket!” He never reads my page! He’ll never know I called him that… He is trying to one up me on the mom status too. He has Ruth’s homemade sugar cookie dough ready! Like it isn’t Christmas!? He said just in case! Ummm throw them in the pool just in case don’t add another layer to clean up! (Mind you Cole already said the last time he was home from grad school this house needs a mom! Lol!) One good thing about having friends over is they have to clean then! He called last night to boast about that too! Said all it took was a little effort! So Cole will be happy when he walks in today. Only. Maybe not. He doesn’t know about the friends Caleigh is having over…yet.
Might as well throw this one in while I’m updating the home scene. We’ve gotten one letter from our subdivision since I’ve been here because of the crazy weedy back yard! All that has been fixed now. The weeds are gone. They were as high as we’ve ever let them get. Keith even has some tool to snip the palm tree fronds with. And you know how close I was to writing that committee a letter! If they only knew what was going on!?! The. Very. Idea! And I’m like which neighbor turned us in?! Or how did they see our back yard!?! Maybe drones are doing the checks theses days in Gleannloch Farms! I begged for a picture. Keith NEVER sent one. Smart. Man.
Shawn Frost is passing through on her way to Florida this weekend so we are excited for that visit!!!
Next week Kevin has fasting labs Monday morning (the usual), an ultrasound, vascular follow up appointment with Dr. Sternbergh on Tuesday, and we see Dr. Tyson the hepatologist on Thursday for the first time since transplant! She is now who follows his medication (Tac) levels. And most importantly she will release us to the Houston team! That’s how close we are to going home! I’ve even turned in the move out date form because if you don’t you pay another month’s rent. The official move out date is BLACK FRIDAY! But I’m hoping to be released mid November. When we were deciding to do one more month here Kevin was only about 4 weeks post transplant and we just didn’t know. He used the transplant team here to help guide our decision to stay one more month in the apartment and sure enough had we decided not to renew the day of his procedure last week we would have no place to go. Well. A hotel or something but we praise Him for directing us each step of this Red Sea Road! (That reference is for you Heather!)
October 23, 2017
Arteriogram this morning. Dr. Sternbergh is doing the procedure. They said the actual procedure should be about an hour to an hour and a half and the recovery is 4-6 hours. Keith flew over to wait with me.
9:45 am Anesthesia was just in. Kevin signed consents. He said it could still be about an hour. The nurses walking me back said what a tough kid he is. He didn’t even flinch when they started his IV. (Tell me something I don’t already know!)
1:00 pm they just rolled him back.
2:15 Dr. Came out. He said the procedure could not have gone better!!! You should have seen the narrowing! He was like Dr. Brandt with Bailey and had his phone out showing pictures! Oh. My. Goodness. It was practically closed. Now it’s GOOD and open!!! He placed a 5mm stent. He will be good for life!!! He said his bigger artery made him able to do that. Most stents are smaller. Praise the Lord!!!!
3:00 Keith and I are tucked away in the hospital bed “parking lot.” Kevin has to be flat on his back for recovery until 8:30 pm. They said he can eat whatever he wants but they will tilt the bed up. He is resting now and maybe will sleep through. We have the lights out but we can hear the neighbors through the curtain. And we pretty much know their personal history. Hashtag: where’s hippa now?
9:00 We are back at the apartment! Every single nurse and dr and etc told us how strong Kevin is and what an amazing job he did through all of this! No complaints. Just steady. Maybe now we have turned that page! Countdown to Home. Ultrasound next week with follow up to vascular is what is next. Well what’s actually next is feed the boy. We are ready too. With Keith here and his love for walking up and down every aisle of the grocery store we happened up on my favorite Monjunis pomidoro sauce! Wat!?! All this time I had that at my fingertips! Usually we have to go home and smuggle back jars or get it for Christmas. Kevin doesn’t love spaghetti but it’s my favorite dish ever! I would ask for it for my last meal if I were ever in that position! But he likes Alfredo so he gets that. The more Monjunis for me… yum.
*blue card update. He added Plavix for short term. We need to add that to the blue card. We picked up the script. He starts it tomorrow. They gave him a dose today.
October 18, 2017
Kevin had labs on Monday and two clinic visits yesterday. Labs are the best yet. Tiffany and Bailey got to go with us to clinic. Bailey listens so good when the doctors come in and talk!
Vascular: Dr. Sternbergh went over the CTA results. Kevin does need a procedure next week to open up that hepatic artery where the new liver was connected. The ultrasounds have been showing the “turbulent” images around that connection and they have been watching it. The last ultrasound in the hospital last week caused them to order the CTA to get a clearer picture. That showed “short segment of high-grade stenosis of the hepatic artery presumably at the anastomosis.” Dr. Carmody sketched us a picture of the smaller and larger arteries connecting saying the flow does change here last week during the “observation virus” hospital stay. Sometimes it’s nothing. Keith explained it with oil field pipes and images:) The vascular doctor we saw yesterday is the one who does all the transplant endovascular procedures. He said while it’s not a completely common thing it does happen in 5-7% of transplants. It’s totally treatable. He said his job is all about keeping the best flow and currently Kevin’s artery has “severe narrowing.” Friday his office will call us with the outpatient procedure time for Monday. They will go into the top of the leg. We pointed out the soreness from transplant and he said they will check the area with ultrasound before using it. If there is any doubt they will use the other side. The arteriogram will give them a picture of the narrowing and how best to open it: balloon or stent. If he uses a stent it will be in for life. He said it’s not one of those that gets replaced. Kevin does have an unusual anatomical artery there but he said it’s just the way he was born and had nothing to do with the transplant but it does explain how he has to get to the area. (Not that I totally get that. But it’s Kevin so of course he’s in the 5-7% and was born with that!) He had Kevin sign the consent forms then his nurse came in with a booklet of what to expect and surgical shower gel packets to use before surgery. Nothing to eat or drink after midnight Monday.
Transplant: We then saw Nancy and Dr. Bohorquez one of the transplant surgeons. He looked up the pathology report and said it seems like it’s all settled. I would prefer to hear from Dr. Sonnier on that since he was on rotation when that “lymphoma stuff” was brought up. Just me. Personally. Nancy said Kevin will do the procedure next week. Still Monday labs and take prograff not cellcept. Have a follow up with vascular at 5-7 days from it. After that he is cleared from surgeon visits but has to see Hepatologist. Dr. Tyson is that doctor here. We’ve seen her at evaluation and pretransplant. She then will release us to the Houston team. Not sure if we see her once or twice. She will adjust meds like surgeons have been doing to keep an eye on his levels. Nancy said to go ahead and make an appointment 5 weeks from yesterday for Houston! I’ve already started that first thing this morning! They will not let him go until he’s established there. Even then they keep an eye on the labs until after he’s met with transplant in Houston. So, our days are numbered! I was so excited to hear five weeks from yesterday until I looked at the calendar and that’s the very week of Thanksgiving! I don’t do numbers so I don’t know what I was thinking. I was hoping it would be two weeks! It feels like it will be two weeks! So let me live in those #unrealisticexpectations.
October 12, 2017
5:30 CTA we will get results for this next week. He was back in no time and we packed up and we’re outta there! Home and resting!
3:35 Devon Hopped back in. NP. The CTA is on for today. In about an hour. So NPO for now. His late lunch just arrived so glad he was showering and not eating so we can knock this procedure out then maybe be discharged.
3:00 Dr. Carmody the surgeon who did the transplant came by! He said he saw that Kevin was in. He asked if he could bring by two medical students. Sure! He explained a little more what they may be seeing when they say “turbulent” and drew a picture of Kevin’s huge vein reminding us of the huge liver he removed and the smaller liver with attaching it to a small artery. Small to large equals turbulent flow. I asked him if he wanted to tell them and he smiled and said he didn’t want to be in “surgical denial” and say you weren’t there in the OR there was good flow. Because he said stuff happens in this situation and he didn’t want to say no don’t do anything about it. And this is common. My guest tray was delivered. He seemed awed by that. I was like I’m not leaving the room and miss information coming in that door:) I told him I was taking this to Houston! Let the guests pay for a tray!
3:00 Someone from vascular I didn’t catch her name. She said he had some “elevated velocities” and would talk to the chief vascular doctor (Sturnburg?) and one of two procedures may happen. A CTA where contrast is bolused (spelling?) in through IV and if they see a narrowing of the artery they will use a Cath to open it up much like they do in the heart. I wrote down the word endovascular. It really has nothing to do with why he’s in here and the procedure may not even take place today. If they can get it scheduled tonight they will. They may simply repeat an ultrasound in two weeks.
2:30 NP Devon
He said the ultrasound had one image that he wants the vascular team called in on. Nothing too concerning but he wants their input. “There is a change in the hepatic artery.” They call the image “turbulent” and that is from the flow of blood through it and the waves it generates in the image. He said worse case scenario was a need for another procedure or stent. It is the artery with blood flow to the liver. Could be from edema (swelling) with it compressing and shifting. He studied all the previous ultrasounds. He even gave us the option of not knowing what was next. We were like oh no. We want to know. Knowing is better than not knowing or shock and awe! Because in my mind I can imagine way worse than what he e explained.
11:00 Still in the hospital under observation. The ultrasound that was already scheduled for his one month happened first thing this morning. We’ve seen social worker, NP twice, and surgeon Dr. Marthur. They need to let the magnesium drip in his IV and see that the ultrasound is fine then we should be free to go home. Everything looks fine from yesterday’s CT scan. Random fluid still present from post surgery. They are not concerned about that. Labs are good. They held the cellcept so I need to ask when to restart that. Kevin voiced yesterday just how nice it was to hear them hop in and say the labs look great. They would even explain that they looked for pancreatitis and would tell us what that was (oh how we know but they don’t have to know we know!) and hearing them say no signs of infection brought such relief. Like we didn’t think he would have same old stuff with the new liver but here we are. It’s just so completely weird to be normal. Hydration. Quickly. So he can keep anti rejection meds down. I’m very thankful. One new tidbit we learned the NP said when they say don’t eat or drink before an ultrasound we can ignore it because he’s post transplant and does not have a gallbladder. The gallbladder is what blocks the view and messes with images. Who knew. Kevin told me later he was going to not eat or drink only 4 hours before. 🙂 They called this a “bump” in the road. We have a room with a view of the Mississippi River and the Huey P Long bridge. That never gets old. Now Keith and Caleigh on the other hand… end of the nine weeks. That’s an entirely different story. She needs just one ounce of OCD in her to survive being home with daddy! And she was given zero! No Stress and mediocrity are her bffs! Pray for Keith!
Oct. 11, 2017 Yesterday’s Neurology Today’s ER
Neurology appointment at Baptist Ochsner facility yesterday with Dr. Brandt. She examined him. His question and answer score was 65 and anything over 55 is worth figuring out. My words. So his headaches since they are recurring. Right side. Painful. Long term history. Off and on. No need now to determine triggers because of all the new meds but she gave him two meds for as needed. One he’s used from Dr. Pope called triptipan (?) and the other a nasal spray that has a z in it. And a “free trial” coupon that cost us $113 at the end of the day. Even the pharmacy tech kept running the coupon cause she kept saying free is free!
Currently we are in ER. He was vomiting and nauseous all night:/ :0 I will paste my text thread to Keith cause I’m sure we will just be here for hydration and get those meds in to keep him from rejecting. Can’t take rejection meds if your not keeping stuff down! And the only place he went was to that Baptist hospital!
Thread to KT:
Rough night. Kev was nauseous he thinks from not having enough food in him when he took 8 meds last night. It hit him at 1 am. Then at 3 he asked for more meds for nausea. Label said every 8 hours. But it’s 4mg pills not 8 mg dissolving ones. So at 5 I gave him another one. He was even in his bed. First time to try to sleep on the night back there. By 5:30 he came and got me he had vomited. I had a trash can ready for him earlier cause he asked for one. Poor kid. And it’s time for meds again. He wants a piece of toast.
Vomited again. Can’t take meds. Called Nancy. She’s calling dr. He may have to go in for IV they don’t want him to rehydrate.
Dehydrate
Nancy wants us to get him to ER. Dr said. IV. Needs meds and so I’m rushing to get ready to leave.
Oh my! Call me when you have a minute and things have calmed down. I’ll step out of my meeting…
Ok. I’m trying to think how to get him to ER and park. Was there a valet closer to ER like where you dropped off your mom?
Yes
They have valet there, too.
Ok. No one was there but finally they came. In ER room now
Okay
BP 164/104!
I think that is typical if in pain, or vomiting/nausea??
Yes.
They just said that same thing
Good
I’m not a doctor, but I play one on text message
I only know recently what it should’ve been under 130
He’s got IV in. No fluids yet. Labs drawn. Waiting on dr.
10:25 Inconceivable. CT scan ordered for noon. But before then he needs to drink 2 full cups of CT nasty fluid. Contrast junk.
Do they not understand nausea and vomiting?
I know. Right! Great day! They gave him zofran and pain meds
How bad is the pain?
7
Oh wow! I didn’t realize he was in a lot of pain, too.
11:00 Met Denise the NP from transplant. They may admit him after CT scan or if he feels up to it and all is ok they may discharge him from ER. His labs are excellent. Won’t know anything until after CT scan. He’s sipping the nasty contrast. Almost time for the next cup. BP 138/97
12:15 taken to CT scan
1:00 ER dr said CT scan looked good. Nothing abnormal. Getting with liver transplant team to see what they want to do. We are so tired. Not great service in the room. I have to step close to the door to get service.
3:30 Surgeon Dr. Martur came in w NP Denise. They can’t admit him officially but can keep him under “observation” overnight just to be safe. So we have a room upstairs already they said. He has a bad headache now.
6:00 the Nurse brought his prograff. I am the literal beast and we take that at 8 and 8 so was going in full panic on her for several reasons. He hasn’t eaten anything. We are in here for nausea. Give him anti rejection meds on an empty stomach and he’s gonna be MORE NAUSEOUS! I’m a mom. You are an ER nurse in America! How do you not know that! Also he had a horrible headache. Horrible. So we asked for headache meds who knows how long ago. No orders were in. Finally orders are in and she brings oxycodone. I said that’s not what he takes for a headache. And named the several that he can have. So she went back out and got it. We couldn’t have a nicer nurse but somehow nice today isn’t good enough?! Lol!?
7:00 we got to the transplant step down unit floor. Observation. Just in time for the cafeteria to close. Kevin said he doesn’t want anything so that’s a good thing. They gave him a sandwich in ER to have something before taking meds. He had half of it and a graham cracker. He had enough water to take meds. But no water the rest of the day. Not even a pitcher and glass. I guess cause it’s an ER room no frills. But I just told this floor nurse that I think he’s going to dehydrate in the hospital trying not to dehydrate. He had one IV fluid early this morning. Since then only sips of water with meds. The transport guy got there so he was ready to move Kevin. He asked in the hall if Kevin needed the telemetry. Someone said no. So the transport guy removed the telemetry. I already felt like I was running too much so I hated to tell that guy who touches every elevator button and door handle in this hospital please step away from my son’s incision! Another nurse came bolting in but it was too late. So we made helpless eye contact with each other. I asked Kevin if he noticed and he said why didn’t I say something cause it’s too late now! Lol! The NP for transplant is going to stop by then I’m leaving for a quick trip to grab overnight things. And maybe nourishment for me!
October 9, 2017
Labs were really good! Liver enzymes are in the middle of normal range. The creatinine was elevated. He’s finished a couple of meds so from a dozen to ten with more to drop off along the way. They just need to see him stable. He sees neurology at Baptist Ochsner tomorrow as a consult for headaches. I actually called ahead because we have not been to this campus. The girl said get to the second floor and ask the director which elevator takes you to neurology. I said I thought I was calling neurology. I saidwe have never been to this campus. And asked her what elevator she took? Like is it letter or color? So she repeated once in parking garage get to the second floor and ask a director which elevator. And could she help me with anything else!? I had it on speaker so Kevin could hear and see how patient I can be because I wanted to scream well how about helping me with what I called for!?! But instead I said thank you and hung up. There was an optional survey but I already wasted too much time! We will go Keith on this appointment. Leave early. Earlier than any normal humanbeing would!
He’s still having headaches. They were more intense leading up to the weekend so since his Tac level is lower I was hoping that would help relieve them.
We also wrote the thank you to the donor family. Big sigh. Tears fought. I joked with a friend that there isn’t a Pinterest board on thank you’d to organ donors not is there really a card. But I would look in every store and finally found a simple blank one with pretty green stuff on the cover. It spoke to me because of my new love for green being the color of transplants! I penciled on paper what Kevin wanted to say then he wrote it from that adding a few words here and there. But really what words do you use. I know if it were me receiving the letter I would just want to hear a tiny bit about who got the gift and a thank you. So we kept it simple like the transplant notebook recommended and added these verses that I can’t get away from at this time in my life. Philippians 1:3-4 I’ve always loved verse 3 since my Louisiana Tech college professor mentioned in in class but this time around I really looked at that next verse:
“I thank my God upon every remembrance of you, Always in every prayer of mine for you all making request with joy,” Philippians 1:3-4
We thank God with JOY for this gift given to Kevin! I looked it up in every translation and it just made me have happy tears.
October 8, 2017
Well, Nate went east! We were as ready as could be. The coordinators even call to check to make sure we knew there was a storm out there then asked if we had plenty of medications, food and water, and to know they were available 24/7. Houstonians know how to hunker down! But there is also nothing like seeing the hand of the Lord. We prayed and asked Him to protect us and the people in Nate’s path. I feel like He knew the pump situation in New Orleans couldn’t take even a Cat 1 or 2 hurricane so His hand shifted it over ever so much. I screen shot the path of this thing all along the way from the moment we first got word of something. Our apartment complex sent an email mid week giving us the list for hurricane preparedness. I was like what! It’s October. Sure enough my faithful Click 2 Houston hurricane app had Nate out there. We were ready. Curfews were in place. Everyone was to be sheltering in place by dark on Saturday. All devices charged. All chargers to charge without “walls” were charged. And an hour after the curfew they lifted the curfew because of the storm shift. We kept sheltering because Nate was exactly east of us and storms do unpredictable things. It was too close not to be careful. Praising Him this morning for completely protecting us from the storm. And from us almost flooding our own apartment! We filled up the tubs with water only for Kevin’s huge tub to empty in no time. So I sent him back with a lid and told him remove the drain thing and put this down. Mid way preparing a blue apron meal I asked did he turn off the water! Just like home with the pool. If we don’t set a timer we are toast! It was to the brim full!!! Caught it just before splash down! Yikes! Fasting labs in the morning for Kevin. He’s been dealing with headaches off and on so I can’t wait to see the Tac level and the neurologist on Tuesday.
October 7, 2017
Waiting for Nate
We are ready and hunkering down. Tuesday at clinic Kevin got his staples out! He’s already much more comfortable! He’s tried to sleep in the bed but the still small amount of fluid makes that uncomfortable. We saw Dr. Sonnier in clinic and he did let him have the headache script. And he’s needed it a couple of times this week already. So thankful for that relief. The “lymphoma” issue from this time last year is popping up again because of the pathology report from the surgery. They went over this report with us in clinic. The donor liver was biopsied along with Kevin’s old liver. The donor liver is excellent. The old one well it’s all the same old stuff. And from last year’s bone marrow biopsy the final word was something like his body is doing what it’s suppose to at that time. Huge spleen. Huge liver. Huge lymph nodes doing their job. The report in clinic was from Ochsner and they sent it to Mayo Clinic. There is one test outstanding but Dr. Sonnier asked for the results from last year’s bone marrow biopsy and it was sent to Dr. Sonnier the very next day. He passed them to the pathologist. Praying it will all reflect the same. I really don’t know what to think about all that. So will wait and trust. I know Dr. Sonnier examined Kevin well. Practically tickling him under the arms all the while saying he himself couldn’t handle an exam like this! Kevin said later it was ticklish. So cute. But when I told them we had this issue pop up about this same time last year I might have seen relief on his face. He said it was good to know someone else was thinking along those lines because their pathologist was “impressed with the size of the lympho” something’s (?). Sorry. Can’t remember that word. It was one blurry time last year. He had just been listed in Houston and endocrine, oncology, infectious disease teams plus hepatology, hospitalists, rheumatology… I feel like we walked through it with faith but didn’t bow down to the crazy what ifs. And it ended up being nothing then. I get that they needed to know especially being listed recently then and he couldn’t have any high risks over his head if a donor became available last fall that would cause those surgeons to hesitate picking Kevin. I’m thankful for a great memory and this page. I could give them the wonderful doctor’s name who we went to and they called her. Plus, I don’t know how anyone could forget a bone marrow biopsy. It didn’t happen to me but goodness. After the doctor telling me she’s had grown men scream during it and Kevin was just so strong. It may as well have happened to me! Cole drove Kevin to it last year and I met him there because it was our church’s annual couple’s retreat. We go to Galveston every year. It’s inconceivable that it’s been a year! Gonna keep our eye on Nate…
October 2, 2017
11:25 am We called Nancy and she returned our call very soon. We called because of the horrible headache. He’s at his maximum dose for this 24 hours of Tylenol. (2,000 mg max) And sadly Tylenol doesn’t even touch it but we had to try. Advil was very effective pre transplant but that is on the Do Not Take list. So she is checking with the doctor about what he can take. We gave her his headache history again and what has worked. The Fioricet (acetaminophen, butalbital, caffeine) is what he’s taken last year and they would give him at Methodist. So we will see. GREAT NEWS the liver enzymes are TRENDING BACK DOWN! She said those are back to normal range. She does not have his Tac level yet but will get back with us. She thinks it could all be related to the meds he’s on.
Horrible Headache
Kevin took Tylenol for a headache after 9 last night then went to bed with it worsening. I actually slept on the couch by his chair he sleeps in because he just kept needing head massages. I even pulled out ice packs and cold cloths. Nothing. We had labs at 8 am and are waiting to hear from Nancy and will ask what else can he take for headache. I’ve combed the side effects pages of the medications he’s on and prograff (on for life) and valcyte (stops Dec 5 according to the blue card) have headaches listed as side effects. But he’s also a headache kid. He’s had migraines. Not completely sure if it is even weather related. We had rain yesterday so it brought humidity. Poor kid. Headaches are the worst!
October 1, 2017 Healing Here with Kevin
It’s October. Reflecting back on my college days I always loved October. Things were no longer back to school but an established routine was in place. I was walking again across campus being not faithless but believing. I repeated this newly learned scripture because I was a literal over achiever stressed about not making an A! And overwhelmed with being in college. College. That’s for smart people. Today after streaming our church services with Kevin in the apartment I was loving the message and wanted to add more to my prayer card section on forgiveness. It had one card with two verses. After today I’m flowing in forgiveness verses and strengthened in that area of my prayer life! And so thankful that our church now streams live. All these years technology never meant so much to me as it does now. And the timing, I’m sorry but am claiming my God sees me and Kevin, and for now, his careful keeping at the apartment, and He allowed the door of live streaming to open at our home church for us:) I know so many places we can hear sermons or stream but after being away since July 24 it’s just so welcome in my heart! I just was walking by Kevin who is resting, and I can’t help but be so thankful for Keith too. He is doing so much while I get to heal here with Kevin. Actually I’ve accused Keith of becoming me with all things Caleigh and homework! I’ve actually heard him enunciate and clench his teeth! I’m the one saying be nice be nice be nice! He even dragged her out of bed at one am after seeing a “remind message” about some homework that was due and wanted to see if she had it done! He called coming home from work one day telling me that he had a spread sheet put together of all the things she hadn’t turned in or was missing! Yikes! A Spreadsheet! You do not want to get between THIS man and his spreadsheets! He’s doing so good! He’s letting Caleigh have friends over and even taking them to fun places. After homework of course. He is getting to connect with Caleigh while I’m here healing with Kevin. He’s taking her to school. Picking her up most days. Getting her to all her activities from band to tutoring. He’s always been available anytime I wasn’t, but never this long term. He did however recently mention he told the Callanan’s he’s giving her back to them! But I think they have a successful system in place now.
Kevin was standing in the kitchen Friday night and prayed over our pizza. (I can only Blue Apron prep so much people!) And I realized what a rare sight this was. We get out for labs and clinics. He walks around the apartment and interior grounds But seeing him and that day no gauze! I said I need to hug you! And I started crying while hugging on him. He is still hurting and tender so it was a gentle hug but oh so precious. And I cried and he laughed! It reminded me of grabbing Cole his last day of 8th grade in our living room without the fan. (Cals description only now it has a fan so it’s the living room that use to not have a fan!) I wanted to see Cole get off the bus for the last time as a Doerre Warrior and when I walked in from the garage he was standing there! What! I circled my arms around him and bawled. He just smiled and laughed looking down completely not getting it! And this hug to Kevin was the same. He’s been kind of unhuggable these days with all that new liver stuff going on. Well, and it was just too much. Especially laughing at myself because I recently had spoken to a good friend who was cleaning out her boys rooms and found a P. J. Funnybunny book and was crying over it! I even gave her the “Emma Award!” but asked for it back in no time! Keith is right. Misery DOES love company! I’ve cried to her so many times over the dumbest things! And boy can I relate to her finding and not knowing how much it bothers you. Delayed reaction can be impossible to get through! Of course I cried with her but also have to chuckle just a little. Because I KNOW when I was crying to her over the seemingly insignificant things that reminded me of change, she was thinking: there is just no way that’s ever gonna be me. I know because I thought the same thing! Then it is. And so today I am so thankful for October. Again. Because change does happen but so does October!
While we have a routine here now we are also seeing how close to home we will be soon. And when I see Kevin I am thankful for Jehovah Rapha my God who heals. I continue to ask Him to heal him from the inside out. But I GET to be here with him while he heals. God made this all happen. He answered prayers here we didn’t even know to ask. He’s healing ten minutes from Ochsner. There are speed bumps all through the apartment and hospital parking lots. No big deal unless you look sawn in half being held together with 77 staples! Even going over them slowly and carefully it’s so painful to watch him out of the corner of my eye. I just keep apologizing! And secretly hating the speed bumps! If we were home, I mean I know I say the Hardy is my friend but with all the labs and appointments I now see he’s doing post transplant we would be in the car forever! More than Kevin could take. God sees. He knew that. We didn’t even think about that. What even in Houston is a ten minute drive away!? We can’t even get out of our neighborhood in less than 7! (I timed it in my 4 kids in 4 schools carpool days!)
I’m learning to cook the Blue Apron way. This is unlike anything I’ve ever experienced. I wouldn’t have done it in Houston because I have a full kitchen and pantry. This box comes to our door every Tuesday. Kevin loves picking the recipes. I love to watch him study food. He’s a Foodie for sure! It’s the least stress I’ve EVER been over that ever present dilemma: what’s for dinner!? I don’t even care what he picks. I have no idea what we are having I just know it’s gonna be good! (Unless it’s fish then he gets a double portion and I get lots of yummy veggies!) I’m learning new techniques and just different ways to make fresh vegetables! It’s the neatest thing.
He’s also healing away from all germs. We are isolated here and we didn’t even think about that part either. They say not to be around crowds for three months. Other than when company comes (and no one comes if they are sick or think they are!) He’s getting to heal and have the strongest possible recovery. I’m a mutlitasker to the bone. And I know if I were home I would be distracted by so many things! I really do get to keep just the closest eye on him and truly take care of his every need. He may be twenty but I can’t help but see my little no kneed cutie when I look at him sometimes. And to think what all is going on inside of him I just want him healed. Healed from the inside out.
September 29, 2017
From the labs this morning his liver enzymes are still creeping up. Not as up as before transplant but above normal. Today they are 47/53. His tac level is 6.3. Creatinine is 1.1 We are adding back a mg am and pm of prograff. So, 2mg of tacrolimus [generic of prograff anti-rejection med hence the term for the test tac level] (We had to remove one earlier because of the elevated kidney function levels and because of the lasix for fluid retention) He’s not wearing any gauze at all today! Nancy was happy to hear it because she knew he was battling that! So labs again Monday and based on those labs maybe a biopsy. She is scheduling one now and will most likely cancel it but they just like to be prepared and cautious. She also wants him to STOP taking aspirin until after they determine if a biopsy is needed. We noted all this on the blue card. And I opened the transplant notebook to reread the “Rejection” page. Here are the 4 things to watch for
1-Elevation of liver function tests from blood work.
2-Temperature of 100°
3-General feeling of malaise/tired flu-like fatigue with aches and pains.
4-Dark urine light stools
TREATMENT:
Treatment can include:
•Increase dose of prograff can effectively treat rejection
•Sometimes steroids are increased (sometimes hospitalized for IV steroids)
•Thymoglobulin given by IV (hospitalized for this as well)
***reminder that almost all transplant patients have at least one rejection episode at sometime. The most crucial time is the first 3 months. The blood work is the earliest sign of rejection even before the patient looks or feels bad.
It is a fine line they are walking with Kevin trying to “trick” his body. Nancy uses that line often. The meds have to make the body think the new object is not foreign even though it totally is. I’m not jumping to anything. I’m remembering several influences on this situation. Good ole pediatrician Dr. Pope says when you hear hoofs don’t look for zebras. It could only be horses. My dad has survived two rejection episodes. And my God is seeing all. And that gives me great peace.
September 27, 2017
Nancy called with lab results from this morning. Creatinine is 1.2 so it’s going down. Liver Enzymes are trending up and “they” don’t like that. They were 18/29, 30/34 and 40/41 now. Tac level is lower 9.3 So. Labs Friday. They want to watch it.
September 26, 2017
Wow! We had a marathon long weekend of fun and family! Kevin had one rough night of random pain at an 8! But so far this is Tuesday and that hasn’t happened again. He had labs yesterday. They called and said stop the lasix and drop the prograff to 1 mg twice a day from 2 mg twice a day because his creatinine (kidney function) was 1.5. (Elevated) And his prograff level was high at 11.3. Normal range is 8-10 and she said they’ve been running it high. His BILI is the lowest ever at 1.9! So out with the blue card and change the prograff dosage. Then today he had a clinic visit with Nancy and Dr. Mathur. He said keep the dose of prograff the same. Absolutely no lasix. Labs tomorrow. And normally the staples would be removed on this week but since Kevin is still leaking from a drain site and the incision they are waiting until that stops. Otherwise it could be too moist and cause it to open. We don’t want that! So our questions: is this leaking normal still. (Yes) can we get more mesh please! (Kevin had 5 but we bought some thinking it would work and I wouldn’t have to keep washing but it didn’t. Kev had already cut off a couple mesh things so it left us with three. And that’s a lot of pressure to keep them clean and dry and ready for bandage changes! So they gave us plenty!) The main meds came from our mail order insurance and the cellcept (prevents rejection) didn’t look like the one from Ochsner discharge day. So we had them look at it. Transplant education at discharge day said to make note of manufacturing changes because sometimes they want to watch those labs closer. When are labs needed again? (Wednesday) Kevin lost 10 pounds right out of the hospital. He gained 10 with all the fluid retention. He’s back down 10 pounds. So we are hoping that means the fluid is absorbing. No ultrasound this week. The doctor didn’t think anything changed that much. He cautioned us on that creatinine increase. He said it was a 50% increase and they just don’t want to be careful with that. He said his liver numbers were a bit up at 30 and 34 but they are still in the normal range.
September 21, 2017
5:30 Nancy called. Ultra sound images were good. The groin area has a hematoma, and it will resolve on its own. Caused by the line they needed during the surgery. Bruising is normal. Still no timeline. But she said she is getting it for us!
Tiffany and Bailey flew in! I had the place ready for her! Washed all the soft blankets in dreft. And vacuumed and swiffed. Sure enough once we walked in the door we spread out a blanket and she was all over the place. Playing and getting around. She played so hard she was out of breath!
September 20, 2017
Heard from Nancy the transplant coordinator. All numbers from labs this morning are good except for potassium. No bananas. No orange juice. He can have grape juice. She is checking on the time frame for us for length of stay. She’s putting a note in for Dr. Cohen for tomorrow. We are at back to back ultrasounds now. 3:30 and 4:30
September 19, 2017
Clinic visit at 1:30 with the surgeon. This one was new to us. His name is Dr. Humberto Boroquez (tried to get a good look at his name tag since he was new to us and they rotate through clinic) He was the best! So nice! And speaks with an accent. He answered all our questions and checked Kevin’s incision and bruising sites from all those removed lines. He’s adding to tomorrow’s ultra sound the groin area where there was a line removed because it’s bruised and painful. Just to check.
Questions answered by Nancy our coordinator and or the surgeon:
•timeline here especially for our apartment. The 3 month lease ends 10-24. 5 weeks from today. Nancy is checking with Dr. Tyson his hematologist. The timeline is tricky. They want to watch him closely so it depends on how the leakage does. What the ultrasounds say. They are mostly following the fluid. She explained again the last one with the crazy medical terms I wasn’t following. It made sense while in the office. Not anything I could comprehend enough other than to be relieved it meant totally NOT what I thought when reading it for myself using dictionary dot com for all the words I didn’t know!
•He had his first post transplant headache. Bought Tylenol and a coke. Because life before transplant Advil was our friend. Now it’s the enemy. The headache could be from multiple things. We hope he still doesn’t get migraines but most likely a side effect of elevated prograff levels even though that was late last week. His hands were a little shaky which is also a side effect of some of the meds. Diflucan also causes prograff levels to go up so once that is stopped they will watch those levels even closer. (10/6) Vitamin D needs rechecked in 12 weeks.
•bruise and pain in groin area from removed line. Adding to ultrasound tomorrow.
•JP drain stitches will be removed when the staples are removed. They don’t want to do that while there is still fluid seeping out because of the risk of infection. They want it to be healing. Usually it’s about 21 days. Tomorrow is 2 weeks for Kevin.
•for the leaking the surgeon said instead of tape he could use this mesh stuff. Well Nancy came in later with it and was like trying to stretch it over his head. He ended up stepping into it and it holds the drain pads in place without taping. I have bought every kind of tape imaginable on the gauze aisle!
•the surgeon checked his areas where he is leaking the most and said it’s more of an inconvenience than anything. He said he will put him on lasix through Monday.
•I told the surgeon it seems so amazing he got out after a transplant on day 5! He replied that’s what being 20 will do for you!
After the surgeon left Nancy hopped back in with last minute things. She added lasix to the blue card. We told her how much we loved that surgeon and she said he’s the one that goes to Puerto Rico often to help them with transplants. They use to have a lot of patients from there but now they have been trained and are doing their own. She said his favorite thing to say is “You got a plan?” We always need a plan! And Kevin’s plan for “crap” shirts worked well. He walked around the hospital in a black and gray type one and the wetness was hardly visible. I told him no one cares and we are in and out! He agreed with the doctor, for what he got in return it is hardly worth complaining about the inconvenience.
September 18, 2017
Amy called with labs. His levels are stable. Repeat labs on Wednesday. Clinic visit Tuesday. Ultrasound also on Wednesday.
Tac is 8.4 / BILI is 2.2 (normal under 1.0) / ALT is 41 range 10-44 / AST 21 range is 10-40 / Alk Phos 106 range is 55-135 These are the best they have been in so long I don’t even know! He asked me this week to go get him some “crap shirts” and a couple of robes. The gauzes keep leaking through so he doesn’t want to ruin any of his “nice” shirts:) I found 7 and I’m washing clothes like he’s a newborn! Not to mention have I mentioned how much I love looking at him! He’s looking so good! It is also the best thing ever when he is blessing our food to hear him say: Thank You for the Liver! We thank Him all the time! Thanks will forever be in our heart!
September 17, 2017
Jeanie called today and spoke with Dr. Sonnier. For now keep Kevin’s prograff 2mg am and on. Fasting Labs Monday morning. No lasix for swelling until after they see him Tuesday in clinic. He’s still changing gauze frequently. About every 2-4 hours. His Tac Level went from 12 to 6.6. Tac is short for the generic tacrolimus which is prograff and that’s his anti-rejection meds. He will take them for life and getting the dosage level correct is what it’s all about. This weekend we have Tiffany and Bailey. My parents are coming with Maureen. Keith and Caleigh! So much to look forward to! And maybe some beignets to share.
September 16, 2017
Labs at the crack of dawn! Lol! And wait to hear what to do. At 3:30 Jeanie called. (Hospital transplant coordinator on call this weekend. She did the notebook education and tested us before discharge) She said Dr. Sonnier reviewed the labs today. He’s the surgeon on call this weekend. He said the prograff level is now 12.1 and kidney function is good at 1.0 and to continue to hold prograff tonight. Change the blue card from 4 mg to 2 mg 2 times a day of prograff. His liver functions are looking good too! We asked about lasix and she said since his prograff level was high they would not put him on it. She will see if the doctor wants to add it tomorrow. She did say all that fluid is completely normal.
*Start this after labs in the morning at the Transplant clinic.
September 15, 2017
3:30 Amy called and said hold prograff for tonight. Labs in the morning. His prograff level is high. They will call back tomorrow after labs to tell him how much to take and when.
-*-Just saw Briova is the correct spelling. And I have several numbers for them. I need to figure out which one is which.
At 4:00 am he woke me up and his JP drain had leaked the amount to wet his shirt … weird?
The wet stain is size of large orange to small cantaloupe. We have labs in clinic this am.
Weight
Wed: 166
Thurs: 164.2
Fri: 167.6
We are waiting for our coordinator to call with their thoughts. It’s actually Amy while Nancy is off through Tuesday. They said from the other day if he gains more than 3 pounds to call and it’s still dripping. With gauze on it, it is still soaking through the shirt. The incision was the problem the other day and for whatever reason this morning it’s one of the two sites where they pulled the JP drains before leaving the hospital. Just perplexing.
Coordinator called while we were still at Ochsner and said get to the nurse in the clinic to let her look at his drain site. His labs are good so she is asking the dr for lasix (fluid pulled) The clinic nurse Michelle sent us out w “abd” gauze pads and tape and gloves. These type are more absorbent gauze than what I grabbed at Walgreens . The draining is normal but she said keep it dry. For now we wait to see if they order that script. He does need to get rid of the fluid.
The Breova pharmacy called about his speciality medications prograff and cellcept. They will call every month before they are due and confirm shipment. It was 45 minutes today on the phone because it was first time set up. And the pharmacist had a chat about side effects and what to avoid. We heard it in the hospital but it’s ok to hear it again. Any manufacturing change they let us know because that could alter the absorption slightly. He said they monitor that but also let the doctors know if there is a change in manufacture so they can keep a close eye on the levels. It’s all about those levels. Always ask before starting any new medications because it could affect the levels. They are available 24/7 as well as the team of doctors we have here and in Texas. Avoid grapefruit and he said some sodas have grapefruit. It’s fine here or there but not everyday. Avoid blood orange things. Keep him monitored by the dermatologist because a side effect is squamous cell skin cancer. We’ve had him with one since 2011 so they are keeping an eye on that. Another side effect is the swelling in legs and feet. Especially it’s a side affect of cellcept. Normal. Walk. Exercise. Also it can affect blood pressure. We are currently monitoring that twice a day. No live vaccines. It was a long call. And it’s who our insurance uses to get his main meds so I listened. Kevin napped!
September 14, 2017
Noon
They populated the patient portal with the ultrasound results late last night. I sent them to Keith asking him what he thought they meant and he replied: that’s what doctors are for! They did say if it was “alarming” the doctor reading it yesterday would call our doctor and then we would be called. Nancy called and said the surgeons reviewed the ultrasound readings before the entire team of surgeons and were not concerned. The fluid was not worse. My thinking is the JP drains pulled that fluid out since surgery and the last of those was removed on discharge day. So that fluid is now needing to be absorbed by his body. The surgeon was reminding us yesterday that Kevin had all kinds of blockage in the old liver and now this new liver has great openings and is working to train the body with the better flow. His body is having to get use to absorbing that. I told our coordinator that I tried to interpret that language and it was good to hear they were not concerned. Ok. Whew. Fasting Labs tomorrow. Fasting labs Monday. Surgeon clinic visit Tuesday. Repeat ultrasound Wednesday. We can call with any changes or concerns always. *Nancy is off and she gives his chart to Amy until she returns*
September 13, 2017
One Week! It’s been one week since transplant. Dr. Carmody told me a week ago it would be like a roller coaster ride. Some ups and some downs. And sure enough there was a little drama today. Like the climb up the coaster to the first drop. So far it was not a huge drop after climbing up but a smooth turn. Kevin had that “leakage” last night then this morning he was swollen on his left side. (Liver is right side FYI) So much so that Kevin said he could feel it over the edge of his shorts. (I was like that is a muffin top!) But is it normal!? We called in early and they called us back wanting labs and a visit in the clinic to see the surgeon. He already has a scheduled ultrasound today at 4. We dropped Keith off at the airport and headed to the lab.
Dr. Carmody (surgeon who did his transplant) was actually there today and consulted earlier but once he walked in and saw Kevin he looked relieved! The look on his face after seeing Kevin is what helped me be relieved too because Carmody was just visibly relieved. He examined him thoroughly. Explained stuff. But he thinks it’s just normal fluid. Tracking to that spleen area. He doesn’t want to give him a fluid pill yet because it’s hard on the kidneys. He poked around on him. Touched around his scar. He said he was healing. He could feel that. I also showed him pictures of the leakage. He added some orders for the ultrasound. That’s at 4. He said, “look at him. He looks good. He walked in. He feels good!” I know when he walked out he was saying how relieved he was that it wasn’t a hematoma. |Ruth said that’s a blood clot after like a ruptured spleen. Glad I didn’t know that earlier:) | We did the right thing. Call. Wait for their instructions. Follow them. And I love that we got to clinic early from labs but they checked him in and before you know it the surgeon was hopping down. He got there before the labs could be processed! Our new transplant coordinator also was in the clinic room. Love that we got the surgeon today and another chance to ask questions to our new coordinator. (They rotate around so in clinic we could see any of them)
For now we have routine fasting lab for 8 am tomorrow but they could change based on today’s labs. Today was white count and chemistry. Not prograff level. His white count was elevated yesterday so they are watching that. Nancy will let us know today’s labs and what to do tomorrow.
Nancy just called. She said no labs tomorrow. If there is anything blaring in the ultrasound they would call the on call doctor and get us. But she will see it in the morning with the doctor. His whites counts went down. They are at 7 from I think 11 or 12 yesterday.
September 12, 2017
8:00 I ran to Hobby Lobby for a side table with drawers Kevin wanted by his comfy chair and got back in less than 10 minutes with Keith telling me when I walked in that Kevin’s incision has “leakage.” Kevin saw his shirt was dark (from wet not blood) and a trickle of wet. But it was clear leakage. So we sent a pic to Tiffany and checked the transplant notebook. Page 13. Call the on call coordinator. There is a number for Ochsner On Call and they get the message to the correct coordinator. He’s been “painting” it with betadine.
7:00 Kevin shucked corn in the kitchen and chopped us some green onions or scallions. (Somebody tell me what’s the difference!)
4:30 Nancy (new coordinator) called with new “orders.” She said Dr. Carmody reviewed the labs and wants to add Ursodiol 3 times a day. So I added it to the blue card. (We had this already from before transplant but she’s calling in the new script to Ochsner Pharmacy)
Kevin had a pretty good night. He called me for pain pill at 4 am. At least this time I heard it! In the hospital he would never raise his voice and just quietly say, “mom, mom…” he wouldd text. Turn on the light. Nothing. Call me or holler! I can sleep through a lot! He had fasting labs at the clinic this morning and we met with his new coordinator and the pharmacist. Keith dropped us off and we walked in. He ended up asking for a wheelchair because that was a lot of walking! After labs we went straight to the hospital Bistro for breakfast. He has to take meds twice a day and they are important to be taken at the same time each day. Other wise rejection could occur or some serious side effects. So they schedule labs around this time. He also needs to take with food so the cafe is close enough to eat then get back to the clinic. (He learned the hard way yesterday by taking meds and didn’t eat soon enough. Bad nausea!)
After breakfast we went to the clinic to meet his new Post Transplant Coordinator. Her name is Nancy. Her brother was transplanted a few years ago. She was so nice and very informative! She went over again what we had learned yesterday before discharge just to make sure we get it. For now they are keeping a super close eye on him. His labs. And they change the amounts of medications often. So we keep up with that blue card. When we come we bring it. He also takes his temp and blood pressure twice daily. We keep up with that in the transplant notebook and bring it to all visits. He weighed 160 pounds today. Normally he’s around 170-175. So that was a gigantic liver like the surgeon said. He had some elevated numbers from labs this morning. The prograff (anti rejection med) level will not be back until after noon. So once it comes in on lab days the doctors and team look at it then communicate with the coordinator (who is also a nurse) and she calls us with what we need to do.
We stayed in the room and then the pharmacist came in. She went over how important it is to keep on top of refills and checked our blue card with the system.
*i have better notes but since keith is here I hopped over to get my toes done! Going on memory:)
**I’m not leaving him alone for a long time.
***he has to be careful with potassium levels. They can’t be too high or it interferes with the medication.
September 11, 2017
Just typing that date I have to say We Will Never Forget!
3:30 Kevin is showered and in normal clothes. We are waiting on transport and Keith is parked outside. He went and got Kevin a push button recliner for the apartment that heats and we are out of here!!!
Pharmacy was in for teaching. We are very informed. Kevin’s list of medications are on a blue card. It goes everywhere with him. Clinic. Labs. Etc. She said NO HERBALS. NOTHING EVER FROM GNC. No GRAPEFRUIT. NO POMEGRANATE. Those interfere with the prograff level. And that keeps him from rejection. The cellcept is for life. (Because Kevin’s indication is PSC.) Baby aspirin is for life. Most of the meds have a stop date. It’s all on the blue card. No probiotic with antibiotics. So no florastor. If he forgets his 8 am meds the cut off time is 2:00 pm to take that dose. If he remembers after 2:00 pm she said skip the missed dose and take the 8:00 pm on time. If he misses that and remembers the next day call the coordinator. It’s all in the black transplant notebook. He will be on a steroid but they already gave us a taper off schedule. If it says stop on the blue card always ask the coordinator if they still want it stopped. Never stop a medication without asking first.
Lost all track of time. Kevin’s surgeon Dr. Sonnier and team rounded through. They are sending us home! (Nola apartment home) He told Kevin he got an excellent liver! They loved all the questions his sibs asked. Especially the roller coaster one. The NP kind of went over them again for this doctor:) Very busy. Patient education with the transplant coordinator. We went over every page of the black transplant notebook. No public places for 2-3 months. We don’t have to lock ourselves inside but avoid crowds. Be creative. Hit the parks at uncrossed times. Avoid malls unless it’s a non busy time. Same with stores and restaurants. Go when they are not at their busiest. She said DO NOT WEAR THE MASKS. They do not do anything to prevent catching germs. She said the paper ones are not designed that way.
Dietician came in too. She went over what he can and cannot eat. I knew grapefruit. But also nothing pomegranate. (I bet POM would not like hearing that!) She said they are popular now but a no for transplant patients. Heat all meat. Even sandwich meat. That was new to me. So she said just heat to steam in microwave.
9:30 Respiratory checked in. She watched him with that deep breathing devise and said he’s doing good and to remember to use it throughout the day.
9:00 am Melissa Transplant NP She checked in and said once the drain is out today he can shower and maybe go home today. We will see. She said Dr. Sonnier will round with her later today. (One of the surgeons who did his surgery!) At first she thought it was time for a routine ultrasound but then said it’s for 7 days after.
8:30 The nurse removed one of the extra IV’s. It started bothering him yesterday. They put several in before surgery. So many lines and now he’s losing them one by one. He still has one JP drain. It should be removed today. And the dressing on the central line can be removed later today.
7:00 Kevin got out of bed on his own and walked to the restroom. He actually has finally crossed several hurdles after surgery. Got up unassisted. Passed gas. Had a bowel movement. He also seems to be going longer between asking for pain management.
September 10, 2017
5:00 The Central Line was taken out. I would say not without drama. The nurse who was “pulling” it struggled removing the “stitches.” She had to call the charge nurse and she struggled removing them as well. But it was comical because she said I’m going to ask which resident did this and first say good job and then yell at them! Once she got them snipped the nurse really had an easy time. I was only nervous because it was a central line! And this entire process took 20 minutes. Then once the line was removed she held pressure on it just for another 20 minutes. He is so happy to have his one gone!!!
This afternoon we had family from Bossier drive down and visit only to head back in the same day! Greg, Patti, Ainsleigh and Carrie’s visit helped us pass this afternoon with so much fun! It was great to visit and catch up. Everyone was heading out that have been here except Keith. He’s in it until we say he can leave:) It was great having everyone. I was just telling one of the tech’s who all everyone was and where they came from. She thought it was great everyone seeing Kevin. I said yep: He is loved!
Physical therapy came by and took Kevin waking and he did 6 steps. He’s been resting a lot so that wore him out! They said walk him one more time today.
10:45 Dr. Mathur and Melissa rounded. He loved all the balloons. He asked Kevin what his favorite movie or character was. Kevin said Hulk! The doctor liked the Guardian of the Galaxy 2. They bonded over the balloons! (So Mam Maw Sheo did good!) The drain comes out in one more day. The central line will be removed today! All his liver enzymes look good. He answered all the questions and they both loved that the sibs had some:
Roller coasters yes but not anytime soon! Diet will be gone over in detail later with a list of foods he cannot eat. No football, lacrosse or any high impact. Kicking the soccer ball is fine just no aggressive attempts. (Or something like that) all the other questions he said could all change so the first 6 weeks for sure to be careful and we would know more later specifically.
He is doing great and they are happy with his progress. Could go home as early as Tuesday!
8:40 Jennifer said they advanced his diet and are discontinuing the CVP!
***Along with the self med box Kevin also was shown the other day how to “paint” his incision. In the medicine box are packages of large swabs. 3 to a package. He paints above it, on it, and below it.
8:15 Melissa the transplant NP was in and will be back with Dr. Mathur and is putting in a diet change with a pause that he needs to have a bowel movement. She was happy he was out walking yesterday. We asked her about the blob in the drain and it was just tissue. Not at all worried about it and said they can change that out.
Jennifer nurse: the charge nurse is trying to get that CVP monitoring discontinued
8:00 am Kevin has been passing gas! We got to face time Caleigh last night and she is doing great and even had some questions for us to ask the doctor because we didn’t know the answers:
•Can he ride roller coasters
•do we still have to eat “that sodium diet”
•They mentioned no contact sports and Cole and Kevin both were asking for how long? I’m like what exactly do they consider contact sports because I know they are going to want to keep kicking around that soccer ball.
•Tiffany wants to know:
•will he need antibiotics before dental procedures?
•When can he go back to school?
•When will we know if he is rejecting the organ? (I told her we have a notebook and some of these answers are probably in there. It’s in my lap as I type so am about to cuddle up to that good book!)
•When can he go in public places?
September 9, 2017
Cole stayed in the room with Kevin while I slipped out to dinner with family. We tried to go to Johnny Sanchez (Aron a Master Chef judge owns this) on a mission from Kevin who read the menu but it was an hour wait on a Saturday night so we hopped next door for pizza. He passed gas too! When I told the nurse she got happy! She told Kevin that nurses and moms love that news!
10:50 endocrine doctor rounded and said his blood sugars are fine. They always as a precaution check them all day because it’s normal to have high levels after surgery. But Kevin’s never really were so he’s stopping all day checks and said in morning labs if there is a concern they can address it there.
10:30 Dr. Mather (surgeon rounding) Charge Nurse Danielle and Transplant NP Melissa all came through. Kevin’s thump on the stomach sounded better. So he was happy with that. He said all his liver numbers were trending excellently. We had two questions.
1-why did they not need any pints of blood? He answered: we have really good surgeons! We all laughed. Then he said they try to do a bloodless incision. And they may have sent some of Kevin’s ahead and circled it back through. (?) Kevin’s asleep now and he’s my exact listener. I get it but then can’t really retell it.
2-What is done with his old liver? He said they send it off to pathology. They slice it up looking for any other evidence of anything that might have been missed. (I guess like underlying diseases.) We see those results in clinic.
8:45 Melissa the NP for transplant came in. She said if things go as well as they are he could get out mid week. 6-8 days is average stay from incision.
7:00 am
We are responsible for pulling the meds today. They pull about thee days and put in a box. Then we pull them for the times required and put in cups for today. They said have it done before the nurses change or something like that. So when they took his vitals at 4 Kevin woke me and said we need to pull the meds. I will do the blue card you put them in cups. Then we went back to sleep. The nurse came in at some point and was happy to see the meds pulled but she said we were early but it was all good. So far there have been WAY worse med scenarios that we went home with that I had to call my pharmacy friend to step us through! Take this without food and this with food but an hour before or an hour after. Overwhelming! But these so far are 6 am 8 am 6 pm 8pm and he doesn’t have any 6 am ones. And it’s mostly just for the first few months.
September 8, 2017
We ended the night a pretty hospital routine way. Watching Master Chef. I cannot tell you how wonderful it was for him to want his iPad and open it to this show. I’m not a big cooking show watcher. Like really. It’s stressful! But over the past 15 months I have loved watching him watch it and grown to be addicted to it rooting for our favorite chefs. And on the side learning a few random useless things! And tonight’s show pretty much had us both in tears so I can love any show that makes me cry!
10:45 we got the liver pillow and the blue card education for medication. The pillow can be signed and is used to press on his abdomen when he needs to get up. The blue card organizes the dosage of meds. We start pulling our own meds tomorrow. They check them all then he takes them at appropriate times. It’s to prepare him for taking them at home.
6:00 He is in a new room. It’s actually the exact same room we were in when he was here a couple of weeks ago. 8070 Transplant Step Down Unit. And we have the nurse who was our nurse when we were an almost transplant back in August.
4:30 We are waiting on a room in the transplant stepdown unit! They are currently cleaning it. I know the nurse we had yesterday told us about this bright bright r2d2 type light that cleans the rooms. They set it in different corners and places around the room. Not sure if it’s all rooms or ICU rooms. Sounded cool. So if we are ever driving over the Huey P. Long Bridge and see a light show from the third floor of Ochsner we will know another room is being cleaned!
4:00 the nurse removed his IV fluids.
3:30 we were given a transplant notebook by the liver coordinator. They will be back by in a few days to really go over it.
2:45 Dr. Jax removed one of the JP drains.
11:15 Samantha one of the social workers came by and checked on us and visited a while. They don’t just let you say you have support they want to hear the details!
11:00 endocrine doctor came by and is following his blood sugar levels.
10:00 Jasmine did a bedside ultrasound.
9:45 Dr. Marthur a transplant surgeon examined Kevin. He thumped his abdomen and said because it sounds like a drum he needs to pass gas. He can have liquids with bites of crackers otherwise if he eats he said it would come right back up.
7:30 Dr. Jax she said his A line can come out. Happy happy to lose lines.
7:00 am Kevin had a pretty good night. We slept well. Hospital noise is now white noise to us. And that’s huge considering how alarming and jarring it all was in the beginning! Dr. Hart was the first one in. (Caleigh’s tutor’s brother.) He is so nice. I feel like we are watched over so well.
September 7, 2017
*this place is so busy. I open a note in my phone. Start and stop little updates and when time will post them. And there is a window so we are being watched. And I can’t put a sticky note over it like my PC!
9:00 Kevin has had a monumental day! And my God has had a MONUMENTLIER one! I don’t know where the time went. The nurse today was so nice and talkative! We heard such great stories. Our NOLA Pastor and his wife visited and prayed over Kevin. We had surprise company! Pastor Pope and Mrs. Barbara hopped around the curtain with a Mickey Mouse thumbs up! And I hung up on Ruth jumping with tears to hug them both! Sheila and Mam Maw got to see him at a normal hour and Kevin realized for the first time their presence. Cole flew in. Tiffany and Grant and Bailey drove over. I’m hearing such great stories of Caleigh “Callanan” that we are all wishing we were her!
Kevin wanted the catheter out! So the nurse took it out this afternoon. And I looked at him and asked: is that allowed? Next thing you know Kevin is asking to have help walking to the bathroom! I know we get excited about our kids potty training but it doesn’t stop when they are two! Who knew it continued when they are twenty! One nurse said well you won’t go much because you haven’t had much it’s just the sensation from the removal of the catheter. And we step out. Walk in to see a great amount and hear his nurse proclaim well, you proved me wrong!!! It was the hardest thing ever to walk away last night leaving Kevin here. But I knew I needed some sleep. And I knew he was in such good hands. He had two nurses on it all night and constantly monitoring something. I am struck with such great awe as I see each and every line and tube and cord coming out of him. I see even more how great God is! He spoke and breathed and created, and we fill an entire hospital room with beeps and bells and machines and tubes and tubes and tubes and tubes and stand in awe of the great wisdom He poured into willing servants to invent and train others to use to give my son that most precious gift of life. I told a friend having Dr. Jax share her story with me earlier that she lost a brother and knowing his organs were donated gave them such happiness. I see now that new joy. I’ve focused on the sadness of the loss of life (which truly is very real) and not the joy and beauty God makes out of the ashes. Those mourning the sometimes unexpected loss of loved ones truly feel that joy knowing that a part of their loved one brought unexpected new life to someone else’s loved one. It is almost unwordable! And that’s not even a word but it captures exactly what I can’t word! I didn’t get too far out of my praise time today. I camped out on He is Elohim! One who is great! Mighty! Majestic! El Roi: The Strong One Who Sees! And all day as I looked at Kevin I’ve whispered to Him, Lord, I will never ever be able to look at Kevin without KNOWING You are Jehovah Rapha! I AM YOUR HEALING! When the nurse walks in and announces its time for your prograff (anti rejection meds) I told a friend it sometimes turns me into cement but I quickly have to say Lord I’m not going there. He then is my Banner! My explanation only here (so not contextually or biblically accurate) but to me my: Jehovah Nissi which to me I see when I’m deepening in trying to grab that worry I see His white banner just waving! Flickering ever so gently so it catches my peripheral vision. And it’s just such a beautiful thing. I Love You Lord! And I do lift my voice to worship and praise you and along with my voice I squeeze out every bit of my heart in adoration and love for YOU! Thank you Lord God Almighty for Kevin’s gift of life-his new liver!
3:30 Kevin was moved to a new room around the corner still in ICU just a not as much observed.
1:30 Caleigh texted and asked how Kevie was and … wait for it: does he have a scar!
12:30 Dr. Galati (Houston liver doctor) texted me to check on Kevin. Love that!
11:20 Debbie the physical therapist is in getting Kevin in a chair. They said they normally put them in the room chair but since he will be moving to the step down unit today she’s putting him in a wheelchair! Well, ok! (Me: he seems tired and I’m not sure he will sleep much in the chair but I get why they want him moving)
11:00 Daneeka the NP for transplant came singing in the room! She was happy and smiling! Jay showed her his blood sugar numbers and she was just so happy! They looked great! Normally patients need temporary insulin. He doesn’t need insulin. They will keep checking especially as he starts drinking and eating.
10:15 Jay started removing several of the lines. Kevin is resting.
10:00 Dr. Carmody (surgeon who did the transplant and spoke with me before in Q&A) stopped in with his team and said how great Kevin did. He showed him where to expect to be sore. He said normally they pull it all down but he said your big ole liver (and spleen) had us pull down and up and to the side. He said it was tricky getting in there but once they got the liver out there was plenty of room for the new one. He asked us if we had any concerns. We are just amazed! He likes the blood pressure below 160. It’s about 140 now and he may give something temporarily. He said he going to get the lines out and hopefully move off of this floor later today.
The social worker Samantha was rounding with that team and stayed back and asked questions. She asked Kevin is he having and stress or depression and how he handles everything that has happened. He said prayer. She asked me too. I said lots of prayer and support from friends and family. She asked how we got through it and I said it was really a calming and exciting day. I completely trust this place. I know they know what they know. 🙂
9:15 Food service brought in a tray of liquids! Yellow Jello. Apple juice. Lemonade. Broth. Coffee. Kevin is like. Is that mine? I didn’t order it.
8:45-9:50 Jordan is doing a bedside ultrasound. I am actually seeing Kevin’s liver and blood flow. And mostly saying I’m seeing it because the only thing I’ve ever personally seen on an ultrasound were my babies! She said we will be seeing a lot of them and to get use to it! Love that. God is amazing! In case I haven’t told you lately. She hopped out to check with the doctor and hopped back in a couple of times to do a few more images.
8:30 He asked for a fan after I told him the room is as cold as the thermostat will let it get. |Loving my blanket Michelle! And socks Rebekah and Melissa!|
8:15 swallow test. They let him take three teaspoons of water. Then he sipped from a straw. This is preparing him for oral pain meds.
8:00 am It is a small world. Caleigh’s math tutor, Mrs. Bloodworth, and former math teacher at Doerre when she heard we are coming to New Orleans texted me and said her brother was there! Well, this morning in walks her brother ~ Dr. Hart the Executive Vice President and Chief Medical Officer of all of Ochsner! He was so impressed with how well Kevin looked! And he said he’s seen a lot of patients after transplant. Kevin talked to him. He gave us his card and cell number and said to let him know if there is anything he can do. Then he hopped out and spoke to all the staff around Kevin’s room.
7:15 am Kevin asked questions about his surgery. Like the timeline of things. How long it took. He didn’t know we were in at all. He spoke just a little then asked for pain meds. He’s at about a 7. Jay is today’s nurse and he talked to both of us asking about Harvey and our “back ups” and experiences here. Kevin is resting. He looks so good. He did tell me “his abs hurt.” I bet so! |Keeping the cell phone usage to a minimum while in ICU.|
6:45 am the tube is out. Dr Jax talked to me on the other side of the curtain while the team of people removed it. She was a sweet sweet doctor. Somehow I told her I just feel for the donor’s family. She said if it helps when she was younger she lost her little brother and they donated his organs and if it makes me feel any better it really helped them. From a donor family perspective.
6:15 am We went to the apartment last night after getting to see Kevin for about 10 minutes with Keith, Aunt Sheila and Mam Maw. Brian his nurse let us all in. It was 2 am before we pillowed our heads. But Kevin was able to communicate with his nurse and move all his extremities when asked. We didn’t see that but he gave us that update. Kevin didn’t know we were in the room last night. This morning Keith dropped me off only one can be in here during shift change. When I walked in Kevin’s eyes were on me for a minute. I gave him a thumbs up. He’s intubated (has breathing tube in) but is pretty much doing all the work. His nurse said he’s hoping to get that out before he goes home. He said Kevin had a great night.
September 6, 2017 We Got The Call!
I will try to put bullet points with time below throughout the day:
10:04 Dr. Carmody (surgeon) just came out. Everything is done! Kevin is doing great! He will be in recovery for an hour and a half then we can see him. They will take him up to ICU. They said he will be asleep all night. He said no blood was needed. Usually in the nation about 7 pints are needed. None needed for Kevin. He said at first he was worried about the case because Kevin has a huge liver and spleen. He was concerned about that spleen bursting. He said No Contact Sports! He said he’s producing bile and all things look great now. He reminded me from earlier that transplants are like a roller coaster. Up and down. All is good now. But things could change but they are on it. And … I hugged him!!!
9:43 4 hours and 7 minutes in
What I am forever grateful for is precious friends and family reaching out to us. Every text and verse and prayer has been our encouraging strength to help us stay strong. I just told a good friend how we had church in the waiting room earlier. The college in Tennessee Kevin attended sent us a link to join them in a service live link and they prayed right at the beginning of service. (Keith and I held hands |i know in public even!| and prayed and listened to that service with our Bible open and hearts so full! Our church here and in HoUSton (Harvey font) prayed and beautiful people sent me images and words I will never forget. Jane sent every dr and nurse in Methodist that she told about Kevin today. All this I slowly sent to Kevin. I know I have his phone but I started it with while you were out: as I type this I’m listening to a huge hug (!) a friend sent me a gift in an email of a beautiful Christian album! I’ve been meaning to download a while back. How she knew!?! We are still waiting out the second half but am joining so many in giving thanks and praises to God and His precious healing and every present hand!
(Church link http://Faithforthefamily.com )
*not sure if they archive it but want it for Kevin for later.
8:50 Dr. Sonnier just hopped out. He wanted to update us as well and let us know we can relax. He said he’s doing really well. He and Dr. Carbony both worked on him this part. He’s going home while Dr. Carbonay and another finish. Keith and I both thanked him so much. I had tears. The surgeon gave me the BIGGEST hug!!! I got to hug Kevin’s surgeon!!!! Whew! Sooo thankful and blessed for the great knowledge and wisdom our God gives them!
8:44 pm Kaylah the nurse who updates us just came out. She was ALL SMILES! She said the old liver is out. The new liver is in. They are letting it profuse for 20 minutes or so while the team takes a break. Someone is watching him for bleeding. All is well so far. She did say that she could tell us that his liver weighed 71/2 pounds! And it was the second biggest liver she’s seen! And she feels better for him already! Next step is connecting the bile duct.
5:45 Kaylah the nurse from the operating room came out. It has started. Incision was made. She said we are in it for the long haul! I am so happy to hear it. I told her I needed someone to tell me like by standing on their head THIS IS THE ORGAN!!! She just smiled. She said next time they come out will be when the old organ is out and the new one is in and whenever the surgeons need for her to update us!
5:00 the coolest thing. I was praying through a prayer a friend sent and in the middle of that prayer Dr. Carmody came by and said “we are still waiting on the organ to get here but I’ll come out and talk to you in a bit: give me 6 hours!” How cool was that! He’s seen me once. Recognized me in this mass of surgery waiting room and told me that. I soooooo wanted to go chase him down and ask: so. This is happening?!?!
3:15 I took this picture (will try me best to insert it here or above post!) the nurses and anesthesia teams came in to get him. He had just hopped down to the restroom. Isn’t that they way it always goes. Leave to go potty and the food arrives! So I got to chat with that great team. They are first class. I know I asked them over and over if they saw the organ. And they were wishing I would stop asking cause I kept rewording it to be sure they knew my meaning! As best I can tell the nurse said the procurement team has the organ. They said it is a good one. I’m just keeping it a little back because we know things can change and they can stop the surgery for anything. And we would be fine with that.
3:00 I’ve still been back here. Kevin is prepped and ready. I do know they haven’t laid eyes on the organ yet but on paper and all they seem excited about it. Anything could call it off. But for now it’s on and we are in pre op waiting. Pastor Jayme came and prayed over Kevin and visited a while. Nice distraction and fun. We are so touched for the time this Pastor and church family has taken to pray over Kevin! Keith just landed and is ubering his way here.
2:00 still waiting
12:00 I am now back in the room waiting with Kevin. He is ready.
11:45 Dr. Carmody took me in a room to tell me what he knew and gave me ask questions. Once he said he knew Dr. Ghobrial and Dr. Galati I breathed a sigh of relief. He asked about Houston after Havey. Was encouraging us that we will come back stronger. He came just before Katrina here. I do know he said they have not seen the organ yet and that the donor was standard brain dead but was high risk due to blood received. He wasn’t concerned about it at all. More stuff he said. Will add later:) He mentioned he would try to connect bile duct to bile duct but we needed to know that might not be a possibility.
10:36 They called him back in OR prep. The nurse will call me once he’s ready and I can go back.
10:30 I called Shelly and once she answered they called him back.
10:00 am Shelley called. If we haven’t gotten called in 30 min call her. Timer is set.
8:42 am we got THE CALL Kevin is Primary
6:17 am we got the call to officially be NPO
12:01 am (midnight) we got the call to be back up.
September 6, 2017 12:06 am
Just got called for back up to another center. Considered high risk but only for +CMV {which she said most all people walking around are} and the fact that this donor has received a lot of blood. It’s a great young liver. No social history. No fast yet. No time set yet. It’s early on and we will hear something tomorrow. Debbie is the on call coordinator.
We had the best visitors come through on their way back from a family wedding: The Sargents! We are blessed to be so loved and cared for! We had a great time showing them our little world and catching up with them.
They placed the organ Sunday night for the last organ he was back up for. It was probably my first self inflicted anxiety or panic attack. And really it’s just insane. I’m a believer. I love the Lord! I trust Him completely. And family was in. We got a call in the while in the French quarter and it was just so exciting. Hope. Expectations. Sadness. So many emotions running through my head. And I know he was getting hungry the next day once he had to be NPO. And I expected that we wouldn’t get called off until early Monday morning like last time. 5 or 6 am. Why I plant that in my head I will never know. But I did. And pushed out figuring out what for Kevin to eat once he could. Hoping it wouldn’t and we get that back up! So at 1 am Monday when they called it off. Kevin wanted NOTHING in this apartment. So me and Cole and Cal went with Kevin to forge for food. Nothing in our area was open. Then the internal boiling of my insides started happening. Like telling myself why did I not plan better. Why are we out this late! And I circled who knows where trying to find an area closer to late night college kids or interstate travel. All the while the kids thinking I knew where I was going. Then Kevin saw an IHOP. And that’s actually what he was wanting. But once we got in one of the waitresses smelled like cigarette smoke and normally I can handle that but mix that with boiling innards and enter mama nausea. Then just sitting and trying to be fun while the entire time I’m thinking how sick I might be! Yuck! And then come the emotions. It sunk in as I looked over the table at Kevin. The restaurant was starting to populate with college kids. Nice. Mannered. Like they had been studying or just out having fun. Seeing clumps of them out and being normal and just having heard Kevin say something like how weird it will be to be back in college. And thinking about the donor and the family. And the family that received the life gift and how happy they must be. Yet how very emotional I was. How Kevin handles nausea so strong and well, I will never know! I almost called Keith to come pick me up! But laughter, and hearing what Caleigh thinks a gap year and a leap year are plus deep breaths and constant inner cries for help from my Lord settled me down. I realize I’m a basket case. And if somehow I can remember IHOP is open all night I don’t have to wonder what Kevin will eat! But I may never know what he wants. And after being NPO (nothing per oral) all the while then I will do whatever it takes to get him what he wants! (And the fridge has normally things he will eat!) Cole was the best after it all. Before I went to bed he wanted to tell me goodnight and he gave me the biggest hug! We couldn’t ask for better love and support and He puts them right in our path no matter how far out of the way they had to go because of Harvey to get in our path!
September 1-3, 2017
Keith and Cole and Caleigh got in late Thursday night! They went back and forth if they were coming due to I 10 closed because of Harvey. They ended up going practically to Shreveport and down 49 and about 3 ish hours added on! But it was the perfect long weekend for everyone with Cole out Monday and Caleigh actually out until Wednesday. Sheila Roland and Justin hopped in as well for some of these days. We had a blast with them. They all got to got to church with us. And as we were eating in The French Quarter on Saturday we got called for Kevin to be a back up for a standard brain dead donor. The primary is at another facility. He was still able to eat and drink until Sunday at 3. The surgery for the primary is after midnight so we should hear something in the middle of the night or early morning. We really don’t go a week without something happening here.
August 31, 2017
Labs and Clinic visit with Dr. Tyson (Dr. Galati of NOLA) She was happy to see us again. Hadn’t seen her since evaluation. She talked about how many back ups we’ve been and discussed that time he was primary. She said she knows they want to get Kevin transplanted and hears his name all the time! As discussed before being discharged last week they want him to rotate antibiotics every two weeks. Taking one per day between two weeks of the augmentin then two weeks of Cipro. Switching on September 3. We go back to clinic visits and labs every two weeks seeing her NP and then she wants to see Kevin once a month. But like I was thinking she said she hopes she doesn’t see us again:)
August 28, 2017
Praying and praying for all those in Harvey’s path since he closed schools Friday and all this week. We are keeping updated with Keith and social media and it’s heartbreaking. We are not there but feel like we are. It’s just all so weird.
Jaimie sent this today:
He is technically # 6 on our list today. However looking at certain factors, he could be #3.
August 26, 2017
9 am labs
1:00
Hospital Liver Coordinator called. His white count is higher than previous but still low. His liver enzymes are a little higher. (Reminded her dr sad stop Imuran) Not worried about it. Didn’t check amylase or Lipase. Wanted to know how he was doing. I said he’s eating lunch. Doing ok. Just checking on him. Said she hopes they get something soon for him.
So nice of them! Love that they called to check💚
Hospital Stay 12 (First Stay at Ochsner) admitted August 23 to … August 25!
August 25, 2017
Robin is the nurse again today and Hilary the NP. His MELD is a 25! Wow! That’s the highest he’s ever been. Most of the numbers stayed the same for calculating it. The INR was elevated so they think that’s it even though they do not know why nor is it a concern for them. His Lipase is lower too (381 from 500+)so that’s a very good thing. That puts him one step closer to eating real food.
Kevin wanted me to call Jane and let her know it’s a 25. I also ran everything by her as Houston Transplant coordinator I wanted her take on what offers to accept and all. She said on the phs donors stay away from West Nile, Hep C, toxoplasmosis, (she can’t imagine they would offer him one with any of those) … all other things she said are treatable. She is going to capture his high MELD. She said every time it goes up they can capture it. And to not be concerned about the INR. It’s a sensitive test and is sometimes high when it reads low. Creatinine 0. 8 Sodium 135 INR 2.5 BILI 7.3
We had company visit! Bill and Debbie and my friends Jeff and Michelle and Kella on their way to PCC. It made the morning pass so quickly! Then it seemed out of no where they were fine letting Kevin go to the apartment. He’s on antibiotics. (Will switch kind every two weeks) Has pain meds if needed. They gave him a Vitamin K shot for the elevated INR. And they want us to have labs in the morning and to be seen next week by the NP with labs again. Before I knew it after Kevin ate his first real food for lunch and did fine we were discharged. Harvey is looming in the gulf and we are praying for those in this storm’s path to stay safe. We also pray that the next hospital stay is the liver transplant! I am amazed that the wording of Kevin’s MRI/MRCP said “inflamed pancreas” which is not officially pancreatitis. The wording said no evidence of cholangitis or pancreatitis. Just inflamed. This keeps him on the list. He was temporarily on hold within Ochsner. Not with UNOS (united network of organ sharing). Such a praise! I’m melting into this place as laundry is going and we keep most of the bags packed for “the call!”
August 24, 2017
Last night they moved us to the transplant floor in the West wing. So floor 8. (That’s the 5th room of the day if you count the “parking spot” they pulled his bed into after the second ER room as we waited for the MRI/MRCP yesterday! It literally looked like a parking lot but with curtains hanging from the ceiling for yellow painted lines.) It was after 9 pm and I was so ready for a shower and bed and when they came into move him they startled me at first because they used “offer” words like primary and orders! But they were in hospital lingo with floor and area terms which at one point I looked at them and said are we getting an organ!?! Then they saw my face and explained no. A bed opened on the transplant floor! And it took until after 11 pm to get to where we are now. But the room is bigger! I lost my excellent view of Old Man River but it is still a pretty view.
This morning his nurse Robin and the NP Hillary gave us some lab results but still no word on the images from yesterday. Personal best as I joke in MELD at a 23 and a BILI at 9.5. We all joke about how only pre-transplant patients celebrate getting sicker. His Lipase went from 500 to 966 so for now still NPO. He did say he had a bit of a headache.
Asia is the social worker for the floor this week. She came in as happy as ever and explained how the rounds work here. She said they all come around at 11 and round in a group: surgeon, hepatologist, nurse practitioner, social worker, etc. She said she stays around after in case there are questions we want to ask or things we didn’t understand. Currently letting Kevin rest. His pain has been being controlled and he hasn’t had to ask too many times for pain meds. That’s a praise!
Jaimie sent this message in the portal this morning based on labs:
“MELD today is 23. He is now listed with that MELD of 23. He is #7 on our list officially. He could be #3 based on certain factors.”
11:30 Still no images. Dr. Lott (not Latt! I try to see their name tags because we don’t know anyone by face and I haven’t learned the scrub color system!) and NP we’re just in. There was a problem with getting them. She said should have them soon. Like in 30 minutes. So we will know if ERCP is happening soon. If not he can have liquids. But since Lipase is still elevated if pain then back NPO.
12:15 Ok. NP Hillary said they finally saw the images. He has no active cholangitis and it even commented no active pancreatitis (however we know labs tell us otherwise) so no ERCP Needed. The telemetry heart monitor he’s wearing since ER (protocol) that he hates can be removed! He can have broth! And she said they have laptops to use if we need one. Cool. (Just watch as he adds liquids if pain persists to back off)
1:30 Here is an answer to prayer about being away from home and my getting food! Ochsner allows family to order off a similar menu and it’s delivered to the room! No stashing bananas here! With Tiffany at Tx Children’s and friends and family always hopping in I never had to worry about how I was getting fed. Hospital cafeteria food is better than no food. Any. Day.
Ochsner Hospital ER
Kevin awakened me at 5 am. He went to bed last night with pain meds. He said he hadn’t slept all night. So we made a quick plan to head to ER.
7:00 am zofran and dilaudid given.
8:30 Dr. Voigt (ER dr) said the amalyse/Lipase number was elevated. Waiting on transplant to chime in.
9:00 Hilary NP for transplant team said they will probably admit him. Is reporting back to hepatology for what they want to do. His MELD was higher than when he came in. Like maybe a 20 or 22. She said they can capture that one.
9:10 dilaudid and zofran
Orders: antibiotic. Fluids. Steroids.
BP 108/72
9:30 Drew cultures
10:15 a message from Jaimie the transplant coordinator here:
“I will cancel the appointments. His MELD is 22 today. This makes him #8 on our list. Given factors of other candidates, he could be #3. I hope he feels better. I might come visit ya’ll later today and give you the powerpoint. I have meetings til almost 2 I think though. If not, I’ll try to make it to see you tomorrow— if you’re OK with me stopping by, let me know.”
11:15 NP Hilary and Dr. Latt stopped in. They moved him to a quieter room in the ER waiting on room to open. This liver doctor we haven’t met but he’s on the team. He ordered an MRCP/MRI to look at the ducts. He may do an ERCP just to stretch things out. He said he thinks Imuran is causing Kevin’s pancreatitis. He said its unusual for cholangitis to. (I would say Houston usually goes here too but always circled back and said yep. Gunk and cholangitis causing Kevin’s pancreatitis) He will speak to the team about discontinuing the Imuran. We mentioned he’s been off it during hospital stays before. But he’s taken that since diagnosis in 2012. Dosages have varied. His numbers are greater than 500 so for now they are holding off on transplant for a couple of days. He’s not on hold on the main list just the inner list here. (Just to me and Kevin this doctor reminded us of Dr. Khan who use to work in Dr. Galati’s office. Gave us “information” and was knowledgeable. But not sure if we connected completely)
12:30 They moved us to the MRI/MRCP waiting area. He has a room on the 10th floor after this so I’m following him around with his back pack and my hospital survival bag. Once we get to the room we have “stay” bags in the car.
2:00 in the room 1061! Took an oxycodone. And they will alternate with dilaudid to control his pancreatitis pain.
We also did get a visit from Jaimie our transplant coordinator! She is the coordinator for out of town listed patients. So she can relate to us really not knowing anything about the city or hospital! She gave us GREAT insight of listed and procurement details. She also gave us good finds for around town from groceries to newspapers. Things to do and things to stay clear of! She reassured us even more about the PHS donor offers we may her in the future. Some of those organs are better off than the DCD donors. Anyway, how amazing that she stopped in. Jane in Houston did that too when we were in the hospital or she would always call and check on Kevin. These people are amazing! I’m alone here and if I thought about it long enough I could cry but the staff are so personable. Even walking to find coffee downstairs (every machine on all the floors we were on are “broken” which I found out today they just all need refills) there are friendly smiling faces everywhere. I feel bad for my first thought of this place when Dr. Galati ever mentioned it a few months back! :0
7:00 Julie NP from transplant came in. She’s on through the night. Super nice and friendly. She examined Kevin and went over all that is happening. So far still waiting for picture to come back.
Tuesday August 22, 2017
Answers to questions:
I noticed labs were cancelled for this week and wondered why. She said that after seeing him they said monthly labs and visits to clinic every two weeks until he sees Dr. Tyson. After that she will decide if clinic visits can go to monthly.
I asked if she knew our current place on the list. She said he is #10. And she could see some of the ones above him are pretty specific type needs and she reminded us that Kevin is a “better surgical candidate” than most.
I told her we turned down a back up offer and asked her all about that liver. She said the primary center actually accepted that one so it went to them and had we accepted back up we wouldn’t have gotten it. I told her it was an emotional day and really we need more information and clarity on those PHS donors. She said this one statement that gave me a huge sigh of relief: Ochsner has a Zero disease transmission rate with those donors and typically those donors are very young and healthy. Anything they tell us during the call for an offer is treatable on a temporary basis. I asked all kinds of what if type things especially after reading up on different diseases that make a donor PHS and said would we want to be careful with Kevin if they stage of the disease was in one that could do more harm to him as an autoimmune patient. She said the procurement surgeons decide when they see the organ and once they test it if it’s viable. So I’m assuming that if the “disease” was in rough latent stages the organ would most likely not be transplanted. I told Keith it’s like my mind goes to some dark alley with surgeons saying well here’s an organ let’s not waste it. When actually they never do! Of course they are only going to transplant what is transplantable! But I’m a step away from that back alley mentally! I’m just not medically inclined enough.
I asked for further clarity about different centers and back ups. She said Tulane is a transplant center. So the time we were back up for a different center she said it was fine for us to be at the apartment. We were close enough and they do that all the time.
It was so good to talk to her. She is arranging a meeting time with us when we come Thursday for appointments. She has some good reading material which goes into more detail for us she said that would help us.
August 20-21
School started today! Keith and Caleigh face timed me and I got to ride along with them to drop her off and pray in the carpool line! Kevin has been in some pain the past couple of nights. We are watching him very closely. I don’t even want to count how long it’s been since his last stay! I love how the Lord is keeping him stable while we wait.
Sunday morning he awakened me at 3 am having not slept at all and was needing nausea meds. Then at 7am I was awakened by a call from a coordinator with a back up offer. This one was a PHS (public health service high risk) the donor tested positive for syphilis. And we turned it down. We haven’t had one of those types yet. We haven’t said no to any offer yet. We are allowed to. We don’t lose our place on the list. And in church yesterday Pastor Jaime spoke from Psalm 78 how good God is and yet how quickly people forgot. And this verse hit me: “Yea, they spake against God; they said, Can God furnish a table in the wilderness?” Psalms 78:19
I don’t know if I can explain my heart here but at 3 am that was one of those cry out to God moments again for Kevin. I absolutely don’t know what else to do when he’s experiencing such symptoms and I just go back and climb in bed??? It’s a struggle for this mama! So sitting in the church pew it hit me. Did I doubt Him? Was this the table He was spreading in our NOLA wilderness? Even though we made the unified decision with Keith, Kevin, Tiffany & Ruth… and had peace about turning this offer down, I was taking it all in on the pew. I was feeling for that donor and ended up an absolute mess. It’s never good when your tired and weepy. Pastor’s oldest son and his wife prayed with me across the pews after church. I wasn’t close enough to the exit to get out without making eye contact:)
I need to call our Houston coordinator and ask random questions we have. I feel like we made the right decision and we were tired and it’s so hard to see Kevin hurting. I know that there is NOTHING to hard for God! I am asking Him for a pristine liver for Kevin and complete peace about the offer if it’s anything but. So many are praying this for us. And after a good night’s sleep and several calls and texts from family and friends I’m not as mental. Or am I!?
August 17-19 Back Up Again!
Kevin had a rough week. It seemed like maybe he was brewing another episode of cholangitis that may need a hospital stay but it kind of passed. It turned into a three day back up of which we are forever grateful! (It’s why we are here!) This time around they called Thursday mid afternoon offering us to be back up to a standard brain dead donor. They said continue to eat and drink because they didn’t know times yet and it could be tomorrow. Friday at 4pm rolls along and we still haven’t heard another thing so we made the call just to check. The coordinator said still no news and that because they were one of the earliest to know it’s a longer wait because they are trying to place all of the organs from this donor. That made complete sense. She gave me the name of our on call coordinator and then said she was on for the weekend so we at least knew who to ask for. By 5:30 pm the on call coordinator called and said the donor surgery starts at midnight so Kevin cannot eat or drink from that moment on. She also said this organ is at another facility and we could “wait” at the apartment instead of going into the hospital. They would call us if we are actually needed since we are 30 minutes away or when we are cleared. I asked since it was at another facility didn’t they want a back up at that facility? She was like oh no we know where Kevin is in the line and he’s the back up…and we want to get that kid transplanted! Well ok! I’m literal as well as visual so I’m actually needing to call our actual coordinator and fill in the blanks in my mind here! (Because my mental confusion can’t hang with with the rapid information they give in the phone call and we’ve hung up before the fog lifts!) We always learn new information with each experience. So we waited for that next call… we’ve been working on a 2,000 piece Star Wars puzzle so we actually did that between family calls (we watched through face time Bailey eat some green beans!) and watching videos of Caleigh’s exhibition Keith sent from Friday family Fudrucker band night.
I will say we are tired. And I can’t say we have done anything physical but the mental and emotional side is draining. As much as I try to dismiss it. It just is. At 5 am Saturday morning we got the “we are cleared call” and that means Kevin can eat and drink because they placed the organ. Last night he said let him know when they call thinking it would be earlier in the night because he said I want to wake up to eat! He went to bed hungry. But by 5 am he said he was just so tired he would eat later!
This is normally an emotional time of year for me with all the back to school happenings. I have so many friends sending kids to college, I’m sending a kid to college again Monday! Cole starts Grad school at UTSA (Univ. of Texas at San Antonio) and Caleigh starts HIGH SCHOOL! I cannot tell you how weird it was to see in the video Keith sent of HER marching on the band lot to an actual set and pattern! She was my number one band fan when we followed Kevin’s tuba playing for 4 years at Oak. It’s just so weird. It shouldn’t be her. But it is! And she LOVES IT!!!! And that makes me so happy! I love when she face times me after practice and the happiness just exudes! I’m thinking not me. No way would I be happy after hours outside in the heat! I’m also not musically inKleined:) I would have a heat headache and not be friendly!
Kelly called earlier this week and asked who is making the pancakes on Monday?!? I love how different people in my life know me so well that they are thinking of us at this time in ways like that! So, I prepped Keith on this! I said just be glad you are not making a panther paw! I said she is the Hurricanes! You can make a mess of it and say GO CAINES!!! (School is named after former superintendent Jim Cain so I will forever struggle with which spelling of Cain?! *Cue the veggie tales singing the homophone song here!) But I said for the “cuteness factor” keep them round but when you “plate” them, swirl the syrup around the pancake to make it look like a hurricane! (Here there is even greater discussion as to which way the hurricane swirls in the Northern and Southern Hemisphere I learned on a neighbor hood Facebook group {!} WAT?!)
I’m thinking I’m picking up Blue Apron lingo here! We have now had two deliveries and it has been the best thing! So far only one side dish we both decided we would never eat again but everything else has been delicious! (Not a fan of Korean rice cakes with “insert weird mushroom name here!”) It takes up time and is right up Kevin’s foodie alley! Now to feed that boy some breakfast!
Thursday August 10, 2017
We got a call last night to be the back up for a standard donor with the organ coming from Florida. OR 1:00 pm today and surgery 2:30 pm. He already had labs and a doctor appointment so we were heading there anyway around that time. It was called off because the liver didn’t look good. So he can go back to normal activity. And that equals eating and drinking. This time the wait didn’t really happen since it was called off before the wait. But we did get ready. I have a bag by the door now and am thinking it’s not getting unpacked. That’s 3 calls in 9 days!
Finally, I had a cool way the Lord met a need today. We really have all we need. The basics. We are fine. I was missing a clock or two because I love them and they are everywhere at my house in Houston and a blanket or two. Well, a drawer in the dresser in the furnished apartment was broken. Came that way so — we turned it in and thought they would just come repair it. Instead, in they come with a complete dresser! When they left, I was putting my stuff back in the drawers and found that one drawer had an alarm type clock in it and another drawer had this perfect white bed spread type blanket! He met both of those random wishful needs for me and it made me so thankful to know He knows; He cares; He sees; He provides.
Tuesday through Friday
Alex visited and we had such a good time with him! We visited the World War II museum then stayed home a couple of days. Kevin wasn’t feeling great. His BILI was high again. He was “back up” again so couldn’t eat or drink but today before he flew out late we were able to ride on the Natchez Steamboat and take him to the Cafe Du Monde in the French Quarter by the loading dock for the boat tour. It was perfect for Kevin! He could sit inside and take in the scenes of the Mississippi River in the air conditioning. We played a lot of games and watched some movies. And poor guy. When I hopped out to tell him goodbye I was crying before I got around to the curb. I got back in the car and Kevin just looked at me and said, “He’s not even your kid!” It could be a mix of him leaving here and the fact that I know he’s leaving for college next week! Just trying to live that life verse of mine. Crying when people cry. Laughing when people laugh! Romans 12:15
Monday, August 7, 2017
Kevin wasn’t feeling great early Sunday morning. He had to take nausea meds and was about 99.5. He held his own and so far has rested and stayed out of the hospital. We’ve been absolutely blessed by so many texts, calls, packages and encouraging words! We feel so loved. Kevin met one of my Moms In Prayer mom’s earlier today. Kate treated us to breakfast in the Garden District. She got there on a street car! We ate at an authentic New Orleans lunch counter. Kevin thought that was cool. Our first blue apron arrives tomorrow for my foodie son! We are anxiously awaiting his great friend Alex Stayte to get here tonight and stay through Friday! We had a nice weekend with Keith and Cole and Caleigh who went ahead and stayed since they were pulling into the parking lot practically once we got word Friday that it was a no go. It was so good to have them around!
Also our transplant Coorinator sent us an explanation of DCD donor. We had a copy of the slide PowerPoint but it didn’t make it to NOLA. All the other books did. Here is how the slide we saw in transplant evaluation read:
“I tried emailing the powerpoint but the file is too large. The slide for DCD says this. ‘Recovery surgery harder on liver, but donors younger and healthier on average than other donors. Excellent outcomes in large series at Ochsner. May be offered before you get as sick. Survival very similar to livers from other donors.’ Basically, DCD stands for donation after cardiac death, these donors typically suffer from irreversible brain damage but might not be deemed “brain dead”. The donor’s living will or family will decide to withdraw life support. Once life support is withdrawn, the doctors wait for the heart to stop. Sometimes, the heart doesn’t stop and in this case the liver transplant will be cancelled and you’d be notified that “the donor did not arrest”. Which I think happened in Kevin’s case this past weekend. The slide says it’s harder on the liver and this has to do with the amount of time where the heart isn’t beating/perfusing vital organs. Ochsner has excellent outcomes with these types of donors and these are usually what is offered to recipients. As of right now, Kevin (and family), has agreed to accept DCD offers. This makes his offer pool larger (meaning he’s more likely to get offers more often) I hope this information helps! Jaimie”
Friday August 4, 2017
***Thank you for your prayers! It’s been an emotional day. We actually just received word that the transplant will not happen today. We continue to wait for His timing. We know it will surely be very soon! “But they that wait upon the Lord shall renew their strength; they shall mount up with wings as eagles; they shall run, and not be weary; and they shall walk, and not faint.” Isaiah 40:31
*I sent this explanation to a friend to explain more and will paste it here.
A more detailed explanation would be that the donor was a DCD “donor after cardiac death.” It’s 5 minutes after support is taken to “procure the organ”
This is unfortunately and fortunately what can happen. I know many things can stop the process. God has other plans. He has a different donor still out there! He’s in completed control! We can only TRUST Him. Only He can guide and lead in this way.
The surgeon was just in. Explained so much. Wow! All the more in awe of God and how anyone gets transplanted! It is a higher risk of being “called off” due to the specific requirements for organ procurement from this particular type of donor.
We. Got. The. Call!
5:47 am we heard from Alitza the transplant coordinator on call. She had an offer for us! She said he is the primary! I was awaken from sleep so it took a second for it to sink in. But she said at first we needed to be at the hospital at 7 and that Kevin could eat something light if he ate this second. He ate some applesauce.
7:30 admitted super nice lady. Came out and gave us both hugs.
8:30 in a room getting ready for surgery. Nurse is Janet. He’s having labs. Tests. And more tests. Janet said the times are these: 4:30 in The OR and 6:00 Cut time. Also she had to remind us that anything could happen. Even once he is under the surgeons could decide the liver is not a good one so it could be cancelled. We completely understand this and have it always in the back of our minds. We know it’s His perfect will.
9:30 She needs his advance directive from Methodist.
Room 1047 D elevators
Nurse talk: she’s been a nurse for 30 years. Janet. Her son was born on the exact same day as Kevin. She explained so much! Pain levels after surgery. Specifically to let them know if there is severe abdominal pain. Normal pain level should be between 0-6. He will practice with a blue card after transplant on preparing and taking all the meds. Sounds like they will be super organized. She explained the R word. Rejection. And not to be worried if it starts or anyone calls with it because they watch it close and keep an eye on it to catch it early.
10:00 Dr. Seal transplant surgeon discussed that we have a DCD Donor (the donor had major neurological brain trauma but the heart is still beating) they are very specific with these and in the past they were avoided because of bile duct complications but these days they are great. And have done hundreds of them.
10:15 Dr. McMann resident and she came in with all the consents. She explained also the donor specifics. Low risk. Hep B Core Antibody. CMV positive. Said his chest X-ray and ekg looked good. Surgery should take 6 hours. Waiting room is the 2 nd floor. There will be lines his neck and groin. Also arterial lines in wrist and groin. He should come out of of surgery round midnight. He will go straight to ICU intubated. With JP (?) drains. They are looking for blood. Also if hemoglobin drops it could mean internal bleeding. He will have a foley. And the incision will be a chevron cut. At about 5:00 am they will start weaning him off all things. He will be in ICU a day or two. Then he will be transferred to the 8th floor step down unit. He will also have an ultrasound of the liver after surgery.
10:30 Dr. DeGregoria transplant fellow surgeon. She said Dr. Seal and Dr. Sonnier who we met in evaluation and she will be in OR. Dr. Sonnier will start the case at noon. Which means they will look at it as soon as noon. She explained in detail about the Hep B. This donor has been exposed to that virus. The donor is cleared of all infection. No signs of active virus. It means extra meds for a while after surgery to make sure of no transmission.
11:30 nurse went over his lab results. She was impressed and all the people here are saying how quickly he will recover. Everyone is so happy for him. He has a personal best again on that BILI front at a 7.8.
*****OR time is now moved up to 3:30****
Pastor Jackson from the church here came and prayed over Kevin. Pastor Pope called in on speaker and prayed over Kevin. And our nurse after getting Kevin’s history sent a Chaplain to pray over Kevin. I came to the hospital with this song in my heart: This Is My Story This Is My Song Praising My Savior All The Day Long! And no matter what happens we will praise Him. We have perfect peace. We just continue to trust Him with Kevin’s perfect healing. Kevin’s remind band bracelet has Isaiah 40:31 “But they that wait upon the Lord shall renew their strength; they shall mount up with wings as eagles; they shall run, and not be weary; and they shall walk, and not faint.” Isaiah 40:31 and he is absolutely living it. Kevin is calm. Excited. Happy. I took a picture on the way here of the red light we were at with the Huey P Long bridge ahead and the time 7:22 am with the map of NOLA on the dash. Through the windshield there is a sunny yet rainy day seen. I told my family group chat that it describes this moment perfectly. Happy for this day. Hopeful for all it holds. Yet sad for the donor and their family. I asked Kevin in the morning while getting ready to come in my nervous chatter talking out loud did he think I should wear make up. Then I realized I needed to pray over him. He was sitting on a bean bag we brought from home just chilling. I knelt beside him and we prayed. I looked up after and wiping tears of joy said well I guess I got my answer! It’s a no make up kind of day. Words will never express how thankful we are for this gift of life. I’m really good. Then I’m crying. Then I’m really good.
Tuesday August 1, 2017
1:00 pm
Labs are rescheduled for 2 today. And I had questions for Jaimie so she called me and filled in some blanks about the back up process we just went through. When we got to the floor last night it was so late that really the place was empty. We roamed around looking for the nurses station and I told her the place was vacant. We took a wrong turn so once we found the station there were two people. The lady gave us a security band after we said we were here as back ups. (She didn’t seem like a nurse or anything. She looked really tired too!) The man asked if we found the waiting room and said they would call us back or something. We knew the on call coordinator said it would be 3-4 hour wait. She said that time of night that floor is quiet anyway so it did probably feel weird. She said they really don’t want to admit him so the coordinators all knew he was arriving and it was all behind the scenes and we did the right thing. But once we waited and waited and waited and had no contact with anyone I finally went back to that station and he gave us a timeline kind of. He said the primary was called back at midnight. So the actual surgery started approximately an hour and a half later. And he said once they take the liver off of the ice they usually dismiss the back up soon after. But the on call coordinator calls us to tell us we are dismissed. She explained all that to me because it can be a while and is different for each one. The surgeons take a jet to the organ and that timeline varies for the primary and the back up. Times are set by the procurement team. Once we got the dismiss call Kevin had already scoped out this vending machine that was refrigerated and he bought himself a lunchable! He consumed it in the elevator ride to the first floor! And I had a cheese pizza for him at home and we were excited to taste it and realize how much like Johnny’s pizza it taste like!!! (A place known only to north Louisiana people!) It’s called Theo’s Neighborhood Pizza. Well Theo we think you must know Johnny!
We need the following packed for next time:
•Two blankets!
•Warm clothes for Kevin!
•All the earphones in the house
(Something horrible was on the tv. I finally got up with my short self since no one was in there and turned it off!)
•chargers
•books
•small pillow
•flashlight or book light
We did pretty good for newbies but it was just really super weird. But the entire waiting room was ours alone so we may as well make it home! It was the coldest place on earth!
It’s 4:00 am and we are still here but got the call that we are free to go. He can resume regular activity. I had her cancel the 9 am labs since we are so tired.
At Ochsner. West Tower. 8th floor. Transplant step down unit. Waiting. We are back up. It’s our first time. We’ve been here since 11. Poor Kevin. He hasn’t eaten since we got the call. And he has routine lab appointment at 9 in the morning back here. I think Kevin is a brave and courageous champion! Taking it all in. Strongly. Quietly. Patiently. Holding his own. A friend texted me earlier that we will have our Phd in waiting! Indeed. Yes indeed we will! And sent these encouraging verses:
“Thou wilt keep him in perfect peace, whose mind is stayed on thee: because he trusteth in thee. Trust ye in the Lord for ever: for in the Lord Jehovah is everlasting strength:…Lord, thou wilt ordain peace for us: for thou also hast wrought all our works in us.” Isaiah 26:3-4, 12
Monday July 31, 2017
Jesus Jesus Precious Jesus Oh For Grace to Trust Him More…. this hymn was ringing in my head as the clock ticked down to leaving for the back up. That was 10:30 pm.
3:30 pm
We got the call to be back up! We haven’t even been here a week. When they offered it and asked us if we could be at the hospital at 11 pm I was like. Well, that’s what we are here for. We were seeing the Dunkirk movie so I stepped out when I saw I missed a call and ended up missing the end of the movie because I was getting all the information and settling down. They actually were so super chill. This particular time the donor is brain dead and they have a primary so Kevin is back up. He has to be “on campus” and once we get to the 8th floor in the West tower we may wait a while. Like 3-4 hours! From the moment we accepted the back up offer Kevin was not allowed to eat or drink. I told Keith and he was like go sneak him something! Lol! I told him he’s such a Troutman!
Sunday July 30, 2017
HOTX vs NOLA
Kevin hit the tired wall. He stayed home all day and rested. The family left in the afternoon and it was tough on me. The only thing that makes me laugh is how much they make fun of me for saying NOLA or referring to New Orleans Louisiana. They say it isn’t a thing. Like I made that up! It’s a thing! So Keith keeps trying to say HOTX or HOT-X! For Houston Texas. That’s going no where my friend! No. Where!
Saturday July 29, 2017
Copying a devotion from a book gifted to me “kindle wise” from Heather. I keep hearing from Him spot on every time I open this!
“Standby Time
With or without warning, there will be long days defined by laborious waiting. Waiting for a call, an update, or a result; waiting at home, in the car, clinic, or waiting room; whatever and wherever…waiting. Because of the unseen and unknown, waiting can be marked by adverse reactions, namely worry, anxiety or depression. Satan loves this worry-filled standby time because there is a lot of idle space for him to potentially move in to your spirit. Although difficult to do, one of the greatest efforts you can make is to replace this worry with hope. Hope in Him. For in this hope we were saved. But hope that is seen is no hope at all. Who hopes for what he already has? But if we hope for what we do not yet have, we wait for it patiently . Romans 8:24–25 from Canopy: 366 Days for Parents of Critically Ill Children by Anna Turner
July 28, 2017
We heard from Jane in Houston. Actually the caller ID gives me a near heart attack when I see who is calling. And even when I say hello to her I’m waiting to hear is it an offer! I told her and she was like oh my voice would be raised to an octave that only dolphins could hear if that were the case! She was just checking on us and reminding us we can call her anytime for anything!
Caleigh had to go to Hobby Lobby! It’s literally walking distance. She wanted to look at dress patterns. So we had fun doing that. Houston people who know how to sew she may have questions. Anyone in her contact list she may be face timing you once she gets her machine back. The girl who didn’t like patterns is now willing to try them! Can’t wait to see what she turns out!
We introduced Cole to Cafe Au Lait and beignets or what Caleigh calls sugar pillows!
July 27, 2017
This was our first day without appointments. We actually had to finally go grocery shopping. I looked up the stores in the area and we just decided to stick with Walmart Super Center! Maybe we will venture into Winn Dixie or BreauxMart in the future. Keith, Cole, and Caleigh are coming in tonight for the long weekend! We heard from Jaimie and she cleared up some appointment canceling and scheduling they are doing. I can see all this on the app but wait until it settles down before peeking at what is next. They want to see him every two weeks with labs. They also want a re check on labs so next week he has that. Mostly the white blood cell count. He’s typically low and it looks like his baseline the doctor here said but wants to recheck it just to see.
July 26, 2017
We had an appointment with the social worker team. They just started this for relocated transfer patients. They just want to meet and make sure once patients are relocated that they have all the support they need. They just talk. Get to know us. And they gave lots of good information for the local area. Also she’s a great contact for any questions. We got back to the apartment and absolutely crashed. It all caught up to us!
We also visited a church our church in Houston actually supports as a church plant here. It was a very good service. We are looking forward to going this Sunday.
July 25, 2017
•We got as far as Lafayette last night.
•Made it to New Orleans for labs then we saw Nanette the liver NP here. She is very nice. We like her! (She is the equivalent of Erin, Phuong, and Samantha in Houston)
•Heard from Jaimie (NOLA liver coordinator equivalent of Jane in Houston) and he is #13 on the list. Several people like 6-7 ahead of him will be skipped a lot because they are multiple organ. She said answer every call even blocked ones. It could be anytime.
•sat in the apartment for the first 10 minutes at 79° Someone had turned off the main switch! (Whatever that is) So, we’ve met maintenance and handled that problem!
•unloaded the vehicle and started the settling in process
•Feel truly blessed!
***they said when sending packages make sure to send “signature required” or they will leave it at the apartment door. And sometimes that’s not such a good idea. If we are not home they will accept packages at the front if they aren’t too large. Front office said it depends on the carrier. Sometimes they leave a slip with delivery window for another day.
July 24, 2017
We planned on leaving on the 25th in time to get the keys and move in. But Ochsner called and had an opening for Kevin to see the liver NP. Originally scheduled for next week. This is huge because they put him on “hold” until they see him. They just want to lay eyes on him. And the first available was a week away once we got here. So when we got the call that they had a cancellation we just took it. I love what a good friend texted me: “And YES, I totally believe you got this appt and no hold time. El Roi – our great God SEES you and knows exactly what you are going through and what you need. He sees. He truly sees YOU!!” To which I replied AMEN!!! And yes!
We left in a bit of a hurry. We did get to celebrate Tiffany’s birthday dinner. So glad to be surrounded by such a great and loving and caring family before heading here. Tiffany and Grant gave us the cutest clothes basket filled with stuff for move in! Bailey cracked us up. She has gone from guttural growling to high pitched squealing! But she’s so stinking cute! So we don’t care!
We are beyond blessed by beautiful giving people in our life who are stepping with us and encouraging us and lifting us up in so many different ways. We are overwhelmed with their generosity, love and care.
July 21, 2017
Apartment hunting. The first of the week I heard from Ochsner with a list of apartments to check out. It took most of a day to call and find out if there was a first floor availability for next week. Then we realized we just needed to look in person to have peace about the apartment. Keith and I left Wednesday and looked most of Thursday. I had several appointments already set up so part of the ground work was done. We narrowed it to three and by late afternoon put a contract on one! We should have known it was the one based on its proximity to Hobby Lobby for when Caleigh visits but still trekked through the day. There’s nothing like visually seeing, hearing, and smelling what’s around the place. Pastor also gave us a church to visit. So we drove the route to Ochsner and church and definitely love how close it is to the hospital. It is less than 10 minutes to get there and we don’t have to use major roadways. Because of our insurance we got a corporate but without bedding. They cover one number. We definitely could have gotten it for less had we done all the leg work but we would not have been reimbursed. We tried. So in the long run it will be easier on us! I’m for easy! We just need clothes, bedding, and food. Tiffany and Grant gifted Kevin a Blue Apron box that he will be thrilled to get once we move in. He already has appointments for Wednesday July 26 so we will relocate on Tuesday July 25. We need to get there before the apartment office closes so we can get the key and wait for a liver! All week He kept giving me peace about all of this and especially showed me through many protecting and providing verses that we are doing the best and He will provide and protect. Keith keeps telling me to make the most of it and it’s an adventure! I keep asking myself is this really happening? It’s just so weird. Face time and weekends when family can visit will be our new friends! —well, not gonna lie, Cafe Au lait and beignets will also rank pretty high!
July 12, 2017 Wednesday
Listed In NOLA!
We knew today Jaimie (transplant coordinator in NOLA) was presenting Kevin. We heard from her late afternoon that he was being listed! The first call was to inform us and field all our questions. Goodness did we have questions! We then called Jane (HMH transplant coordinator) and ran everything by her. So much we never knew to ask but pretty much both places are the same. Just at Houston Methodist Hospital *HMH they get the sickest of the sick and the MELD scores are higher. Like 30-40 in average transplant. Kevin’s a 20 NOLA 22 HMH. That’s all based on their most recent labs. Jaimie said it would be best to relocate because then we would be given more offers. Kevin was graded A by the surgeons as an excellent back up patient and primary patient. We spoke with Kevin first. Had a huge talk in our room with him because we know he voiced he wants to be transplanted in Houston. But he also wants his life back! We are dual listed. We can still get offers from both regions. I asked. We can be in NOLA Jane said and she could call with an offer and tell us to catch the next southwest flight back to Houston. We were glad to hear that because we didn’t want to like turn our backs on them here. And we didn’t want them writing us off because we were in NOLA! She’s like that’s why we encouraged you to go there! Everything we mentioned that THEY did she would reply with a similar yes we do the exact same thing. We just didn’t know because of how low Kevin’s MELD has been. For example when Jaimie called back once Kevin was officially on the actual LIST she said he is #14! I told Jane who I feel like all year I never knew to ask a number. Especially for his case. She said, oh, he has a number but we didn’t tell you because it’s too depressing! Here he is in the 300’s. They want him there yesterday! So, we are getting our ducks in a row. Realistically I can see us heading there the week of July 24. She was fine with that. I told her we needed to find a place to stay first. The social worker can help with this and in the education classes we heard several ideas.
Kevin can never be without a caretaker. For now it’s me with lots of support and back up for things here. We’ve been asked several questions and we honestly do not mind them because it helps us process it all too! And it makes me feel normal when I hear friends asking what I was concerned about. So that feeling I had before we heard officially that Keith kept telling me to get out of the sock drawer…was right! Even though it will all fall into place there are some details that need to be arranged! So, I’m staying in that drawer Keith! (For the record anytime we would have company come over. Family. Friends. Especially sleepover long term visits I would hear they were coming and start organizing my sock drawer and sweeping under the washer and dryer and refrigerator! He would always be so dumbfounded but it’s just the process I start with then finally end on surface clutter. He starts with surface clutter and we meet in the middle! All the while telling me to get out of that drawer!)
July 11, 2017
Jaimie called needing Kevin’s last scope. I feel like we have sent this twice already but in actuality I have only requested it twice and am not sure how it wasn’t received or included with other records. I called the doctor’s office who did his last EUS and had them fax it directly. I did ask Jaimie if she could see the fax machine:) So the report from Dr. Nguyen made it this time! (That was the one done in September 2016 and it was testing the suspicious nodes that so far have only been blood. Repeat and keep a close eye on but nothing to keep him off transplant list. )
July 7, 2017 Day Two of transplant evaluation in NOLA
Kevin is fasting for today’s appointments. He’s not eating or drinking all day and wasn’t allowed anything past midnight. He has 6:45 am labs (turn in beloved orange jug), 7:15 am ultrasound, 8:00 am X-ray, 8:45 am ECHO, 9:45 am drink prep for 11:45 am CT scan. Our coordinator will call and tell us where to meet her around 10:30 am. And that’s our day. They could add to it if they need anything. Caleigh is rocking the waiting room with a red Ochsner hoodie and sweet tart headphones watching mermaid shows on her iPad. Keith looks like he’s chaperoning on the bus trips we take: sleeping soundly while sitting straight up! This hospital does not even look like a hospital when you walk in. We all thought it seems more like an airport or a mall. It has a completely different feel about it. It does have a hotel connected called Brent House Hotel and an open concept. Valet parking is five dollars! I am reading all the material from yesterday. So far my favorite quote from the kachunked booklet is from Corrie Ten Boom–Worry does not empty tomorrow of its sorrow. It empties today of its strength.
Jaimie the NOLA transplant coordinator came and found us. Kevin was a little behind in the appointments because the first one took longer so it bumped the day. She gave us a booklet on getting around and settled in here. She wants to present Kevin next Wednesday so if we haven’t heard from her we need to call or message. I thought I had the app but Kevin saw me open it and said I was on the internet. So I must have saved the shortcut to the patient portal in my patient portal bubble of all things patient portal. She is finding out different things for us like do we need to move here as they see him getting nearer or higher on the list. There are a lot of people here from further than 6 hours away. Their transplant center transplants between 30-35 so this is the place to be for people like Kevin.
July 6, 2017
Ochsners New Orleans Day One of transplant evaluation in NOLA
5:00 am awake and get ready
6:00 am breakfast
6:20 am leave for Ochsner the rainbow guided us right to this place!
6:45am Park
7:00 check in for labs see people with orange jugs and wonder what do they have.
7:10am register for labs
7:20am Kevin is called back for labs. They take 17 vials and send him out with two cartons of diet cranberry juice which mom carried around all day because he didn’t really want them. Mom was afraid he may pass out. So she kept them for in case of emergency.
7:40am Check in for bone density test. He was given two pages of his scan and after Keith and I both read it we realized we knew less than before we read it. Have no idea what that was.
7:50 am check into transplant clinic. We “thought” we could have a free afternoon because nothing was listed from 8 to 4 so we knew we would slip away and come back at 4 for last test. Only… we stayed in exam room 5 allllll day. All. Day.
(Since we were clicking through appointments this next one I went back with Kevin and Keith and Caleigh stayed in waiting room. When we realized it was the see all transplant team I called Keith and said get back here. He walked in without Caleigh and I was like. Where is Caleigh??? He said he LEFT HER SLEEPING IN THE WAITING ROOM AND SHOULD HE GO BACK AND GET HER!!?? I’m laughing til I am crying over this! We are in New Orleans! YES. GO. GET. HER!!!! And Who Dat gonna leave my daughter in a hospital waiting room asleep!!!!) There’s another funny story about him not hopping out of bed straight at 5 am so Kevin could hop out at 5:15 but we will save that one. It makes me laugh cry too!)
8:00 am Kevin was given a goodie bag of before mentioned orange jug and instructions on said jug along with a small container. He is to give urine sample now in small one. And carry the other one around for 24 hours using it to collect urine and keep it refrigerated returning it at 8:10 am being sure to urinate one last time before turning it into the lab. So now we know what all those orange jugs are.
He was given a STACK of paper work to complete and periodically the lady would pop back in reaching her hand in for whatever paper he finished. One paper said vaccinations. Yikes! Cole came through here. No service in the room so my plan of all things digital was epic fail. But Cole found one shot record so he sent a pic. Kevin listed all vaccines we had or knew from that.
8:10 am Pharmacy representative stopped in the room. She went over all medications for post transplant and explained about how long each would be taken and how much they are. We have a printed list as reference in the file. (At one gas stop we saw an Office Depot and Cal and I walked in for a binder. Came out with a green flex file and organized it Thursday night quickly with the few things we brought. And glad to have it after all the papers and cards we got!) So much of this I know or am familiar with from my dad. You start out taking a lot of meds then they wean it down to one for life. In most cases. Almost every patient is rejecting the organ in the beginning but they adjust the rejection meds to keep it from going further.
8:20 am Financial lady stopped in. She went over our insurance plan. She is actually covering for Vanessa whose liver finance contact but on vacation. She answered lots of financial questions Keith had. Too bad he didn’t have his spread sheet. Basically we need to walk into Methodist billing department and have them file things properly. Our insurance covers transplant under a different section and this hospital files things in two ways. Personal: like stitches and broken bones. And transplant. All things hospital stay should be filed here and covered 100 %. Even on the way to New Orleans I answered a call from a machine telling me we need to pay some emergency doctor and we were turned over to creditors. They gave some long number and referenced an even longer one. Oh well. I didn’t write anything down. I figured it’s their fault for filing it incorrectly and we would handle that another day. I answered because we answer all calls! Until we get the liver!
8:30 am Nutritionist hopped in. She peppered Kevin with questions on what he eats and what is his diet. Dr. Galati would be proud cause his first answer was “2 gram sodium or something with high fiber!” She gave helpful tips on what is a low sodium item. Anything between 140-150 mg is usually low sodium but joked it was lettuce! She said anything below 200 is good. Usually no deli meat. Use lean cuts of meat like chicken or turkey baked instead and slice that. Also she said there were several Mrs. Dash low sodium marinades that are good. Use herbs and spices to bring flavor to food. Trade off. If you eat a higher sodium meal like chick fil a fast food then go easy the rest of the day. Other low sodium ideas is black label bacon center cut. (240 mg not bad when you need that fix) Tortilla chips that are 70 mg for 13 chips with fresh made grocery store salsa or Keith’s homemade.
She asked him what all he ate. Drank. Liked to do. Exercise.
9:00 – 10:00 am we left the room to go to another room to hear education of all things transplant. So very informative and we were given an entire kachunked binder including power point over info given. It was question answer and the presenter was a nurse and current transplant coordinator for A-N. 16,000 people are listed. 6,000 are transplanted each year. An apartment complex she referred us to was Levee Run Apartments after transplant. Hospital Stay is 5-10 days and we are to stay local for 6-8 weeks. They can get us in this place for all transplant patients very inexpensive. (Insert here huge plan needed for move in to that place day. It’s not anything we worry about now or once we get the call and are on our way to the hospital. But they will get us in but cannot get assigned a unit until discharge. I’m imagining a container of items needed to survive 6-8 weeks from pots and pans to linens and such.) They explained fundraisers and who to use to guide us if we ever chose to do this. Mentioning and reminding that funds can be tucked away for the day kids go off parents insurance. Or just to replenish travel expenses…)
The average wait time here is 3-6 months. They actually mention where people are on the list. Houston never does. I guess it’s a region thing. O is the longest list. And AB is the shortest with currently 5 people on it in the entire region. They may wait longer due to rare blood type. Kevin is O. Just because you are higher on list does not mean you are next. It’s all about MELD score and blood type. Even size and age are considered next. They get offers from all over.
If he is admitted to a hospital locally they want to know and may transfer him. They went into detail about when you get the call. We have 30 minutes to leave for the hospital once we hang up. Since we are 5 and a half hours away they will expect us in 6 hours. We go to admit or ER. Once there they send him to ICU or TSU. Kevin will be prepped for surgery almost before the organ is in the hospital sometimes it’s on its way. They discussed DBD, DCD and PHS donors. We realized once a body is pronounced dead the organs cannot be donated. There is a small window of time upon arrest and organ donation.
DBD- donate after brain dead
DCD- donate after cardiac arrest (heart stops before brain stops)
PHS- Public Health Service high risk
And some families of donors give a certain amount of time for things to take place and if it doesn’t happen then they respect the wishes of the family and sometimes those organs cannot be donated. So much to think about. We learned a lot more about organ procurement than we remembered.
Timeline of surgery was given: 4-6 hours after which he will have breathing tube and IV’s and drains and in ICU for at least one day. He will awake and know somewhat where he is at that time and that’s a good thing. They see signs of liver recovery as he wakes up. At least 5 days in the hospital and once discharged 6-8 weeks stay locally to make it to all the follow up appointments and labs. The first day after discharge is always a follow up. Tuesday’s is surgical follow up in clinic days. Once the surgeons have confidence in his transplant success they transfer him back to hematology doctors who follow him before sending him all the way back home. They said we could ask to be followed down the road closer to home but if we are transplanted at Ochsner then we are always their patient and can ask or call anytime even if they are not following him.
They mentioned a website we can check I think srtr.org to see the survival rate of all transplant centers.
They are gathering information and tests and will present Kevin within two weeks. We can call if we haven’t heard from the transplant coordinator by then. Jamie is our transplant coordinator here and we meet her tomorrow.
10:15 Dr. Tyson Hepatology she packed a punch. Questioned us and was very thorough. We couldn’t tell her if Kevin was cirrhotic. I’m sure we know. But at the time we were blank. We couldn’t even remember when he had a biopsy! But gave it our best guess. We sent all this stuff so I did not refresh and although tempted to bring “all medical records” as each reminder stated I chose not to. I did pull out the most recent ERCP for her to make a copy of. We explained all his hospital stays. Cholangitis. Pancreatitis. When we mentioned adrenal insufficiency she was not convinced. And my lack of info to reply wasn’t that great. Mom to Dr. Dr wins every time. Like all I know is they said his use of budesonide caused it so switched the steroid. But she said he’s on that for AIH. yes. It does both. I need to come back to this. I feel like they couldn’t ever truly test him because to be off steroid would make him sicker but he needs to be off it to check cortisol level. To see if he’s adrenal insufficient. She also said he could probably stop taking all medications. Why not? Was her reply. Because he’s already in need of a transplant. So. She seems concerned about the risk of what he’s taking doing damage while waiting for transplant. I don’t even know what to think of that. My first thought isn’t a good one. She must not be a mom. Let’s completely torture him already! He’s living in such a crazy life now. Definitely gonna go to houston with this thought. Already ran it by tiffany and we both think it’s like medical malpractice. Thinking like that why not pour alcohol down him too. That ought to put him in liver failure! She was nice and informative I’m just not familiar with her bedside manner and treatment plan. We’ve heard this place is aggressive! Now we know! In all that we did explain that his meds have gone from high amounts to low amounts based on his labs and settling down his system. She wants labs in the morning for vitamin levels. Today his MELD is a 20. Leaving Methodist he was a 22. She did say she would like to see two weeks on one antibiotic and switch to another one. Then switch.
11:00am Amy the Social Worker she questioned us without looking like she was questioning us then after folded the paper and paper clipped it. Friendly and funny. She squeezed information out of us by story telling kind of. Some direct questions. She asked here for the list of caretakers. She was satisfied with close family members and let us know that after transplant Kevin has to have a caretaker 24/7. And will for a good 6-8 weeks. Lots to put into plan here. Especially if we are NOLA transplanted. They may ask us to move closer as they see him creep up the list. They seem to be confident that they can tell when he will even be two weeks out. Another question for Houston. She needs to secure our power of attorney and advance directives we filed in Houston. That’s all she may need if she cannot pull them from Care Everywhere. Monday’s are labs. Tuesday’s are surgeon clinic follow up. Same as Houston asked how are you handling this. Kevin is a quiet soul. He replied his faith and prayer and my tears could not be contained. I didn’t keep up with who was in the room when the tears flowed but different people sparked them and all I could do was all I could do! And that’s let them flow until they don’t. Wipe and redirect. Wipe and redirect. Sometimes it just all catches up to you. They have been around this for years. They work in it everyday. It’s commonplace for them. It should be commonplace for us but some things just take it out of you. I know we have a friend in her and are able to reach out to her or her team at anytime with any question. She also kind of started a conversation I knew was out there but didn’t want to completely address that elephant in the room. She just point blank asked so what are your long term goals once you are 26 and are off your parents insurance. When he turned 20 in my mind I was like wow. 6 years. But that’s my timetable. And this lady’s now but not our wonderful faithful mighty God provider and King’s! When that panic grips I have to give it to Him. But she in my terms piled it on. Kevin did fine. He wants to go back to college. Get a degree. Get a job! It was time for lunch after this and we needed that break.
12:00-1:00 pm we meandered and found the cafeteria because we had to be back in “the room” by 1. Kevin sat down and said “I like it here and all but I really hope I’m transplanted in Houston.” Just a lot to take in. He says so little that I don’t want to over analyze that but boy could I!
1:00-3:30 pm was an eternity. I have pictures of everyone sleeping in this exam room but me. I was so tired I could have but just knew the ID or surgeon would hop in!
***finish this later Kevin wants to play a game!
Infectious Disease PA Jodi Hermes was in next and she quizzed us on vaccinations. She asked for a letter from his ID doctors in Houston clearing him for transplant. We are not completely sure why or who asks for it so I called once back to hotel and spoke with Rhonda the nurse at Dr. Feinstein’s. She said she would figure it out. Also Jodi wanted to know which pneumonia shot he received. Rhonda was able to find it. He had the Prevnar B on May 21, 2016. So he needs to get the Pheumovax 23. They want both. He also has no antibodies for Hep B (even though he was vaccinated) so he needs to start that series again. We opted to do that in Houston since it’s now, one month, and 6 months. She wrote a script for that.
Dr. Dennis Sonnier the transplant surgeon came in. He was young and very nice and knowledgeable. He gave us a little more detail of the actual surgery. Called it a chevron cut. Showed us where on Kevin he would be cutting and explained all that procedure. Asked if we’ve you tubed it yet. That’s a no. But Keith will now! He drew out a sketch of the liver and showed how it will connect. I asked if the bile ducts are toast because of PSC what will they do. He said they make that call once in and if so there is a procedure called the Rout and it connects to the intestine. I really am not 100% here. But there is a plan and a drawing in the file:) It made perfect sense when he was drawing it. He showed us a meld calculate website to use for MELD score. I have an app as well. He asked Kevin what all did he know about organ donors and explained those three initial donors again. (DBD, DCD, PHS) He asked him how does he feel about all this. Kevin’s basically said what he always says: I just want to feel better. And he does. I feel like first, he is a no worries kind of kid, second, we have a transplant survivor in our family, and third, he’s been educated this last year by world renowned doctors and nurses and medical staff in Houston. We could both get jobs answering phones for doctors offices on the weekend. Probably. At least liver doctors! This surgeon is one of many many. The team rotates. There are two in the transplant surgery. He said they get offers from all over. I asked why and he said because they hardly turn away an organ. They are aggressive and want to get sick people feeling better. Perplexing how confident they are. While in Houston we are not sick enough and here they seem to make me feel like we will be transplanted once listed in less than 3 months. They transplant at 25-28. Houston is 30-40 MELD. The question I asked was hard to get out because something was said somewhere today about once it’s “clamped” it has to be used. I asked more of the what if type scenarios. He explained that there are times when they have to go back in from leaks or blockages but they follow very closely. Sometimes the new liver needs thicker blood and they wait to see it produce bile. I really don’t know what I was getting at but just trying to link it all together. It was the end of the time at this room and we had a lot of wait time between them hopping in so exhaustion set in!
3:30 Kim from transplant sent us on our way making sure we knew what was next today and tomorrow.
3:45 He checked into EKG and was out in no time. No one could decide what we wanted for dinner so we all hit the hotel and took naps! Kevin is fasting after midnight for tomorrow’s appointments. The day starts early again tomorrow.
Hospital Stay 11 June 22 to 29, 2017
June 29, 2017
9:00 Samantha came in and said all the numbers are trending down. BILI is 6.1. She’s fine sending us home, but she’s getting with Dr. Seelbach and seeing if we can go home.
10:00 Seelbach said he’s releasing us! He’s happy with all the trending down numbers. He said the report from the ERCP was interesting and thinks the cholangitis triggered the pancreatitis. My thoughts: only it presented as pancreatitis so masking the cholangitis and revealing it in the ERCP. Yikes! We may need an FBI probe on the unmasking. Why it wasn’t revealed sooner causing me much less tears!😂 I think everyone is learning stuff and Kevin isn’t textbook anything.
This was an entire week in the hospital to the day. We thought he would be in for two or three this time last week. So… we are going home and going dark. (And possibly by the time we get home it will be dark! Hoping for express check out!)
June 28, 2017
Kevin needed pain meds and nausea meds last night. He felt warm and his temp stayed in the 99s. Other than sweating through a few times he slept well and long. The floor had staff meetings so we had a late morning getting things started. Win for a sleeping tired worn out boy.
10:30 Samantha just was in. Kevin’s BILI is 6.6. Up from 5.5 yesterday but it’s probably from all that poking around and stirring things up. She said good news is he will have a higher MELD score. I joked and told him it’s his personal best. Goodness. The marker we’ve had has been 5.8. It started all this. It was the number that flew him home from college. I’ve had to massage his head several times this stay and sometimes I ask him what has been the worst and best hospital memory. So far the worst was still a few stays back. Room full of family and crazy uncontrollable pain and maxed out on meds where they couldn’t give anything. It was the worst for me too. The best was two days ago. When we were offered the back up. Such a great moment. He shows very little emotion but both of these memories we all had tears. Painful tears and happy tears!
Possible go home tomorrow was given today all depending on tomorrow morning’s labs.
She explained the ERCP report. There were strictures above the stent so all of this hospital stay is brought to you by “recurring cholangitis.” And my panic when they wanted to take it out who cares! And that caused the pancreas to be set off.
Andrea came as a follow up for Dr. Nguyen from the ERCP procedure. Reminded us that he opened up the bile ducts that are beaded like a strand of pearls. Went over the report and showed us the sludged stent in the images.
3:45 Dr. Seelbach Not gonna let him go home w BILI this high. 6.6 today from 5.5 yesterday. He wants to push fluids to wash out the BILI. He joked and said it should be at a 4 and made a wager. He tried to slip Kevin’s recently acquired sour patch kids candy in his pocket! So he likes the blue ones. Good to know.
5:40 Dr. Galati and Samantha came by. He discussed his ERCP and they told us Kevin’s MELD score is 22. He told some good stories and chatted and as he walked out confirmed that it was cholangitis that made the pancreas mad. He really wants to transplant him but asked about when we go to New Orleans. He wants to know what’s going on! All Kevs liver enzymes are improving except his BILI.
June 27, 2017
Happy 20 Kevin!
You have been NPO all day. We are waiting for an ERCP. It’s 2 now and it was suppose to be at 1. It’s been special. All the nurses have been hopping in and telling and singing Happy Birthday. Jane brought books and a cake. Emil brought coupons for he cafeteria or Starbucks! The party will progress.
So far he’s still battling pain. He has BILI Dr. Seelbach says of 5.5. He’s trying to run a fever so this procedure to remove the stent and possibly replace it can’t happen soon enough! I posted an album on Facebook for him to look back on all his birthdays. Something to pass the time while waiting and fun times to remember.
Dr. Nguyen stopped by before the procedure and said he would not replace the stent. Too much risk for infection since it’s so sludged up now. He said he heard he had a rough night and all about the back up offer. He said that means we are close!
3:15 Kevin is in ERCP
3:40 Dr. Nguyen said he removed the stent. Did not replace it. Swept out the debris (sludge). He is recovering.
June 26, 2017
9:30am
Over the weekend in the hospital even though those here are the best care takers it is just not the same as during regular business hours Monday through Friday. Not all the resources are there. And maybe it’s because I didn’t exactly know how to tap those resources. So I started to feel left behind and fallen through the cracks. God used so many people this weekend to tell me “wait…,” but I’m just going to say I did wait Saturday and Sunday but with Kevin falling apart and in pain was to me, long enough!?! 🙂 :0 🙂 But what I didn’t know was behind the scenes what was happening until this morning. And all I can say is…Lesson learned!
•Naomi one of the charge nurses stopped in. (She calls Kevin “Kevs”) She told us the story of how hard everyone worked to get Kevin in last Thursday when all the beds were taken!
•And I almost refused Dunn 10. Like who are these people and don’t they know!? We are Main 7 people. It was Dr. Carbajal. Jane. Naomi. And Dunn 10 charge nurse we met once in. Who knew.?!
•My 💜 is full again. We are loved. The weekend at the hospital is you get what you get and you don’t throw a fit❣️(this is hanging in my house and I still throw an inward fit a time or two.)
•And Jane just called. She had so much to follow up on. Explained his current numbers. His amylase is 192 and Lipase is 272. (It’s the amylase that has to be under 400 to get transplant offer. Good clarification.) She said his cholangitis is most definitely causing this. It’s a catch because auto immune is causing that:) we are scheduled to see them from previous follow up Wednesday the 5th before going to New Orleans. She said if he’s feeling fine skip appointment and head to New Orleans. If not keep it. She will call us Tuesday. She also asked what cake flavor he likes. He turns 20 tomorrow and they want to stop by. (Made me cry after hanging up)
•Kevin is asleep now since his pain shot. I told her we caught this early. She said yes we did and was glad. But I said he kind of fell apart over the weekend. Thursday even seelbach said how good he looked and what’re we doing here?! Just like that tiger Carbajal described. Everything’s fine and then BAM. She said seeing the numbers where they’ve been she can’t imagine what he’s had to endure. |Poor Kevie.|
•The nurse brought consent papers to sign for ERCP and I told Jane I guess Galati team knows. She said most definitely.
•I asked where the stent was placed and she said that she didn’t have access to those images but is a good question for them. I don’t know why but when they said Friday that it looks like the stent isn’t doing its job and let’s take it out it made me panic (unsettling). But what do I know?
•And anytime I have questions we are to call her. Someone answers on weekends and fields it. Certain people are on a list to call her if called. Or something like that. And we can call Galati office answering service and one of their nps will call. Good to know. I’m always like well we are in the hospital already! But she said sometimes you do have questions when no one is around. So call.
•Jane also said he’s not having full blown pancreatitis. Which I remember Dr. Galati saying last time and at office visits. It’s labeled that and all but it’s not full blown.
11:00 am they came and said Kevin is NPO for tomorrow’s procedure. At least he got full at breakfast.
Noon: A very exciting thing happened here between 12 and 1. We were wondering why NPO because usually an ERCP he can eat up until midnight. Two different NP’s were here one from Galati and one from Nguyen and as they finished up their exam and visit Jane walked in. Our transplant coordinator. She said a very nice O+ lady is on the operating table getting a great O+ liver but they cannot get her to stop bleeding. So if they can’t get her to stop she will be fine but they will stitch her back up for another day but that liver could be going to Kevin! She said it was a very very very long shot. I had tears. I looked and Kevin’s eyes even looked teary. She said to go about our day and we would know something for sure by 6 if not sooner. Wow! Kevin and I were praying around 12:45 for His will to be done and as we were praying Jane walked in saying Kevin could eat. They were able to get the recipient to stop bleeding. Which is an amazing thing! We are so awed by this gift of life program that we have no words but thanks! Jane said she couldn’t think of a better gift for Kevin’s birthday. After she got it all out she got teary because she wanted it so badly for us. So we gave her huge hugs for all she does for us and how much she cares. We continue to pray for the lady with the new gift and for His perfect will for His healing for Kevin. It will happen in His time!
June 25, 2017
11:30 Kevin slept well, and once asleep the pain was managed. He took pain meds at 8:45am tablet then 10:30 a shot: 5 pain level. We streamed his church from college and watched service this morning. He is napping now and we are waiting for doctors to come through. (So far it’s been their PAs and they basically are just checking on Kevin. I really don’t feel like asking them the questions I have because well. Just because. Unspoken and unwritten is sometimes best!)
3:30 He’s had to keep on the pain med schedule so I’m not really keeping up with is like yesterday. But Dr. Carbajal came in who knows Kevin and I hit him with my questions! He answered them left and right. He does not think Kevin is pancreatic insufficient. He said basically he isn’t following that textbook rule of complaining after and during meals. But not all patients follow that rule. He said its hard to tell if it’s the autoimmune hitting the pancreas but he highly thinks it’s the bile duct recurring problem especially where the bile duct enters the pancreas. So when the bile duct is enraged and inflamed it causes the pancreas to be. So possibly that stent needs to be exchanged. The stent was scheduled for replace and exchange in August. He said it could just be getting gunky. (Sludged up) As for the pancreas he compared it to the tiger at the zoo. Sometimes it’s just so settled and happy then the slightest things sets it off. Bowel rest is absolute best. He said it’s a good sign when he is hungry. Good sign. Kevin is hungry on full liquid. (Cream of wheat and chicken broth full liquid). I asked is this chronic or acute because he keeps having it. He said it’s like acute in top of chronic. He said most liver transplants are connected at the common bile duct. I guess that can wait until when and if that happens. I’m sure if it’s not a good connection then the small intestine place will be back up like Dr. Nguyen said happens with most bile duct diseased patients. His levels are coming down a little so he was encouraged by that. Cole and Kevin have the switch fired up again and he was really encouraged to see the controllers out. He said that’s always a good sign. Also I asked about if it is the autoimmune hitting the pancreas and he gets a transplant what will cause that not to keep happening. He said the new liver will relegate that and it usually will not happen. He did say it’s common for newly transplanted patients to get pancreatitis. And the treatment is the same.
June 24, 2017
Pain meds close to midnight last night. Then again at 3:00, 4:30 then again at 7:30 and again 9:45. He is looking very yellow. I am not liking the trend today of this pain. Somehow we haven’t seen anyone from Team Galati and we have questions. Hopefully someone will still stop by. Or for sure tomorrow.
3:30 Carbajal just came in and said keep the diet the same for now increase the amount of IV fluids per hour and just see how the numbers go. (Kevin texted because I got my car out of valet, dropped Cole at RMH, and parked in a cheaper garage)
9:00 NP for the hospitalists came in. Laura is her name. She was checking in for them. Helping them out. She said the numbers were still >600. I asked why we can’t get an actual number and she said once it’s above normal range some labs just record it that way. I told her I was only curious because we came in 850 so wanted to see if In the last three days any of the >600 were trending below. She was super approachable and encouraging and kind!
6:30 am
From Tiffany on why does Kevin get pancreatitis (with pictures!)
From Tiffany on why does Kevin get pancreatitis (with pictures!)
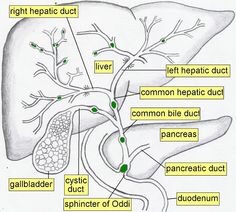
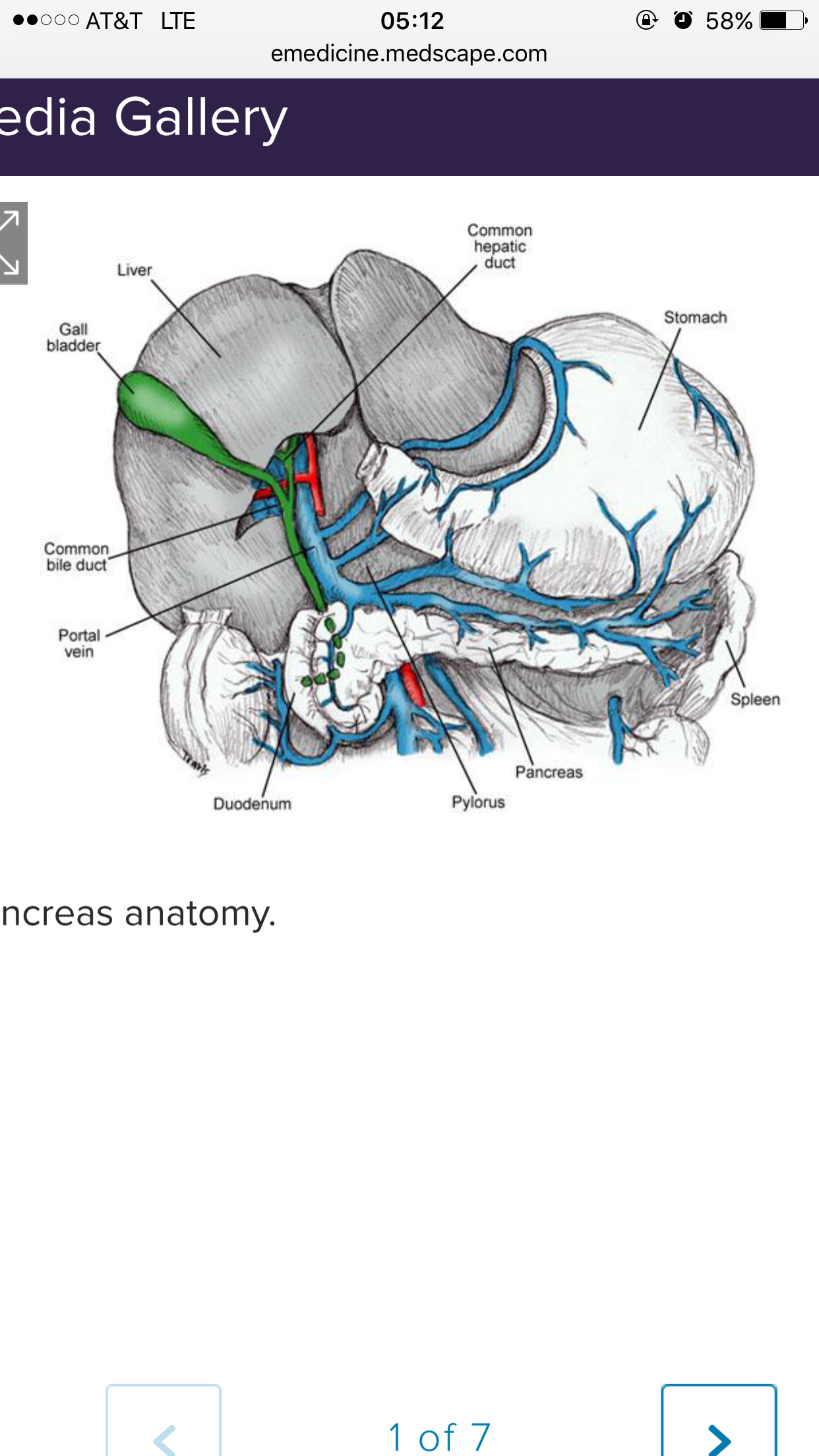
Why does Kevin get pancreatitis?
The pancreas releases several enzymes (amylase, lipase) and hormones (insulin and glucagon) to aid in digesting food. Any kind of blockage in the bile ducts obstructs the flow of digestive juices from the pancreas. There’s nowhere for these digestive juices to go so they get trapped in the pancreas and start to kinda digest itself- causes inflammation. Anytime you eat, the pancreas (along with the gallbladder) gets stimulated to release enzymes (from the pancreas) and bile (from the gallbladder) to help in the digestion of the food. That’s why Kev gets hospitalized, no food, and IV fluids only to stop stimulating the pancreas to produce these enzymes that are just getting trapped. No food = No enzymes. Unlike the liver, the pancreas cannot regenerate itself. That’s why it’s so important to get this thing treated and nipped in the bud before it starts creating scar tissue in the pancreas. I’m not worried about permanent damage in his pancreas because of his blood sugar levels. He’s never had “diabetic issues”. Because the pancreas releases insulin and glucagon (a form of sugar), if it was permanently damaged then he’d basically have symptoms of diabetes- and need insulin shots to compensate for the pancreas not being able to get that insulin out. And that’s not happening 🙂 so that’s good.
As for why they say no transplant when you’re in full blown pancreatitis … I think it just has to do with the fact that all these organs are connected. Any kind of inflammation in any of the organs near the pancreas (gall bladder, liver, spleen etc) can trigger inflammation in the pancreas. So if it’s already inflamed, they don’t wanna make it MORE inflamed, leading to more severe possibly irreversible damage to the pancreas.
The pancreas releases digestive juices full of enzymes through the pancreatic duct. And you can see it’s connected to the common bile duct. Which is connected to the liver and gallbladder. So with Kev’s PSC, the bile ducts are being blocked causing the pancreatic enzyme juices to back up into the pancreas.
That “sphincter of oddi” is a little muscle (like a butt hole 🙂) that pushes bile and pancreatic juices into the small intestine for digestion of food.
I don’t know if that answered any of your questions …. I hope it didn’t cause more questions. Just read your blog and wanted to send you some pictures I found that made sense to me with all the connections!
June 23, 2017
9:00
I asked the nurse to call the doctor and see if Kevin could be given the next step of diet because he is hungry. He got full liquid but the food service was closed so we journeyed to the hospital cafeteria and got vegetable soup, yogurt, and apple juice.
7:00
Pastor visited and encouraged us greatly with these verses:
“I had fainted, unless I had believed to see the goodness of the Lord in the land of the living. Wait on the Lord: be of good courage, and he shall strengthen thine heart: wait, I say, on the Lord.”
Psalms 27:13-14
6:00 We are now in Main 7 room 786. It’s on the side of the hall that doesn’t have a shower. Kevin doesn’t care in the least but it does bother me. Maybe they will send us home sooner! There is a community shower across the hall. Makes me feel like a freshman in college again! I told one friend Dunn 10 was like the Marriott and we left that for the motel 6! We got here and the thermostat was on 90
5:45 Dr. Nguyen found us in Dunn 10. He said it looks like the stent isn’t keeping him from having pancreatitis. He thinks it’s his autoimmune disease hitting it. He said if we are still in here Tuesday he can remove it. Unless we want to keep it until after New Orleans. If you know me then you know all I was doing was focusing on not crying because I don’t understand any of this pancreatic stuff they’ve been slowly dropping on us. I mentioned I have questions and great concerns to myself earlier. And. Then the transport came to move us to main 7. Normal place we are use to. It’s good enough timing because I had to focus and pack quickly and load the transport. Once Kevin and I were alone in the new room, then I tried to talk about it with him. And definitely it is upsetting to me. Kevin just takes it all in. What is wrong with me?!? Just seepy. I need some questions answered and some good research in a quiet environment along with pictures of these organs in front of me! Topped with I don’t like what they are saying so I kind of don’t want to hear it. And it’s confusing. Can we just pick a lane and stay in it:) For the record Keith called and I told him all of the above and he was just mad! Said that I just need to wait and hear what Galati thinks. Lots of times these doctors talk off the top of their heads and are just kind of thinking out loud and Galati comes around and wipes that away or explains it a little better. So yes. I will wait.
10 am
Samantha NP followed by Dr. Seelbach
BILI 4.4, Lipase >600, LFT’s 5% lower
Added potassium. Seelbach asked how many times has he had pancreatitis. Said soon it could lead to insufficient pancreas (?) but we have a while perhaps. Never heard of that. He’s leaving him in NPO. Will let Galati decide when he can change diet. Waiting on labs from this morning. Last nights Lipase was still >600. He came in >800
Maybe I will research insufficient pancreas. Last night he mentioned it could be his autoimmune hitting the pancreas. I have questions about that too. And great concerns.
June 22, 2017
Late this afternoon we heard back from yesterday’s labs. And Dr. Galati direct admitted Kevin. I was happy that he made it through the night without waking in pain and having nausea like the night before but it was short lived. He was pretty flat lined. Tired. Not feeling well.
We are in a different wing of the hospital because the Main 7 floor we are usually on was full. They will move us tomorrow if/when a bed is a available. We are actually on the transplant floor in Dunn tower 1056. Pretty nice.
The doctor so far has ordered the routine set up for pancreatitis. NPO. IV fluids and IV antibiotics. Labs. Cultures. X-rays.
9:30 PM Dr. Seelbach came in. He’s just so funny. He said Kevin just looks so good! He hasn’t seen any numbers yet so he will treat him as pancreatitis for now. He hopped back in after texting the np to get the Lipase and it was 850 and total BILI 4.6. So he’s keeping him NPO and ordering an ultrasound stat. I think Kevin just doesn’t fit the mold they want to put him in!
June 21, 2017
*Fried sent this verse Tuesday evening who even knew how much we would need it in days ahead. (Added Saturday in hospital reflecting back on the week)
Psalm 123:1-2 KJV
[1] Unto thee lift I up mine eyes, O thou that dwellest in the heavens. [2] Behold, as the eyes of servants look unto the hand of their masters, and as the eyes of a maiden unto the hand of her mistress; so our eyes wait upon the Lord our God, until that he have mercy upon us.
My prayer tonight:
Lifting up my eyes to the Lord our Master. Looking and waiting for His hand to supply the need of a liver for Kevin. Waiting for His hand to move, be it Houston or New Orleans. Waiting for the blessing and the mercy of that answer to prayer for all of you.
Awakened in the night
Kevin tapped me around 2 am hurting. He was thinking its feeling like pancreatitis. He was at about a 5 so I gave him medicine for pain and nausea. He went back to bed and is still sleeping as I log this at 7 am. I’m thinking labs and a call to Jane today if he’s feeling half way better if not we go in for IV fluids. I am remembering Dr. Nguyen who placed the stent said it can be painful when the sludge and stuff passes intermittently through his bile ducts. (Or something like that)
June 19, 2017
Pray For Kevin
*** I was just about to post this remind band post when New Orleans called! Kevin will be evaluated on July 6-7!!! Such a praise!!!! Soooooooooo happy they called early today!!!!!!!!!!
**** looking at the calendar Kevin takes his last antibiotic on the 6th!
When I cannot fall asleep or am awakened in the night it is a perfect time to pray for what is on my heart at that moment. Many times I reflect on the remind band I wear always that our church’s Journey class created for Kevin. I’ve made up different acrostic meanings for each letter but in my mind they sometimes go away forever once I’ve thought of one in the wee hours of the night so I wanted to put the ones I remember somewhere and here is a good a place as any! (I am a random counter by nature like my mother in law is a random leaf drawer! She catches herself drawing leaves on her leg just with her finger so she’s not tatted up! But I count things. Doesn’t mean I remember the number and I recount the same things all the time just some things just look like they need to be counted! So I count!) I can always hop back here and add to each letter as my mental madness remembers and prays through them time and again.
P — Pray! Power to heal and Promise for hope of healing.
R — Remember: He remembers. He knows. He doesn’t have to be reminded. He named the stars. I find myself needing this because I think I’m reminding God what Kevin still needs. Yet. He remembers!
A — Almighty. Always. Amazing. Awesome.
He is an awesome God!! Great in strength and power and might. When we are weak he is strong!
Y — Yahweh. Name of God so holy. Yes. I have a prayer outline from our Pastor through His names and grab it many times and cry out to Him and praise Him!
F — Fear Not! Fight! There is absolutely no way to face any day without Him!
O –Overcomer
R — Restore.
K — KEEP. Keep asking. Keep seeking. Keep knocking. Keep circling praises and promises! Know.
E — Encourage.
V — Very courageous Very Calm. Very Kind.
I — Isaiah 40:31 remind verse!
N — Need need need a liver!
Non-shall! (A Caleigh quote!)
Here are some verses that pop in my mind as I lift him up for healing this way.
P: Pray for healing: “He healeth the broken in heart, and bindeth up their wounds.”
Psalms 147:3
Another one for P: “Come, and let us return unto the Lord: for he hath torn, and he will heal us; he hath smitten, and he will bind us up.” Hosea 6:1
R: he remembers “He telleth the number of the stars; he calleth them all by their names.” Psalms 147:4
A: almighty: “But his bow abode in strength, and the arms of his hands were made strong by the hands of the mighty God of Jacob; (from thence is the shepherd, the stone of Israel:) Even by the God of thy father, who shall help thee; and by the Almighty, who shall bless thee with blessings of heaven above, blessings of the deep that lieth under, blessings of the breasts, and of the womb:” Genesis 49:24-25
A: Almighty: “He that dwelleth in the secret place of the most High shall abide under the shadow of the Almighty.” Psalms 91:1
A: Almighty: “Saying, We give thee thanks, O Lord God Almighty, which art, and wast, and art to come; because thou hast taken to thee thy great power, and hast reigned.”
Revelation 11:17
Y: Most holy name of LORD God: Yahweh: “And God said moreover unto Moses, Thus shalt thou say unto the children of Israel, The LORD God of your fathers, the God of Abraham, the God of Isaac, and the God of Jacob, hath sent me unto you: this is my name for ever, and this is my memorial unto all generations.” Exodus 3:15
F: Fear Not: “Fear thou not; for I am with thee: be not dismayed; for I am thy God: I will strengthen thee; yea, I will help thee; yea, I will uphold thee with the right hand of my righteousness.” Isaiah 41:10
F: “For God hath not given us the spirit of fear; but of power, and of love, and of a sound mind.” 2 Timothy 1:7
F: Fight: “The Lord your God which goeth before you, he shall fight for you, according to all that he did for you in Egypt before your eyes;” Deuteronomy 1:30
O: Overcomer: “And Caleb stilled the people before Moses, and said, Let us go up at once, and possess it; for we are well able to overcome it.” Numbers 13:30
R: Restore: “And David said unto him, Fear not: for I will surely shew thee kindness for Jonathan thy father’s sake, and will restore thee all the land of Saul thy father; and thou shalt eat bread at my table continually.” 2 Samuel 9:7
R: “For I will restore health unto thee, and I will heal thee of thy wounds, saith the Lord; because they called thee an Outcast, saying, This is Zion, whom no man seeketh after.” Jeremiah 30:17
K: Keep circling: “And seven priests shall bear before the ark seven trumpets of rams’ horns: and the seventh day ye shall compass the city seven times, and the priests shall blow with the trumpets.”
Joshua 6:4
K: Know : “That I may know him, and the power of his resurrection, and the fellowship of his sufferings, being made conformable unto his death;” Phil 3:10
E: Encourage: “And David was greatly distressed; for the people spake of stoning him, because the soul of all the people was grieved, every man for his sons and for his daughters: but David encouraged himself in the Lord his God.” 1 Samuel 30:6
V: Very courageous: “Only be thou strong and very courageous, that thou mayest observe to do according to all the law, which Moses my servant commanded thee: turn not from it to the right hand or to the left, that thou mayest prosper whithersoever thou goest.” Joshua 1:7
I: Isaiah 40:31
“But they that wait upon the Lord shall renew their strength; they shall mount up with wings as eagles; they shall run, and not be weary; and they shall walk, and not faint.” Isaiah 40:31
N: Need: “But my God shall supply all your need according to his riches in glory by Christ Jesus.” Philippians 4:19
June 8, 2017
Follow up with Dr. Nguyen. He’s the best! He checked Kevin out at his office and scheduled a stent removal and replacement for August 16. He said his goal for Kevin is to keep him out of the hospital! He thinks the stent is helping keep the recurring infection down. The pain Kevin experiences sometimes could be “sludge or stones” passing intermittently through the stent and ducts. He’s on antibiotics too so that helps. He’s glad he’s made it three weeks. Kevin hasn’t been feeling all that great but he’s not in the hospital either! Keep an eye out for symptoms of infection: fever chills nausea. We spoke with the business manager too. Insurance stuff needs to be handled ASAP for them. So Keith get out your spreadsheet and check this one off. We need to call her back once we get things settled who pays what and what percent.
I told Kevin as we drove back that He sure has surrounded him with some of the absolute best of the best doctors! They are happy to see Kevin as an outpatient. This doctor especially since we’ve only seen him once as an outpatient. Every other time was bedside. He does all Kevin’s ERCP procedures. He was also happy to hear about us getting evaluated at New Orleans. He gave us a story about a kidney transplant patient who was called by Galveston with an offer. Very encouraging visit. Such nice staff!
Tuesday June 6, 2017
New Orleans called! We got two calls in the same few minutes. The Optum nurse on the home phone then New Orleans nurse Shelley on my cell. They have in my words deemed Kevin worthy to be evaluated! Insurance has approved it too. She went over a quick list of things they want to perform and have their own:
-abdominal ultrasound
-CAT Scan
-Bone marrow density
-Echo
-EKG
She needs better copies of these reports:
-EGD (mentioned Feb 2016)
-colonoscopy
-endoscopy
She is moving us along to Teone who will call in a few days to actually schedule him. She went over logistics with me. I mentioned getting a plane ride to New Orleans and she said it doesn’t help with getting more offers. We are still 6 hours away. She said at evaluation they will tell us honestly what they think. Like if moving closer would help. Not that we are considering that yet. We know we will miss out on some offers because of distance.
Once he’s evaluated, which should take about two days, it goes to committee to decided if they will list him. That takes another two weeks for the committee to decide.
•Kim Taylor the nurse with insurance called and spoke to Keith. The half a day he’s home between out of the country and taking off to South Texas! She gave him information about New Orleans travel reimbursement and answered questions about our coverage. Kevin spoke to her as well. Finally got to hear from her and I’m pretty sure we aren’t completely understanding her role especially since Keith asked some questions and she didn’t have the answers to. But it’s an answer to prayer that he was home and could field the call.
•today was one of those days before the calls late afternoon that I spent the early morning adding to my praise page and kind of trying to not focus on New Orleans and wonder if and when I should call them. So basically being a mental case without fessing up to it to myself which should have tipped me off that I’m actually mental! He knew I needed to start my day focused on Him and mostly rest. I did have that same random numbing feeling after hanging up the phone that I have gotten a time or two in the past just knowing that I’m hanging up a call from these health professionals. It makes me cry every time. Or really fight the tears! Hard to explain but just a lot to take in and every once in a while it catches up to me. So thankful beyond words to know that they will evaluate him! Just so thankful! Praising Him for His continued guidance and opening doors. And still completely trusting Him for Kevin’s complete healing. While wiping praiseful tears..
Labs May 22 and May 30
Jane called us with those numbers and placed them in the portal as well. His BILI has creeped up to 4.1 but the “pancreatic numbers” are lower. Not normal but lower. He’s feeling ok. I tell people so so. He texts me about twice a week in the night that he’s at a 5 and is taking a pain pill. He did drop this set of online classes because he missed too much from being in the hospital two weeks and wasn’t feeling well. So we met the deadline to get our money back and we will see the next session where he is. He also has been very tired. I am too! Sometimes I wake up and I know that I am me but other than that I have to get where I am currently very slowly! It’s funny but weird!
May 23, 2017
Follow up at Dr. Galati’s office with Phuong NP. It was a quick visit. Labs from yesterday LabCorp were a tiny bit elevated still. BILI 3.3 I did add since it’s been a while since we’ve seen her (Samantha is now the NP in the hospital) that Kevin’s BILI lives between 3-4. I said we use to freak out when it was in the 2’s! Just a little BILI-humor. His “pancreatic numbers” are lower than when he left the hospital but still considered elevated.
Dr Nguyen’s office called while we were here to schedule Kevin’s follow up visit with him from the stent placement. June 8 at 1:45. Reminder to actually find where this office is. We’ve been once. Mostly we see this doctor bedside. The stent should need to be removed and replaced in August. They usually stay 3 months.
She wants labs again on Monday. Then based on those they will be in touch. Ideally she wants Kevin to stay out of the hospital but smiled and said he doesn’t actually cooperate much here. She was happy to hear we are pursuing New Orleans.
Jane called and went over the lab numbers. His amylase leaving hospital was 235 today it’s 189. Lipase was 366 and today it’s 200. (He’s considered a good candidate for an offer as long as these numbers are below 400)
She is penciling him in on June 21/28 one of those days for a follow up in the transplant clinic.
Hospital Stay 10 — May 9 to 18
(I finally counted them! 10 stays in 14 months)
May 18, 2017 Thursday
It’s GO HOME DAY!
We saw Dr. Dinikar first and he broke the news that some of his numbers are creeping up. BILI. Amylase and Lipase. So he checked with Dr. Nguyen to get his thoughts. Dr. Galati and Samantha came through next and Galati dictated a text to Dinikar “Kevin can GO HOME!” We will see Phuong in Dr. Galati’s office Tuesday and labs on Monday. That. We can do! (Al three doctors are fine with us going home for the record.)
May 17, 2017 Wednesday
Procedure Day: we now know the ERCP is scheduled for 11:30. Dr. Nguyen will place a stent and if all goes well we should be home tomorrow or Friday.
We were awakened with the best and most encouraging visit from our Pastor. He read all of Psalm 34 to us and just truly encouraged us. We are so blessed to be so prayed over and cared for by our Pastor and so many others.
The procedure went fast! Everything was early. The same doctor performed this that has ever done anything ERCP wise–Dr. Nguyen said the following:
•main duct looked good
•he placed the stent as a trial
•it’s in a good position in case he does pass sludge or stones to hopefully minimize pancreatitis
•he did minimal activity in there he said smiling as Dr. Galati requested
•he swept debris out before placing stent
I asked what was causing the pancreatitis in his opinion. He replied two things:
1-sludge/stones can intermittently be dropping down causing pain or
2-an autoimmune problem causing pancreatitis and squeezing the bile ducts causing pain.
2:30 Dr. Dinikar and Dr. Lin
Dr. Dinikar (hospitalist usually one of three Kev sees while on the 7th floor) during his visit Dr. Lin–ID popped in. And we were just talking about what to send him home on antibiotic or not. So they could discuss what to do. Also they are both excited we are looking at New Orleans. Dr. Dinikar also had a chat about how is Kevin eating. He said he hates to say it but based on numbers now he is actually malnourished. He encouraged him to eat proteins and put protein powder on ice cream. Get fro yo everyday! Concentrate on proteins and fats and bulking up to be ready for the transplant surgery. Honestly we told him Kevin eats well when he feels well. He also said don’t try to run but do weights and bulk up. And…..if all looks fine then we go home tomorrow!
May 16, 2017 Tuesday
Today was basically keep calm until the procedure tomorrow that was suppose to be today but couldn’t get scheduled. So up until today the basic of this entire stay has been get him in. Cool him down. Get lots of opinions and think through situations. Get consensus from the entire team. Decide on an option. Wait for it to happen. So not many people hopping in today. We did however feel like we were in an episode of hospital room fixer upper! The Purell hand sanitizer dispenser for this room has been broken since we “moved in.” So if you happened to get in its realm it spit cleaner out on you or the floor. We would clean it, leave it, drop a wash cloth to soak the stuff. No complaints here. We had other things to bother with. But today. Someone else noticed it. Her name is called: The Charge Nurse. So in no time a worker was in removing it and moving it to a better location because this “said dispenser” has broken already twice they say. Once it was moved, there was a place in the wall that needed “patching.” And then a place beside that patch needed some “touch up.” So we took Kevin walking across the street and got us some food. By the time we got back one entire wall was being repainted! The paints didn’t match so…You know. Had to do the entire thing! So we took our food to the 7th floor waiting room. Adventure at its absolute best for a hospital stay! How much more like home can it feel when they start redecorating rooms we are in! Some of the staff wanted to be sure we could handle the smell. And didn’t want to be moved. Ummm how sad is it that a hospital smells like a hospital even with an entire fresh coat of paint on one wall. We did leave the door open for a bit… but other than that. We were pleased with the fix:)
Kevin signed his risk papers and he is ready for the stent to be placed tomorrow morning. Nothing to eat or drink after midnight. We don’t have a time. Just AM.
May 15, 2017 Monday
9:20 am Jane called
She had answers for the question when he has pancreatitis can he accept an offer? The two schools of thought have confused and perplexed us. She spoke with Dr. Ghobrial (transplant surgeon) about this and he said he would transplant a patient if their numbers were below 400. Keith had just wanted a value and even Dr. Galati said on Friday that the statement was too broad that “no surgeon will transplant a patient with pancreatitis.” I told her I realize that term means something different to each one speaking to us but it is good to have some clarity. Overall we still completely trust them to make that decision when the time comes. She saw Kevin listed on the schedule for an ERCP this Wednesday. Sometime today we will confirm if it’s Tuesday or Wednesday. (And Kevin’s says please be the sooner of the two!)
>>>we also asked her if we should have been alarmed that someone from surgery/post transplant stopped by. She said no need to be because they are trying to make it protocol to have someone from that team stop in when a listed patient is in the hospital.
10:00 Samantha NP for Galati stopped in. Wanted to know how his weekend went. She agrees with number for pancreatitis. Will check with Dr. Galati about the ERCP and confirm what day it will be on. So far he’s managing the pain but it’s still present. She said looking back at Kevin’s ERCP history it does look like it’s time for one. This is his longest stretch between them.
11:00 Dr. Nguyen came in. ERCP will be Wednesday. He tried to get him on the schedule tomorrow but couldn’t. He said he is fine staying here. And I asked how long will the stent be in place. He replied for 3 months. So if all goes well it will be removed and replaced every 3 months depending on,of course, how he does with it.
11:30 Dr. Carbajal
He was resting when he came in so he said let him keep resting. He was glad he was getting some rest. I did tell him Kevin is hungry but then for got to ask if he can move to soft food. But later our nurse called him and he approved it. Happy day!
2:20 Dr. Galati with Samantha
He wanted to see how all things moved along from Friday. Comparing from then to now Kevin said he’s feeling much better. All of his numbers are at baseline. We asked about the stent. He’s fine with having it as long as minimal contrast is shot up there. He feels sure Dr. Nguyen can be in and out with the stent without doing more harm. He reminded us and drew a picture on the white board of what is happening in the bile ducts. They are open to all kinds of bacteria and kind of hold on to it since his plumbing or drainage isn’t working. We asked if getting a stent has any drawbacks when being considered if a donor becomes available. He said absolutely not. And that they would probably pull it in all that process. He showed where the stent would be placed and where along the duct would they transplant. It’s about half of the new one with half of the old one.
4:45 Dr. Lin
She checked in on Kevin. She was glad to know he’s getting food. She said she asked last week how long will you keep this boy NPO! He will get Soft diet for dinner. Also she went over what Dr. Nguyen and all think that the stent is needed to help with the “back flow” of bile and the passing of “sludge” type stones and said to ask him if Kevin’s ducts are separate or together at the intestines. I completely understand it when they are saying it but then lose my train of thought when I go to write it up. Anyway. Hoping it will help keep him healthy until transplant.
May 14, 2017 Sunday –Mother’s Day!
8:30 am Dr. Nguyen stopped in. All of Kevin’s numbers are coming down. Even the liver panel numbers look good he said. He is sticking to his plan of a stent on Tuesday.
May 13, 2017 Saturday
Last night Kevin still had the look of a “sick” kid. His pain has been more manageable and he’s tired. Good news today the Lipase and amylase are both lower and in the 100’s. He actually said he was hungry. So maybe they will step up his diet to “full liquid” and he can get things like cream of wheat instead of broth. While grabbing coffee down the hall one of his nurses said if it were up to them to pick who gets the organ he would already have a liver! We want that perfect liver! So will wait…
11:30 Cleaners were here to mop floor and clean so I ran down to get a banana and milk. I walk in and it’s Dr. Nguyen! At least I didn’t miss him. He thinks let him cool down for now and maybe on Tuesday put in a stent. A stent in the bile duct because when he keeps getting pancreatitis the pancreatic duct expands and closes up the bile duct causing increased BILI and side pain. So he thinks the stent would help like reinforce the bile duct. He said he always thinks about a stent then talks himself out of it! I said we trust you!
11:40 Dr. Seelbach walked in to check on Kevin. He said his numbers all look good. And he thinks he can go to full liquids.
Friday
May 12, 2017
Keith sent this: “Samantha just came by… still waiting on pancreas numbers from labs. For some reason they did not run them or put them in, so they are getting those now. She was not sure of next step. She wanted to talk to Galatti and the team first. The ultrasound did not show anything with gallbladder or any other issues. Checking on bowel movement. That could contribute to pain if constipated. We shall wait….”
Dr. Carbajal just came by… labs looked better today, but contrary to how he is feeling, so stay on clear liquids. Wants to try alternating pain pills with iv pain meds because they tend to stay in body and last a little longer. Will talk to his boss and dr. Dang. Still wants to do ERCP as last resort
A little old man came by to see Kevin (Johnny McDowell??). He had a transplant 14 years ago and was just visiting everyone on the floor. Kevin was asleep so I talked with him. 🙂
“He need nutrition!”- Dr. Lin :)She listened to belly and said nothing going on down there. Will talk to Carbajal about adding to iv (all above came to me from Keith testing updates)
3:00 I was back today for this visit: Dr. Galati with Smanatha examined him. He definitely needs to make “poop” happen. He’s constipated. So they are ordering the appropriate things. We had a comical conversation including seeing his Ronald Regan socks to knowing substances that can make a rock “poop!” Just so glad Kevin isn’t in great pain like last night. We asked about the levels and exact numbers for when “they” say he’s too hot to handle with those pancreatic numbers. He said once again that shouldn’t be an issue and stuck to his guns. He said it was too broad of a statement. We just want the rules! Lol! I told them exactly who came by and told us otherwise. We may never know.
*i forgot to add he wants to know if Kevin “goes” tonight. He wants to be texted.
4:30 am Text from Keith: “He got some rest! Prayer and pain meds worked 🙂 He just requested some more pain meds, but the pain is not nearly as bad as last night!”
Late late late Thursday
***if you are seeing this please pray for Kevin to get relief from pain and great discomfort (in side and belly) that came on around 6:30 Thursday evening and continued to increase incrementally until we left. We had the nurse call the attending physician to let him know that Kevin took a turn for the worse. He had checked on him around 4:30pm and Kevin said he asked if he had gotten worse. I was out. Kevin wasn’t hurting then. So that is why I had her call. Like was he expecting it? Seemed like a weird comment for Kevin to tell me the doctor asked. Anyway. I know his numbers are back elevated and he is still only allowed clear fluids. That wasn’t what we wanted to hear. And Keith came up to let me go home and I texted him in the room so Kev wouldn’t hear that no way was I leaving. He replied what could I do:) Well sit and worry and cry all over him I tell you what! That’s what I could do! Before I left the nurse came back in with a report from Dr. Carbajal saying Kev could have one dose of “what Joey McGee calls Christian heroine” [kevin somehow knows this!] a diuretic to relieve swelling that seemed so visible to me, and heartburn type medicine. I was talking with Cole on the way home about Kevin’s swelling. Just wondering if all that fluid retention from IV everything is causing increased pain. The doctor cannot let him off IV fluids yet because of pancreatitis. I am most troubled by the timing of it all. And it started out in such a good way. This entire hospital visit is completely backwards! He came in feeling ok but with elevated numbers and now is having great pain after being in for three days. That’s usually the start transitioning home. I prayed over him with Cole, Keith, and Caleigh. I just couldn’t walk out without hugging and kissing his cheek and laying hands on him and praying for great comfort and healing! By the time I got home with the kids Keith had texted that so far the dose has helped and he is resting.
May 11, 2017
I forgot to mention that yesterday while we were out walking with Kevin we ran into Mary downstairs. She calls Kevin “my son” and hugged him. She was so happy to see him. Then this morning she walked in the room first thing to clean and just had a fit! She was so glad to see him on her first stop of the day and she hugged him and preached! She told us to not worry! God has a plan. He put you here for a reason and he will do it in his time! And how one day he will not even remember that he was sick! She is beautiful and so kind and happy!
After her talk our charge nurse came in and we ended up chatting awhile with her. She actually knew where I went to kindergarten on Guam! My boys thought I just made that up! (Carrie she is in your place in her big family. When I told her I was 6th of 8 she said: LUCKY! She was 2nd but the first girl.) She also wanted to know the story behind this admittance. I joked and said all the same symptoms he ever has are in a bag and it’s like he reaches in and pulls out one! This time elevated Lipase and Amylase numbers. She said she has learned as a nurse on this floor that the liver, when it has troubles, invites other organs to the “party” so they keep a close eye on all those other organ’s numbers. This time the pancreas was invited! Lol!
I’m sure the doctors will start rounding through soon enough.
11:15 Samantha for Galati
Ok. So much for numbers behaving and trending down. They were elevated again so they will not advance his diet. He will stay on clear fluids the rest of today. Per conversation with Dr. Carbajal they are changing up the IV fluids adding something with more kick (my words cause I don’t remember what else is in it) Which could explain the recurrent pain even though he’s had worse so for now it’s manageable. But. Stink. Didn’t want to exactly hear that but it is what it is. (Kellie says that all the time and I can hear her voice there)
1:30 Dr. Lin from ID stopped in. Listened and examined him. Explained old school and new school of thought w pancreatitis elevated numbers. Some say eat– feed them. Others NPO. When eating the pancreas produces enzymes that cause pain when the bile ducts are backed up so that kind of explains the pain. Eating … digestion enzymes produced by pancreas not working w bile cause it’s backed up = pain.
2:30 Traci an NP for the transplant Surgeons who will work post transplant hopped in. I had dozed off during Avengers and tried to be not a woke up! (Family words there) She was amazing. Sweet. Kind. Informative! Packed a punch! She said she wanted to lay eyes on Kevin. She explained so much. Asked a couple of things. And I said to myself and perhaps Tiffany last night that I haven’t even cried this stay. During her talk I had to reign it in a few times. Then she confirmed that from a surgeon’s perspective he is considered too hot now pancreatic wise (my words) to be transplanted if an offer comes around. She wanted to make sure he wasn’t needing ICU. I was like what is that tipping point? And I said this is where we would have to completely trust y’all. Hopefully y’all will make that best decision. She said so many eyes are on him and she cannot wait to get Kevin on the post side. Explained a bit about that. He will have a different coordinator post transplant along with 5 NPs who will live in his pocket for about a year and multi manage him. I cried when I asked about how if not now will it happen. Because this is the 10th stay since February and getting it to line up is just a miracle. I did say as a believer I know that I know that it will happen and He knows but in that moment the tears just surfaced because I felt disappointed that right now it’s a no for an offer today. Not that there even is one. I think I’m fighting my want to. And if I’m totally honest a little bit of disbelief if this is ever gonna happen. I asked her how many 19 year olds w AIH and PSC with pancreatitis get transplanted. 119 liver transplants last year alone so she said that many. They all come with something. But I feel like maybe I wanted it too much. I wanted her to be walking in saying we have a donor. Cause we have never met with this team before. It makes my wheels turn and I wonder why now. She said she will try to hop back by and also may tap Dr. Nguyen to peek on Kevin. All this writing and I still don’t think I’ve explained exactly the conundrum. It’s like waiting for a baby to arrive! Goodness. We have put in the 9 months for sure! This “delivery room” waiting is killing me! I’m am ready for that joy when this is behind us! I think if I could I perhaps wouldn’t have let her leave the room until she said Kevin was a good candidate. But I really wouldn’t want that. In this last few months we have wanted to know if he actually has pancreatitis when they say he has it because Dr. Galati has said he doesn’t and he wouldn’t be passed up. Galati’s words were you’d be in ICU and wouldn’t even cut your hair! I told Traci this. Threw Dr. Galati completely under that bus. I said Jane will reply no. Surgeons won’t touch him. Galati says yes he’s fine and I will make sure they know he’s fine and texts them in the room! But none of these questions are ever answered with all the players in the room so we have completely conflicting answers until today when I just point blank asked this lady. She said Dr. Galati is brilliant but no one wants to mess with a hot pancreas! She said it’s a tiny organ but you don’t mess with it! Hence. Tears. She said as a believer herself that she knows He knows. And it may be He’s saying I know Kevin’s donor and he’s not ready yet. So we connected on His timing and I guess my want to will have to fall in line at some point but possibly not before I have a “crying gag!” (Silently as not to scare Kevin!)
May 10, 2017
Kevin had a good night. He needed pain meds only once.
8:00 am he’s having X-ray of abdomen
8:30 am Dr. Galati & Samantha came in and were kind of shocked Kevin was even in. But at the same time not surprised and fine with it. I think the “team” has many members! Sounded like I was sitting in on a logistics meeting after they heard what brought Kevin in this time. He asked where we are with New Orleans and said they would be back by since Kevin was down at the X-ray.
11:00 Samantha hopped back in to see Kevin. Routine exam and questions.
1:00 Dr. Carbajal examined and said he could add clear liquids.
2:30 the nurse said Dr. Galati ordered an ultrasound so until that procedure hold off eating. (And we ordered broth. He’s gonna hate to miss that…)
2:35 Dr. Feinstein walked and and said he hates to see him here! He’s so funny! He meant it too. He hates to see him here. He saw the soccer game playing Cole and Kevin are watching and he’s not a fan either of Real Madrid. He said things were progressing well. Numbers are lowering. Maybe another two or three days. He said to ask about a helicopter at Ochsner because they do have access to those. He will speak with Dr. Carbajal.
2:50 left for ultrasound
The rest of the day was filled with visitors: Cole then Pastor … Pa then Baby Bailey with Tiffany and Grant! Brightness! He took pain meds just before falling asleep. And watched a lot of cooking shows:)
May 9, 2017 He’s Being Direct Admitted
Jane peeked at the labs:
4/26: amylase 101 Lipase 115
5/8: amylase 714 Lipase 1350
BILI 3.5 he’s been hanging between 3.2-3.6 on BILI. So it’s the “pancreatitis” levels that are concerning her. She called the team and said they want him direct admitted. She also called “our floor” Main 7 and the manager said no rooms yet but once one is available we will be called by admin. I think it’s a grand plan to wait at home for a room verses that hospital waiting area. No matter how many Pokestops I can get! Praising Him that he isn’t in a lot of pain either. If we haven’t heard by 4 today then Jane said call her again.
6:00 pm he’s in… 7th floor 754
6:30 pm Dr. Carbajal checked in and will start IV fluids and has him NPO to try to settle down the amylase and Lipase numbers.
I failed at IV placement detection. My first job in the room. She placed it practically in his elbow. Well. If it gets too irritating we can have them place it elsewhere.
May 8, 2017
Cole took Kevin in for labs today. I was able finally to go visit Magnolia Market (not sure what the official name is) in Waco! We were honoring a friend (who shall rename nameless) for her 50th birthday! I know the Lord rearranged all of our schedules for us to be able to get away for a girls day. (Even though the day started finding out a thief had broken into and rummaged through 2 of the 4 vehicles parked in our driveway. It’s all junk so they basically just made a mess. People said they were probably looking for guns. So many cameras all around in home security systems that he was seen in several neighbors cars! Don’t people know they are being watched 24/7) Anyway…late evening Kevin still wasn’t feeling well. So we will call Jane in the morning and see if she can take a peek at those labs.
May 7, 2017
Caleigh walked into church this morning and said mom, we have snack tonight, and I was like…. no that’s usually the first of the month or the end of the month. This is the middle of the month. So weird to feel like it should be the 16th and it’s only one week in this month… I looked at the greeter and asked what is today’s “Number!” And still was in a daze. But wanted to post a tiny update for keeping up with Kevin’s latest not so good days. Probably the last few days he has either been chilled with a low temp of 99.3 ish and no higher than 100.2 but has not felt great. He says he just does not feel good. Had a pain pill once only so far and has basically rested and completed last week’s online class assignments. I think he’s hit a wall. I’ve done laundry like a mad woman because I know we could be taking a trip to the medical center soon. I would like to think that it’s just a viral bug type thing. And it very well could be. He did make it the entire month of April without a hospital stay! The last few days his eyes had dark circles under them, very yellow when he pulls down the lids, and he doesn’t have much of an appetite. We are pushing fluids but he isn’t a fan of much of anything when he starts feeling bad. He wondered down this evening and seemed a little better. Maybe he needed a complete day of rest. We will see… I really loved April.
May 4, 2017
Tion from Ochsner called and said they received the medical records. How about that “fourth being with us!”
She asked a couple of questions:
•When was he evaluated in TX? July 18
•Is he planning on going back to school? Yes, taking online. We are flexible.
•Any kidney problems cause she saw all the various MRI and CT scans? I said no other than a kidney stone in the fall.
***She is giving this to the nurse and hepatologist, and they will look at them and decide. We will hear from them within two weeks. Horray they called!
May 2, 2017
Jane called and said she sent Kevin’s medical records: 6 cds and full reports to New Orleans Ochsners Clinic. This is the next step to getting evaluated there. I am so thankful she called to let me know as Kevin would say: the deed is done.
April 26, 2017
Dr. Galati and Jane in the transplant center
•”You’re Killing Me Smalls!” Kevin had this Sand Lot movie shirt on, and we spent the first 5 minutes discussing it with Dr. Galati. He’s never heard of it. So he looked it up. Will have to check back and see if he watched it ever!
•Next visit can be 3 months
•Meld Score is the lowest it’s ever been. 14. So I asked if New Orleans can tell us no!? He said no. They look at his entire history and Jane said he is a dream transplant team’s candidate. (Unless the region has a cut off limit and some do.)
•I also asked if things could be getting better on his insides. He said well who ever has the nerve to ever stop the antibiotics we will see! And that for better or for worse the antibiotic he is taking now is doing its job keeping the infection down. One way to relapse with long term antibiotics is building up a resistance. Dr. Lin from ID said she is happy with his first 30 of 90 days and to check back as he nears 90 days. We didn’t need to see them we just called in and spoke to the nurse who called back after speaking with the ID team.
•He asked about what online classes he is taking and how his physical activity has been. Kevin has been doing great. Driving again and all.
•Direct donation: we had heard about this but thought it didn’t apply to Kevin. Well, it actually does. But it’s a difficult topic to speak of. Basically we just spread the word that Kevin needs a liver. And then if anyone who is aware of the need knows someone who passes suddenly or tragically they can have their organs given to a specific person. And in our case they can say they want their friend or loved ones liver to go to Kevin. And believe it or not there are stories about people doing just this. Only thing is how to go about this topic of discussion. Keith says we most likely will not. But we do have the wrist bands and so many people already have texted me with different comments people make and it’s a type of organ donation awareness by asking prayer for Kevin. Dr. Galati and Jane said they have spoken at church gatherings or events about becoming an organ donor. If we ever have an event then he could speak. My kids already think I’m on the dark side when storms roll through or accidents on the freeway cause us to be at a standstill I usually comment that we may be getting a call because maybe some fresh livers may be showing up. They said watch out if I start asking your blood type and what time you go to bed.
•I just have to silently chuckle because he said there’s your wrist band: if anything happens to you I want your liver!
•And I have to mention here that Jane said the financial lady we met with at evaluation has been carrying Keith’s spreadsheet around drooling all over it wishing all the patients had one. It’s pretty intense. Color coded. But sense needs to be made of it all and sense is about to be! We have our people on it and they now have their people knowing to bill all things transplant to Optum. (Under United Health Care which we have for normal stuff through Keith) Optum covers 100% of transplant.
April 24, 2017
We received the letter snail mail from our case manager for insurance Friday. It was a cover letter stating at the bottom there were enclosures. Only. There weren’t. So we basically got a letter from her repeating everything we knew but with no document to sign even though the envelope was labeled “Time Sensitive Material”…. the level of misunderstanding and miscommunication along with frustration is increasing with each contact with them but after running it by Jane our Houston transplant coordinator she did say that case manager is the one who approves the bills. (Which to me makes this all the more ironic because Kevin wouldn’t have insurance without Keith.) Keith spoke to her and she said we should buy a lottery ticket because the chances of this happening is so slim! Then he came in with the mail today (Monday) and the “enclosures” were in! Good grief. So Kevin signed the documents stating we are his parents and anyone from Keith’s company’s insurance can speak to us about his illness. Which he’s had and been insured by said company since 2011. He turned 18 we didn’t hear from them. He needs a transplant and is listed at 19 we all of a sudden have to have their approval to speak to us. It’s a legal thing and we get it but I am not afraid to call it what it is: ridiculous. If you knew someone you didn’t want to see your private info then knock down all the doors and let them know. When you are us and you don’t care leave us alone. More people are gonna jump through hoops that are hiding things than those of us who are not. We just want him better — yesterday. Make them sign the papers. Turn the tables.
April 20, 2017
Celebration of Life
Kevin was asked to participate in this service of thanksgiving and remembering. We didn’t know what we were going to face but it ended up being truly inspiring. It was a little over whelming because neither of us knew very many people there. We recognized a few. It was a big crowd but once the program got underway and I kept telling myself not to cry I don’t know these people I ended up finding my Kleenex. The stories were amazing. The people in this room were so Kind–doctors, surgeons, nurses, caregivers, transplant recipients…they all had a story.
April 13, 2017
This is the last day of the 5th 6 weeks so summer is ALMOST here!!!
We had an email again from UHC RN to docusign the same document and before we even saw it she sent another email voiding it and stating she is sending it US mail. Good grief! Kevin will probably have a liver before our insurance gets approval to speak to us. Insanity. Absolute insanity.
April 12, 2017
The UHC RN with our insurance who needed Kevin to sign a release so we could speak to her sent it via email to docusign. Well, either we are idiots or she is because we would fill out the basic information then it would generate an error. Basic. Information. We all tried it. One hundred times. So very frustrating. I say face time us! We will show you he’s our 19 year old son and we aren’t some insurance thief trying to fraud out this liver patient! What is their reasoning behind such mistrust! I know she has access to our family health file and can see who we are. That was our one job today and we failed. Miserable. But her inbox tomorrow will show it. She gets a response every time we tried.
April 11, 2017 (***finally updated a weeks worth of all things transplant and Kevin.) I was ready to fax the forms yesterday when they were sent to us. I couldn’t fill them out fast enough! However, that part about insurance was blank. We have insurance and our insurance covers transplants and also steps them outside of yearly coverage under separate coverage so all things transplant don’t keep renewing each year. Keith has a spreadsheet. And handles this part. But when he sees how claims are filed sometimes they get sent back because they are not filed correctly. So we really weren’t sure what to put in the blanks for insurance. Keith said he’d call them today. So I gave him until noon. I called him at work and asked what did he have. He had calls out there and was waiting. Here is where another answered prayer happened because my anxiety of getting these forms over there yesterday was intense! But I also know I didn’t want to call United Health Care. I mean I would. It would be an ordeal. So I just said ok and hopefully they will return your call today!!! Another interesting note is Kevin’s current MELD score is a 20. It’s from his recent back to back hospital stays. They can keep that one until April 18th so I am really wanting Oschners to see that score! I say I cannot go through another hospital visit like the ones we just did because they were awful. Just awful. And he wasn’t sick enough and was so sick! As Dr. Galati said this is the life and face of liver disease: your life is tanked!
Keith called on his way home from work like he always does 🙂 but no new news. So we didn’t say or do much more because it was late. However, THEY called after hours! I was out and Keith who never sees calls actually got the call from our insurance. They needed to speak to Kevin to get his permission to speak to Keith because he is 19. But we have filled out and Kevin has signed 50 million forms giving us permission but this lady said our case is RED FLAGGED because he is 19 and they needed permission to actually call Keith back. If she only knew that we answer every single call that comes to any phone in our home or family. Once I hear it’s not a liver I let them know the only reason I answered is in case it was a liver. Then hang up and block and delete the number. Anyway. Huge answered prayer and another door slung wide open! Keith took all kinds of notes. The lady was so helpful! She said it was late her time so she would call back because she has more information. She wants to talk to Kevin. Sometimes she said something like regions call her with offers and she hasn’t been able to give us info because of red flags. I don’t completely understand that but it sure sounds good! She said we owe nothing and should always owe nothing transplant wise. Doctor visits are different. I listed her in my contacts so we would know. Goodness this made my night so now forms are ready to be faxed. As techie as I am I don’t fax. Never have. So Keith will send them at work tomorrow. It’s still a lot to get together. There’s an entire list of things needed but Jane has them at her fingertips. (Or at least I hope!)
The lady said the only hospital who has a problem with filing transplant claims incorrectly is Methodist! Of course! She said do not even worry about Oschners. They know what they are doing. And she spoke highly of their transplant center… she explained the regions to Keith and gave him some websites and told him about centers for excellence. I need to look those up.
Our insurance will cover Kevin and one caregiver up to a certain amount. So gas, hotel, etc is covered. This is a relief and an answered prayer!
We helped move Tiffany and Grant and baby Bailey across town during all this so it was a good distraction. I wanted to update this page but it really has been a lot to process. We will only go with His complete assurance that this is His plan for Kevin. And we are trusting Him and waiting on His healing of Kevin either right here in the medical center of Houston or 5 hours and 36 minutes away in New Orleans. Kevin is having good days. Doing online class work. I walk in and he’s making protein for breakfast and smoothies with protein powder in them and has a wonderful spirit. He’s picked up the guitar he got several years ago to kind of relearn. I love how creative he gets with his time. We mailed some RemindBands to the Big House today where he lived last year in college and Nina at the mail place just took Kevin in and said God will heal you. Bring me one of those bands! And she commented on his spirit. (How she picked up on that in 10 minutes of buying and packing envelopes I don’t know but it was a wonderful feeling for me.) I am so proud of Kevin. In precept today Heather mentioned how Moses wasn’t ready and took things in his own hands but then went to the wilderness for 40 years to tend sheep until he was ready for what God had planned for him. It was a neat picture to me for our situation. (And we are studying Acts and today mostly Stephen!) If we could control it…and my kids worry I might start taking out people with Kevin’s blood type (!) but not really. I would never. But we know God has a plan and know He has a time and when He is ready and knows Kevin is ready it will happen. It will be perfect. It will be beautiful. I just hope it’s not 40 years! Caleigh needed this pep talk earlier. She just had some questions and concerns and I am thankful her timing was when I had an analogy that made sense to her. I gave her Moses. Because today is precept Bible study day. And it was fresh on my heart. She wants him to be able to go back to college. We will get through this. Kevin will get his life back. That’s all she wants. (Little sweetie.)
April 10, 2017 Monday
I never heard from Oschners so I called them back. They called me back within a couple of hours. Teion called and gave me a list of things to do and look for specific forms in an email. Had me set up his patient portal. And had me send a picture of his ID and insurance card. She needed those to start the entire process. She rattled off all kinds of stats!
•we had to call insurance first. If they do not approve of this or are considered out of network we need to know before we go
•we must live within 6 hours driving distance or we will have to move closer *I looked it up later and from our house to their front door it’s 5 hours and 36 minutes! An answered prayer: Pastor spoke on 3 green lights when making a decision years and years ago. Peace in prayer, A word from scripture, and Circumstances or an open door. We keep asking Him to help us and guide us in this next step of being dual listed. All those three lights are brightly beaming!
•they need all records from evaluation at Methodist
•he can never ever what so ever come to an appointment without a caregiver.
•bring a list of other willing caregivers and make sure those on the list know they are on the list of approved care givers. They will call them. They need to be willing to come to New Orleans and support Kevin by taking him to appointments when we cannot. The social worker will ask.
•The entire process from now until being listed in New Orleans could take as long as three months.
•she sent an email for patient portal then an email with three sets of forms. Fill them out and fax them to her and to current facility.
•call insurance. Call insurance. Call insurance.
•got Cole to help print all the forms because my phone decided to not find the printer when it was in the exact same room and has always allowed me to print from it.
•we made it through this first step “calling Oschners” when I first couldn’t even imagine how one starts that process!
April 5, 2017 Wednesday
I made the call. Jane sent the number during the phone call in traffic yesterday so I took a deep breath and dialed Oschners. Where on earth do you start after they say hello. We were connected right away to exactly who we needed to be. (Krystal) She took our information and explained that a transplant nurse would be returning our call soon. I asked when can I actually expect a call back. She said if I hadn’t heard by Friday to call back. I thanked her and told her I appreciated her help because this is a huge step for us. She was really friendly. An answered prayer: direction and care and confidence
April 4, 2017
4:00 pm
Dr. Galati follow up w Erin
•our biggest question is should we get listed elsewhere. Before we could ask Dr. Galati mentioned it to us! Of course there is a tiny side of me that thought goodness is he kicking us to the curb! I was kind of hoping for a “not yet. Let’s give it some more time.” Instead he said: GO! Anyone who has been praying for Kevin recently will know even if you didn’t know what was going on exactly that this was an answered prayer for direction and guidance in his healing. So we start that process and he will have Jane contact us with information. A New Orleans hospital called Oschners is the next closest transplant center he recommends.
•labs next week– his albumin is extremely low (my thought the next morning was that lab was during the hospital stay that he was mostly clear liquid and full liquid… so protein level would be low normally???)
•follow up in 4 weeks in the clinic. And check in with ID after 30 days on antibiotic.
•we wanted clarity on the two different answers we got over the surgeons being hesitant to offer Kevin a liver when he is in the hospital or has recently been in. Dr. Galati said he would make sure the surgeons realize Kevin is fine and he feels that it wasn’t an issue. However Jane his transplant coordinator seems to infer that they are hesitant especially with the recent pancreatitis issues. They both differ here too. Dr. Galati doesn’t think Kevin is or has had full blown pancreatitis. While the transplant clinic is concerned. They are basically the same unit so it is perplexing the differing opinions. Which means all the more how out of our hands this is. We cannot possibly control any of this so it is a good reminder to wait patiently on Him and trust His plan.
•I had an entire folder of medical history that Tiffany dug up after giving Bailey’s doctor all our family medical history on all things liver. Well, I never even mentioned it! It was in my lap and I used it as a desk for my notes and once he mentioned New Orleans I was just not thinking straight again.
•He gave a very personal story about his sister back in the day needing a bone marrow transplant and she was in a different state and her husband could only come in every so often. The transplant center said she needed more support so after his family sat around her table he volunteered. At that time he said he left his residency and went and stayed with her. He said you get creative at times like this. And something in me knew that I needed to refocus. I had already teared up before this at the mention of New Orleans because as I told him we still have a 13 year old. Later when I told the 13 year old she said she would be fine and listed how many people she knew that we knew that would either take her completely in or help get her where she needed to be.
•he texted Jane while still in the room to reach out to the Troutman’s and closed with asking Kevin to do an extra effort on the nutrition.
5:30 pm When you have a 4:00 appointment in the medical center you are still in the medical center traffic at this time. Jane called and asked was it a good time to talk!? I was like well we are in traffic so of course! It was the absolute most informative call ever! Another answered prayer: understanding and clarity for direction. She said she would send us the number to Oschners clinic in New Orleans and asked if we had any questions. So I started in with them:
•How can we be listed and not live an hour away?
>>>She explained the Organ Procurement Team’s job and timeline. Yes, some donors have a more time sensitive dilemma but we would get offered the ones that basically do not. She gave an example of them getting notified of an organ donor available in let’s say Amarillo (can’t remember exact town)…. the procurement team would take a medical transport flight to the hospital where the body is and wait for all other organ surgeons to arrive. Before this Kevin would be called with an offer that would be something like, “we have a possible offer. No eyes on the organ yet but it’s about 9-12 hours out so make your way to the hospital but we have plenty of time.” The body is on life support and once the team arrives and opens it up and gets eyes on the organ they will call again if it’s a viable organ. If so we will either already be at the hospital prepping for surgery while the organ is placed in an igloo cooler and placed on a medical transport flight back to Methodist or Oschners depending on region the organ is sent to. I did ask how long it can be in the cooler. She replied about 9 hours.
•Will we have to live in New Orleans?
>>>At first we would need a week to ten days there for evaluation. We have already been evaluated so they can use most of the evaluation records from this last summer in Houston. But it will require about that much time to go through the similar procedure while not running all the same tests but meeting with most of the same type teams. (Heart, liver, social, financial…)
>>>if he accepts an offer here we will need to live there from surgery to about two months. She isn’t expecting that long because she said she knows Kevin will do well and expects him to just bounce right back and within two weeks they will be sending him home. Another answered prayer: surrounding us with great people and professionals who absolutely have Kevin’s best interest at heart! (We talked for 20 minutes! Then Kevin and I chatted about all she said the rest of the way home just processing it. He seemed excited. If that masks sense. We laughed because Keith will joke when he visits us in the hospital and say we are on vacation. We were like we really will be in New Orleans! Maybe we will hop around and see the zoo and aquarium…)
>>>we will have follow up visits there as well about once a month.
•Who do we say sent us?
>>>we will be self referred. That’s the procedure. She will be helpful and has a working relationship with their coordinator as well. We can be listed in up to two places. We will contact them then they will get us forms to start medical release of information and Jane will handle all of that.
•will we still get offers from Methodist?
>>>yes. We will have a clone of the team we have here. Transplant coordinator. Doctors. Surgeons.
•Are we able to petition for exception points?
>>>No. We were declined earlier in this process. I mentioned how many more times we’ve been in the hospital and she replied for the most part the board does not put a value on that. And this region we are in does not offer exception points as generously as other regions. I did mention that sounds unfair but she said they are working on more unity across the board. I can’t even imagine how anyone ever selects who gets what donor when. I know there is matching and miracles but am happy not to be in their shoes! Jane is amazing. She has the best phone and explaining voice! She always sounds like no question I ask is ridiculous. And happy. She is happy to help us. We thank and thank her and yet I feel we cannot or haven’t thanked her enough! God is so good giving us her for our transplant coordinator!
RemindBands
At our church all day the Journey Sunday School class Kevin is in passed out RemindBands with #PRAYFORKEVIN and Isaiah 40:31 on them. At a couple of hospital stays ago Scott and Pastor happened to be visiting Kevin and they mentioned wanting to do this. They wanted Kevin to think about it and let them know. Kevin picked the color and verse. Scott designed them. And today they were passed out at church. It is an overwhelming thing to feel so much love and support. Kevin didn’t take anytime to choose the verse either. I’m glad they didn’t ask me. I can be a little wordy … but love that the Lord put this verse on Kevin’s heart. “But they that wait upon the Lord shall renew their strength; they shall mount up with wings as eagles; they shall run, and not be weary; and they shall walk, and not faint.” Isaiah 40:31 We have to wait on the Lord. When we think of all the things that go into getting an offer it’s impossible for us to control the MELD score and the perfect match and no current infection and are we an hour away … only God can orchestrate all the things that lead to Kevin’s healing. Thank you church family and all those who lift Kevin up with or without the prayer bands. We are strengthened and blessed by your prayers and support.
Hospital Admittance 9 from Kirby ER by ambulance transport 3-17 to 3-23, 2017
March 23, 2017
Being discharged! Hoping the pain will be more tolerable at home. They slowly cut his IV pain meds in half letting him us pull form. He will have 90 days of oral antibiotic and follow up with Galati and Feinstein.
March 22, 2017
Last night Kevin needed nausea medicine. And pain meds throughout the night. He called the sleep he got “fractured.” The neutrogean shots are killing his bones… Dr. Carbajal warned us of this. We’ve seen Samantha so far today and the ticket home is all about managing the pain. We also asked about when do we ask about getting listed in other centers. We were going to wait until he was listed a year before asking but Keith mentioned it last night to me on the phone so in our conversation with her today she mentioned another patient in ICU now waiting on a transplant and that patient is going to go to another center once they are well enough to leave here. Houston transplants (as a reminder) at a very high MELD score. Kevin’s is considered low but in need.
March 21, 2017
7:00 Dr. Galati walked in with Samantha and Kevin texted me but I never saw it. He examined Kevin and discussed labs and ultrasound with him but basically said he needs a liver. And asked if I was around. Then said she has my number so she can call or text with questions. I walked in and probably missed him by 5 minutes! Kevin did text me. And it’s probably a good thing that I missed him or I would have cried all over them too! So I texted him that I was sorry to miss him and thanked him for stopping in so late. And he called me right then! I cannot even tell you how much I needed to speak to him. I know stuff goes on when all the teams walk out the door but it was great confirmation today after kind of feeling what is going on.?!? The Lord hears my heart and wonderings!
We discussed these topics on the phone:
•gallbladder — he said it’s a no. Never. That gallbladder isn’t coming out. Patients like Kevin all have gallbladders that look like that.
•he said what is happening with Kevin is classic PSC all the small to medium bile ducts damaged.
•the ultrasound didn’t show anything bizarre to him
•the pain Kevin is having he said based on examining him is also attributed to his large liver and spleen. Larger to him now and it goes along with everything he has going on. Unfortunately. So pain and discomfort from that. Growing pain type thing.
•it’s not flaming pancreatitis
•he said we need to control the infection, get with Dr. Feinstein team who has a 90 day plan for extended oral antibiotic care when he goes home, talk with the surgeon Dr. Ghobrial to remind him to be looking for a match for Kevin, think about applying for extended criteria.
•I finally remembered to ask him about the nor-ursodiol study and he said be careful with those when reading them. They could be for 5 years ago Kevin. I did remember you couldn’t be in the study if you had a Bili higher than 3. But mostly I just wanted to know if that drug is available and FDA approved here. And what he thought. I told him it just sounded promising. Dr. Sonny mentioned it to us. Bailey’s liver doctor. He had recently heard about it. Dr. Galati said he would check into it.
•And lastly we would regroup in the morning!
6:00 I walked Cole out talked to Keith and Tiffany on the phone. Then knew I couldn’t walk back in the room in the state I was in so I texted Kevin that I was just going to walk around. It felt great to walk and pray and wonder and gather my thoughts.
4:30-5:30 Kevin was gone for the ultrasound. Cole waited with me doing an etch a sketch of Sherlock. Inconceivable. For whatever reason I was nearing a melt down. Aka. Big Cry! And none of this is happening to me. It’s all happening to Kevin!
4:15 Granix shot given by nurse and she said they would be doing a complete ultrasound. Didn’t know that.
4:00 Dr. Linn evaluated and talked about picc line. She is fine with him going home on augmentin. Kevin is fine with the PICC line being removed before leaving here. Something she was saying with all they are doing that his lab levels look good but his pain is not responding that I tried to keep the tears in. She pressed on his side and just seeing him wince and her see it…well they seeped out. Like it’s the unspoken. What next except a liver.
Sheryl brought us a yummy lunch and chocolate granola!
Samantha and Dr. Seelbach they came in behind each other. Nothing really new. Dr. Seelbach definitely wants his pain more controlled before going home.
12:00 He officially is now on Low Sodium diet and can be removed from IV fluids! Maybe he can get more sleep now with less frequent trips to the restroom!
11:00 Mary a wonderful friendly cleaning lady just prayed over Kevin. I’m literally wiping tears! She’s got a beautiful Nigerian accent. She packed a punch! I’m telling you I am sitting here. Thought I lost my vault. Found it. It’s quiet in the room. Every once in a while I look at Kevin and just pray and ask what are you doing next Lord. Then Mary walked in. And cleaned. Gave him a talk about God being in control. Out. Of. Nowhere. Then prayed!!! How precious!!!
8:30 hemoglobin 3/19 8.9 … 3/20 7.7 … 3/21 today 8.5 so he’s good. No blood transfusion needed.
7:15 Mersha the nurse said his hemoglobin dropped to 5 from 7.7. So she’s doing another draw not from picc line to make sure of the number.
March 20, 2017
We had Michele and Jeff visit bringing Newks deliciousness. Keith, Cole and Caleigh crashed the party too. It was good getting through the day with good visits!
6:00 AJ gave him the Granix shot (neutropoegen)
5:00 Andrea from Dr. Nguyen came in and said it didn’t look like pancreatitis anymore. And that he had some “ascites” and reminded us she had documented this on him before. It’s nothing that won’t take care of itself. She said some patients have huge bellies and have to be “tapped” but Kevin doesn’t need that. I told her it’s the first I had heard of it. Kevin said he kind of remembered them saying it before.
Dr. Feinstein came in with company here. He wants Kevjn to go home on a pill. But definitely long term antibiotics. Will be ready to hear what other teams chime in on. We feel like last time this happened he ended up in the hospital anyway so long term didn’t help. But for Kevin anything if the PICC line is removed. However it has been nice for him during 4 am labs. No stick. He sleeps right through it.
We had great visitors today! Megan and Heather then Tiffany and Bailey!
10:15 Dr. Carbajal His white counts are down. For care of PICC line he said flush it twice. We were only flushing it once. Oh well. He wants him to have a neuprogen (?) shot. To help immune system. It may hurt in his bones as it gets things going. (Can’t remember the exact wording)
9:55 Samantha, Dr. Galati’s NP, stopped in. They are watching his lipase especially. The Bili is still trending down. No procedures yet.
9:00 am AJ his nurse brought in a full liquid menu! A step up. He was happy to be able to choose cream of wheat vs broth broth or broth.
March 19, 2017
3:00 Dr. Carbajal came by. He said keep it clear one more day. He said being hungry is a good sign. Bili and lipase are down.
10:30 Dr. Nguyen stopped in. It’s always good to see him! He said he saw the labs from this morning and the Bili is back down in the 3s from 5.9 so something’s working. But he thinks it’s still that gall bladder. He said it’s producing sludge. Not stones. And perhaps as the sludge is passing it increases the level of pain and adds to pancreatitis. Those numbers have been elevated before. He wants to address suppression again. Long term antibiotics. We know long term steroid use caused adrenal insufficiency in Kevin. Long term antibiotic use (I called it infection suppression) I need to look back over my notes and see why we stopped that. I feel like it has something to do with Dr. Escudier who did his bone marrow biopsy and screens for lymphoma. He said possibly keep it clear another day. All levels are lowering. He will see what ID thinks. We explained we were going to be hearing from them Monday anyway because his labs Friday were not good. Then he had fever. So basically Kevin kind of fell apart too early:) For now no ERCP.
After this Kevin and I finished watching Crown college chapel and Kevin and I started thinking out loud. Kev thinks if it is the gallbladder doing all this then why not get it out. His MELD isn’t where he will get offers anyway he said. But I think that the gallbladder gets what the liver sends it so with gallbladder out the liver will still send same stuff??? Then we decided to leave it to the smart people.
9:00 Dr. Carbajal’s MA she examined Kevin and is texting the doctor to see if she can move him to a full liquid diet vs clear liquid.
A verse from our Pastor:Deuteronomy 26:7a, “And when we cried unto the LORD God of our fathers, the LORD heard our voice, and looked on our affliction…”
March 18, 2017 Saturday
*all night Kevin was just so hot. I was freezing! The room was as cold as it could be. He sweat through the sheets.
He alternated pain meds but went longer between asking. They also tried the TPA to unclog his other half of the PICC line but it didn’t work. He even sat with it “soaking” for two hours. We walked around with Cole. Rebekah brought a yummy dinner.
12:45 Dr. Carbajal visited. He said the telemetry can go. He said he was registering a fast heart rate and sometimes they put it on for the wrong reasons. He will increase diet tomorrow to full liquid if all goes well. He’s hoping nothing major needs to be done and that Kevin will respond to current IV medications. He checked the scrape on his leg. He loved Kevin’s shirt! Kevin is a hit wearing that goofy thing!
12:00 a fellow from the liver team came through. He examined Kevin. He said we probably know the routine better than he does. But he’s going to be sure to let the other teams know we are here. Especially Dr. Nguyen. (ERCP dr)
“For God hath not given us the spirit of fear; but of power, and of love, and of a sound mind.” 2 Tim 1:7. Praying His Presence goes before and around Kevin and you. He is a mighty God. Lifting Kevin up.” My BSF leader sent that verse and prayer. I needed to be reminded of this. Simple truth but easily forgotten in uncertain times. Just when I think I am done updating people and can’t ask the same thing again and honestly a little overwhelmed with what may come next … He gives me that… precious. I love how He cares for us through others caring and reaching out in the simplest of ways.
10:20 Dr. Carbajal’s MA came in and checked Kevin. Mostly took notes. Asked questions. Told Kevin someone may steal his cat shirt! Lol!
10:30 The nurse wrapped Kevin’s soccer/ultimate frisbee scratch on his leg. He got cleated while playing yesterday. Just random. But today she said it looks like it’s bruising. She kept asking what happened and we repeated “cleated” or “kicked accidentally by a cleat” and she said I don’t know what that is! So we just left it at that. Too tired to even make her get it!
He’s also wearing one of those telemetry machines. Goodness. I asked why and she didn’t know. Maybe because he was transported… but when he sleeps his heart rate lowers and “they” call. I remember we had this on a previous stay and all the doctors thought it was ridiculous for Kevin. I was asking is it his blood pressure or oxygen levels or heart rate? Oh well…it just means he’s being watched that much closer.
March 17-18 ER Methodist 59 & Kirby
We remembered to listen to Jane. We got down here after 10 pm and didn’t even sit in the waiting room for three seconds before they called Kevin back to a room. They did labs. The doctor spoke to Dr. Carbajal down the road and said they will admit him. He is running fever and has chills. Has side pains. They started IV antibiotics: Zosyn and Vancomiacin as well as fluids. They gave him pain meds and nausea meds. He’s sporting a random St. Catricks Day shirt for St. Patrick’s Day. Shamrocks and cats! So we are hitting another holiday and got the end of Spring Break this year. I went 10 days about without updating and now I have 2 updates in one evening. At least they can use his PICC line. They mentioned once we get down the road they can clean out the line. Now the other side is behaving sluggishly. One side is blocked.
I tired my best to fix a Soup tonight that was “bowel resting” … Jane said earlier when she called with his labs that one way to bring the numbers down was to relax the bowel. I looked up a chicken and noodle home made recipe. I’m talking cut that fryer into pieces. Yuk! Shopping to serving was forever! And he didn’t feel like even eating it. Well, so much for homemade chicken noodle soup. I could have cut lots of corners but was watching sodium intake and keeping it clear liquid-ish as possible. So much for self inflicted clear liquids.
The ambulance transfer was very easy. The two gentlemen were so nice. I followed them to the Bertner entrance by the water wall. They rolled Kevin right up to main 7. I did peek in the ER for what I could see. It looked like a zoo. Glad we remembered Jane’s tip. This time we are on the opposite side of the hall. 763. It’s 1:50 am..
March 17, 2017 Friday
Jane called and said she was glad we didn’t remove the PICC line this week. (He finished Zosyn infusion Monday morning) It needs to stay. Or at least that is her thinking. She will get back with us after speaking to Galati and Linn. His numbers are not that good. Especially the Amylase at 391 and the Lipase at 466. (364 and 380 on 3/7) Also his Bili is higher at 5.3. I don’t have the ones in front of me to calculate the MELD score. His last one was a 20. I can only imagine it is a little higher. So, we wait to hear what they want to do. If we need to she said get in. I asked with these numbers would we be allowed to accept an offer. She said it would be on a minute by minute basis. They would retake the labs. But if they are what they are most surgeons say it’s too risky. So the treatment for pancreatitis is IV antibiotics, bowel rest, and possible IV fluids if he has to be hospitalized. I did keep the menus from his clear liquid and full liquid diets. But really it’s broth broth and broth. Juices. Fruit ice things. Hot tea.
For the record since he’s been home he has had pain. In a three day period maybe one of those days his pain is managed without taking anything. The infusion every 6 hours if I haven’t already stated it…killed us. We are so tired. Reminds me of new born baby days. Kevin slept for two days. Is still tired. I tell people we wake up tired.
So I was glad to hear what the labs from yesterday’s home health visit were so quickly even though I don’t know what to do with them. We are blessed with Jane as our transplant coordinator. Before her, I use to be the Kevin waving flag! I told a friend today it is nice knowing she is going to hunt down the teams and find out what they want us to do. I use to go back and forth calling and messaging and waiting making sure all the right people knew. It was nice to hear her say she would get back with us. Waiting and watching him.
I also asked her to have the financial people call Keith. He’s been spending hours trying to tackle the insurance part of all this. We have transplant coverage but it’s a circle they way things get billed and covered. I thought about going in the study and seeing if I could help Keith with the stack of medical letters and spreadsheet but decided against it. I don’t do numbers! But sometimes I think I should at least learn them. But then I borrowed a Kevin phrase: it’s not pressing…
It’s a little overwhelming thinking about what could be next. I know we can’t do or control any of it. So I have to just give it right back to Him. (Several times in a day!)
Also he is trying this evening to run a fever. 100.4 So watching that and perhaps will need to get him looked at in an ER.
March 7, 2017
Erin at Dr. Galati with a Shanghai by Jane!
Jane knew the picc dilemmas and called earlier and said she would meet us at the 1:00 appointment and bring her bag of tricks for the picc line. One side is clogged and the other side is trying to be clogged. (My words) She said sometimes you gotta show them whose boss! She gave us our labs from the home health nurse yesterday! (Explanation point because how weird it was to watch labs being drawn in my dining room and get them back in less than 24 hours! I still don’t have a portal for LabCorp…) His pancreatitis numbers are creeping up. They are elevated. Too bad that ER dr didn’t check them. He would have discovered the source of Kevin’s pain. (Just wait til I get that survey! I say that every time then forget by the time I get the survey!) Bili 4.3. And she mentioned that with a donor if his numbers for pancreatitis (amylase and lipase) are not settled he could not be considered because of the “morbidity rate with pancreatitis at transplant is just too high.” {hold it in hold it in hold it in!!! My pep talk to myself to not cry out loud after she said that!} We had Erin who tagged team with Dr. Galati. Kevin was hurting. They could tell because when they poked around on him as usual he was guarded and he’s not usually this way. I asked Dr. Galati what he thought that meant what Jane said earlier that if a liver is available and his numbers are elevated he said with pancreatitis you are in ICU and you don’t do anything! Not even cut your hair! So Kevin’s numbers are elevated but he’s not having full blown pancreatitis. Erin recommended as well as the doctor that he could continue on his home health antibiotics we have 5 days left. And they didn’t send him to be admitted as long as all things stay the same. If a fever breaks through or any increase in pain to call. The bit about the elevated pancreatic (my words so I don’t have to keep typing amylase and lipase!) kind of took me back. Diet wise keep it low fat and if difficulty eating do liquids a day or two to help settle things down. They gave us free samples of Nexium and want him to add that for three weeks.
I had asked before while in the hospital if being in the hospital took us off the offer calls. And then they said no it actually increases our chances. The surgeon according to Jane is “thrilled” when Kevin is in because he just wants him to get a liver. Erin is going to clarify what communication is going on with those things between Jane and the surgeon and Dr. Galati because we kind of didn’t get the same answer. A great friend reminded me as we spoke of these things that what does it even matter. Like, how can we even control the statistics and levels of Kevin’s numbers to be exactly where they need to be at the exact time of the offer. She said it’s totally up to Him and He knows exactly the time and circumstances. Goodness. That’s twice at least in one day of me being reminded that waiting is an ok thing when I am so ready to not be waiting, but, I got it. Kevin showed me a great verse while in the hospital about waiting on Him to renew our strength! Jane reminded me again to please if we have to go to an ER to use the stand alone one on Kirby and 59. They call the transplant team. Erin chimed in that she agreed unless it was any type of abdominal bleeding. When you are rushing and making decisions sometimes you just can’t remember. I mentioned it on the way down Sunday night but couldn’t 100% remember the intersection. So we go where we know. And we know Methodist. The last discharge we were standing on the curb waiting for Keith to pull in and I told Kevin isn’t this exciting! It’s like leaving for vacation!!! He replied well then that must mean this place is like home to you. He got me but as much as it’s not home it is now a welcoming friendly place because of familiarity and friendly caring nurses, doctors, and staff on that 7th floor! I have called that floor twice since we got home. And it has to be like home if you RECOGNIZE the voice on the other end out of multiple multiple staff who answer and call them by name! They answer our questions and sound so happy to help!
The PICC line is killing us. I told all of them today that Kevin said he’d rather be in the hospital then have it. We give meds every 6 hours which once you finish it’s like 5. And then this cleaning and flushing and clogs and blood seeping back in the line. I told Keith it’s just scary! He was like why? It’s nothing! I said well it leads to his insides. Keith slayed me with well … so does your mouth! I think we both think it’s Icky. Kevin said he’d rather be sticked and sticked until he cannot be sticked again. He wants it out! They said leave it in after day 10 for about a week and then in clinic they will pull it. We have so many questions about it. But we will hopefully survive this “phase” as Jane keeps reminding me. Before she left I asked could I hug her! She let me:) As we left the office we ran into Aracelli too and she hugged both me and Kevin…Dr. Galati walked by and was like none of this in the halls! It is very clear to me that they are doing everything they can for Kevin! In John it says to ask in Jesus name:
“And in that day ye shall ask me nothing. Verily, verily, I say unto you, Whatsoever ye shall ask the Father in my name, he will give it you. Hitherto have ye asked nothing in my name: ask, and ye shall receive, that your joy may be full.” John 16:23-24 I cannot even imagine the joy when He heals Kevin! I will ask in Jesus name to do so!
March 6, 2017 ER room til 5 am
Home Health rescheduled for this afternoon. Medication set up to be delivered tomorrow. Spoke with Jane about the ER visit and she was encouraging and reminded me it’s not a sprint but a marathon. (Dr. Galati’s office at 11:10 was at lunch.) She’s just the go to now. There are so many people over him that she coordinates things best. I’m reminding myself of this more than anything else. Also, the ER doctor once we were clear to leave kind of begged Kevin in a please don’t get hooked on pain meds kind of lecture. We listened and Keith even asked what the signs were. But since we have pain meds at home we didn’t even ask for a script. So already we aren’t who you think we are. I know when I was telling this to Jane earlier I just cracked. I couldn’t hardly get it out. What a tough spot. My child is in pain. He gets meds. He gets lectures for getting meds. Yet he’s in pain. I want to talk to every doctor one day years from now when this is over and let them see that perhaps Kevin isn’t in their 80-90% stream of ER patients trying to get pain meds. Most of them Keith reminded me are on the transplant list because of their poor life choices. That is NOT US! And that’s what makes me cry. They all figure it out in the end. But days like this just make me sadder…
Kevin is getting to take an online class this semester. He’s already had one of the two offered. So today after all he went through all night he is starting New Testament survey and is excited about it! Such a good thing. He even had the textbook in the garage from his bins so we just went out to where we stored his college bins…three of them…and found it. Great happy moment for me today! Seeing him excited and driven about class is such a good thing. Take that you *”pompous” ER doc😊 *Jane word…
March 5, 2017 ER 10pm
Kevin has been experiencing some pain today. By 10pm it was at an uncomfortable 8. So we gave tramadol. It seems to worsen so we headed to ER. He missed his 11:30pm Zosyn home infusion. I texted the home health nurse who was coming in the morning for labs and bandage change in case it turns into a long night. No sense in her coming if we won’t be there.
So far it was a walk in. No one else in ER. Kevin had an EKG he passed the dr said with rock solid results. They pulled labs from his picc line. They did a chest X-ray and scan with dye to look for clots. This ER dr wanted to rule out other things. He was so sorry to see a 19 year old in here for something so serious. He’s not the only one. It’s almost more than we can take to see him in such pain. I start thinking crazy thoughts like goodness who is really figuring out this kid and how much more are we going to take!?! I want to sit down with the doctors and say so what do we know!? Is all this expected? Normal!? It’s all an Internal battle and I was just so proud of finally getting through IV home antibiotic infusions. We’ve all embraced it. Everyone except Caleigh has given him his treatment. So to go from we got this to I don’t think we have this and never will is just where I am at 1:40 in the morning Monday in the ER.
3:00 am gave him norco for pain
3:35 We get to go home. All ruled out ok…follow up tomorrow with Galati
They didn’t run amalyse or lipase though for pancreatitis because he said it wasn’t hurting there when he asked kevin. So. Who knows. Dr thinks is musculoskeletal … like a strain… but if it worsens or he’s not right to return.
Hospital Stay 8 admitted Saturday Feb 25 to Thursday March 2, 2017
March 2, 2017
Going Home With A PICC Line!
1:00 PM
Education on PICC line for an hour. We got to practice. Kevin gets medicine balls to infuse like baby Bailey. We got all kinds of info. If we get home today we are in charge of doing the next two infusions if home health nurse doesn’t make it until tomorrow.
11:00 AM
Ok. I never updated yesterday’s second half of the day. I got to walk over to TX Ch and see Baby Bailey at one of her check ups. All the teams here were waiting on ID to chime in on what antibiotic to send him home with. Dr. Lin walked in at 4:30 in the afternoon yesterday and repeated his history. And with that came to the conclusion that he needed to go home on IV antibiotics if we were fine with that. A PICC line would be put in and home health would be tapped. Our first visit this summer with Dr. Feinstein in his office he mentioned this as well. At some point it’s just what is next. Augmentin worked to keep Kevin between visits until it didn’t. Levoquin was next oral antibiotic and we came into the hospital having just finished that one this time. He’s taken that a few times. She said the PICC line people work until 7 so it may be the next day. But within the hour they showed up at the door like Tommy Lee Jones at the site of an accident! (Fugitive reference) PICC line was in before Cole and I got back with hot tea from across the street. Today we have seen the floor nurse who has printed us great information on PICC lines. I had Kevin read then pass to me. Social Worker came in to ask a few questions and the case manager is contacting our insurance now and we are waiting for home health to stop in perhaps and educate further.
I know Phuong from yesterday told Kevin that she is out today but to speak with Jane about a follow up visit for next week.
Jane is our transplant coordinator and wonderful contact! She gave me this information when we spoke about a follow up:
•see Galati in his practice next week because he is triple booked at the transplant clinic
•she is the PICC line queen since she worked the 7th floor for years before becoming transplant coordinator and her mom had a PICC line for 9 months
•she said purchase these things:
1-package of diabetic socks at cvs (cut off the feet and keep the picc line covered at all times to prevent pulling etc)
2-get “press and seal”
3-get water resistant sports bandage wrap
*to shower keep sock on, wrap with press and seal, then wrap bandage around that.
***if the picc line bandage gets wet and home health isn’t coming then it needs to be changed because bacteria can get in from the wetness. We need to go to an urgent type clinic to get the dressing changed.
?Questions I asked about this new situation.
I told her his pain is not that much better. Is this where we will “live” now. She said no that it is just a “phase” like what he has been through with routine hospital stays and 6-8 weeks between. This “phase” will settle in. I told her I was a little bit apprehensive but she explained all things PICC line and I know we will get more education before the day is over so my head was somewhat unclouded after just speaking to her. Plus. I have Tiffany who will be all things PICC line too! People have been texting with PICC lines are the best! And it gets us HOME! Which gets my teenage boy sleep. Uninterrupted sleep.
March 1, 2017
11:00 AM
Dr. Seelbach just hopped in. He ordered the CT scan and CTA (angiogram) yesterday to rule out vasculitis. Immune system attacking blood vessels. Anyway. He sits. Asks how’s Kevin feeling. I’m like how do the numbers look. He replied I don’t know I haven’t seen them yet. So I said how about any results from CT/CTA. He looked and then was like oh yeah! And hopped out. Then after a while came back in. He said he’s fine! No worries and the rheumatologist agreed last night all they are doing w him liver wise is exactly what she would do. So…possible go home tomorrow if ID and Galati’s team agree and he’s waiting to see which antibiotics to send him home on.
He still has been alternating pain meds. Seems to be making it further apart. He did something to his left hand yesterday. The IV was changed Monday night to the right arm so they are watching it. Could be he slept on it weird.
Tuesday February 28, 2017
I started the day thinking it was March! It comes quick enough already so let’s wait.
We started the day with an answer for gall bladder removal by Galati’s NP Phuong. And it’s a No for now. Cole and I actually ran into Dr. Galati last night in the hall. Cole was leaving for the night and I was going to pick up a bite to eat. I was like hello Dr. Galati. If you are headed into Kevin’s room I will go back. Didn’t want to miss that. But it was late. We had already seen someone from his team that day. And I knew he was leaving town today so I said if you’re not that’s fine! He asked so what’s going on with Kevin. I said same old stuff plus they want to possibly remove his gall bladder. He replied….I will talk to Phuong in the morning… So all day everyone kept deferring to “the Chief” and I met him “accidentally” in the hall last night. I did tell him that Kevin just wants to know what Dr. Galati thinks. So this morning the revolving door of teams visited:
9:15 am Phuong. She will be back in clinic as outpatient NP which we originally met her as. Samantha will be the inpatient NP. It is a no for now on the gall bladder removal. “For Now” They are hoping this course of antibiotics will get him feeling better and they will “transition” for home. But she mentioned we will be in a few days.
10:00 am I missed Andrea from Dr. Nguyen (ERCP) team I was out walking Kevin’s phone trying to hatch an egg on Pokémon Go😂 I figured it’s not decision day since Phuong came in with a No. Kevin said that they said for now they will watch this antibiotics and see how things go before a possible ERCP. Yesterday that was a no. And now it’s possible. But both teams are really not wanting to because it can cause more risk of infection going in by pushing debris up in those bile ducts while trying to also sweep them clean. And his last one was two weeks ago.
11:15 am Dr. Seelbach (hospital trio shifts change between Carbajal/Dinikar/Seelbach) He is ordering a CT of chest and abdomen and tapping Rheumatology Dr. Popovich. He is concerned with Kevin’s ANKA markers and vasculitis. Of which we know nothing. He said it is part of Kev’s autoimmune disorder and vasculitis attacks major veins and could be damaging if untreated. I remember Dr. Carbajal kind of questioning himself aloud about is this visit PSC related or AIH.
He asked how Kevin was doing and we replied: tired and rotating through pain meds.
Also this morning a nursing student came in and asked if she could hear Kevin’s story as part of her education. Kevin said: sure. She is here every Tuesday for her clinical. I joked and said let us know if you figure anything out that we should know!!!
6:00 Dr. Mona Migu Rheumatology
She visited for an entire 45 minutes. She was very thorough. We liked her accent and mannerisms. She wanted to know the history and how and what he was treated with. She mentioned Dr. Seelbach contacted her and said yes Kevin has the 2 types of antibodies … and that he has atypical antibodies and his immunoglobulin levels are high but she is not concerned that it’s vasculitis. (Attacks the large blood vessels) She knew Kevin had CT scan and said she didn’t think we would ever see her again but would look over the angiogram and make a note in his chart with her cell phone number if anyone had questions. She gave us her card. She let us ask lots of questions between discussions. I did ask since she is a rheumatologist looking back on Kevin’s start and his diagnosis of AIH and the treatment TX CH used: immunosuppressant plus steroid would that be the course of treatment if we came to her office. She said yes. It is the exact treatment. She is not worried about the positive antibodies and said with AIH and PSC it is not uncommon to see them. She did say there is a completely aggressive treatment Retairemal (?) Infusion but she said that is very aggressive and usually results in causing infection. She is the second doctor today that said it is a mechanical problem (drainage) and it’s not uncommon for the spleen to be enlarged because the liver isn’t functioning. Platelets (flat shaped) get trapped in there as well other cells and that adds to risk of infection. It all made such sense when she was speaking. It’s a jumbled mess in my head now. But she examined Kevin and when she saw Kevin’s nails were bitten she said: Don’t Do That! Of course we asked the question to end all questions: how and why did his immune system ever do this!!! She said no real known cause. Your born with the predisposition to have it. Could be stress or infection. But no one knows. Dr. Pope said it best way back in 2011: Just Dumb Luck! But I figured I had an audience with a rheumatologist. I’m gonna ask! I know she also said Dr. Galati is the boss. He’s seen these numbers before and he is not surprised by them. She said usually the liver doctor handles this treatment just fine. She asked about the amounts of immunosuppressive medicine and we said it was as high as 250 mg and they kept checking the thypourine metabolites and it was within range. She said that is the highest dose she’s seen. But he’s not at that level now. It was nice to finally speak with a member of this team. We tried in the past to follow up with one. Especially after the October fall apart hospital stay. And they said they would look at our records and really never got back with us. They sent us to a fellow. So we didn’t even make an appointment. When we spoke with Galati and Erin about it at a follow up visit he said he was making an executive decision and we didn’t need to worry about it. So now that we saw them in hospital because of some markers triggering them and they have chimed in I’m guessing we are absolutely where we need to be. But for the record, I never like hearing a doctor say: you will never see me again….
Monday February 27, 2017
6:30 pm Kevin was given a breathing treatment. He has been coughing and it seems to be worsening. So Dr. Carbajal ordered breathing treatments.
6:00 pm Dr. Lin is back checking on Kevin. (Infectious Disease Team) I asked Kevin what she said and he said she said, “get that bad Larry outta there!” But I was here and she didn’t say that! She caught up on his history but she remembered the dates of his hospital stays better than we did! And the things concerning him… she likes how well Zosyn is bringing down the levels but it may not be doing anything about the strictures. Or the pain. He is still piggybacking two different pain meds even though they are farther apart in the day. Once she heard the gallbladder is inflamed she did agree that it could be adding to all the other issues. And it could tip the balance it could put a lot of stress on the liver. Removing the gallbladder stresses the whole system. She is so friendly. I had seen her in the hall the last hospital stay and was just waking past her and she stopped me to ask about my son:) Kevin didn’t have that team last time.
***What I will remember about this day is Tiffany and Bailey were down for a weight check and asked if I thought it would be ok if she stopped by. I said I WILL PAY FOR YOUR PARKING IF YOU BRING THAT BABY BY! (I’m not leaving the room on “figure out day”!!) So Bailey stopped in and Kevin and I were so happy for this visit! She’s so cute! Made our day!!! During this visit we got a call from Crown College. They went over on a conference type call what Kevin needed to do to take online classes. He looked this up last week when he was feeling ok. Today was the deadline to apply. And they break the classes up. Like Semester A and B. Since he has some already this time he has taken one of the two so he will take one class. They said they will completely explain the situation to the instructor and if Kevin has any problems or set backs then they will be as flexible as the class allows. This makes me so happy! These classes all will completely transfer but perhaps one day when we are looking back on this journey Kevin will be finishing his degree in pastoral studies at Crown. Praising and thanking Him for this direction in Kevin’s life.
Liverpool is on so Cole and Kevin are in the zone!
2:00 pm Dr. Carbajal
Doing well according to him as far as liver panel goes he is happy to see Kevin responding to this course of antibiotics. He is asking ID for input. Here are the Bili levels by day:
Friday: 4.4 pediatrician
Saturday: 4.6 ER Methodist
Sunday: 4.9 Methodist
Monday: 3.5 Methodist
We asked about his opinion of removing the gall bladder and he is hesitant. He said it really needs to be a “hot” problem. He’s seen recovery of this surgery go into liver problems. (I’m thinking ok. Let’s do it. Maybe he will get a higher meld score coming out which equals transplant …but that’s just me) He did say that Galati is the chief and he will make that final decision.
12:15 pm Andrea popped back in and said for now let’s see how this course of antibiotics does and then they will re-evaluate for possible gall bladder removal. So she speaks to Phuong and Dr. Nguyen. Phuong speaks to Galati and Nguyen. So it’s a big square but circulating information on Kevin. So no surgeons will stop in today…. we are in a holding pattern.
11:45 am Andrea NP for Dr. Nguyen stopped in. Explained that after his last ERCP he noted that next time possible gall bladder removal. And we are at next time and it’s been one and a half weeks. They are all discusing it!
10 am Today is figure out day. The MRCP showed strictures deep in. She mentioned that Dr Nguyen’s NP was leaning towards recommending removing the gallbladder. They are pondering that… but I was like well if he gets a liver the gall bladder goes anyway:) hint hint
Galati leaves tomorrow so she will ask him. And we will wait to see what they decide.
Sunday February 26, 2017
Keith and Kevin are giving me updates. I am packed and ready to stay and will head there after church. So far today they said Dr. Galati’s on call team came through. Dr. Nguyen’s NP came through. Kevin said she said they probably will not do another ERCP since they just did one but it still could be cholangitis or pancreatitis and are treating with IV antibiotics and for now liquid diet. After 9 am he is NPO because they want an MRI.
They changed his steroid from prednisone to hydrocortisone and are pushing fluids. He can take 100 mg tramadol for pain and fentanyl for break through pain.
Saturday February 25, 2017
Caleigh’s DI competition! It was a loooong day. We left the house at 6:30 am and were waiting to hear from Kevin’s lab numbers. The PCP office said that would call with them. They called Kevin to tell him they weren’t in but they hadn’t forgotten him. He let me know. He also needed nausea meds and pain meds. Once they called and told Kevin his numbers were elevated we knew we needed to get him admitted. I stayed with Caleigh to let her finish her DI day and Keith headed to the ER with Kevin. He got to be apart of that experience! I missed a call from Dr. Placencia while in DI. She had been calling Kevin because he’s 18 or older and have his cell listed as contact. When I could call her back she said she was just so concerned about him and that every time she called to check on him he said my mom is at DI. So I told her that yes I was at DI but we had a plan! And that Keith had him headed to the hospital. I thanked them so much for getting us the numbers so fast. It really did help us decide what to do. Overall we knew even without them if he worsened we would have gotten him in. His Bili is 4.4 from Friday and other labs are elevated as well.
2:00 pm arrived at ER and triaged
4:00 exam room ER the ER doctor came in briefly and got things going: labs and IV and contacted Dr. Carbajal. He came through and wanted an ultrasound and admitted him. Room 769
At the awards for Caleigh (they placed 4th so are done) I saw portal messages with results. I peeked at the liver panel and his Bili was 4.6
Caleigh and I headed straight to the hospital to see him just because I wanted to give him a hug! I thought his eyes looked feverish. He just looks like a sick little boy…. kids are always your kids even when they are old enough to sign their consent for treatment! Keith stayed the night.
Friday February 24, 2017
Kevin has been out of the hospital for a week and a half but this week he hasn’t been doing all that well. He’s had to take pain meds a couple of different times and is tired, nauseous, and not eating well. We were able to see a doctor at Dr. Pope’s office because I was kind of thinking maybe he is viral or trying to fight something normal. We love that office! We started out with the np on a walk in and ended up with Dr. Placencia. She was very thorough. She actually was able to access Kevin’s medical records through EPIC! This is huge! They could see all his last labs and trends. I’ve wanted this for so long! Shared information for Kevin! Phuong had called also while we were in this office and mentioned what labs to have checked and to try to share them with EPIC so they could see them. Dr. Galati is out all this next week. The transplant coordinator was out all last week. So we just went to the one who knew him longest and he was out the afternoon… it all worked out though.
Hospital Stay 7 — 2/8/17-2/14/17
February 14, 2017
We are being discharged! Admitted 2/8-2/14
Noon
Dr. Carbajal was back in going over medications. No one has problems with Kevin being discharged. He needs a follow up in a week or two. The nurse had just given Kevin some pain meds and he is resting waiting on lunch and official discharge papers.
11:45 Phuong stopped in next. We discussed all that happened and I asked her about what Dr. Carbajal mentioned and it’s just the nature of his disease PSC… the common bile duct was swept and dilated. The part about all the smaller bile ducts having “poor flow” of the contrast just went right past me. It is the nature of PSC… she wants him to be seen. Now Dr. Galati is in the transplant clinic every Wednesday. So she will let Jane know to schedule a follow up for him.
11:30 Dr. Carbajal
It’s his rotation starting today. He is checking with Dr. Nguyen and will see if he has anything else he wants to see before discharging. He mentioned three dilations…which made me want to revisit the report handed to us by Dr. Nguyen after the procedure.
Awakened to Ray taking Kevin’s labs and letting us know there is a tornado warning. We will wait that out!
February 13, 2017
6:00 pm needed pain meds alternating just to keep it under control.
4:00 pm
Needed pain meds for side pain. Probably expected because of al that cleaning out.
12:30 pm
Back in the room and hungry!
11:30am
Kevin Update: I’m in recovery with him. He did fine. No stent needed. They will keep him one more night for sure. Dr. Nguyen said his problem is not so much in the common bile duct where a stent would be placed but up in the smaller ducts too small for a stent. He dilated it. Drained and swept it out. But he said he looks good.
10:45am
Kevin’s just gone back for the ERCP procedure. Dr. Nguyen spoke to me quickly before. He hugged me. Said he would look and see. Maybe a stent this time to keep that bile duct open longer. He will see. Praising Him for Dr. Nguyen
9:00 am
He is resting and waiting for the transport to take him to the ERCP. His last meal for soft diet he had cheese quesadillas with sour cream and salsa last night and I think it’s so funny that he said the sour ceam tasted like the salsa! He said it was just weird. Also one of the PCAs asked why he didn’t have the Grammys on and his reply was I don’t even know what that is! He was reading a book after his headache settled. She just laughed!
February 12, 2017
They started his IV and reminded him NPO after midnight for the early morning procedure. (ERCP) He had a bad headache. So twice at the 4 hour interval he took headache meds (Feorinal or butal/acet/?) He takes it at home. It’s a step above Tylenol and liver safe. He experienced nausea and needed meds two different times and he needed pain meds at least twice. So it was a very good thing to be here after all.
10:00 -11:00 am
We went from being asked if we wanted to be discharged today and the procedure Tuesday could be outpatient in one hour to never mind. A cancellation happened and now a Monday time is available Galati and Nguyen teams want him here. We were fine. We had that energizing info and they let us go dark before officially starting the IV again so we left the room!
February 11,2017
Keith sent me updates:
“Kev is sleeping. The stinking machine went off every 30 minutes all night long. I was so mad! She would come in and thump it a couple of times and leave…. one time she just silenced it and left so it alarmed again about 30 seconds later!”
“Stephen came in this morning and changed the tube…no problems since! Idiot!”
“Dinakar came by… nothing new…he just wished they would do the ERCP sooner. Wants Kevin up and walking around today”
When we got back up there we all walked around the hospital including gift shop. Kevin found some great pieces for Tiffany of which I snap chatted her to never let them shop for her! They have weird expensive clothes down there. Just sayin’!
February 10, 2017
Keith stayed the night with Kevin so I could sleep at home. He has a trip out of town so I knew I better take it!
1:30 Dr. Nguyen’s NP Andrea came by while I was out to lunch with Tiffany. She told Kevin the ERCP would be Tuesday. And that his numbers haven’t gone any higher but they also haven’t gotten any lower. So without being in the room I can only put together that they want his pancreatitis type symptoms and elevated numbers to settle down. And/or they may just not have an opening until Tuesday.
Kevin is hoping since he’s not having a procedure he can step up on the diet from clear liquids. We will see how he tolerates if they will allow it.
9:00 am Phuong came in and there is a definite stricture shown on the imaging. She has contacted Dr. Nguyen’s office to see if an ERCP can be scheduled today. Kevin is in pain from this and is not able to eat much. His MELD score is now a 20. To my “MELD score calculating” knowledge this is the highest he’s been. She said she would let the teams know that… “hey…Kevin is in the hospital and if there’s an offer just reminding them he’s here and a good candidate.” (Something like that)
6:00 am they came for him to get his MRI/MRCP
Between pain meds and transport arriving we were awake and I said Kevin do you know what today is? (Beside’s Hillary’s Birthday!) I said exactly one year ago you called me from Crown college and said your friends told you at lunch that you were looking kind of yellow. I said send a selfie. You did. I sent it to Galati’s office and I will never forget being in a workout barre class and stepping out to take a call from Araceli his medical assistant. She said the doctor wanted to see you Friday that your bilirubin was a 5.8 and that we should know he wants him to stay “for a while.” Kevin and I recounted the hospital stays…in the dark hospital room early this morning we were going on memory we mentally listed six admits and Kevin commented: what a productive year. Each one as we listed the stays we could remember so well because life still happened in and around each admit. Great memories of family and or celebration was weaving through each one. (Spring break, Easter, Wedding shower and wedding, back to school…) Productive. Yes, we went from the absolute unknown to diagnosis to being listed for transplant. Now let’s get HEALED!
Pain meds 5:30 am 8:30 am
February 9, 2017
7-10:30 PM the scheduled MRI/MRCP ended up not happening this evening. He will be first thing in the morning. He’s clear liquids still and tried jello and hot tea. Still hurts to eat but he was hungry. (Can hardly take this!) So 6:30 am they will come get him for that procedure.
2:00 pm Andrea from Dr. Nguyen’s office to check on Kevin. They are thinking along the same lines as Dr. Galati. She is pretty sure Dr. Nguyen would want imaging first before an ERCP. She is hoping to order one for today and hope it happens today.
1:45 pm Dr. Galati visit bedside
He was catching up. He did ask Kevin if he was disoriented? But he is not worried about his ammonia level. (I never even knew there was one but now I find myself telling Kevin to be sure to let me know if you are disoriented and then it dawned on me that he may not remember this conversation when/if he’s gets disoriented!) Anyway, he couldn’t believe we never went home yesterday. (After the routine clinic visit) He was checking his numbers and pain level. He wants to first order an MRI/MRCP before doing an ERCP. He explained the risk of too many ERCPs with an infection possible behind a structure causing an abscess. He had someone with him from the Woodlands rounding with him and he introduced Kevin to her as his youngest patient on the liver transplant list.
10:20 am
Dr. Dinakar isn’t worried about any of the trigger words I heard yesterday: sepsis, ammonia levels, lactic acid level. (He said he is not “encephalopathic” I think that goes with those words) He said usually the ER sees the number and it’s an example of technology getting ahead of us. Examining Kevin and seeing how he is comprehending takes that number to a different meaning. Makes sense. He mentioned he has fluid on his belly but will not do anything at this time. He contacted Dr. Nguyen and he will be by. Most likely he will have an ERCP tomorrow or the next day.
Pain meds 7:00 am 1 pm 10 pm
February 8, 2017
Pain meds (fentanyl) 6:30pm 9:45pm
5:30 PM
He made it to the 7th floor. (771) Liquid diet but eating jello hurt. They are checking triggers or sepsis markers. I think because we came in through ER and his number one reason to be there was abdominal pain. So they mentioned lactic acid and ammonia levels. Something to piece together tomorrow. 3 things I don’t think we’ve ever had mentioned or given … I thought I heard his MELD score was 18. Earlier at the transplant clinic it was 15. So something is going on. (Or I can’t understand the nurses!)
2:30PM
We hadn’t left the medical center yet cause we took Tiffany to lunch. Kevin was hurting and has been on and off for the last several days. So I called Jane. She said while we are here just walk over to ER. If he starts feeling better we can hop out. But, his pancreatitis enzymes are elevated again. His liver enzymes are elevated as well so possibly be cholangitis. They already have admitted him and he is going to a room on 7th floor main. In ER Dr. Dinakar already came by. He starred IV antibiotics. Ordered fluids only. And is phoning Dr. Nguyen (ERCP) to have him check.
10:30 am
Kevin’s visit at the transplant center with Dr. Galati and Jane the transplant coordinator. Discussed Kevin’s side pains and spleen side pains. We told them he has “hit the wall” several times this month and I told them I am now not calling the minute he gets a fever! (But we wait it out. See where it’s going.) Jane encouraged us in that every week when the board meets the surgeon Dr. Ghobrial mentions Kevin’s name. She said she cannot say this to every patient but Kevin’s name comes up so often. With every offer practically. She feels that is how he will get the best liver when a patient is about to receive one and then is too sick or has to decline it. He will be the next choice. She told us a story of one person she was calling. They didn’t answer. They didn’t tell her they would be out of town so she called the police. And they found them. They were in church! So, I told them I answer every call! I keep my phone where I can see or hear it…it will happen. It was good to be reminded of it. She will call later with his labs and current MELD score. I need to actually see when there is a follow up appointment.
January 25, 2017
Dr. Escudier follow up. MRI over hospital in Dec lymph nodes no change. “Prominent lymph nodes” His platelets were 83 a little better. White counts 2.5 still low but she blames it all on his liver disease. She measured the enlarged spleen. Something like 24cm. She mentioned her 40 year old nephew had a liver transplant at 12 and is doing great. Good to hear! But we get the all clear from her. Especially since he’s being seen by other doctors. Unless they want him to come back to her we are listed as prn.
January 17, 2017 Tuesday
Kevin went all last week just so strong. Working with a church ministry and just getting outside and playing soccer and basketball with kick:) Then, Monday night he came in and said that he’s actually had some side pain the last two nights. I wanted to know what he didn’t tell me when it started and he just said because it’s just like annoying. He ran a low grade fever of 100.8 and I am thinking we will be leaving for the ER really soon. But, he went to bed and has powered through whatever it was.
January 12, 2017
Follow up with Dr. Galati went well. Nothing at all revealed in the scopes to be concerned about! Good news:) In 4 weeks he wants Kevin to be seen by him but in the transplant center. Jane will call us and schedule this.
January 6, 2017
Kevin has a colonoscopy today at 7:15 am arrive at 6:15 am down at the medical center at Texas International Endoscopy Center.
January 5, 2017
Kevin has a colonoscopy tomorrow so today is prep day. Last time he had one was at Texas Children’s (Dr. Olive for Dr. Walsh) before crossing over to Texas Liver Specialist on November 18, 2014. He can start the day on liquids only. Then starts the moviprep at 4 then 8. This prep is different than last time. I told him because he’s an adult! What do I know. We spent the day moving Kevin into Tiffany’s old room: he now has lots is space, Tiffany’s stuff to Caleigh’a pink room, and Caleigh to Kevin’s old room! Great distraction!
January 3, 2017
Dr. Galati’s office called and wanted to see Kevin this afternoon. He went over joint pain and blood in his stool. He wants to scope Kevin this week. Friday Kevin will have a colonoscopy. So Thursday is prep day. He spent a good thirty minutes with us. He had mentioned the next time Kevin experienced this he would scope. He mentioned ulcerative colitis not saying he has this but he said it sometimes goes along with his PSC. It’s good to know he will get checked out quickly.
Joint pain / diffuse arthralgia was mentioned as a kind of traveling arthritis. Not saying he has this. Keep an eye on it. Especially let him know if there is redness or swelling. It was on and off about three weeks. Mostly ankles and knees and elbows. None today.
January 2, 2017
The ER doctor said he spoke to Dr. Galati’s fellow and they agree since the hemoglobin is 10 we can go home. We got here at 12:30. It’s almost 6. We are waiting for the IV to be removed. They never did IV fluids. Just labs. So they said we need the discharge papers and a nurse to remove his IV. But goodness. We were never admitted I told her we never left the waiting room! She said it’s the same. Crazy stuff happens here. Funny and crazy stuff. But. We want out!
Here is why I know we needed to go to the hospital. Neither Kevin or I have laundry done:) But, he just didn’t look great yesterday. He was quiet. I knew he wasn’t sleeping. And I knew he was noticing blood in his stool. I knew we were calling today. The lines were all down. We had a storm. So one call service told another call service that we called. Dr. Galatis office is closed today. It is Monday but observed New Year’s Day. I did hear from the doctor on call. He looked at Kevin’s file after asking several questions and said he wanted Kevin to be accessed and the only place to get that done today was down at the ER. I said well what if we wait and call tomorrow when the office opens. Because I only called today thinking it was open:) He said because they cannot tell how much blood is lost we just really need to go. They will do a hemoglobin lab. He mentioned his baseline lab is showing 8.5. He said if it’s higher than that they will let him go. Then we can call Galati and schedule a scope tomorrow. If it’s lower then they will admit him. So. We are waiting for the results now. Which means I have time while life isn’t happening all around me to update this page and check out the pokestops in the medical center!
Jan 1, 2017
Kevin has not slept well lately due to being up all night with diarrhea and has noticed blood in his stool. For the record I would guess maybe in November the check up with Dr. Galati he said if this happens again to call in and most likely he needs to be scoped to band the varices. (Spell check doesn’t like that word!) But I remember it was the EUS with Dr. Nguyen then the Follow Up with Dr. Galati that he explained the watermelons spilled on the road for us to understand esophageal and rectal varices. And I hated to hear it then. It took me a while to update that one because the images it made me think of. The blood is finding any channel to flow and sometimes the channels are not strong so bleeding can occur.
December 26-27, 2016
I tried to reach someone at the doctor to ask about the joint pain. It seemed to get a little better. I sent a portal message and left messages. I did hear back from Nicole because it’s a holiday week and most were out of town. Erin Yates called us back just to hear more details. She said she would speak to the hospitalist and call us an. Dr. Dinakar gave her information for us. He said up to 2,000 (?) of Tylenol per day for joint pain. Only Tylenol. I told her he liked Advil and she said what I knew: no no no. So it was funny. She left us with well tell Kevin to pretend to take Tylenol and if it gets worse get to the ER and Dr. D who we’ve seen in the hospital before would be on call and familiar with him. We never went in for joint pain. They said it could be viral or (lost my note) {found the note: virus prodrome and yeah no wonder I don’t remember it. I think it means random and can go away on its own! But I did Dictionary . Com it and had to look up the word it had defining the word. I think these people could speak simpler. Just sayin} but some random word. Anyway. Who knows. He did tell her if he doesn’t move he doesn’t hurt! Problem solved. Don’t move!
December 25, 2016
After opening presents Kevin looked like he wasn’t feeling well. He was having pain at around a 6 dealing with joint pain.
December 20, 2016
Dr. Galati Follow Up Christmas Week
Energy level is good. He played soccer recently. Some diarrhea. He asked what he did during the day along with any thoughts on school. We pointed out if you chart Kevin’s in and out of hospital along with how he feels on a given day up against a semester it would be difficult to keep up with class. He asked how many admissions he’s had since last February. (I need to go through and number these) We randomly answered 6-7 not counting ER trips that he’s not admitted. He asked how is the rest of the family doing with this. How are we doing with this. I was flat out honest. I told him if we keep talking it would make me cry. He’s had experience with me on this one for sure, so we moved on. I will say it’s just to tender. Anyone can ask about Kevin and it’s just so close to the surface of my heart strings that tears just form. It is what it is. Dr. Galati called the situation “a burden.” That is an inside family joke because the older kids always referred to Caleigh as “the burden.” I joked with Kevin and said so now you are the burden! But really it’s not a burden. It is hard to explain this but we just handle it. We accept His will and perfect timing for our lives and trust Him completely with all things. But lots of people refer to “it” in such a way. I guess maybe one day we will look back and perhaps call it that. But for now we anticipate Kevin’s healing in His hands. Life happens all along the way.
Araceli was getting the laptop up and running as Dr. Galati asked questions about his MELD score and if he was denied exception points. His current MELD score is a 16. He was denied exception points but since then he has been in the hospital double the times since the first letter to the board was written. He was texting Jane the transplant coordinator. Kevin and I usually have a list of questions. This time he only had this: What’s. Next?
Dr. Galati once the laptop was up wanted to ask about the previous hospital stay the first week of December. He asked was the pancreatitis symptoms better. Kevin said yes. It could have possibly been Imuran related or gallstone related or even sludge. While in the hospital he did have another ercp. But he’s back to normal tolerating a regular diet. On the PSC side of things he’s awaiting transplant with intermittent fevers. He’s finished the 7 day antibiotics.
Where are we now: this is the watch and wait and hang out and stay close and answer every call even if we don’t recognize the number time. The doctor said chronically he won’t feel right but to look at the things we can fix. Even though there are not a lot of fixes he compared it to a machine that goes on the blink every once in a while and you kick it and put a new fuse in it until it gets going! He acknowledged what an odd situation it is to be in waiting for that shoe to fall off. He doesn’t have the luxury of saying hey, I’m clear, I’m done, I can get on with my life. He said we are tethered to them and they are tethered to us:) It is the nature of the AIH and PSC over lap. Tricky cases. Transplant is the answer ultimately. We discussed or rather I asked if we could be called even knowing 99% chance we might not be transplanted could we just be in the waiting room for the incase:) They have that system in place already. And I know we have been in the hospital and been told we were very close and one of those identified “back ups.” He told Kevin to stay out of the hospital during Christmas while he was out of town! We will see him in 4 weeks. (For the record Kevin had complained about ankle and knee joint pain but I dismissed it as soccer soreness and bike wheelie popping in the side yard…)
Hospital Stay 6 —12/1/16-12/8/16
December 8, 2016
We made it home! Hopefully Kevin will listen to his doctor and stay away for a year!
10:15
Seelbach came in to look at him. Said he could go home. He said he hasn’t seen the numbers yet. Isn’t too concerned about the numbers. He likes to look at the patient. So. The wait for discharge begins. Tick Tock Tick Tock. For the record one week ago tonight we spent the entire night in the ER. We will be happy to get home!
December 7, 2016
11:00
Phuong came in and we talked a bit while Kevin slept. She explained the results of the ERCP. She saw the report and spoke with Dr. Nguyen. He did say it was harder to “navigate” the ducts. She said that’s the part of this disease that she hates so much. She said they feel helpless. She knows I do. Then Seelbach came in while she was here and they discussed watching him today “mimicking” home care so tablets and off IV. Then tomorrow if all goes well they will send him home.
She was such an encouragement whispering not to wake Kevin and just discussing anything I asked. Explaining things. I told her Kevin and I list questions before and here we go again with, so, what happened. Why did he get pancreatitis? 😂 We’ve been here all week but why again are we here! It does all make sense in a small way. But she said to always call in with any symptom. I asked does that Bili level seem to be one of the best markers? She said yes if it’s trending up. It could be a sign of strictures or infection. Either way. He needs to be seen.
December 6, 2016
Treasures of Darkness (from Isaiah 45)
ERCP at 3 but before that we had visitors. Christopher and Anna Claire had appointments across the street of all days so they made a quick visit to see Kevin. So cute. They made cards and had to see Kevin at the “doctor’s house.” Cole brought up Kevin a book of magic card tricks which was a perfect distraction for not eating all day along with the biggest stack of cards written by Hillary’s kindergarten class. Such treasures in that stack! They don’t even know Kevin but took the time and drew and wrote him get well wishes. Classic cuties!
The ERCP went well. No stent was needed. We may get to that point in the future but for now Dr. Nguyen said dilatation works best for Kevin. There were strictures. Significant blockage. But he swept those bile ducts clean. Mentally we think this was his 6th one. (Will fact check that later!) It doesn’t matter how familiar we are with it. It just never gets any easier watching him be pushed back. That’s why when the doctor hops out by Kevin in recovery and explains how the procedure went to me and what he did I am just so thankful and happy and relieved…did I say thankful!!! These skilled doctors. God’s great guidance and healing and protection. It’s just overwhelming and joyful all at the same time. I really need to send Keith back for recovery. The doctor is probably like look lady I just swept out your son’s bile ducts you can’t be expecting me to wipe your tears too! A friend sent a great basket of plants with balloons and of all things right when we needed it, the gentleman delivering it found us in the waiting area of the ERCP! How does that happen?!? Like. We live in the hospital room. 7th floor. For a smidge of a day we hop over to who knows where (we stick to the people transporting Kevin in his bed like glue! You should see us all crammed in the elevator!)
We are surrounded by so many praying and faithful friends and family. Bekah brought up dinner and more than food we just, somehow, in a hospital room had a fun night of laughter and visiting. Tiffany hops over and we watch baby Bailey kick, I am thankful for my beautiful family!
I am reading a book given to us by PC at a previous hospital stay: Off Script what to do when God rewrites your life by Cary Schmidt. (We chaperoned a teen camp he spoke at and I had heard part of his story) It’s been a tremendous encouragement to me. I’ve been taking pictures of the pages that speak to me because it really was Kevin’s and I hate to mark up someone else’s book. That book is a treasure, today we were blessed with so many treasures but even if no one knew we were here we know that He knows and loves us and is completely in charge of this rewrite of Kevin’s life and that is enough.
“And I will give thee the treasures of darkness, and hidden riches of secret places, that thou mayest know that I, the Lord, which call thee by thy name, am the God of Israel.” Isaiah 45:3
December 5, 2016
6:45 Dr. Nguyen came by and talked about the ERCP tomorrow too. He is considering putting a stent. Kevin had one the first ERCP. It didn’t go well. But no matter what with a stent or not he still returns. If a stent then he has to return for removal and replacement. Without a stent he has been returning for ERCP procedure to help with infection and cleaning out the bile duct. So. He will see when he gets in there.
12: 45 Dr. Seelbach came in. It was good to see him. He was chatty. He told Kevin looks like you just need to get in the mind set that this is going to happen almost every quarter. And if it doesn’t–great! He said his amylase and lipase numbers were the highest he’s ever seen. He particularly questions more about the pain. Where it starts. How it feels. He and Kevin connect over that. (I don’t like re-living it and it didn’t happen to me!) He asked if the pain makes him lean over and focus on that only. I was like yep! He does the “double over old man walk.” (Truth be told Keith always tries to film this! Such a bad dad!) But it’s an outward sign to us at least to know how Kevin is feeling without saying a word.
12:20 Phuong came by:
ERCP either Tuesday or Wednesday. It still needs to happen because of the strictures in the duct and the dilation. She drew the picture because I was like isn’t dilation a good thing. Opens. Flows. Well, the stricture / blockage / caused the duct to open the opposite way. So it flows back ward into the organ. (Bili is elevated) Got it.
I also asked transplant questions. How many does she see. She said sometimes they go weeks without one and sometimes they have 3 in one day. She will check to see and confirm with Jane our coordinator to be sure where she shows Kevin on the list.
7:00 am We slept straight through the night! No blood draw at 4 am. “They said” there’s a new protocol in place. If the liver patient doesn’t have a procedure that day then blood draws can wait until between 6-8. It’s an attempt to let patients get more rest. (He joked and said it’s getting the doctors on board because labs post later and if they don’t see them they start ordering more STAT!)
December 4, 2016
9:30
We walked Keith down and ended up staying away from the room for 45 minutes! It seemed like 10. But Kevin was worn out. Actually experienced some side pain once we got back up and he took tramadol. Just recording it to see if it correlates with diet or walking.
5:00 I came back home with Cole and Caleigh to shower and get more clean clothes for Kevin, and Keith sent me this update:
They brought in his two bottles of protein at 5:25pm
Dr. Carbajal came by. He said the MRI showed some scarring and dilation which is typical from PSC. Pancreatitis seems to be responding well to typical treatment. We will see how he does on some more solid food. Dr. Nguyn wants everything calmed down for the possible ERCP on Tuesday (if they do it)
Possible that past ERCPs could have caused the pancreatitis (scarring, etc)?? They aren’t sure….
11:00 He took zofran for nausea.
10:00 am His nurse disconnected the lines so he could walk around and get some exercise. He actually didn’t get far before he was feeling nauseous. So we sat downstairs and looked out the window at the wall of water then he returned to the room. Progress.
The nurse practitioner for Dr. Carbajal was in early. She also was a wealth of information. Just discussing his symptoms. She was encouraging sharing patients she’s seen before with this crossover of symptoms and diseases. She said to document all the recurring infections. She saw his Boston cup and connected over that. She use to live behind Fenway. So. It was good. He’s been up since 6:30. He was hungry. It took an hour and ten minutes to get the food. Liquid. Food. They are seeing if he can add soft food.
He slept fine. He didn’t need a pain pill. The “shadow nurse” ended up having to redo labs for whatever reason because his blood clotted. So awake at 4 then 6:30. So we ordered his breakfast. Cream of wheat, chocolate pudding, orange sherbet, 2% milk, hot tea–that kind of full clear liquid diet. It’s Sunday. He’s still basically resting his pancreas because even though the numbers were significantly lower they were definitely still elevated. So he’s easing back into solid food.
December 3, 2016
We had a visit from Hillary she helped us get moved to the new room. This one has a shower. All the rooms we’ve ever stayed in have had their own showers. So it was weird not having one but fine. Then Keith brought Cole and Caleigh and they brought games. Unfortunately for me we hadn’t ever played one of them so Keith read ALL of the directions to us. Every word! Lol (it took an hour and a half to hear them!) After his procedure since he was tolerating clear liquids Dr. Carbajal allowed a full clear liquid diet. Basically he’s still hungry on this…
10:45
Looked up some of his numbers in the portal:
Lipase 1287 U/L standard range 13 – 60 U/L
Amylase 1018 U/L standard range 13 – 73 U/L
Bilirubin 3.3 standard under 1.2
There are many many more but the first two above explain and confirm pancreatitis which is why he’s on nothing by mouth to rest the pancreas. And will add back foods after the MRI starting with clear. His cafeteria lady today already brought him a tray. We were like. He can’t eat. She said I know. But I ordered him up some so when he gets back he will have something and she added so don’t touch anything now! Lol!
10:00 MRI/MRCP was suppose to be first thing and it’s 10. But his nurse called and told them he’s NPO until this. So they said they are coming for him. Kevin has been sending me recipes that look good. Poor kid is hungry.
4:00 am tramodal for pain
December 2, 2016
8:45 pm Meds plus tramadol
Dr. Ngyun came by at 3:45pm Friday
-Saw interesting ultrasound that they have not seen before with Kevin
-Could be stones in the ducts, but it could just be air (they look alike in an ultrasound)
-Will see better in the MRCP later today.
-Will let pancreas rest the rest of today, maybe clear liquids tomorrow. If pain starts back up, then will have to back up again with no food or liquids.
-Still plan on ERCP Tuesday…
2:30 Andrea Washington (Dr. Nguyen’s NP…he’s the ERCP procedure doctor. Gastro doc) She was a wealth of information! Answered so many questions. Explained what biliary pancreatitis is. They want his pancreas to rest. Kevin described the pain to her as sharp and stabbing. All the ducts are in the same vicinity and one can irritate the other. The pancreas does endocrine and exocrine. It helps digest food coming in and out. Since it is irritated it needs to rest. That’s why he’s not eating or drinking today. They will do the ERCP Tuesday. The ducts being so close together they don’t want to do the procedure too soon or it could actually irate it to cause pancreatitis. She was glad we came straight in. All his labs pointed to pancreatitis. Elevated lipase and elevated “something else” 🙂 We told her when they came in the morning and said all this we were just so tired we didn’t quite put it all together. Now we get it.
10:30 Food no food
Phuong and Dr. Carbajal just said kev is NPO. No food or drink. He has pancreatitis. Possible billiary pancreatitis. Like maybe a stone passed through biliary tree (?) Food and drink irritate it.
They saw the lipase level elevated. Dr. Nguyen wants ERCP next week maybe. MRI today of bile ducts. Ultrasound definitely showed sludge.
*I could not make sense of stuff. Just so out of it. Poor kid. He ordered breakfast cause they called off HIDA scan. Before he awoke to eat it they saw results of film and said NPO. they want to settle it down.
7:00 in normal room on 7th floor. Home away from home. Tired.
4:30 am Ultrasound of gallbladder and abdomen
4:00 am zosyn IV antibiotic started
3:45 am
ER doctor confirmed it’s the usual stuff. He’s admitting him. Still in ER room. Waiting on room assignment.
“The Lord is good, a stronghold in the day of trouble; he knows those who take refuge in him.” Nahum 1:7 (thanks Ruth!)
1:30 am
Kevin made it through triage. We are in an ER room. He’s nauseous. Side pain of 5. And I’m seeing very yellow eyes. It’s Friday morning. My absolute least favorite day to be at the hospital. Especially if he’s going to be admitted. It just seems like nothing happens until Monday. But. It’s early Friday! So here’s hoping.
December 1, 2016
9:30 PM
Keith texted me and said that Kevin was taking a tramadol with a side pain level of 6-7 and going to bed. He didn’t end up staying there. By midnight he was hurting and asking to go down to the ER.
5:00 PM
Kevin’s had on and off good and not so good days. Not so good: low grade fever and nausea. Good days: he’s wanted to go Christmas shopping. He’s walked the Ren Fest. He’s played basketball. Helped at church in the teens. He’s been planning or thinking about the young people between teens and college age wanting to reach out somehow to them to get them back connected. I love where his heart is. It’s back on a baseball field. Only this time possibly softball. Just something to connect with them. I heard him mention how much the field rentals are in our neighborhood and he came in with an old baseball glove trying to round up some worthy equipment for a pick up game. All the while I’m thinking I hope you don’t get hit in the spleen with a ball!
Dr. Galati Follow Up visit Thanksgiving Week
We had questions about the strongyloides test. Remember I was only on the edge. Glad I didn’t jump in. He said he read an article recently and it all came from that thought that people from areas where this parasite is found are among us. So the possibility is there even without traveling to the countries where they are common. Now they are implementing this lab for all transplant patients. Kevin’s was negative! And I did ask could this be a false negative! He’s not concerned about them at all.
He mentioned his serum albumin has for the first time maybe ever — dropped. It’s a measure for protein. He wants Kevin to be aware of his protein intake. (80-100 g a day) So we got a nutrition talk– add more egg whites to the two eggs (carton by the eggs) yogurt, nuts, beans, beef and chicken, smoothie w protein powder. He didn’t think he was malnourished and joked about us feeding him three peas under the door to his room while we ate steak! But he thought he had lost weight and that number was low so we got the talk.
We went over things that happened to him since we last saw him. Kidney stone. Random fever. If he has another kidney stone and they don’t administer pain meds once we walk in the ER he said to call their office! They should give pain meds!
They are transferring all things IT to a cloud from a server. They sent me the last labs and I was able to pull them up on my phone. Courtney calculated Kevin’s MELD score which was an 11. (Not getting us any closer to that liver but the recurring infections are…)
He sent us with labs to Smith Tower and is especially checking the bile duct cancer marker. He’s checked it before. He’s keeping a close eye on that.
Very thankful for this doctor and his staff!
November 21, 2016
Thankful that the fever never returned. Saturday he did experience some nausea. We got him out to play some cornhole because it was a perfect day outside! He didn’t attend church on Sunday due to a headache and we were heading to Lufkin that afternoon to meet and pick up Mam Maw from Aunt Sheila. So he felt like riding and making that trip. It could be because exactly half way is a restaurant called Ralph and Cackoos. I don’t cook that good or do seafood. So it’s worth the trip for Cajun seafood lovers. Today he felt up to playing ultimate frisbee with friends! We have a follow Up tomorrow at the medical center seeing Dr. Galati. Hopefully we will get some answers to that blood test from last week.
About that portal. They have replied to me. Then I happened to ask Kev if he got any reply from the help desk because his email was used. He actually did hear LAST THURSDAY!!! And it’s all their fault. They have Kevin’s information in their system twice and they apologized and said we should be able to open a portal in two business days. This is why 18 and older kids really cannot be trusted with their health information! I really could box his ears in. But. He doesn’t check his email. EVER. One step closer to getting it.
November 18, 2016
Kevin awakened us at 3:00 with fever of 101.5 along with nausea and chills. We gave Tylenol and called into the doctor. Dr. Galati said to treat the fever today with Tylenol as long as it is responding. If fever persists tomorrow he wants him to get in.
November 15-16, 2016
This one gets two days because it is still unsolved. A simple patient portal. Galati’s staff last visit asked if we had a portal set up to LabCorp because many times patients walk in and say the labs are in because they’ve already seen them. We don’t have one but let me show you the bubble on my iPhone labeled “portals” because Kevin has so many! I want a portal to end all portals!!! So after the lab tech drew all the viles she needed I asked what was the “strongyloides” one? How long is the turn around? And she said she has never seen that one before. Then I asked is there a patient portal for LabCorp that we can register for. She found us a pamphlet and said it is so easy. Just follow these instructions. I was elated! Another portal to get information and organize all these labs! Perhaps our days of taking the printed labs and inserting numbers in a spreadsheet are over! We can click the portal and see them all… EPIC EPIC EPIC (not enough EPIC’s to describe this feeling and failure all at the same time!) Its all about how they connect their health vault with Microsoft accounts. And who knew we already had a Microsoft account. But once I started the “simple process” let’s just say we need to go back to Galveston to that couples retreat because it got ugly! When I’m stressed over “simple not working out,” my frustration is just that. Frustration. But people around me think I need a padded cell! And I have a very difficult time explaining my frustrations without making the person hearing it think I am frustrated with them!
Ok.
Keith.
Let’s just get it out there. Mr. Monotone Jones himself. He can calmly relate the hysterical to a room full of monkeys without so much as inflecting his tone of voice.
Seriously! While I on the other hand, have been accused of being, what’s the word, animated. They say I’m too –animated. All I did was go to the website. Click on create an account. It said we already had an account with that email. So I went to my “written mind” that secret place we all have access to that we list all the username and passwords to all the places we have usernames and passwords. I’m talking from Walgreens to Costco photo center. And there wasn’t anything Microsoft which means I didn’t ever knowingly create an account. So I hacked into what would be ours that one of my family members must have randomly done. Got the password reset so I could get moving on the LabCorp portal. Only to get everything in. Including Kevin’s last four digits of his social for it to tell me INVALID.
Something did not match with their records. So in my infinite knowledge of creating patient portal accounts I thought oh, it has to be Keith’s information like birthdate etc. So I changed it to him and thought well we can add Kev under this. INVALID message again.
This went on and on. I redid. Retyped. Thought it was me misspelling something. Got very frustrated. Said these words to Keith because he didn’t seem as passionate as I was about getting this portal open!! We’ve been getting Kevin’s labs for five years and not once did anyone ever tell us they had a portal.
Give me this portal!
Keith couldn’t remember if or why he had ever opened a Microsoft account (which includes Xbox live so the children should be glad I didn’t drag them from their sleeping beds!) instead I told Keith with enunciating and teeth gritting that I was going to be putting his birthday in the system and it will show me you were the creator of the account!
He went to bed.
Can you even believe this! I was going to conquer this portal business. I cannot even tell you how many accounts I almost created.
INVALID means INVALID.
I gave it up for the night. Well. Early morning. Then got back at it sometime the next day but dragged Kevin into it. I made him sit back with me because after all he is 19. So part of the INVALID could be that over 18 thing. Who knows. I did not want to use a different email but decided to try Kevin’s email. He could have his own account because he is Kevin and it is all happening to him.
With great anticipation we filled out the easy step by step process using Kevin’s email and it said
INVALID
So I started the process for speaking to a human behind the portal help desk. My cell phone has decided it will drop calls or sound statically only while in my house and only sometimes. I was on the cell phone and went through several holds and transfers to finally get to the person who could help and she couldn’t hear me! I was trying to tell her to call me back on my land line.
We were disconnected.
But I walked straight through the house. Found two dead home phones and then one with some life and started the entire process over again. I got through to a sweet soul who has now “opened a ticket” for me and is having the real tech support call me.
On the home phone.
No call yet. No LabCorp patient portal for Kevin to speak of.
It’s. All. I. Want. For. Christmas.
November 14, 2016
Keith reminded me that we haven’t heard back from the frozen stool sample. It was something I checked the portal often last week thinking they would put the lab results in there but actually let the weekend sneak up and knew it was a Monday call. So after leaving Araceli a voice message that we were checking in and hoping no news was good news just touch bases when she was available. She called back. Asked me to get him to labs because it has been time plus his next visit with Dr. Galati is next Tuesday before Thanksgiving. Then she said Dr. Galati added this one himself and told me to please write down the name to know what to ask the lab tech to be sure they see that order. She said she has never heard of this test before and had me write “strongyloides igg antibody” and didn’t even tell me one thing about it other than Dr. Galati is still researching Kevin’s elevated eosinophils (a white blood cell). I’ve had friends and family google it and will not list here anything because we see him next week. It’s just a test. Not a diagnosis. And why jump in when there isn’t even any water in the pool to swim yet. I’m going to just wait and relax by the “edge” of the pool and ask all my questions next week. We. Have. Questions. We. Have. Thoughts.
November 3, 2016
Kevin had been having diarrhea last week like 4-5 days. So we called into Galati’s office just to inform them. Usually one can let such stuff fly by. But they want to know stuff like that. Blood. Vomit. Nausea. Chills. Fever. Diarrhea. (Basically the same list we tell our kids they can wake us up for. Ever!) So they said the doctor wanted a stool sample and to get by LabCorp when we could.
Poor Kevin!
So. We pick up the kit. They wrote a sticker on the container that said “frozen” and Kevin said the guy said bring it frozen, but I figured that was because it was mid afternoon and we were taking it home. Who knew that Kevin could produce a sample so quickly. In the hospital when they ever asked for one it took him days and every single person that walked in the door would ask anything yet? So we brought it right back not frozen. And they sent him right back out with it and said to freeze it and return it tomorrow. I started with poor Kevin and I will end this update with poor Kevin! (Now we know why people have “garage refrigerators”) However to be around the two brothers throughout this entire dilemma had me laughing tears. Potty humor at its peak! But, POOR KEVIN!
November 1, 2016
Dr. Escudier called. I was in the carpool line. I will gladly pay the fine for answering calls from doctors! She saw his cytology reports and had to call because it was good news nothing genetic or anything to worry about. Completely all clear. She said she remembered us and just thought we could use some good news! I was so happy! Especially after the kidney stone all nighter a few days back!
Also earlier in the day we saw Dr. Pope for a follow up from the kidney stone. We called down to ask where do you want us to follow up. They said PCP was fine. Dr. Pope’s follow up went well! He is referring us to a urologist. We mentioned we had seen Dr. Sukin back in the day. And I think he said Angela will be getting with me. To help make that appointment. (Reminder and note to self follow up here.) He checked his urine sample and things looked better on a kidney stone front with ketones (?) and blood in the urine kind of front. (I will be blitzing anyone I know whose had this experience!)
October 30, 2016 1:30 am to 7:30 am
Kevin seen in Willowbrook Methodist ER
Kevin awakened me at 1:30 am in a lot of pain. He said it wasn’t bile duct or liver but more starting in the right testicle and shooting up his right side. Yikes! And yikes! Gave him tramadol then just decided to head to the closest Methodist ER since one time they mentioned to us if it’s an emergency get to one close (because hospitals are everywhere now) and if needed they can transfer him to the medical center. I will admit I was concerned something from the torsion surgery of 2011 went wrong all these years later. And as soon as we walked in they saw some of his history and ordered an ultrasound of the groin area. His pain this entire time on “that pain scale” was a 10+. So, as we sat after triage Kevin wanted me to go ask if there is anything they could give him for the pain. (At the time I didn’t know why the lobby was full) The nurse said that we would be taken back soon and there was nothing more that they could give than what he already had. The ultrasound ruled out a couple of things. So, back out to the lobby. We waited a bit more then got right back. They did a CT scan. Gave him morphine. 20 minutes later the pain was back at a 10+ so I walked out because Kevin asked if I could see if they could give him anything else like when he’s in the hospital with a painful bile duct infection they alternate pain meds. I also asked if they could see his entire history. They hadn’t seen it yet so I tried to fill them in quickly. It’s just the worst thing seeing him hurting and doing nothing! I haven’t had a kidney stone but know enough people who have and they all agree how painful it is. Goodness. The pain meds piggybacked finally worked or the stone passed. Who even cares when the pain is gone. The doctor said there wasn’t a stone actually seen on the scan in the right side but there is a stone in his left kidney so they know he’s a stone producer. [Also before he came home from college last February he went to the ER in Knoxville with his RA and Dean of students for this same pain.]
We walked in asking for pain meds and being judged (my thoughts) and by the time we walked out they completely understood us. I know pain med addiction is a huge problem so when one really needs it they have to put their guard up. The nurse was funny and told us to stay away from the “Rave” going on over at the racetrack because they have had a dozen girls overdosed over the course of the night. We had seen them in the halls as we went in and out of the procedures and I was thinking in my own mind that if they who basically with “self inflicted” injuries delayed Kevin’s need for medical attention then I know why they place two officers at the entrance to the ER. They would have slapped the cuffs on me and hauled me to jail for how much I felt like going off on them! My son who didn’t ask or do anything is in so much pain!!! And I did not handle it well. Not at all. But I didn’t go Mama Beth on anyone either. Keith was with us and I would text him and say I don’t know how much more Kevin can take. Then Keith would reply well, he’s not pulling his hair out yet. He had been with him after torsion surgery and the pain was off the charts and Keith said he was pulling his hair out. And that was suppose to help me! Such a horrible horrible night. Poor Kevin. I did nothing and went through nothing and yet have been flatlined from this! The nurse even brought me a warm blanket because I think he thought I needed treatment and that’s ALL he could offer:) Once the pain stopped and the stone supposedly made its way to the bladder Kevin was better than himself! He was happy. Talkative. And the doctors didn’t see any reason to transfer him to the medical center so we walked out passing another boyfriend chasing an ambulance to meet his girlfriend as they opened the back pulling her out on a stretcher. Our rough night was over but those poor poor doctors and nurses and techs that treat emergency room victims. Their night never ends! We climbed in bed and slept all afternoon.
October 28, 2016
Dental cleaning for Kevin. He had a filling that was falling apart so they wanted to redo it that afternoon but needed his doctor approval. He did fine. And who knew that the dentist needed a liver transplant listed patient’s doctor for approval to fix a filling. It all matters.
October 24, 2016
With great rejoicing I want to share that Kevin’s bone marrow biopsy/aspiration revealed nothing to worry about! He is currently recovering from a normal common cold. They are watching him very closely but are happy to know he can still be normal.
Huge relief all around. Continue to pray for his perfect healing as we wait on a liver transplant now with no “known” other problems. (Cytology (?) results are still out there and she will get back with us once they are in.) whatever that means…
We know so many have prayed for this specific test and just wanted to get this out and once again thank you all for your prayers!
“Rejoice in the Lord alway: and again I say, Rejoice.” Philippians 4:4
Oct 19 Dr. Galati Follow Up
Mental note listen to voice recording*
(Honestly it is Nov 16 and I am just now updating this. I’m going with flatline. I flatlined. Some stuff I have just rolling around in my head and I’m kicking myself for not getting it written. It really helps me to be able to look back. But to write it I have to process it. And sometimes I just let it roll around. So add denial to flatline and you’ve summed me up perfectly this month!) {Caleigh and I went and got nails done recently so with both hands taken my nail lady who knows us pretty well asked how was Kevin. What a test. I had to speak without crying to answer because my hands were tied up. Such. A. Challenge. So I knew I wasn’t ready to write updates if I had such difficulty answering an almost stranger!?!}
This was an afternoon appointment. He asked Kevin the following:
•Are you on a steroid? Yes–5 mg prednisone
•Were you on it before? Yes–at initial diagnosis aug 2011 and tapered off by Dec 2011. And nothing for a while. Budesonide was the next steroid he was on and off until the last hospital stay when the endocrine team said stop. We reviewed that to familiarize him with Kevin’s history of steroid use.
•How are you feeling on it? Better. More energy
•Any fever. Chills? No
•How about the belly pain? Still there every once in a while
•He saw his LabCorp from the previous week and said the dosage on Imuran looks good.
•He asked about Dr. Escudier and the bone marrow biopsy procedure. He asked Kevin how did it feel? “It was ok.” *i don’t know if I’ve mentally recovered and Kevin is like … it was okay… Love Dr. Galati’s comment: I never caused you that much pain.
•It was a biopsy and an aspirate. The aspirate is the part that hurts. {He told us of his intern time in NY with a hematologist and they did bone marrow biopsies all day. So he went into great detail of how it was done and described his first one to us. I already could pass out knowing Kevin went through it but steadied myself as he described the bone marrow being sucked up the needle.} Basically the pain only lasts seconds (like I know) and it feels like a jolt down your leg.
•He wanted to be updated on Dr. Nguyen and the last procedure [EUS endoscopy w Ultrasound to get that lymph node sampled] he did on Kevin. He wanted to know when we saw Dr. Escudier. We told him she said the lymph node biopsy was just a bunch of blood. Dr. Galati said he would reach out to them both.
•He asked about the career path Kevin wants and if he thought there was a college here that he could live at home and go a couple of days just to keep the wheels turning. Kevin said yes but then I reminded him he doesn’t feel great all the time. Some days are not good. He was just asking for future not expecting him to be enrolled. We don’t want that kind of stress added to Kevin’s day. All that stuff will happen when it happens. Kevin’s timeline isn’t the same as an average 19 year old.
•He discussed how out of control he feels Kevin’s Autoimmune disease is. The reason he says that is based on the labs, and Kevin’s total protein in his blood is really high. (Sometimes used as a benchmark for how active an Autoimmune disease is in someone) It’s always challenging and he said do we “super duper Immuno suppress him” then he runs the risk of infection. He said it’s very difficult. All sorts of other problems and “phomas.” (If I heard that correctly)
•He said we have to sort of pick your battle: are we going to treat this underlying Autoimmune disease at all cost? (Just throw the atomic bomb at it?) Or do we say you are destined to be transplanted and go that route. [He was thinking out loud] We are keeping his feet in two buckets. Sort of treating the AIH and also on the list for transplant.
•Based on current labs those thoughts hit him. But for now unfortunately the system was down so he will look at Kevin’s past file later. He could not see the entire file. But was thinking out loud about changing him from azathioprine to one of the other immunosuppressants. (Cellcept,…about 10% of the time they have to switch to other agents)
•make a note and he’s thinking about it. Nothing immediately. Just remember it’s an option.
•He said the main thing now is the infection and making sure the bone marrow is behaving.
•I mentioned that the platelets are low. He said with these Autoimmune diseases sometimes the platelets can clump. And then the machine inappropriately calls them low. He said he could talk to Dr. Escudier and she can totally see them and prove they are being made in his bone marrow and consumed in the spleen. It’s trouble if your body isn’t making them. Also we remembered infectious disease doctors were not worried about them at all. They said the platelets are in the spleen. It’s huge.
•I asked if they were ruling something out and what. Dr. Galati said it was because of his eosinophils being too high.
•The bone marrow is the window to your physiologic soul he said.
•we asked do we still see him in his office and not over at transplant clinic? He prefers to see us in his office for now. He’s in his office 5 days a week while in clinic only Wednesday mornings.
•we told him the new symptom is blood in the stool. His response was two fold. It could be hemorrhoid or rectal varicies. We did mention that Dr. Nguyen spoke to us that after the EUS varicies were seen in his esophagus. He said someone 50 years old with these symptoms you think hemorrhoid. Diverticulosis. Cancer. Said he was just a little too young to mess with all that. But because Kevin has liver disease and cirrhosis he could have rectal varicies. (He called it another curveball)
•He asked how often. Kevin said everyday last week but nothing this week. So he had Courtney make a note that if it happens again he would want to do a scope.
•He explained varicies in what I will call a metaphor using Houston traffic! Varicies are the result of blood not flowing properly through the liver. And so the reason his spleen is so big is it’s a plumbing problem. So instead of blood going to the liver it takes a detour and goes to the spleen.
He asked us how we go home. I said the Hardy toll road and he explained that on that 4 lane road with no traffic we can go 90 mph yet somewhere along the way a truck dumps 10,000 watermelons. Traffic stops. Cops come out or the watermelon patrol (!) they move all the watermelon over so that one lane is open. Cars back up. But we know the area so exit the Hardy toll road and go around the back roads around a development and get back on the Hardy five exits down. That is what the body does with blood.
•the liver is a choke point because of scarring and the disease it is not allowing blood to flow through. (5-6 lanes down to 2) That’s when it heads to the spleen. From the spleen it’s being shunted to the esophagus and stomach. Ultimately the blood has to go to the heart so the watermelons are the liver and cirrhosis. It’s making sense to me!
•then he added that the rectal vericies are the exiting the Hardy to the 610 loop and are just going around the other way. All these vessels are connected.
•the plan is any sign of blood call him. He can “band them” and I asked of course what does that do?! He said it puts a road block on cars going through the neighborhood! We don’t want the cars going through there because those are the varacies. We don’t want that. But I was like well if the old good path isn’t open…??? I don’t even know what I was trying to ask …He completely understood my question. He said you block it off. The blood goes in a “different safer direction.” The problem with the varacies is they can hemorrhage. (This sentence alone is why I’m flatlined for Kevin. Can’t get that thought out of my head. What. That old path isn’t getting any newer or more open. Is it?! And I remember Keith’s dad always had to hop in and get “bands” with his liver disease. It just has brought back a lot of memories.)
•if he is doing ok come back in 4 weeks. Labs also in 4 weeks. Loved hearing that!
•They have a solution. We know what to look for. And since it’s been a while since this visit actually happened (it’s Nov 17 and I started writing this yesterday) I can add that Kevin has been feeling better. He’s helped at church many times with different things. He’s hopped out on the exercise bike. He’s ordered books from Answers In Genesis to read. He’s had a headache here and there that can slow him down but he’s been doing better. I just finished a Philippians Precept Bible study and seeing joy in suffering and knowing we are to follow Him were perfect reminders that was so uplifting to this flatlined mama. Sometimes my following Him was not looking straight ahead to Him but sometimes passing Him dragging all the things behind me all the way past Him so much so that I am trying to take that lead. Constantly looking back at all Kevin’s been through and trying to follow as my Precept teacher explained so well, when you turn your head to look back you misstep, get all wobbly looking over your shoulder and cannot be following Him. To follow you have to be behind and walking right in the steps they take. Much needed reminder. Praise Him!!! I will trust Him! He will heal Kevin in His perfect timing. He uplifts the flatlined. None of this is even happening to me! I made the mistake of saying out loud “when Kevin hurts I hurt.” So now Cole walks around asking me after hitting or smacking himself or Kevin “Did you feel that? Does that hurt!!” I don’t think Cole reads my updates even though years ago he did one time say when I died he would carry on the blog for me calling me blogger beth, but that brother has been the best brother a brother could ever ask for. I think he knows exactly what it means to hurt when his brother hurts. He’s way better at handling it with laughter!
October 14, 2016 Bone Marrow Biopsy/Aspiration
The Bravest and Strongest Boy I Know!
Kevin did great! While Cole and I were walking back to sit with him after the procedure the nurse said he did better than anyone. Some of their patients have even screamed before they even touch where the needle goes in! So proud of him! I asked him before the procedure to be ready to give me a number for when there is that 10 seconds of pain I wanted to know where on that scale of one to ten it falls. I kept in all my tears until I saw him and he was fine. So tears of relief. But he wouldn’t give me a number. We have a follow Up appointment on the 24th for results.
October 12, 2016 Right Heart Cath
The dr just came out. He did fine. He’s clear for transplant! Most liver patients have “pulmonary hypertension” … honestly I don’t know what he said. Had to ask Cole. He popped out so fast. I just know we can’t accept a liver unless he had this. So we are a go now:)
Official report findings:
· Right heart filling pressure is normal.
· Pulmonary hypertension is absent.
· Wedge pressure is normal.
· Cardiac output is normal.
· Intracardiac shunt is not detected.
Normal filling pressures.
Normal cardiac output.
October 7, 2016
Kevin is Kevin
Next week Kevin has two procedures. One on Wednesday, a right heart Cath, and then a bone marrow biopsy on Friday. It has taken a while to get the right heart Cath scheduled. The tag line for that one that drove me was “if he gets an offer for a liver he cannot accept it because he hasn’t had a right heart Cath.” I cannot even tell you how much that drove me. And I was patient. I would call. I wouldn’t leave a message I would hang up and try a different number. Marie gave me two and one was direct which that one was always a recording so I always phoned the one she called “general.” She said they are super busy so be patient. And I was. Until it was just past that point of no return. The poor girl that answered the phone yesterday got all my questions when she tried to reroute me. I gave her the history of my calls, told her he is a 19 year old who needs a liver and actually wouldn’t be offered one without this procedure and I somehow cannot ever get a call back. I asked where does our name go. Is there a high turnover in the process and Kevin’s return call never happens because it’s on someone’s desk who left? I told her I just want to know the process behind this. He’s been in and out of the hospital and even during those stays I have said should we get that heart Cath? They have always said just wait and do it outpatient. I’m really curious. Not mean. Just completely curious. I’ve said this too often: I just want to walk around with the white coats to see and hear behind the scenes. It doesn’t help that I’m so literal!
We had a list of questions to ask Dr. Galati’s office so I called in. I asked them all:
Can he have these two procedures in one week?
He needs a refill of prednisone.
His standing order for labs expired and we need to be sure the next one has been sent.
We need to reschedule a follow up since his heart Cath was scheduled on the exact same day.
She confused me at first because she mentioned he needed to do most of this through the transplant clinic. I’m sure I hyperventilated through the phone because whoever this was I had to mention that we just spent the better part of the summer and early fall trying to get a return call so I was not comfortable calling up the transplant clinic. I know we will start doing that and very soon but if I tried to call now I don’t even know who to ask for. She did agree and say it’s an entire world of its own. And the next available appointment over there was not with Dr. Galati. He rotates between clinics. She put me on hold and returned with good news for us. She said: Kevin is Kevin and he can still be seen here in this office and made us an appointment for next Wednesday. I was so relieved! We will cross over. I know. She called Kevin one of their high risks patients that they like to keep a close eye on. So blessed by that! Really am. I didn’t even need to hyperventilate.
October 4, 2016 Good News!
Follow Up Day at the Medical Center
Endocrine with Dr. Mejia and her attending Dr. Sharma
He will not need labs for cortisol levels because he’s taking a low dose steroid. It will not be a true result unless he goes off it. They said there is no need for that now. Most likely he will need to follow this same treatment plan with the transplant. So in my mind, not Kevin’s, I was wanting to know his cortisol level. I wanted to see if his adrenals woke up! Kevin looked over at me after I asked the question and no one was in the room and said even he knew that. Well, somehow I missed it:) The low dose prednisone is treating adrenal insufficiency as well as his auto immune symptoms. We don’t need to follow up again. They are fine letting him be seen by Dr. Galati. But reminded him to watch for fever, chills, nausea, and call in with those symptoms. Also, to double the steroid dose if he does get sick because with adrenal insufficiency his body doesn’t know to fight. It needs that kick start from the steroid for now. Once they left the room I remembered the “double the dose” classic question. Two at once or one in an and one in pm. We are going with the am and pm because we remember the dosage in the hospital. They liked the two pills spread apart. But the second one shouldn’t be taken too late.
Dr. Escudier Hematology/Oncology Follow Up
She had Kevin give quick CBC labs. Then came in and went over several labs that were ordered while he was in the hospital that we didn’t have back before we were discharged in the 17th. Compared to today and those last ones in the hospital his red and white blood counts aren’t bad. His platelets are low. While she was looking on the screen she was just so nice and said pardon me and please give me a minute so she could see what she needed to see to compare and poke around to see each lab. Anyway I just took that time to silently pray that He would give her wisdom and insight quickly as her eyes were taking in the screens. In passing we were catching up on different things. Remembering what all their concerns were. I mentioned that he had his EUS with fine needle aspiration on that lymph node last week. And she clicked around and said the results just were posted. (I checked my patient portal messages on all portal sites even while waiting for her. But I didn’t think they really would be there. Actually it was perfect timing. Because even as I update this and have checked we don’t have results dropped in the portal yet.) So thankful for the follow Up timing. She said it looks good. It is enlarged. Probably from his Autoimmune disorder. But, it is just a mass of blood and tissue but they were able to get some lymphocytes to see and she said that is good. So it’s good to have this news especially waiting for a transplant because it makes every area that had any questions as to “is anything else going on” pretty much answered… well except for this low platelets and elevated eosinophils. She wants to do a bone marrow biopsy next week. She described the process and it’s done in her office and said Kevin is so accommodating … it was a long day! We are tired but have that praising and thankful heart! Kevin seems happier too. Could be his energy level is finally where it should be after it was flatlined so long. Or, that unusually heavy question about the enlarged cardiolrehenic (spelling so off!) lymph node is actually nothing to worry about! But everything to smile about! Dr. Galati got it right last visit. He said for five years no one has ever had trouble with this. But he said we couldn’t ignore it either. Glad we got it done! And are hearts are full of relief and praises for Kevin’s healing in His hands! (I’ve dosed off so many times writing this…too tired but not too tired to rejoice in this good news!)
October 3, 2016
We went for labs but the standing order had expired. 6 months ago in April this was given and who knew we would be where we are…needing another standing order for weekly labs:0 Since we will be in the medical center tomorrow I will drop by the form the lab we go to wants completed. I think every tech in the lab knows exactly what to draw and they probably know his birthday after repeating it so often. But it will be nice to not have to be on the phone and even nicer to actually drop by the office and not have an appointment!
Thursday September 29, 2016
Kevin’s EUS procedure is today. I sent this prayer request to our church: “Please be in prayer for an endoscopy with ultrasound procedure (EUS) Kevin is having. They want to get sample pieces of a lymph node that they have been keeping an eye on. We ask that the He would guide hands during the procedure and give great wisdom and discernment to all involved in reading the results and continue to strengthen, settle, and establish Kevin through this entire process.” Pastor Pope was in the waiting room before we were and prayed over Kevin. He gave us an encouragement from the Psalms and explained how many times silver is heated until it’s ready. I love that he expressed that he thinks Kevin has been heated enough because those are my thoughts as well! I will say these last few days Kevin has been on and off with a low grade fever, nausea, and side pain. We called in to the doctor and made sure they knew. We can treat most of this symptoms at home. I also wanted to be sure he could do the procedure today and the assistant said yes because many times the procedure may shed some light on why he’s having some symptoms. So. That’s good to know.
I sent this text update : He’s out. Me and Cole are back here waiting for him to awaken. Dr. Nguyen came out. He said all went well. He biopsied that area. We’ll see. He said he does have something new. Esophageal varices … he said get w Dr. Galati. They usually “band” those but so far he’s not bleeding from them. It’s from his enlarged liver pressure on the esophagus. (?) And he couldn’t band today even if he wanted to because they did the Ultrasound. (Whatever that means)
Tuesday Sept 20, 2016
Follow Up w Erin Yates w Dr. Galati
On the drive down Kevin asked me so mom, what questions do we have this time. I said what questions do you have!?! He was like, well, I kind of just want to know what happened at the hospital. (!) {exclamation all mine because like if he doesn’t know and it happened to him then oh my we DO need a recap! Lol!} I think one reason it’s been difficult to write this update is how very special the people in that office are to me. Erin walked in. She smiles and calls us her favorite family! She said I know so much has happened and we always have this result and want this test and admit you for this but I want to ask you Kevin how are you? And how are you processing all of this? {As long as I talk labs and tests I’m strong. As soon as that part of my heart is poked even a little –seepy tears flow} And Kevin had that stalwart pose as he straightened himself on the examine table to brace for his answer but with his hand on his leg and his eyes on me I saw in those eyes, yes, great strength, but also truth. He shared that he’s up at night and she asked why and when are you taking the prednisone. And he said just thinking of everything. This part I can’t even type! Goodness. It’s a lot. I’m remembering. It was a good conversation. And it’s precious to me that she related to him on that more personal level. Then she answered his question of what exactly happened during that 9 day hospital stay! She recapped and explained each new thing with great detail. Then she brought in Dr. Galati. For the longest time he walked in and just stared straight at Kevin. Smiling. Shaking his head. Studying. Kevin told me later he thought maybe he had asked him a question and he didn’t hear him! I said no I think he was just taking you in. And happy to see you out of the hospital in a follow up visit! He asked who all are we following up with and when is the EUS procedure. (Endoscopy with Ultrasound) EUS is Sept 29 with Dr. Nguyen (our ERCP doc!) We said we are following up with endocrine and they called us for that before we could get all the way home from the hospital. He took out his phone and said well I’m calling you now to see how today went! Lol! We are following up with hematology. He asked how we liked her. We loved her! Both of those appointments are Oct 4. We told him we had a call into rheumatology but they returned our call and said that they would look over his charts they can see and call us back. I told him they never called back. He said as he looked around the room that he was making an executive decision and did not think at this time we needed to see that specialist. Then Erin explained more later about how many people are looking because of all the different symptoms he has going on and they just don’t feel like he has any of the symptoms required at least not yet and hate to add one more set of appointments. Of course I am all for less and I am all for seeing whomever we need to see that could shed more light on his healing.
About that concerned lymph node. We asked where even is it! And what to expect. He commented that for 5 years they haven’t had any concerns doing these type of procedures. But they also cannot ignore it. It’s is best to sample the tissue of the enlarged lymph node and keep watching it. About adrenal insufficiency he did agree that Kevin should order some type of medic alert bracelet and explained the significance of that. His body in an emergency if not know by the medical staff could not recover if the proper procedure for such was not followed.
My notes are not in front of me and I know we had questions questions questions! I had a copy of his last CT scan from the hospital and we had circled lots of things. She explained them away. Medical terminology can set you back a piece. I think we were exhausted from the previous hospital stay. It took me awhile to recover emotionally from this sweet visit. (If you can call doctor visits sweet!) but mostly we needed rest. It’s good to be feeling normal again. Back in somewhat of a routine.
Hospital Stay 5 — 9/7/15-9/15/16
September 15, 2016
Good news. It’s discharge day!
8:45 Dr. Escadera hematology/ oncology wants to see Kevin in 2-4 weeks.
9:15 Endocrine and rheumatology
Follow up with them. They defer to Dr. Galati for which steroid and how to stop budesonide
10:45 Dr. Seelbach
Great news all around from him. They are stopping budesonide. Starting 5 mg prednisone. Follow up with all appointments.
2:20 Dr. Khan
Dr. Khan just came in. He said Dr. Nguyen needs to still do a scope. They want him to go in and get pieces of the lymph nodes. We can schedule on outpatient basis. He was like why are y’all looking at me like you do not know. Ummm. Cause we don’t! lol! We missed them yesterday. Kev was at CT scan. Also we were leaving 40 mi it’s ago. Transport just never came. Cole has been downstairs waiting. So. I guess it’s good that we are waiting we got to hear Dr. Khan and that information.
This is to remind me to follow up with that.
September 14, 2016
He just awakened w pain of an 8 on lower back side right. They gave morphine at 6:30. He’s still an 8:( new pain. I am going to ask if its adrena glands because they sit on top of kidneys and they are “waking them up” …gave hydrocortisone yesterday… We were and still may go home today. Yesterday was such a good day! So this is unexpected. They came back 45 minutes later and gave tramadol. At least we can ask the doctors since none of them haven’t rounded yet.
8:10 Dr. Lin
She saw orders for Imuran to be back. It’s been stopped since last Friday. Also when he goes home this time they just want to give the 10 days antibiotic treatment then stop. The daily infection suppression antibiotic isn’t working anymore. We showed her where they moved the IV and she said the best thing is warm compresses. It should be better in a week. It’s a little red and swollen.
10:40 Phuong Imuran dose is increased by half. So 100 mg. The ID doctor is sending him home when discharged with levoquin. We told her about the extreme pain in his back lower side. She will be stopping back in later.
12:30 Endocrine spokesman Dr. Q (?) like yesterday stopped in to say he will be stopping by with the team after 4. We did ask him my thought for Kevin’s pain if the hydrocortisone is waking up adrenal glands and causing pain. He smiled and said no. It doesn’t work that way and it’s just staring. But. It was in my head. It’s a new medicine. So…I linked it.
1:00 Dr. Seelbach he was going to discharge after endocrine team came through today but once he heard about Kevin’s pain he is holding off until morning because he wants a urinalysis and a ct renal scan for possible stones. He also said before realizing that pain that they endocrine team is referring is to an endocrinology/rheumatologist which he’s been wanting us to go see all along. However now there is an actual symptom. He feels sure the adrenal insufficiency is secondary. The ACTH they injected to test it went up while cortisol went down.
2:45 they took him down for his renal CT scan. No one came by once he returned from this. But mostly the tests may not have been ready since they did them kind of late. Hoping to go home tomorrow after speaking to everyone. So thankful his pain subsides as well!
September 13, 2016
Dr. Seelbach 8:00 am He mostly wants to see him off pain meds before sending him home. For sure wants him one more day.
8:30 am Dr. Lin stopped in and said the test of his cortisole were not what they should be. However it’s not her area of expertise so she is sending endocrinologist by and starting him on a hydrocortisone. We have questions for that team later.
8:45 Dr. Escuediere from oncology did stop by but said the labs were not ready for her to look at. It was kind of early.
11:30 Phuong stopped in. Checked him. Encouraged him to get up and about to keep from getting cabin fever! Later he showered and me and Cole and Kevin went down to get tea at Starbucks.
1:30 Dr. Khan and Phuong came in. They want to see him go home tomorrow. They said this place is a cesspool and we don’t want to be around long! They get sick here! I asked about stopping Imuran Friday and should he stop cold turkey or go off slowly. He said ask Galati. That’s his speciality. Anyway. They stopped it Friday because they wanted his numbers WBC to be able to respond. His liver enzymes have stayed about the same so for now it’s not been a problem.
2:00 Dr. Quervishi (?) stopped in from endocrinology to basically let us know that the tests were run and a team rounds after 3. They may be by as late as 5:30 so if we have questions to get them ready. He explained that Kevin has a low adrenal efficiency … It could be simply a side effect of his budesonide steroid treatment he’s been on low dose for a couple of years.
5:15 Endocrine Team came in. The main thing they are concerned about is how very dangerously low his levels are. So much so that they want him to have like a medic alert type bracelet because if he had an accident and needed emergency surgery his levels being this low could cause him to not recover from it. Like his blood pressure would bottom out. His adrenal glands are not producing enough. One number was 1 another was 2. Steroid treatment is the answer. She said it could be as long as 6-9 months if the liver team agrees. She admitted to not be so in the know with what he has going on. So what she is asking is to stop budesonide because it basically is being absorbed into his body instead of acting like a cream and coating his liver and stomach like its suppose to do. And the absorption has disrupted his adrenal gland function. I asked what caused them to even ask for this test originally. She said it was basically a fishing expedition and was glad they found this. He has adrenal insufficiency. So. They are going to speak with Dr. Galati. She said he has the final authority. I asked will the steroid they want him to take treat his autoimmune disorders that the budesonide was taking care of. She said she wants him on 10 mg of hydrocortisone in the morning and 5mg in the afternoon. So like 8am and 2/3pm. Just because this mimics what your body’s adrenal gland function does normally. It spikes at those two times.
*recorded part of this check voice memos
I don’t know their names
Monday September 12, 2016
He’s NPO until after the procedure. No food or drink. It is scheduled for noon. His IV was really bothering him. It has been on and off. So today the nurse looked at it and thought it was swollen so she moved it to his right arm. He said it already feels better.
Dr. Lin 8:15 am she was glad he’s getting the procedure today. She warned us it may be late. Monday’s things run behind she said at hospitals. All backed up. She said his eosinophil levels haven’t moved much from changing antibiotics but she wants to give it time. Also she is watching the white blood cell count.
Dr. Escudier oncology was able to stop in. We saw her colleague Dr. Foot on Friday. She said all the scans look the same so nothing changing means she may want to take a look and do a bone marrow biopsy. If not while I’m the hospital then on an outpatient basis. While everything is enlarged as we’ve known: the liver and the spleen. She said the lymph nodes were enlarged as well and that just means they are doing their job. Also having been on Imuran for 5 years could be a reason so all the more necessary to do the bone marrow biopsy especially since he’s on the transplant list. To be sure no other rare disease is happening in his body. All the counts are a little better. The esonophils not so much. She wants to watch them.
Dr. Lin 10:15 Came in again to explain a test she wants to run. His cortisol labs twice have been low. I think she said hormone inefficiency. They will draw blood. Inject the hormone. Wait 30 minutes and draw it again. Something about the adrenal and pituitary glands sending signals and they are trying to determine which one isn’t releasing properly (?)
1-insufficient hormones
2-allergic reaction
3-parasite
4-malignancy
I finally remembered her list of 4. Just not too sure what they go with. I think it all goes with low WBC and elevated esonophils.
11:45 transport came right on time to roll Kevin over the river and through the woods to the ERCP! It feels like that. From Methodist across Fannin then trough Scurlock and ink Smith tower.
He went back at 1:15. He’s out by 1:45. I’m with him waiting for him to come around. Dr. Nguyen just spoke to me. He said it was a stricture in the hepatic duct — so higher up. This time after dilating he also swept for cytology. Said his gallbladder is problematic too but to risky to remove. He said he’s glad he did it and got him early before too much puss.
September 11, 2016
Dr. Dinakar (1:30p) MRCP did not make them any smarter. Did not see anything that would indicate any other problems. Asked about pain if better, same or worse. Kevin said about the same with pain meds. Called Dr. Nguyn, and he is going to try to schedule ERCP for tomorrow.
September 10, 2016
All through the night they alternated pain meds. Once he had nausea meds. Between though he did sleep.
7:22 they are headed to MRCP. He told me I could just wait here because all I would do down there is wait in a waiting room:) so at least he’s early and can eat when he gets back!
12:30 Dr. Dinakar said he thinks he will need another ERCP. He understands the wait and the caution but would not be surprised if he has another one. He said he is watching him closely and if he has to will contact Dr. Nguyen tomorrow night to set something up Monday morning. He also added another choice for pain medication. He said always have them call! Don’t let him sit in tears.
2:30 Dr. Fainstein this guy is just funny! He said well I stopped the fever all the rest is their problem! We laughed and laughed. Much needed! He said he would like to see Kevin walk around more. Told him to get up even if it’s to kick me out of my chair!
September 9, 2016 Friday
Dr. Lin ID 9:00 am
She wants to change his antibiotic to see if the eosinophil levels go down. If they do it could be he has an allergy to Augmentin. Most have other symptoms like rash or itching. Kevin’s body may be sending that signal another way through elevated eosinophils. She is consulting with Dr. Nguyen. And Dr. Fainstein will be here over the weekend. She explained how the body tries to push out infection to get rid of it. But with his bile ducts blocked it cannot push it out. Also his body doesn’t stop producing bile. It makes bile everyday whether you need it or not.
He’s had nausea, pain, and lack of sleep. Compared to when we checked in he’s actually feeling worse. Boo.
Phuong 12:00 Confirmed his MELD is 15. Recommends ro keep Kevin off Imuran a little longer because the enzymes were the same anyway. Will check on ERCP.
12:45 Came back in after speaking with Dr. Galati. He wants an MRI. And he wants to consult Dr. Escadere a hematologist/oncologist. She said not to worry too much about that “oncology” part but Dr. Galati trusts her. She said remember that spot on the MRI in May that she said not to worry about? I vaguely do. They want to image that. It was a “cardio” something. I will go back and check my notes. Dr. Galati agrees to keep him off Imuran and not to substitute anything. Especially while consulting this next dr. They are going to let Dr. Nguyen know Kevin is in so he is on the radar. They are hesitant to do another ERCP so soon after last one or even again because of its invasive risks.
The cortisone labs to be done in the morning are for adrenal glad test.
*from the MRCP in May the area is called
“Prominent right pericardiophrenic angle lymph node”
She hopped back in once more to confirm that an ERCP is not going to happen yet. Let’s see what al everything else shows. Letting antibiotics do their work. Ordered an MRI/MRCP Dr. Foot is on for the weekend for the oncology team.
1:40 Dr. Carbajal said Kevin’s labs are looking better. Could be the iron and B12. He’s adding potassium pill and IV fluids with potassium. He wants to see what the pain pattern is after the IV antibiotics have a chance to work. He added there is something to help him get sleep if we think he needs it. We had him look at the arm with the IV. Kevin noticed it seemed swollen. He said it looked ok. Could be they can slow down the rate of drip. Always have it checked if concerned. Dr. Dinakar is on over the weekend for gain team.
So the plan for the weekend is control his pain, IV antibiotics changed to levoquin and flagyl tablet, have an MRI/MRCP, consult with hematology/oncology about the pericardiophrenic angle lymp mode and hopefully kee him out of the ERCP:)
5:20 Dr. Foot Great visit… Great explanation of all that he sees they want him to look for. He explained the levels. Why they could be elevated. How stupid the spleen is! Lol! Big spleen can explain the low blood count. Big spleen caused by infection, or antibiotic, or auto immune … All in all he knows they want him to look at everything through different eyes. He mentioned a possible bone marrow biopsy may be needed. May not. The transplant team may want it to confirm he doesn’t have anything going on. But we will wait and see.
6:00 Dr. Nguyen came by. He doesn’t want to do another ERCP so soon but will if he needs to. He wants him to cool off. Let the antibiotics work. He wants to see the images once they are done. He doesn’t think there is an abscess there. He also told a very encouraging story of a 19 year old boy who had PSC like Kevin who just got his liver three weeks ago! He said he came by to see him to just say hi and he was all white. No more yellow:) He hated to see Kevin in here again. Wanted to know how long the last procedure worked. Asked a lot of questions trying to put it all together. Great guy! We really like him:) He’s been with us from the beginning …
9:30 Probably his worst pain ever. Goodness. Earlier they needed to bring him pain meds at 6 and it was 5:30 when she asked if he wanted to wait until 6 to get the fentanyl or take a tramadol now. He said he’d wait. Who knew. Who knew we would experience our first ever floor coding. The noise blared through the halls. Sirens. It was the room next door. Crazy chaos for an hour plus. So after 7 I peeked outside to see gridlock of hospital staff but it was quiet so kind of shocking to know that many people were out there and no sound inside. The commotion had settled and silenced but the crowd was still present. But. My boy was hurting. So I said quietly I am just looking for his nurse. So I called her. She said she wasn’t in the unit but would get there because I told her Kevin was due pain meds at 6. So he got pain meds at 7. Then at 8:30 the new nurse shift change brought pain meds. By 9:30 he was giving me that look to ask for more. It wasn’t time but they offered Tylenol so he took that. It’s all dumb luck. He manages the pain better if they are rotated every three hours. But the chaos disturbed it. Just like last stay the robbing of the Pixis machine did. I need to learn to bring what we have at home! Great day! He was crying the pain level was that intense. Justin had arrived from Lake Charles so we were able to make small talk and try to take his mind off it. He ended up falling asleep and I just silently prayed that he would sleep it off and let the pain meds sink in. Goodness. Goodness. Goodness. I am just so glad the PCA saw he was sleeping and I whispered to come back later he is in a great deal of pain and needs to sleep. He’s such a silent sufferer anyway and why lately the pain intensifies at night we have no idea. Sometimes it’s just too much.
September 8, 2016
Kevin felt like showering but after he asked for pain meds. He’s at a 6.
Dr. Carbajal 10:15 am
•his wbc is trending lower than normal he is starting him on IV iron and B12 (said it helps raise WBC when it’s low he could be susceptible to “freak” infections)
•we asked about Kevin’s HGT and HCT that Tiffany saw was low and he said yes it’s low and for males they usually transfuse below 9. Headaches low energy are a some symptoms of low HGT/HCT. But they want to be careful because of the antibodies in the blood pool (?) he said they like for patients to use their own bone marrow. Something to keep an eye on.
Dr. Galati 1:45 pm –came in while Sargents were here. He mentioned:
•WBC low and tried to think out loud explaining what could cause this
1-spleen is enlarged holding all the red and white blood cells and platelets
2-imuran could cause low counts
3-peculiar that the eosinophil counts are elevated and have been for a while said it could be allergy related. Like to one of the antibiotics but which antibiotic.
4-he mentioned lymphoma because it can cause low counts but said he has an explanation for all of these. He said with all the scans Kevin’s had recently he should have had some reader notice that. But Dr. Carbajal wanted “specialist” I think he said hematologist so he was more or less wasn’t sounding the alarm but he wanted to control the message. (Kevin says this means so when that person comes in mentioning things we won’t be freaked out hearing it)
•For now he’s stopping the Imuran. Kevin wants to ask him later if that is keeping his liver enzymes in check what will happen coming off? Good question.
He’s gonna look at past scans and get back with us.
he joked after he asked if I had any questions and I said not until I look up lymphoma! He said don’t!!! Stay away from it. But just before he came in his phone died on him and he was googling Imuran and lymphoma. 🙂 So. Galati Googles! Lol!
Dr. Lin 4:30 Infectious Disease
She gave us a good anatomy lesson. Described his spleen and how big it is. It should be tucked under his rib cage. It is huge and way below. She said she thinks because the spleen is sucking up all the red blood and white blood cells that is why it’s enlarged and why she thinks his counts are low. She told us a story of her medical school in China of students from the US teaching them English during a fun Halloween costume lesson one of the girls jumped around and hit her left side on a desk. Two hours later she was sick. They said go to ER. Ended up being a ruptured spleen. She told it to us to make Kevin aware of how careful he needs to be. She thinks Kevin needs a stent. She described how it all should work and how tiny the bile ducts are and that things are not working so the spleen is sucking it in. She said they are thinking on what to do. Augmentin is not working. But mentioned it was a broad one. She almost changed it last time. She said she was locked in a mandatory meeting with the other ID doctors. Not sure if it was over Kevin.
September 7, 2016
Kevin was admitted to Methodist by direct admit. Which even though it was a huge wait (9:30 arrival 1:00 room available but needs cleaned 1:45 waiting on transport to the room 2:30 in the room!) everyone said once we got on the floor that it could have been worse through the ER. He was still feverish and his pain level was around a 7. Dr. Carbajal was practically in the room before we were. He did his evaluation and exam and started orders and meds and labs. Tiffany and Grant brought us some food and Cole hopped in on his way back from Lake Charles visiting Justin.
Dr. Fainstein himself came by too. He is the infectious disease doctor we see but so far in the hospital we’ve gotten someone from his team. We have a follow up with him next week for last hospital stay. So he said not to worry he sees him now:) He actually wanted a different antibiotic and said we had a good run of trying to maintain no infection since we saw him first in June. He thinks he will be feeling much better in two or three days. He started him on Meropenem.
Really great team of people so I shouldn’t complain about the wait. Just seeing Kevin doubled over and sleeping down there makes me crazy. We must have been model “waiters” because they slipped us free parking tickets! Lol! Once up here it was cute to hear the different staff saying to Kevin that they heard he was listed. That means they check on him and are happy when good things happen. At least this mom sees it that way.
He is away at X-ray (6:30) and ordered a pbj and chocolate milk for dinner. So I told Keith bring me a pbj and we left Kevin’s fan. It’s on the must bring list too! Kevin said he almost awakened me at 2 am to bring him. I said I really wasn’t asleep. So we both need sleep. I talked to my dad last night (liver transplant Jan 18, 2007, coming up on 10 years ago) and I know I started tearing up. He said Kevin is being brave. And I saw things differently hearing that. My dad would know. He had to be around family and friends when he wasn’t feeling well. Bravery sees bravery. He is a strong brave boy. Pastor kind of surprised us with a visit too. Surprise because on a Wednesday voyaging down here is a trip to get back for services and AWANA starts tonight! He prayed Psalm 27 over him. Such strength. We love our Pastor!
September 6, 2016
Kevin’s doctor won the appeal! He is on the “low MELD in need” transplant list. But bummer he has been feeling awful. We go in tonight if we think he can’t make it until the morning. Praying he can make it in the morning. Much better entry way. Gives me time to do laundry and pack;) he’s fighting another infection in the bile ducts probably. Has had an “almost fever” (99 to 100.2) since last week and a fever fever 100.6+) since yesterday. Goodness. Pray:)
I did sit today and flipped every page of my Bible because I was trying to find a verse I marked. I could see it. Left page. Right column. It was a blessing to see what I had marked over the past two years. I needed the reminder and encouragement as we face probably another hospital stay but more than that another day that Kevin is feeling yucky, tired and feverish. My poor kevy. I can hardly take it and I’m not even the one living it:0 We do serve a mighty God who fights for us and who put us on the path of this doctor who fought for Kevin! Huge praise!!! I hope I can ask how that phone call went! I do so want to know.
September 1, 2016
Maria called and said they decided not to appeal the exception points. Dr. Galati will appeal the insurance and let us know something Tuesday. After taking this call Kevin texted me 99.6…could be the beginning of something or he could have what seems to be going around.
August 31, 2016
Maria: Transplant Coordinator Phoned:
•I now have that headache in my right eye that Dr. Galati use to joke he would get when Kevin’s lab numbers came across his desk after speaking to her! Goodness it was a lot to take in!
•as Dr. Galati mentioned yesterday Kevin was denied the 22 exception points for his recurring Cholangitis (she reminded me this is not a standard exception point request. Most are more life threatening: for example, someone with liver cancer who would die before having a high enough meld score…so, the only cure is transplant–they are awarded exception points. Unfortunately for Kevin he isn’t sick enough and has the relief options available even though she agreed it’s a horrible way of life with multiple trips to the hospital as well as procedure after procedure.)
•she will meet with the transplant team Thursday and discuss appealing this. It can be done in writing or on a conference call. If it’s written it takes up to 21 days. If it’s a call they tell them immediately.
•I misunderstood the points and wait time. I thought once listed, which Kevin is, that every quarter points were added for wait time. Wait time points are only added IF you already have exception points. She kept referring to Kevin’s meld score as his biological one. So his score is his score and it is what the labs say it is. I’ve heard between 7-13. No points. Just his numbers.
•So first she thinks they will decide to appeal the denied exception points. She did say who knows, Dr. Galati could say forget it. They haven’t awarded exception points for this the last five times or he could try….
•Second, he will appeal the insurance decision denying coverage because of Kevin’s low meld score. Kevin needs to be at a 15 for coverage. They went ahead and listed him because you cannot apply for either exception points or coverage without being listed. She said that’s not a problem. He’s listed. He will not get any offers with such a low score and if they unlist him the hospital will have to pay a fee. So. He’s listed. (Those two little words are the only thing I can truly understand after the entire call! Then I quickly remind myself that with our mighty, all powerful, miraculous healing God we’re good! We are TRUSTING Him and bowing the knee to ask Him believing that He will do exceeding abundantly above all that we could ask or think for Kevin’s liver: “For this cause I bow my knees unto the Father of our Lord Jesus Christ, Of whom the whole family in heaven and earth is named, That he would grant you, according to the riches of his glory, to be strengthened with might by his Spirit in the inner man; That Christ may dwell in your hearts by faith; that ye, being rooted and grounded in love, May be able to comprehend with all saints what is the breadth, and length, and depth, and height; And to know the love of Christ, which passeth knowledge, that ye might be filled with all the fulness of God. Now unto him that is able to do exceeding abundantly above all that we ask or think, according to the power that worketh in us, Unto him be glory in the church by Christ Jesus throughout all ages, world without end. Amen.” Ephesians 3:14-21
•If both appeals are denied they will keep Kevin listed and he will be on the “Out of Criteria” list. I need to ask if I can audit the class again. We had her on day one of transplant evaluation and it was 7:30 in the morning and she gave us a lot of information but nothing applied to us like it is now. Anyway, the out of criteria list still requires approval from our insurance because they have to agree to cover a transplant from “a not so pristine liver.” She gave the example of a liver that has 35% fat. Anyone with a 30 meld score is very sick and most likely in the hospital and too sick for a liver that fat. The cut off for transplant is 30% fat. However, Kevin’s 19 year old body could handle that percentage of fat just fine. So once on this list he could possibly be offered a liver with his low meld score of 7. Reactions to this has varied. I get it because I think well, Kevin’s lived with a not so pristine liver already. He’s use to that. But Keith was like we don’t want that give that to the sick old people! The 30 meld sick patients are too sick for that liver and it wouldn’t help them. While for Kevin it actually could. It’s all just scenarios to help us understand because I was asking a lot of questions.
•I asked how many times can we go before the board. I don’t want to wear out our welcome! The longer he has this and the sicker he gets I was thinking maybe we should hold off asking?!? She said no it’s not like that at all:)
•I said he’s not getting rid of PSC anytime soon so is there an amount of cholongitis infections he needs to have to be awarded the exception points. Like let’s say he’s had 4 recurrences and maybe the board says he needs to have a few more to convince them… Again, she said it’s not like that. This is where she explained the cancer patients and how Kevin wasn’t sick enough. What Kevin has isn’t usually awarded exception points for but they thought it was worth a try because of his age and just how sick he is.
•I asked how long does one live after transplant. And reminded her my dad is a transplant survivor now past 10 years. He wasn’t even transplanted until 70 years old. She said if he isn’t like most 19 year olds and takes his medicine like clockwork on the dot he will do fine. But if he is like most 19 year olds and starts feeling better with the new liver and he forgets to take his medication then he goes into rejection that would cause a situation for new transplant and then maybe a chance they wouldn’t list you because you didn’t treat the first organ they gave you well enough. But usually because of the young age they get one. We talked about how Kevin has had to have a medicine routine since he was 14 but I was not making any predictions. I can only imagine he will do well on that front.
•and I did it. I went ahead and went there. I mean, we already have had two no’s so I asked what if these two appeals are both no. What then? I know he’s listed but how do we pay? And can he stay listed? She said she wouldn’t go there yet. She just wouldn’t. And actually this is where she answered my three way catch 22 question. I thought he had to have insurance approval to be listed. And high meld score to get that approval while we don’t have either now. Kevin is low meld score and not covered. And no exception points. But. We serve a MIGHTY God!!! I cannot wait to finish my praise project. The Lord put this on my heart at least two years ago. I was struggling with that part of my prayer life. Praising Him. So I started circling praises in my Bible reading time. Then I challenged myself to find a praise to circle in each chapter. I know He directs our steps in His word and orders our days but am now starting to really see why He led me to circling praises. I am strengthened by each one each day. And in my prayer time or after a phone call like this one I can open my Bible and start flipping pages and can’t help but praise Him!!! My eyes are drawn to the circles of praises and I am strengthened! We will trust in Him…
August 30, 2016
Dr. Galati follow up from the hospital stay. Well, Dr. Galati may as well have dropped a bomb on us. The “board” did not approve the exception points for Kevin. He is still listed and both of us are waiting to hear from our transplant coordinator. I don’t know why it made me cry it just did. I mean it really never was my plan. None of this is my plan. I realized later today that goodness, God doesn’t need the exception points. We were at Kevin’s labs when it hit me that He can heal Kevin and get him a liver however He wants and we will give Him all the glory. I really need to be excited to watch His hand but I was not in that frame of mind earlier. I see Kevin and know how sick he is and then think he has to be that much sicker(!) I really can hardly take the thought of it. And that’s where I’m wrong. I shouldn’t be heaping on those thoughts before they happen. And I was heaping them on…
•Kevin had side pain of a 5 and nausea going in
•Dr. Galati wants labs today then will let us know how often when he sees those results
•he wanted to know what he was doing all day and said it is good when he feels like it to get out of the house “it’s good for your soul” Kevin has been resting and recovering but lately I’d say he’s getting more energy and more mobile.
•he wants us to follow up with ID of which I told him we have tried. We called them. The office said they would look at Kevin’s records and call us back. I said it sounded like getting an audience with a king! Dr. Galati said go right down there after leaving his office and if we have to wait two hours do it. (So we did. However, no doctors were in clinic but we have an appointment for Sept 13 and asked the nurse to please get our question before one of the doctors answered before then.)
What Dr. Galati wants to know is should he keep taking antibiotic daily since his bile ducts were opened. I’m thinking the kid was on daily antibiotic, still ran a fever and had Cholangitis with all that so isn’t really helping. I know the other too. Once he’s off antibiotic he’s got Cholangitis and is back in the hospital. It’s why we are listed. It’s why we needed the points. If only they would let mamas before that board! Lol!
•for now he can stop all carafate and use otc product if and when needed for heartburn
•he said the “dyspepsia–deranged or impaired digestion; indigestion”… Kevin’s dyspepsia was caused by blocked bile ducts. The ten cent word of the day. Dyspepsia. I waited to look it up after leaving the appointment. It sound like some kind of seepage or leakage. Glad it’s just deranged digestion! So now I can call Kevin deranged! Poor kid. What isn’t in that definition is the extreme pain that accompanied that.
•he encouraged again small meals. 6 grapes instead of non nutritional salad. He’s not against salad but for now Kevin needs nutrition in small amounts. Energy and protein. Eggs. Almond butter. Smoothie. Grilled chicken dipped in ranch nibbled on throughout the day. He said all of that because Kevin said his appetite isn’t what it was. But he weighed 168 so that made me happy.
•We have a follow up with him in 4 weeks
•I have a call into the transplant coordinator. I want to know how many points we get for waiting on the list. How often they are given and if we are really still listed. I feel like insurance didn’t approve because he was too low of a meld score so they needed exception points and now that we don’t have those how can we be listed cause he is too low so we don’t have insurance approval. I call it a three way catch 22. Or maybe it’s a straight up catch 22 and it feels like a three way one! What do I know!!!
We texted to see if Tiffany was working and she was! So we navigated our way to that hospital and floor. She was able to take a quick break and walk us around. It was so exciting to see her at work!
Hospital Stay 4 — 8/11/16-8/17/16
August 17, 2016
12:15 Phuong stopped in to see Kevin and check to see if he was fine going home. If he felt better. We asked about counts if he needs to wear a mask: she said no for now but be careful around people. She explained when to follow up and where. Once he’s listed he is seen by Galati in the transplant clinic (we spent two days there during his evaluation) and we use their office as a back up if we can’t get in. She wants a follow up next week. We will be sent home with Augmentin twice a day for ten days then daily. Dr. Seelbach popped in again to ask if we had enough at home. And to tell us to follow up with Dr. Feinstein in a week or make an appointment. Phuong did say their PSC patients experience this same pain and unfortunately it’s a cycle his bile ducts are in because of the disease.
Noon: Maria the transplant coordinator called. He is listed. They mailed the letter for exception points. They have 21 days to get back with them. If it’s approved they will contact insurance. If the points are declined then she said Dr. Galati will conference call with the board. For now he is listed. It’s a low meld score for transplant here so we wont have any offers but he’s listed:) I think he has a MELD of 22 ( w exception points of recurring Cholangitis)…offers start coming around 30…
11:00 Dr. Seelbach walked in and said he gets to go home today!!! He said now we know. He just couldn’t believe it but that blocked bile duct caused so much pain!
Sometimes the discharge takes a while…
August 16, 2016
Last night he had pain at a 7. After the pain meds it went to about a 4 but right back up to 7. He had diarrhea so we need to ask about if it’s Cholangitis related or c diff related. He wasn’t allowed to eat or drink after midnight but didn’t feel like eating or drinking the smoothie Tiffany and Grant brought him. Cole brought a Redbox distraction:)
6:30 am They came and took him for his ERCP.
7:50 am I am in a waiting room now as they took him back.
8:45 am Dr. Nguyen said he was glad we did the procedure. He did have a stricture. Once opened w dilation pus came out:( he only dilated the bile duct. Didn’t need a stent. He said he remembers he didn’t do well with a stent but needed to do that for the first procedure. Kevin is still sleeping in recovery.
He also mentioned that contrast was injected into the gall bladder and came back out or something like that so he feels that it’s working ok. We asked him bedside if it could be the gall bladder …
10:45 Dr. Seelbach was glad when he stopped by that “we figured it out!” Cholangitis. He said that or even the antibiotics to treat that can cause the diarrhea. So since they didn’t do the X-ray yesterday he said no need to today. He told Kevin best case he goes home tomorrow. Worst case one more day after that. And to get some rest:)
11:30 Phuong just left. She was in for a while. We talked while Kevin was asleep. Then she checked Kevin. Such a difference today because they have an answer. She just hates that he’s going through this. Says normally his Bili level is a sign for Cholangitis. So this time it wasn’t so much because it was below 3 coming in. They are doing their best to get him a liver:) I asked about all kinds of things I remembered. Like there isn’t a GGT number in the standing orders. She said there’s no need since it’s already elevated. Now they mostly want the numbers for the meld score. His liver enzymes are elevated from AIH and he is on the strongest medicine for that and any higher can really throw him into unnecessary infections. She said Dr. Galati is working on a letter. She is going to speak with Maria from transplant. We spoke with her yesterday. She told Kevin she doesn’t want him to lose anymore weight. And to eat small things all day. She said be careful out and about because of low counts. But she wants him on the move more. After she examined him he just went back to sleep.
6:00pm I stepped out to get something to drink and ID came! Kevin got to speak to her and once I got back I found her in the hall. She was glad to know the ERCP helped. She mentioned something about in medical school they drilled that “mitochondria” something was a marker for PSC and Kevin is negative. She said when she saw his age and what he had she knew it was rare. She said we have to be careful of the GI tract. It’s all about that but he has to eat! And to be sure to keep Dr. Galati up to date on how he’s feeling. (Boy do we! If she only knew!) She has an accent so I try. But she has a great smile and genuine care on her face when she updates me. I love this place. She wants to watch him overnight. Could go home as early as tomorrow. Cole came up and after watching a red box Kevin felt like walking around! First time since he was admitted last Thursday! Praising the Lord for that!
August 15, 2016
Tiffany brought me food last night! She can park free at certain times:) Right before she was going to leave Kevin asked for pain meds he was at a 7. He got them. They actually didn’t touch the pain. So a little later he called for some. The nurse had to call Dr. Seelbach and he approved another dose. So am hoping for answers for today. That pain was on the liver side.
His weight is up to 166. He was around 160 when we came in Thursday. Such a praise for me!
Here are the daily doctor visits:
9:35 am Dr. Khan and Phuong from Galati’s practice said his white count is better and Bili is down to 2.2. Pain is possible PSC definitely can cause that. They want Dr. Nguyen (ERCP doc) to stop in today. So they felt no CT scan for now. Wait and see what Dr. Nguyen wants.
Somehow they were in and out and I realized all we didn’t ask… Like what page are we on. Is he c diff and neutropenic. Do we still have to be isolated. Can we walk around. I really think Kevin needs out of this room. To help in many ways. But forgot to ask all of that!
11:00 am Dr. Nguyen he said he thinks the bile ducts are scarred so he wants to do an ERCP at 8 in the morning as long as his white blood count is good (nothing after midnight. Eat light last meal). He wants to dilate the bile duct and look and see what is going on. He said recurring Cholangitis can block things. He said they cannot transplant with an acute infection. (I actually started crying because I misunderstood him. I thought we are hopeless because Kevin keeps having recurring infections so how is he ever gonna get a liver!) He apologized for not being more specific. He meant the infection has to be cleared up. And that happens every time he gets IV antibiotics. He said it’s actually more points to raise your score each reoccurrence. I asked him about all of that c diff and neutrophils and he said the c diff is colonized. The conversation about the neutrophils I got when he was saying the explanation but could never repeat effectively. I told Kevin after he left that I need a refresher on how things work inside. So I should google that!
12:00 Dr. Seelbach wants an old school x ray to see what is causing pain in the belly. Kevin said his uncle calls that “bubble guts!” He said good news that he can come off the neutropenic status and all that stuff can come off the door! I did relate to him about what the ID doctor said how his spleen is storing up white blood cells and that he isn’t a true neutropenic. He started a conversation I cannot even follow about how interesting that was and something about platelets and digested:)
Caleigh asked a while back if we were going anywhere before school started. I was like well, we got through the wedding and at the time all things liver transplant evaluation and I said let’s see. I looked at several options. Finally last Sunday I thought even if Kevin wanted to stay back with nurse Tiffany and bro in law Grant the rest of us could go. So we booked San Antonio then a beach stay at Corpus. Less than 12 hours later we started this week in the ER. So for now. We cancelled San Antonio. But kept the beach place. As it stands it will be daddy daughter get away. I told Caleigh she can check out the place and see if we ever would want to return. I haven’t been to corpus since Keith worked there a summer before we were married!
1:00 Maria the transplant coordinator called and touched base. She said since he is in house she will go ahead and order that ABO that was needed to be listed. She said our insurance declined approval because of his low meld score. I said so the peer to peer didn’t work. I said I wish I could go peer to peer with them! She agreed! But they are moving forward. They will list him after the ABO results and will apply for the exception but she said it is not a standard exception that they normally approve right off. So we need prayer for the board to approve those points! I cannot imagine how sick people are that are on the list without points. Kevin’s life the past three weeks has not been good. I misunderstood again a previous conversation. The exception points he gets is based on recurring Cholangitis. Not how many times he has it recur. Kevin thought she looked familiar. And this time I remembered to ask. And sure enough she had a daughter in Kevin’s class. Use to live in Gleannloch so both of her kids did the same schools as Kevin. Small world:) She will call back once he is listed and when the exception points are added. Then the insurance will approve. It takes about 21 days to hear from the board who decides the exception points.
August 14, 2016
Keith stayed last night. Me and the kids came up after church. We actually all were here for Dr. Seelbach’s rounds. He started him on IV protonics just to give his stomach a break from pills. He asked how that was going. Kevin said much better. He said c diff is up in the air. It’s not pathologic. He said to ask Dr. Lin (ID) about all that. He will discuss with the team in the morning but he may want an image of his liver. So a CT scan may happen tomorrow. Kevin is still having some pain in the liver area. He pressed and pressed on it. We were all laughing after he left when Cole reenacted that scene. Pressing on his liver with his fist and entire body asking does this hurt! Lol!
I am staying tonight and headed down for soup when Kevin showered and as soon as I got it he texted me that the ID lady was just in. Asked him if he had pain. He said no and asked if he had diarrhea. He said no. So I missed her. Inconceivable!!! But he said he pulled his phone out but she was talking so he didn’t want to do anything. So. I headed down to the desk and asked if she was still on the floor. The nurses station said she was and I could catch her coming out of a room soon. I was like I don’t want to just accost her in the hall. And they smiled at me and said Go For It! I mean we’ve only been here since Thursday and all we do is wait to see a doctor or hear results. So I saw her in the hall and I did get to have a great conversation with her! (I told her Kevin was suppose to call me. She said she saw he pulled out his phone but didn’t use it and that he listened to her talk and she appreciated that!––she said she was seeing a patient then was going to hop back down but who knew.) Dr. Lin touched on these things with me:
•she doesn’t believe he has c diff
•she said he is a carrier for it
•some test they do (toxin) not sure here
•neutropenic status she doesn’t believe he is true neutropenic. Yes the count is low but she said his spleen is enlarged and he’s storing them up to fight!
•she thinks it’s severe Cholangitis and her main thing to think about is get him feeling better and what antibiotic to send him home with. So she said she wants to see him here at least one more day and will think about what he goes home on.
•she did say now we will know what to do if he ever has diarrhea
(She mentioned something like once the sample is given for c diff if the lab hears no diarrhea they usually throw it out and don’t even check…)
We have the best nurses! We just finished having such a good conversation with one. Leah. I told her I was able to catch the doctor I missed and told her all that she said. She smiled and said tomorrow the entire team will be in and hopefully they will all get on the same page. I think I get that. (Attending dr ordered neutropenic status and ID dr saw c diff. Not sure exactly which page who was on but each has their own speciality…) She told the best story of Kevin. Was so complimentary of him. She said when he first came to the floor (March) all the floor was talking about the young cute single patient:) And how calm and nice he is. And how aggressive all the doctors have been with him. She explained all about the liver transplant and how he will be here before the transplant and then move to ICU and then to Dunn Tower 4 or 10… She said they always tell their patients we want to see you go even though they love having him because that means he will get better and hopefully they will see him in the park or the grocery store. All of this happening and finally getting some resolution and seeing Kevin feeling somewhat better I can say as Pastor prayed over him in the waiting room of his endoscopy last Tuesday that all of heaven is fighting for Kevin and I heard the verse again today in his message: “They fought from heaven; the stars in their courses fought against Sisera.” Judges 5:20 It is so easy to get discouraged and overwhelmed and I have been in and out of that seeing Kevin hurt. It hurts to see your son hurting. But I realized every time I asked God why or is this enough yet can this be enough and what do we do about the white blood count He comforts me. I realize He created us out of dirt. He made our bodies so fearfully and wonderfully. When I start to fall apart over any of the results I know He knows. He knows what we don’t know. Pastor said that in today’s message. He can see in the dark. I have to trust Him and be strengthened and not overwhelmed. He knows what Kevin is going through and Kevin’s healing is in His hands. Cole and I had the sweetest time in prayer last night. At the hospital we hardly have any chairs to sit on. We were home. On the carpet in my room. I was like chairs everywhere and we were sitting in the floor. Before he went to bed we just kneeled over the ottoman and cried out in prayer for His healing for Kevin.
August 13, 2016
5:30 I called in his food and the lady who answered said he was on a “neutropenic diet.” I said a what? She put me on hold. Anyway. She later told me he needed all his food cooked. Because of risk of infection. Then less than 15 minutes later the nurse came in with a mask on. All day it’s been gloves only. She said he was neutropenic. And pointed to the door and sign placed on it to mask up. So Keith passed all of us out a mask. Except Kevin. We are here for him. And apparently want to protect his weakened state from us. That’s how quickly things change. I really have been researching today so I get to get on the Methodist patient portal and learn some more. At some point today Kevin came out of the bathroom after looking in the mirror and said: I’m yellow! I keep checking the inbox. They send all test results to the portal.
3:00 first dose of vancomycin was given. It was in a syringe and Kevin took it orally.
12:15 pm Dr. Seelbach
He actually said they were questioning the c diff result but would most likely treat him for it. He said the ID doctor would be around again. I’ve waited to update because of this but when I asked the nurse if she was coming she smiled and said that he was the only doctor left on the floor and it would probably be tomorrow. I told her I was very literal.
11:15 am ID team Dr. Lin
She came in and explained how one gets c diff and what you do with it. Also how different antibiotics work. His stomach should be a sterile ground but because of the condition of his liver she said “germs are just waiting to get in”… And hat it is such a fine balance keeping the gut in check. Especially on a daily antibiotic. She encouraged once out of the hips oral to take the daily antibiotic with yogurt. I told her he takes a probiotic twice a day. He is fighting two things possibly. The c diff (Clostridium difficile) and Cholangitis (bile duct infection). I asked how it’s treated and how long. She said a different antibiotic called vancomycin. And they would stop his IV antibiotic he’s been taking since he was admitted. She asked about the different symptoms Kevin’s having. He is only having pain and taking antibiotics.
6:20-8:40 am A Series of Unfortunate Events
Kevin was at his pain limit after 6 am during regular medication visit by his nurse. He asked for pain meds. Then…hours later and several trips on my part in the hall and to the desk we found out that the two rooms on his floor containing the Pyxis machine (dispenses drugs) was robbed…. So they had to shut it down. So unfortunately for Kevin he had to go so long before relief. It’s all I can do not to have a fit on the floor. I’m glad I didn’t. But really watching your kid hurt and asking over and over and over for pain meds. Who knew. At my breaking point I did finally ask at the desk what is on the radar for room 769. You tell me what you have that he needs. Because I think we got lost in shift change. I stood in the doorway forever trying to see a nurse or monitor what could possibly be taking so long. I said he asked for pain meds at 6:20. She explained something happened and the machine was broken into. I said couldn’t they get it from another floor. But at least I knew a little. I walked in the room and wrote 8:36 on the board and was going to head back out in 10 minutes.
Than the second unfortunate thing happened. The new nurse for this shift whom we’ve never had walked in with his pain medication and said his stool sample tested positive for c. diff … I’ve been reading up on it but am waiting for the doctor to come in. Maybe this is the reason behind all those weeks of intense pain! But as a friend sent me earlier: once again Kevin doesn’t fit the profile. The only symptoms he has in common with the info I’ve seen is he’s in pain and on antibiotics. He has NONE of the other symptoms … Which may explain why it took so long for them to ask for a stool sample. They were actually looking for h pylori we thought. Who knows. Definitely relieved to know something. Kevin has said every hospital visit that he is older than Keith and I health wise… I believe it! Poor kid!
*Mona who knows us and remembers him from day one is the charge nurse today. She came in and told me the entire story in more details about the theft. I did tell her that the bad guys know when the nurses are distracted because it only takes one hospital stay or a casual observer to see the routine of the floor. Everyone knows shift change and bedside report and there is even a note posted on the door of the nurses room when to not disturb them. To me that is perfect information for a bad guy. But no matter how secure if they want it bad enough they will get in. And he did. Hopefully when she visits again I will get the rest of the story! It’s all on film so another reason it took so long was they were playing back film and trying to warm all the other floors about what he was wearing… Crazy morning!
August 12, 2016
All around going into another night and ready for bed this night is much better than last night. His pain level isn’t gone but so far has finally been managed. Several things helped this: IV bug juice (he’s on Zosyn); tramadol and fentanyl for pain as needed even though they really barely take the edge off; and several days now on carafate. So the “heartburn” GIRD is lowered to between pain level 3-6 but the liver side pain is increasing as is his bilirubin. I get the test results in his my chart so can read them as best I can once they submit them. That’s the only reason I know his Bili went from 2.8 to 3.2 to 3.4 and this is on antibiotic. I’m definitely ready for that to decrease. But the first doctor did mention “sludge”… Ready for a good night’s sleep:) I did say I wasn’t leaving his side until I saw all the doctors. It took all day. Tiffany walked over after her shift ended after 7pm and I mentioned to her that the only doctor we haven’t seen yet is ID and she walked in the door!
8:00 PM Dr. Weinert
She stepped in for ID team. She packed a punch! Leave it to her to just really feel for Kevin and know exactly what he was going through. She’s the bug juice doctor! She seemed to relate so well to what his symptoms have been. She looked at his scope results I had in the binder from Tuesday. She can’t wait to see biopsy results from that. Explained some of the results: esophagitis in lower third of esophagus; a few small polyps; moderate inflammation; friability (she said wet like-paper not strong) and extra acid was found. (That part needs no explanation!)
She was easy to ask questions to and we really showed her where Kevin was hurting.
She referenced H.Pylori and Yeast describing what they look and feel like. Treatment. But no news yet since the biopsy results still are not back from Tuesday’s scope by Dr. Galati.
She said he was definitely cooking up something???
1:40 pm Dr. Carbajal
They are still growing cultures.
Sludge was in the gallbladder
No infection in the wall of gallbladder
Moderate inflammation
Added back azathioprine and Ursodiol
Changed the karafate tablet to suspension at Kevin’s request. The pill really hurt after taking. (Or that evening set hurt)
9:00am Phuong (Dr. Galati’s NP) was in. She took it all in. Asked questions. Just touched bases with us and will get back in touch once she has contacted Dr. Galati and Dr. Carbajal (hospital attending physician) She also will try to touch bases with Dr. Feinstein his infectious disease doctor. (ID) She said it looks like we may be here until Monday but didn’t know for sure. All I know is I don’t want to take him home until we know why he’s having such pain.
August 11, 2016
10:00 pm — But the pain he is experiencing mixed with heartburn and the heartburn has to have another name because there is absolutely no relief. It’s just been rough. I almost think there has to be something else going on. It seems like maybe appendix or gallbladder. And I voiced that. If they say they will check back in an hour and the pain isn’t better in 45 minutes I am on them because he’s is hurting and I think they need to know. (And I’m like well what’s 15 more minutes!) They have been wonderful and when they walk out I have tears just streaming because I know they know. It’s hard to remember their exact words but they are trying to encourage Kevin and tell them they are here and if they cannot help they will get someone who can.
4:00 he had an X-ray so we went searching for food. We missed seeing Dr. Carbajal too. We walked in and the nurse said you just missed him but Kevin will fill you in. I was like yeah right. Here’s what I was expecting from him in a classic Kevin way: it happened. The dr wanted him to skip his immune suppression medication. I’m not leaving the floor today that’s for sure. I will be on a nurses station coffee fast!
11:00 direct admit to Methodist
“When you are direct admitted and they lead you directly to the waiting room… For hours and hours… Midget is getting spot on cubing lessons!” I snap chatted a picture of Cole giving Caleigh rubix cube lessons with that caption. I’m jealous that she actually is getting it! I have no concept or desire to! That’s how they spent their time waiting but Kevin was miserable. Doubled over. He kept asking me to please go see when the room was ready. So I kept asking. They said they discharge at 11 and 5 so we probably wouldn’t get a room now for hours. Very disheartening.
We waited for hours and got on the 5th floor after 2 and moved to the 7th floor before 10. So it could have been worse time wise but it was pretty bad. Before going up they brought him a pain pill. Then once up on the 7th floor and after we met the new nurse we were able to get an IV pain and nausea IV medicines. After an hour it wasn’t helping at all so we called in the nurse who called in an np. At one point between the pain meds he was to the point of tears. I prayed over him and we were both needing a tissue when a tech came in to put a telemetry on Kevin to monitor his heart. Just routine hospital thing he’s worn one before. Kevin was in the chair and I was standing over him. No one in the bed. So the tech was like whose the patient:) I’d give anything to be! I’d trade places with him in a heartbeat.
9:30 am
We got the call back that Dr. Galati wants to direct admit Kevin to the hospital for IV antibiotics. Again I am relieved because now he will get more help than Keith and I can muster up.
8:30 am
Called Araceli at Dr. G. She’s the medical assistant that hugs me when we are in the office:) She is getting a message to Dr. G and will get back to us….very thankful I got her and not a voicemail! We have plans. I just don’t know which plan to implement. One contradicts the other. But once fever enters the picture most everything changes.
7:00 am
Ok. So yesterday wasn’t as good as I thought:( he made it in his bed all night and I was so happy about that. It was great not finding him in any of his spots downstairs. But that was all the success we got. He said he stayed in his bed and just dealt with the pain. The rest of Wednesday he was miserable. Barely ate. I got in from church. He was in tears from the pain. I can hardly take it. He slept in the chair in our room last night. He awakened at 5:30 with 101.5 fever. Will call Galati when they open. He asked for oatmeal and toast so that’s good:)
August 9, 2016
Hurting Out Loud
This is how I am describing Kevin especially these past few days. He has been hurting out loud. Doubled over. So we had to search for answers.
Today’s scope by Dr. Galati revealed:
•no flagrant abnormality
•he discussed at great length our options:
>The daily antibiotic he takes could be causing it. First he sent a message to his ID doctor and will get his thoughts on if he agrees with him or not. He doesn’t like the time of day Kevin takes it. So we will move it to am with food. Easy enough. We will touch base with him Friday at 10. He wants to know if it helped.
>Protonix: He increased it last week to twice a day and now wants him to drop back down to one a day in the morning. Especially since it wasn’t helping.
>Another option is treat bile reflux. So far none of the acid reflux meds and otc and prescription meds have worked so it could be because it’s bile reflux. Which is not acid but alkaline. He said there is a fair amount of bile in the small intestine as usual but with his liver patients sometimes the liquid karafate for bile reflux helps.
>Kevin’s esophagus might have a motility issue. This is the last option to go to. Dr. Galati noticed that his esophagus wasn’t contracting at a normal rate and it could be because he was under sedation or it could be part of the problem for his reflux because it’s not pushing the food through to the stomach. He said there are tests for this and meds as well but before going down this avenue we will cross off the others.
He really spent a lot of time discussing Kevin’s situation with us and showing us his concerns about Kevin’s stomach. He went and looked up the last scope to compare this one too and in all his liver patients he sees some polyps develop on the lining. Kevin’s aren’t unusual enough to be causing what he’s feeling. Some patients have huge polyps and complain about nothing and some show barely anything and show symptoms. It’s not so much of a one to one correlation.
He said he knew we were wanting an “ah ha” moment but for now he thinks implement one at a time. I told him this was an “ah ha” moment for me! I said if we saw Dr. Feinstein at 3 and he gave him the long term daily antibiotic then I took the script straight to cvs and started it whatever time of day it ended up being:) I’m as literal as the day is long. So we kept it at that time because it’s taken once a day. So in my mind once it’s started then. You stick to it!
So we have plans for an answer and I’m calling that an answer to prayer!!! And for now it hasn’t taken away all of Kevin’s reflux and discomfort but it has surely brought great peace and hope for relief.
August 8, 2016
I took kev to ER early this morning. He was doubled over in pain and they gave him a GI cocktail and sent him home. Even though I kept asking has anyone contacted Galati! They just looked at him and said there’s nothing we can do. Sent us home w a script. I said I’m not filling this until Galati approves it. So I called once his office opened and we had a 3 appt. My head hurts from crying and lack of sleep. Kevin just looked and felt so bad. Galati is scoping him first thing in the morning. He wants to look. Says it’s either flagrantly abnormal or flagrantly normal but just needs to see. Been a long hard day. Love that dr!!! He rearranged his entire schedule after seeing Kevin today. Even put us on the schedule to be seen today. Love his staff!
August 4, 2016
4:00 PM
We Heard From the Transplant Committee
Marie called from the transplant committee and said Methodist has accepted Kevin for transplant! That is an answer to prayer!!! However, the team wants him to have a right heart Cath to measure his pressures due to steroids he’s been taking. She said the transplant process is “hemodynamic” and there is a lot of stress on the heart and lungs when he is on the transplant table they want to be sure he can take it. (When they have to stop the flow of blood to make the transplant when it starts again the pressure could be stressful)This needs to be completed within three months. Cardio should be calling in two weeks. He also needs another set of ABO’s which is blood group labs. It’s an abundance of caution but he tests as an O+ blood type. But he needs to have another set stating that.
Currently Kevin’s MELD score is 11 and our insurance will not approve transplants at a score below 15. (At evaluation his MELD was 15. It changes every lab draw) She said it shouldn’t be a problem once they explain peer to peer and once the committee approves “exception points” for Kevin’s recurring Cholangitis which is the reason he needs a new liver. My reply was, well, we could stop taking some pills over here and his MELD score would jump to a 30 which is what they transplant at. She explained that by a year or a year and a half Kevin, with exception points, will be there. Once the points are given Kevin will have a MELD of 22. That increases every three months because points are given for wait time. This is why in a year she said we would be receiving “offers”… So for now she will call again in a couple of weeks after the insurance is settled. Then she will inform us that he is “listed.”
I know that what she says and what He knows are two different things. I was reminded today in my complete numbness of the day (wondering if he was being presented and waiting to hear the news and seeing him in absolute misery every morning for weeks) that we are to be strong and of a good courage! Joshua 1:9 and I told my Rebekah the very verse she sent to encourage me was my verse when I was expecting Kevin, and it’s what I am being encouraged with on a discouraging Kevin day. He knows and His time is perfect!!!
11:00 am
We saw Dr. Pope earlier today because he is still Kevin’s pediatrician/pcp until he’s 21, and we could get in quickly and closely. Kevin was on the couch again this morning sitting up awake and in pain. Intense heartburn. Dr. Pope called Kevin Skelotor because he said he is a skeleton of his old self but said he looked good and his BMI was great! Unfortunately he didn’t love how he got there. He explained all things heartburn and the different levels of medicine as first, second, and third generation treatments. Kevin is on a double dose of the third generation medication so he said it was worth checking if H. pylori may be at play. We fielded a lot of questions and have some follow up things to take care of. Make sure he can see and has access to Kevin’s records and check on the scope.
August 3, 2016
People Ask How Is Kevin
Here is what I don’t say. I find him every morning on the couch. (The past 3 weeks) He’s in pain from intense heartburn. He isn’t getting sleep at night because it hurts. We have done and are on everything he can possibly be on for it. His doctor knows and is going back and forth with us. He is miserable. I am helpless. He said all day it really never goes away it just gets less intense.
Tomorrow is the day or it’s the earliest of the days that his case will be presented to the transplant team. Dr. Galati was out all last week and wanted to be there to present Kevin. They meet every week I think on Thursdays.
August 2, 2016
We called in to Dr. Galati for heartburn questions. He wants him to double the protonics. One in the morning and one in the evening. After the last visit he said wait a few days and start taking fluconizole again to see if that helps. Kevin said it felt like when he had that yeast infection. He’s almost done with that and there has been no difference.
July 18 & 20 2016
“Helicopter Doctor”
Transplant Evaluation
Monday:
This was the first day of evaluation. It was also Tiffany’s first day of work at Texas Children’s in the medical center as well! So we took her with us and picked her up after. Our day was an ALL day one. Perfect timing!
We started the morning with a liver transplant education class. It was a lot of information. It was a lot of the risks. It was an overview and some information we knew. Some we didn’t. And they sent a packet home to read. Dr. Galati and his staff have already introduced us to most of the information starting a year ago and NOW I know why.
In the transplant clinic the entire rest of that day we spoke with a nurse practitioner, a surgeon (btw he worked with Dr. Vera in Memphis years ago where my dad received his liver transplant), cardiologist, dietician, social worker, financial advisor, and he had labs done as well as a pulmonary function study.
We all slept and rested all day Tuesday in recovery! We did have to address paper work including a care plan for 30 days after transplant once he gets on the list. We filled out medical power of attorney and an advance directive. I was tired and one of those made me a little upset. I “go there” when the question’s are “I desire to die as gently as possible or keep me alive in this terminal condition.” Goodness. It’s just not what you want to walk around thinking about. Especially an empathizer like myself. But it is the WISE thing to have. So once we have those notarized our homework is complete for the social worker! Kevin had to talk the most with that guy! He didn’t just ask yes or no questions but wanted to know how he was coping and who was in his support group.
Wednesday:
Final day of transplant evaluation he had the following:
Carotid Duplex Scan, Echocardiogram, Panorex X-Ray, Chest X-Ray, and a Dexa Bone Density procedure.
3:30 Dr. Galati follow up for a one month visit just happened to be on the end of transplant evaluation. Which worked for us because he’s just next door from the outpatient center. The number one thing bothering Kevin at this time is heartburn. That sounds so trivial for what he looks like when he has it. It’s awful. Painful. And could be another episode of a yeast infection from his “infection suppression” daily antibiotic. Dr. Galati liked that phrase! (Maybe even coined it) We asked about a time line for transplant. Like we know he cannot know but I was like 6 years? He said no not that long but maybe not next month or next year! It could all change in a moment based on Kevin’s symptoms. Which we get. We mentioned what will everyday life look like for him. College wise. He said not to be a “Helicopter Doctor” but he wants him to stay around here. (And I feel sure he coined that term and I love it!) Maybe take some online classes which Kevin is not a fan of. So. Maybe he gets a gap year or two … It’s not pressing as Kevin would say.
I should mention the entire medical center complex is an excellent place to catch Pokemon!
July 14, 2016
Kaylon has been blitzing our patient portal and email with scheduling appointments for the transplant evaluation next week. Kevin will have very full and very long days down at the medical center next Monday and Wednesday. I’m gearing up to take it on, and I’m not gonna lie… just peeking at the schedule and emails is a bit overwhelming! But I am so thankful that it is finally happening and that she is completely handling it all. We just have to show up and follow the directions! And that’s really a Kevin “we.” I am praying that the spirit of the Lord will rest upon Kevin and the transplant team and that He will give them wisdom and understanding and wise counsel and be surrounded by His knowledge and love and might! From Isaiah 11:2
July 12, 2016
Patient portal: Erin replied earlier to my replies yesterday that she is glad Kevin is having a little fun and if he’s feeling fine she isn’t worried about the slight change in blood work.
July 11, 2016
Today Kevin and Caleigh left for teen camp in Arkansas with our church. Kevin as a counselor and Caleigh as a camper. They are at Triple S in Rosebud, Arkansas. I am praying for every teen and counselor! And am trusting Him to keep Kevin strong. He left at 6:30 am. I had him get labs Friday because today would be the two week lab day. By 8:00 am I heard in the portal from Erin Yates at Dr. Galati’s office that his Bili and ALT are creeping up. She asked if he was having any fever or abdominal pain. So far none. He is on maintenance antibiotic that so far has been working fine.
I also got a call from KLon. (Methodist Transplant evaluation contact) Actually she called Kevin who was on the bus to camp and asked him the same things she asked me but he said talk to my mom! She knows more! I actually missed her call. But when we finally touched bases she needed to confirm when we would be available to start the appointments needed for the two day evaluations and an email address to start sending the appointments to once she makes them. So, His timing is perfect. It looks like transplant evaluation should begin next week. Tiffany starts her job as a level 4 NICU nurse on days at Texas Children’s Hospital in the medical center next week too! Praising Him for working that out! He brought her from a hospital in Lubbock to Shreveport to Houston. She will basically be a hospital away when we are down at appointments!
July 5, 2016
Kevin has had a much better week. He must be adjusting to the maintenance antibiotics because so far this week no fever has broken through and he’s feeling better. I checked on the transplant evaluation again. Last time I checked they said finance was the hold up. Today they said finance was approved on June 30 and Kilon (?) will be contacting us soon. Kevin had labs last week actually on his 19th birthday. They came back stable and to repeat in two weeks. (However, he is our teen camp counselor volunteer next week and so I might send him in Thursday or Friday since he will be gone all next week) I am praying that he continues to feel better and is strong enough to make it through the teen camp week next week in Arkansas.
Wednesday June 22, 2016
Maybe I shouldn’t have updated. Kevin awakened with low grade fever. 100.5 so already called into Dr. Fainstein because when he said double the dose of Augmentin we don’t know if that means take two at once or take two that day:) and I’m hoping it’s a normal bug …
Tuesday June 21, 2016
We saw ID today. The infectious disease doctor was the best! He walked in and saw Kevin up on the examining table and told him to hop down off of that. So he sat in a chair and we just talked. We answered his questions then we peppered him with ours. He wanted to hear them all first and then he said I have answers. He said I cannot make him well but I can stomp on the bugs. And he stomped his feet.
Our questions:
•is he taking the right kind of antibiotics? •The right amount?
•how often should he be on antibiotics?
•when a fever breaks through and he’s on double antibiotic what does that mean?
•does he have to be admitted to the hospital every time ?
•can he have IV antibiotics at another facility or at home?
He explained that we all have thousands of bacteria all the time. Kevin’s bile ducts have them flowing like a water hose with mud in it. When it starts to slow down that is when the infection sets in. He asked him about his fever and symptoms. Confirmed this is exactly what he is dealing with and said he cannot cure him but will do his best to keep the infections further apart.
Plan A: he put him on Augmentin as a maintenance dose for 30 days and refilled it 5 times.
Plan B: if he has break trough fever he needs to double the dose and see if that helps if it is a low grade fever. If it is 103 then we go to plan c
Plan C: get to the hospital but call Dr. Galati’s office and have them contact him. And go in under the “23 hour day” for observation and IV antibiotics. If he improves they can send him home with one. If he does not improve he will have to be admitted.
He cautioned that once the infection gets in the bloodstream he can get very very sick. I tried to get a question out without tearing up but just going into this office I wasn’t expecting Kevin to weigh 165 with his phone in his pocket and tennis shoes on. I was already heading off the shock of another five pounds down. And he’s been eating well and feeling ok since Friday before the wedding! So it was a struggle. I only was trying to ask if/when he is at that worst with fever and chills and nausea how long does he have or can everything shut down??? Not sure I got that across but he did not have one Kleenex. He offered me a glove! Lol! Anyway, he was very informative and funny.
He point blank asked where is he on transplant. We replied just the initial call. They are due to call us back. He said if you hear nothing else today–call them now. Call them and tell them you are here and can we stop in to see what next we can do to get the evaluation started. He said he is very aggressive! What else are we doing he asked! What else is going on all summer!? You’ve parked the car! You’re here!
He wanted to know where Kevin attended college. He was happy to hear Knoxville and not some town like Crockett Texas where there is only one home health plan! He said he can set him up on IV antibiotics in college if he needed to. Obviously we are rethinking college for now based on transplant talk.
So out the door we went and I literally stood in the hallway and dialed transplant.
I spoke to a gentleman. He put me on hold a bit while he reached out to Angela to see where Kevin stood. He said financial is the hold up for now and he is sending a message to them. He said K-Lon (?) will be calling soon once that is freed up. I said can I have financial’s number or can I contact our insurance. He said no that it’s definitely something they do on their end. I did tell them we were suppose to hear from them again at most in a week and a half and it has been 2 weeks. (And 2 days but whose counting!) He asked if there is anything else they can do and I said we were just waiting. He said he completely understands.
I was very thankful for this entire visit. In our pastor’s message Sunday night he mentioned a phrase that appears in the Bible only three times. All in 2 Kings 4. “And it fell on a day…” I say find the podcast and listen to it because I may completely butcher it! But it kept going in and out of my mind. Even the previous week as I was thinking how much better Kevin has been and how great God is for answering prayer that hearing those words and in the context of his message I know it is exactly where we are. It fell on a day … Something has changed. It had to happen at some point and who knew when the day would come but it fell on a day… Having so many great days in a row and it all had to start somewhere. The ID Doctor said to live your life. Don’t stay holed up. Leave the theater when you hear the cough but get out and don’t stay confined. Exercise. Have plans. As much as he feels like it. It was just so hopeful. My heart is full and blessed. And it is what Kevin has been doing. When he’s down he’s down and when he’s up he’s up. I like him to be up and going. I want him to get all his energy back but am so happy for this plan. So blessed we got to see the infectious disease doctor today. We tried to in the hospital and tried to get in sooner but it fell on…today.
Saturday June 11, 2016
Let me just say on this day Tiffany and Grant had the most enchanting and picture perfect wedding and Kevin was not in the hospital! He actually turned a page for the rehearsal and has stayed strong! Now he finished his last double dose of antibiotics on Saturday June 18. Just in time for the infectious disease doctor appointment.
Thursday June 9, 2016
I’ve done a lot of “falling at His feet” this week!
Kevin saw Phuong with Dr. Galati as a follow up from Tuesday’s fever and this week’s fall apart!” So far we are all good with holding tight and riding it out as long as he is feeling better and not having fever. Big discussion about all his symptoms especially fatigue. He was encouraged to eat 6 small meals and especially eggs and peanut butter (almond butter from trader joes) things that are easily digestible. He asked Kevin if he liked peanut butter and I think was expecting a yes and Kevin was well, not really! We joked that he likes jelly! Dr. G was like who ever heard of a j sandwich!
The question I have couldn’t be asked without a few tears seeping out. I don’t even know how to word it. Today Kevin even commented as we walked in the Scurlock tower that he feels like that appliance that isn’t working until it gets taken to be repaired. He is feeling much better. At this moment. And while we were in the office. Such an answer to prayer! But my question is when this happens and he has that fever and he is so lethargic its just too much. Is this just what we are dealing with. I needed confirmation of some type that these symptoms will recur and I compared it to like an ear infection protocol. Basically when Tiffany was first diagnosed with “reactive airway disorder” when she was little they gave us an asthma action plan. That’s what I need! It was a very very good discussion.
The phone systems are three days old. I told them I cannot get a person and I’m limited to 5 messages a week in the patient portal. Dr. Galati seemed surprised by that and said he would send Araceli in to talk to who is option 6 when we call. (Medical assistant) Yesterday Araceli was my angel from the Lord! When we finally connected I was about to hang up after she told me Kevin needed to be seen today and she said Mrs. Beth I just want you to know that I would be doing the exact same thing you are doing if my child was sick. Just so blessed by that. She did not know I waited on hold for so long. And if I leave a message and haven’t heard something in 30 minutes I need to call right back. She also said that after option 6 if I need to reach her to call back and press option 8. I never heard that as an option! So good to know. I feel like I informed them of their phone system and patient portal and they helped me with doing exactly what I’m doing. They want a phone call if he has fever. They do not want to be surprised by anything! They want in the Kevin loop. Meanwhile we are moving forward with transplant discussions.
He asked Kevin not meaning anything against me but is what I’ve said true to how he is feeling. Kevin agreed. So I’m not hysterical. Not that he was really accusing me of that:) He point blank asked Kevin if he was tired because of being depressed. Kevin said no. Keith chimed in and told the doctor Kevin is never bothered by anything. Kevin told me after that he kind of thought the doctor was taken aback when he said he wasn’t depressed. He did say a multitude of things Kevin is facing can cause fatigue. He definitely wanted to rule out depression. When the infection breaks out it is fatiguing to fight. Low blood sugar. Various things. I’m telling you it just helped hearing all this it connected some dots.
We asked about any medicine that he can take to help with heartburn that will not counter act the antibiotic. He sighed and was like you know he’s on a lot of junk. He recommended taking anything OTC liquid two hours before the evening meds. So we will try that. You just never know when that stuff will hit.
And it’s wedding week people! Tiffany gets married Saturday. Ruth is in from Florida so she hopped in the car along with me and Keith. The boys were so excited!!! They we’re like oh you’re coming! They looked at each other and said, “Good! You can talk to Beth!” The crazies!!! She told me what Ethan highlighted in his Bible this week and it was this verse from Mark 7 about the mother who fell at Jesus feet for her child. You know it’s a familiar one but then it just means so much more when it is exactly where you are.
“For a certain woman, whose young daughter had an unclean spirit, heard of him, and came and fell at his feet:” Mark 7:25
Tuesday June 7, 2016
11:00 pm
We heard from Dr. G around 1:30 today. He talked about bringing him into the clinic or admitting him. I went over all the symptoms. He is especially tired. Had side pain. Lower. Back. Right. Then tonight front full liver. No high fever since this morning. But took nausea medicine twice today. Early. And just before bed. I would say he is not looking good. I can tell he is not feeling well. It’s all just not good. I would say I can hardly take it but I am not taking anything! Kevin is. Dr. G said get labs immediately. And we will regroup in the morning. Also he reminded me of the cycle that he spoke with us about. He asked how Kevin feels about transplant. I said he is fine with it. He wants to feel better. I told him we couldn’t get into infectious disease until the 21. I know they will be able to help in times like these. He also said that he is very concerned about that fever of 101 in the face of being on a double antibiotic. I told him Kevin is very tired today. Very tired. I couldn’t get him to come down the steps he just didn’t have it in him. I told him my daughter is getting married Saturday…
I made Kevin eat a banana earlier so he could take Tylenol to help with the fever. I got him his favorite Gatorade Fierce Grape. I said this is like those Methodist cups they bring when you check in the hospital. I want to see it gone! He did perk up a little. Going to labs wiped him out! He slept the entire way home. Was nauseous. We waited a while in there because since it was so late the great Tech said we needed a stat order to be able to get them quickly. So I called in to ask for one. They have a new phone system and I’m pretty sure I got lost in the loop. After patiently waiting 20 minutes and hearing all the great information over and over I hung up and kept calling and pressing options. Unfortunately not one option got me a person. I either got a recording or I got the your call will be answered in the order it was received. So I kept hanging up and dialing. I also sent a patient portal message to please fax a stat order:) I got someone and they got the message to the right staff to get it. The tech today we have had before. She loves Kevin. Hates to see him not feeling well. She EVEN remembered my daughter was getting married this week!!! She said if I could only bring him to her church he would get healed. And she told Kevin he must have a call on his life because that devil is fighting him. He must be going to be doing something big for Jesus that devil don’t like. Do you love that!?! I love it. We stayed in there for 45 minutes after labs were drawn. She wouldn’t let me leave until I heard from the doctor and gave them the fax. So we left. Then later she called me at home to tell me that it’s all taken care of. They sent the stat fax. We are trusting Him and absolutely taken such good care of.
I was numb. I told Kevin I was. I prayed over him. Then once he was settled I went to my bedroom closet and just got flat on the floor crying out to Jesus to please heal my son. I talked and talked to Him. Praised Him. He is worthy to be praised! I needed strength for this day that I could only get from Him. I am surrounded by the best too. Kevin is cared for this I know. We are loved.
8:30 am
Please pray for Kevin. He woke me at 6 with 99.5. Chills. Nausea. I checked on him now he’s 101 (2 hours later.) Pain in right lower back side at a constant 3. Makes me numb. Very. Very. Numb. He’s on his double antibiotic. And that new anti fungal from the scope last week. He’s had a headache on and off the last three days. Letting him rest. And praying for healing relief.
Thursday June 2, 2016
We got the call from Angela who received the referral from Dr. Galati’s team for Kevin to be evaluated for liver transplant. She is with the Houston Methodist Transplant Center. Kevin spoke with her and answered questions she had about his health history. We will be hearing from them again in about a week and a half.
Wednesday June 1, 2016
Kevin had an EGD procedure today and Dr. Galati performed it. My prayer was for answers and I am praising Him for one!
Kevin has candida … a yeast infection. Dr. G. came through and explained some things afterwards. Asked Kevin to actually point and draw where he has been hurting. Then he confirmed that’s where the yeast was showing up in the scope. He gave him a script of fluconizole for it. He should be feeling better in a few days from esophagus stuff:) He did take a few biopsies of some areas and will get results back from that in 5-7 days. He has slept all day. We had to leave the house at 4:30 am so he has had a long day!
Dr. Galati also asked if we had heard from transplant yet. We have not so I am expecting those calls anytime.
Another praise. We heard from the ID…Infectious disease doctor that we were referred to by Dr. Galati. That office will see Kevin June 21!
Last week’s labs have Kevin as stable at 2.6 bilirubin. Hoping this week’s are lower if not the same. For the record this morning before the procedure his temperature was 99.7 and to me he looked yellow. He said he told the doctor he has been tired.
Thursday May 26, 2016
I reached someone at Dr. Galati’s office who was able to read to me the message in the portal since its down:) Let me tell you there is not an option for that when you call and get their answering choices. Very thankful for the friendly staff there and courteous attitudes for our dilemma. The message stated that yes he needs to see an ID in an outpatient visit. They recommended Dr. Grimes. So I called them next. This doctor cannot even schedule Kevin until they see his medical records so she gave me the fax number and I called Dr. Galati’s office right back. They did say in the message to let them know if we had a problem scheduling that appointment. So, we did. And again Dr. Galati’s staff let me know they would send over Kevin’s latest labs as well as the notes from the last two office visits. (They asked me what did I think they needed and I was like I actually have no idea!) I did tell Laura who answered the phone at Dr. Grimes that I would probably be calling everyday until we have enough information to schedule an appointment. She said that was completely fine:)
Also in the message read to me Phuong wrote that a rheumatologist out patient visit is not required. I would like to know the why behind this just for closure. We had no idea what to do with that information when they told us at the hospital to seek that second opinion. So will remember to ask later when the portal is back up and running.
Wednesday May 25, 2016
*im really tired writing this so mental note to proof for common sense in a little while.:) Kevin had labs done today and we scheduled his endoscopy for June 1. Dr. Galati will perform it. Kevin has really been doubled over at times with heartburn and acid reflux. It’s a dilemma to time the medications for sure. One antibiotic cannot be taken with milk or calcium. So that rules out all things over the counter like Tums and Alkaseltzer tablets. I just feel for him.
I missed a call from Phuong. Her message said she was touching bases about the questions I had from yesterday’s visit. She also said she would drop the information in the portal. Of which I checked and the entire portal is down. So. EPIC must have gotten a hold of that too??? Reminder to call of I haven’t heard or if the portal isn’t open.
Tuesday May 24, 2016
Huge points for me for remembering to trade cars with Keith for today’s visit. He gets my Mini Cooper convertible I get the luxury cruise liner of a Ford Expedition! When Kevin isn’t feeling great it’s the only way to travel to the medical center. I’ll admit I was a little nervous about self parking in the garage in it but once I ducked down all the way through the 9 stories and arrived on the roof of the Scurlock tower I could breathe again!
EPIC system change up must have gotten ahold of the doctor’s office as well. We had a bit of a wait. But once we were called back Phuong kept us for about an hour going over our entire list of questions:
•he went in struggling with side pain, heart burn, and being tired
She wants to scope him next week. Also mentioned that it could be Hyploria. (? Spelling?)
•hospital discharge questions:
–Infectious Disease (ID)
–Rheumatologist
So these two were mentioned this last hospital stay and Rheumatologist was mentioned at a previous stay. I knew they wanted Kevin to be seen by ID but we didn’t stay long enough. So am waiting to hear what she has found out about seeing one or both outpatient. I know I got those overwhelmed tears asking about these because we just don’t know what to do with the information when the doctor walks in the hospital room and says see these types of doctors or he recommends us to. First, I don’t know a particular name for either type. Why would we? What can they specifically do? How do you think they will help Kevin? And where did this come from? Why now? Not in any voice other than simply what? And softly hug? I’m not frustrated just blessed and overwhelmed and literal! I know they all want what is best for Kevin. But when I don’t understand how to do the follow up its just too much. So she explained that ID could really pinpoint the type and amount of antibiotic he needs. The rheumatologist she looked perplexed. So I have her the doctor’s name who mentioned it and she was like. Oh. I know him. I’ll text or ask him what angel he is thinking. Whew!
I also asked just how much history do the attending physicians see on Kevin. She replied basically only what has happened in the hospital. Because if he is seeing Kevin’s entire 5 year complex history that’s one thing. If he is only seeing this weekend and the last couple of stays than he’s not not truly giving us complete information. Something is missing. So I was relieved knowing he couldn’t see 5 years because I thought
–MRCP report said “prominent right pericardiophrenic angle lymph node” and to “follow up” can signal infection .
Waiting for the appointment I had all of Kevin’s medical records from the weekend’s hospital stay. I noticed the MRI/MRCP that they said looked clear had the above words in quotations. I asked Phuong what they even mean and where on earth on his body is this:) Overall she was not concerned. She said it usually pinpoints infection. And since he is about to be contacted to start transplant evaluation they will a heck him throughly. Teeth. Bones. Support. Financial. Insurance. etc. So for us to remember to kee that in the back of our minds. ✔️
•follow up on our medical letter of necessity since Eleanor isn’t at the front desk anymore.
I quickly briefed her on the insurance company denying benefits for the last two hospital stays. She wanted the information sent to her. She wants Kevin to have an endoscopy. Dr. Galati does these EGD procedures himself. Set up for next week. June 1.
•transplant evaluation process MELD score is 17 based on May 16 labs.
She really thoroughly explained the evaluation process. She and Dr. Galati are both on the team. We had lots of questions and she gave us many many answers. One thing she calculated his MELD (Model for End Stage Liver Disease) Score using these numbers:
Creatinine (kidney function), Bili, INR, & Sodium. She explained there are A+ livers usually needed for very chronically ill patients. The B liver can be used for Low MELD in need list.
Hospital Stay 3 — 3/20/16-3/22/16
Sunday May 22, 2016
7:00 am Kevin had an MRCP
9:00 am Dr. Nguyen stopped in and saw Kevin. He didn’t think an ERCP is necessary because his numbers are better his bilirubin is down. Only if there is a dominate structure on today’s MRCP he would need one. He will check back later with results. We mentioned Kevin is starting transplant evaluation and he agreed after several episodes/ cycles it’s important to track them. He said maybe “chronic” antibiotics or long term treatment low dose but infectious disease will help us with that side of it. We explained that he has had 4 weeks of no antibiotics and somewhere in the middle of those weeks he had very normal and great days but then fell apart again. He is currently still dealing with some nausea.
1:30 PM The MRCP was clear. The doctor is releasing him to go home today! He still will be on oral antibiotics but can rest more at home now that his levels are lower;)
Saturday May 21, 2016
Kevin was moved up to the 7th floor. I knew when we came to visit after Tiffany’s church bridal shower and stepped off the elevator on the 7th floor because one nurse stopped us as she was heading out she recognized us. She asked me what room was he in. I went to check the text from Keith and a CA saw me and said 765. It’s precious and sad all in one blow!
Keith and I tag teamed today. He pulled in and texted and I ran down and got in to head to Tiffany’s bridal shower. We didn’t even have to park the car.
They saw:
Dr. Nguyen- he ordered the MRI/MRCP. (Keith might get fired from this job of note taking cause he can’t remember which of the two!)
Dr. Seelbach- he thought Kevin was looking good. They discussed previous treatment for the two ongoing things Kevin has (AIH/PSC) and will speak with Infectious Disease to get another look at it. If it’s bacterial. And to see what they see.
As I told a friend earlier my heart was in two places today. Half at Tiffany’s shower where she was honored and blessed by so many of our wonderful church family. And the other half at the hospital with Kevin. We all invaded his room after and played Disney apples to apples. I know everyone who stepped in for the random things were shocked again to see Kevin in the bed. One lady hopped in to put a band on him and she was full of energy and told Kevin no way should he be in here and to get out! He is too young she said he needs to get better! Our thoughts exactly.
Friday May 20, 2016
2:30 pm. We touched bases with the staff at Kevin’s doctor’s office around 11 and by 11:15 they called and they said he wasn’t where they wanted him to be. So they direct admitted him to Methodist Hospital. We arrived and were simply waiting for the room to be ready when Brandi (Dr. Galati’s staff) found us, sat down with us, and explained what all they were looking for this time in the lobby! 🙂 She said most likely these will take place: an MRI, an MRCP, strong IV antibiotics, and contact with infectious disease. She asked had we seen them ever before. We said no. So one more thing to look over Kevin and rule out. I think that’s pretty impressive to have had her find us before she left for the weekend. And weird. Yet more impressive than weird. You just don’t expect it. But love it all the more.
4:30Settled in the room on the fifth floor. I like all the people here but the room is different. Kevin shares a bathroom with the neighbor next door. On the 7th floor we had our own private everything. I’m a little weirded out just because of the germ factor. Like. I didn’t pack Clorox wipes. And am I allowed to ask what the guy next door is in for?! Yeah. Seems kind of need to know information to me.
It did take many times asking about when the orders for IV antibiotics would start. At one point they said no orders were in yet that they could see. So we said well, it’s only one of the main reasons he is in for. They said they would page Dr. Carbaju (?). I replied. We don’t know him. He doesn’t know us. We’ve never seen him. How will he know what Kevin’s doctor’s office wants? Also Keith asked me if I could contact Dr. Galati’s staff. Well, earlier today I sent a message to start all this and a note in the portal popped up saying I am about to send my 5th message this week and am only allowed 5. So, no. I can’t message them until the week is over patient portal wise! lol I totally get why they have that setting. I never actually needed it until this week. They wanted a report everyday since Tuesday.
The first IV was placed too close to the bend of his arm. And he asked if I could ask if they could move it. We thought let’s move it before all the antibiotics start. Well, they came in and started them anyway. Said they would move it once these stat drips started and they weren’t as busy. So. It was getting late. Kevin was uncomfortable with the IV. Not to mention just feeling horrible. (I’m thinking let’s get this liver and bile ducts cleaned up!) Drip after drip was replaced. I finally asked when would the IV be moved. He is uncomfortable. The nurse went to get the charge nurse and while I was down the hall brushing my teeth she came in. Wanted to move it to his hand. I looked at Kevin. He didn’t want it in his hand I could tell but he wasn’t going to tell her. I already knew he just wanted it comfortably down more on his forearm. So she placed it there. Then she asked after switching the drip to it did he want that first one removed. Kevin said yes:) After she walked out the door I leaned over to Kevin with my fist on my forehead and whispered: what does it take and I’m sorry. Like why would you want it sticking out serving no purpose? We cannot know. Maybe there’s a protocol we know not of. For the record we now know before the first IV is inserted exactly where to tell them to put it. I’m thinking we will be the Starbucks of hospital IVs!
All the while we had to remind them of Kevin’s other medications. Ask when they would be given or should we get the ones from home. The one he takes in the evenings they said they would bring in the morning. I said well then he will be missing a complete dose. Thankfully they got all of that straightened out. And brought his evening meds this evening. We may have “bad patient” by our name in the file but really I am being pleasant and I think informative. And somewhat advocative. (Not sure that’s a word but it means mama advocate in the most intense yet friendly way:)
May 17, 2016
4 Weeks And He’s Falling Apart Again 😦
Well, Kevin made it between infections 4 weeks. He actually started showing signs of not doing great last week. He struggled with a migraine of which I would say it was a really rough one. He had me up all through the night with him trying different things and medicine to relieve the pain. (Tuesday the 10th) Then around the end of the week he was noticeably more tired. And I thought. Hummm. He could just be normal. He has started helping around the church and having longer fuller days. Then Friday morning the 13th we were preparing to leave for Lubbock to pack Cole and UHaul him back here and Kevin had a temperature of 99. His labs came in too and his Bili level was “trending slightly up but stable” they said at 2.9. It concerned me enough to grab all the medicine in the cabinet to take with us to Lubbock just in case. He slept the entire trip. Then Saturday in Lubbock he awakened with chills, nausea, and a low grade fever of 100.6. So I made the phone call to the doctor. And we got busy packing and loading Cole. I realized Kevin was holding his own and Keith told me his back up plan if Kevin got worse was for me and Kevin to just leave and he and Cole could finish the job. Sunday was his worst day. The trip back to Houston was horrible for him. He was mostly nauseous and it killed me to watch him not eat all the times we took a break for food. I knew Monday we would be getting in contact with the doctor for sure. He could hardly sleep Sunday night from the nausea.
Monday from my perspective. So it’s May 16 and we got in from Lubbock at 2:30 am. Kevin was very ill. Couldn’t find a comfortable place. I had gotten a random patient portal message that said his labs were down to 1.9 and that we could extend his labs for two weeks. This should have been good news but it didn’t match with what I was physically looking at. So we slept some then once the office opened I put in my first call. After that message was left and Caleigh was dropped at school I tried to rest. I went ahead and tried to open the file of labs just to look at and realized it wasn’t attached. So I called the office again because I realized that just maybe those labs were from May 3 since it had 9 different things and his usual standing order Monday labs have about 5. No one at the office could actually help with my question. Here is where I was absolutely unable to sleep because of fear and anxiety. I knew I did all I could so far by calling twice. I also know that doctors are on procedures and can actually have days off. The operator informed me when I asked for specific people who we have seen that they weren’t in the office for the day. 😦 I was hoping to get him in on a sick visit but no one was in the office and or they were totally booked. I also know if he was sick enough we would go straight to the ER. Definitely have done that before.
But I am also so very literal. The last word said extend the labs. It was Monday and time for labs. And he wasn’t looking great. And I couldn’t get a call back. I know the office help had to be swamped. So. Keith and I decided to return the UHaul to Tomball and take Kevin for labs. What could it hurt?
I actually sent several messages in the patient portal to Erin. Especially since she was in communication with us dropping labs and checking on Kevin last week. I am limited in those messages because it counts the words. I let them know Kevin wasn’t feeling good. That we called the office Saturday. Well, the answering service. I also mentioned that they may want to check on that service because we did not get not one call back even from the service asking if we heard from the doctor’s office. Maybe that’s just what pediatricians offices do! I knew in the back of my mind if I absolutely needed to contact someone I could keep calling. I’ve totally done that before;)
Sure enough. Erin called late Monday night! She said she likes to poke around in the patient portal especially after taking a day off because she is usually hosed the next day. And I replied I’m sorry! I hosed you at least three times!!! She did say she wanted to see Kevin the next day at 1:00. She was fitting him in. And that Dr. Galati would be with her. So here I was all day “Beside myself” trying so hard not to be and it worked out. It just worked out. And she was about to have us go early for labs elsewhere and I told her that we had them done anyway earlier that day (Monday) and I think I could feel a high five through the phone! We did good.
I am forever thankful for friends and family I can share this with so openly. We did see Dr. Galati and Erin today. It was a tough visit. Kevin does need to be back on the same two antibiotics. Erin also said when I told her Saturday I had my cvs located in Lubbock and ready for the call that she couldn’t believe I didn’t have antibiotics on hand. She said she would take care of that! Sure enough now I have one “in my back pocket” for the next time If something like this happens again. She said call it in then get him in as soon as possible. I’m calling that a genuine mom card right there:)
In today’s visit we had a two part conversation. Part one we learned his bilirubin level from yesterday went up to 3.6 from last week’s 2.9. They are starting him on two different oral antibiotics and want us to check in every day over the next two days. If he isn’t improving by Friday morning they will admit him for IV antibiotics. (He wants to know does he have fever, is he eating and drinking, staying hydrated, sleeping 20 hours, etc)
Part two of the conversation Dr. Galati explained it’s time to talk about transplant. He thought we could push this out to some point or maybe never. But he wants to talk about it now. A way to look at this and not be as upsetting as it may all sound is to talk about it now. Evaluate Kevin. Let the rest of his team set their eyes on Kevin. His entire team wants to evaluate Kevin. He said they are a big team. A big consensus crowd. And sometimes they are tough at making decisions because they are like a bunch of hens with everyone chiming in what they want. He reminded us that his PSC patients they preach this to: early is better. If he passes through the system and they say you know what he’s a little early for transplant then go back and he’s early. But if the consensus is that they see where his staff is coming from because Kevin has had multiple bacterial infections and time between is shorter they may agree and say transplant now. He strongly believes the rest of the group will agree with him that this is appropriate. He recognizes that in 6 months if we don’t go forward with at least evaluation then things could get more complicated especially based on Kevin’s current track record. He said we all prefer to send our patients earlier. He reminded us that patients with PSC have like a wild card for bile duct cancer. Not that its present now but is something to consider. Dr. Galati wants to get Kevin on the radar screen earlier rather than later. This is a process that could take weeks. Kevin will be evaluated over multiple areas: medical, surgical, physical, education, support both financial as well as care. I feel like someone might come see if I have dust bunnies under my washer and dryer! Lol! Actually, they introduced us to a short version of this process and said we would be meeting a lot of people and getting Kevin’s “team” together over the next several weeks. We are taking it one day at a time and one step at a time. We have many questions.
I asked Kevin how he was taking all of this. He absolutely trusts the doctor and knows we are in the best hands. But more than anything else he just wants to feel better. That makes anything I may be struggling with as a mom just fade away. His quiet confidence and complete calmness is contagious. (After a few tears on my part)
For now, if he’s not better by Thursday night or Friday they will admit him for IV antibiotics. If by Monday his bilirubin level hasn’t changed then an ERCP may be considered. He is cautious about that procedure because every time that ERCP catheter goes up in the bile ducts of the liver if the liver is already not draining properly we could be creating islands of bile not communicating which could cause an abscess and lead to all sorts of complications. ERCP is a good tool but he cautioned it can be overused. Labs on Monday which would mean he is not hospitalized and is feeling better!
May 9, 2016
Three Weeks Today
Kevin took his last dose of oral antibiotics three weeks ago. He has been feeling fine! We are so happy to see this, and praise the Lord for each day he gets through! We try not to let ourselves go where we have just been, but cautiously approach each day.
We are now dealing with our insurance company’s denial of Kevin’s two hospital stays. The wording of their denial of benefits would make anyone completely crazy:
“You did not have a serious infection.””You did not have a bad infection.” And my absolute favorite: “You were stable.”
We are trusting Him in every detail of this! We are in an appeal and have asked Dr. Galati and staff to send appropriate letters as well. Keith thinks this is just an initial step most insurance companies take, and that I shouldn’t take it personal. I am openly trying and asking anyone I know to pray for Kevin to find favor with the insurance company and they will do their proper part. (And that I would not “stress this!”)
April 26, 2016
Kevin had a follow up at Dr. Galati’s today. We saw Phong and Dr. Galati. He has been feeling and looking great. They are going to let him return in a month and after this next week’s labs he will possibly get to go two weeks between labs. We actually didn’t even have any questions. I did record this one as well because Dr. Galati wanted to kind of explain the next step. So below is a paraphrase/quotes from the recorded visit:
“Dr. Galati explained that he fits under ‘recurrent Cholangitis’ and it’s just one of those things we just have to watch. He has finished the course of antibiotics and he said we keep our fingers crossed, and we hold our breath, and we say a prayer that you have no more infection. He did mention that it may be that he doesn’t have any more infection. But, if it comes back and he starts having abdominal pain, fever, the bilirubin starts going up again then we have to entertain the thought that it’s another infection. Then that changes the whole picture here to say, now what. We can certainly follow through with another course of antibiotics, maybe another ERCP he’s not sure about that, he has to see that the drainage is going on. But he pointed out at that point he is getting into this viscous cycle of recurrent infection and what’s the roll over, transplant. That is one threshold to say if you meet this criteria then you flip that switch. Then with all PSC patients the risk of bile duct cancer (cholangiocarcinoma) is there. And he said they are always on edge to see that Kevin doesn’t show up with a bile duct cancer. Those in some cases can be transplanted. He said the challenging part about that is that it’s very difficult to diagnosis because the whole liver looks a little odd. All those strictures and beading. Then you can’t pick out, oh, this is the abnormal area lets biopsy that. It’s similar to the complaints people talk about with ovarian cancer, many times its diagnosed very late, tough to diagnose early, so with cholangiocarcinoma your index of suspicion always has to be very high to minimize the chance that you miss it. These are just the things that hang over everybody’s head you know and leads to anxiety. So. With that said he asked when the last Prometheus test was. He said the numbers are better. But for now we will sit tight. He said with Kevin he thinks we do better with small moves. He called him a small dial person.”
It was a good visit. Everyone was so happy to see Kevin looking and feeling better. Such a difference these last two weeks have been! We are praising the Lord for keeping Kevin stable!
Thursday, April 14, 2016
We saw Erin Yates at Dr. Galati’s office for Kevin’s two week follow up. The things I will remember about this visit are the personal ways I see them care for Kevin. Suprenna checked us into the exam room and she made a comment to Kevin that he was suppose to settle down and didn’t she tell him this the last visit. (He had 99 at the last visit and the next day spiked a temperature that she remembered their office had to try to reach Dr. G who was in a conference somewhere. They couldn’t reach him so they called his wife. She called or texted him and Suprenna told us that her ring tone for Dr. G is “Houston, we have a problem!”) I just loved that. I now know when they say they are asking Dr. G, they will hunt him down if they need to for Kevin! But then she told Kevin how much stronger he was going to be after getting through all of this and that he’s handled it better than any grown man she knows. Loved that. Loved it!
Last visit Erin wanted us to see dermatology for a couple of things:
-spots on back and stomach we told her they were Tinea Versicolor normally treated with pill but the dermatologist knew Kevin could not tolerate that so he gave him a cream.
-hand rash we thought was eczema but was also a type of fungal infection treated with a different cream
Both of those have been improving in the last two weeks. She was happy to know we followed up and that it wasn’t anything autoimmune. I love that when Erin walked into see Kevin she remarked: look, it’s my favorite family! We are loved at this place for sure.
She asked him how he’s been feeling and he said he has had a good couple of days in a row. Especially since getting protonix to help with heartburn. And in the last two weeks since seeing her there were exactly two days that he felt great!
She explained that his stable bilirubin of 2.2 could just be his new normal. But once he finishes his antibiotics and it goes say up to a 4 then something is brewing. Anyway she said keep labs weekly and follow up visit in two weeks.
We discussed his weight loss. Actually he is at a good weight but she said globally he has lost 25 pounds. She did explain to him that he would probably be more of a grazer eating several small meals. So to think along those lines. And it made sense with how he has been eating once he was able to get past the heartburn. I told her before that he would be hungry, take a bite of something then be done and hurting. So thankful for the protonix called in earlier in the week.
Note to self: I recorded this one and will listen back to fill in any details later. For now just typing what I remember without my notes in front of me because I had a moment.
Wednesday April 13, 2016
Kevin had a really good day today! He got over 6,000 steps on his Fitbit. He just looked better. The pain from heartburn has been relieved and he’s only been on the protonix for two days. I sent an update to the “SteveCarrieKeynaPattiBillBethJohnJim” group text with this news and love what my sister Keyna responded with:
“Pain is a terrible companion. It’s very selfish and demands all your attention. Patience , love and prayers are it’s weakness. Keep giving him all that and he will beat it! Love and prayers to all of you”
We appreciate all the love and support we get from so many!
He had an eye appointment yesterday as well. They are keeping an eye on his optic nerve through images because of his low dose steroid use and increased risk of glaucoma. He said for now have follow ups every 6 months. Everything looks great.
Tuesday update:
Hooray! My patient portal blitz got through! I heard from Phong. She apologized for the confusion and immediately sent over a script.
Tuesday, April 12, 2016
Kevin’s Bili from this week is staying stable at a 2.2. He is struggling with something normal: heartburn. I sent the message below after calling the doctor and getting no return call.
“I left a message yesterday for anyone to call us back. Kevin is struggling with heart burn. In the hospital they gave him something called protonics?Or rec. an otc med. I’ve given him Tums and Alka seltzer new chews. The lady who answered the phone yesterday told me to call the hospital? I refused. I cannot imagine who I would even ask for over there. So she said she would get the message to any of the people in the clinic. I never heard from anyone. Not sure what to do:)”
I do realize it was a Monday. And busy. I also realize the lady answering the phone has a job that I never want. But with everything he is on we feel like we are not going to just go get anything! My mom told me about the new Alkaseltzer chew tabs. I was hoping it would be a step above tums. He’s miserable. Food is not his friend. He is down to 173.
I blitzed them after lab results came through earlier today in the portal. Am bound to hear something he can have for relief today.
Tuesday, April 5, 2016
Kevin’s labs from last week: Bili 2.2. So, stable from when he left the hospital:) I’ll take it.
He had a better long weekend. It has had its moments. We are watching him like a hawk! Could be the strong antibiotics causing queasiness. Could be something else. He weighs 175. And I’m watching that:(
Thursday, March 31, 2016
4:39 am Kevin called and awakened me. He was feeling nauseous and had a fever 100.5 by 5 it was 101.1 chills right lower side pain. Pointed to bottom of liver maybe but also to back right side. (?)
Also complained of heartburn or chest pain. Gave him tums first. Gave him Zofran for nausea Dissolved under tongue. And Tylenol for fever.
6:10 am the fever was down to 99And he was feeling better. Heartburn was better.
Sleeping:)
Before giving anything I just sat by his bed and prayed over him: Lord, help us help Kevin. Heal him. Help him. Give wisdom to the doctors. Help them know how to help heal him. We need your strength. We know you know what is going on and exactly how you will use him. We know the doctors explain a little of what they think is happening but you know. You gave him his life now please heal him he wants to give it back to you. He has given his life to you. We praise you Lord.
Obviously we are watching him closely and will put a call into the doctor once they open. Will sleep for a bit before then. Just asking for specific prayer now because he is home on 21 days of oral antibiotics. And this morning seems like the beginning of another trip downtown.
I climbed in the bed beside him and watched his countenance change. His fast talking slow. He fast talks with fever. And the bucket went to the side. I left out knowing he is resting and I am praising the Lord for Tylenol and Zofran. We need wisdom for each step.
And possibly, sleep!
2:55 Erin Yates called
She called to check on Kevin. Her boss hasn’t responded yet. 🙂 For now I told her he has been good. No new fever. She said that obviously when there is a fever and you are already on an antibiotic it means one of two things:
1- your bile ducts are clogged and it isn’t getting through (which Dr. Nguyen doesn’t think as of Monday in the hospital)
2- you have some type of a bug that the antibiotic isn’t responding too. It may mean he needs a different antibiotic.
For now. Keep an eye on things. Remember it’s a 24 hour hospital. Call if he worsens. Go in. She will check on him tomorrow. Keep him on Tylenol for fever.
Wednesday, March 30, 201
We had a follow up to his hospital stay. I will add this appointment was at 9:30. We left the house at 8. Got there at 10. I did call and tell them Houston traffic on this rainy day was a parking lot everywhere. They were so sweet and said they understood and to be safe. Takes all the stress away. Actually this was originally scheduled as a follow up after the Spring break stay but since he got out again Monday they said just keep it. It was a good thing we had lots of questions. We spoke with Erin Yates PA for the first time in person. We have now officially met the entire team down at that office! The clinic and hospital. She was very thorough. We talked with her for 40 minutes. It does feel good to know that they really know Kevin and once again we have heard that he has a “unique presentation” of liver disease. She also knew his history and told him he gets a gold star for highest liver enzymes ever as a 14 year old. I told Kevin now that is something for the resume! Lol! I will have to remember to update his more specifically later. We do need to have a dermatology check. It’s just time.
*I recorded this one to post specifics later…Too tired right now.
Hospital Stay 2 — 3/26/16-3/28/16
Monday, March 28, 2016
Kevin is being released!
We are waiting on discharge orders. We saw several doctors and I’ve summarized each bedside chat below. (From most current to earlier in the morning)
Dr. Seelbach
•he stopped in for the first time this stay. We had a different attending doctor over the weekend. He said Kevin’s kidney function looks great, his liver enzymes have improved and thinks like the other doctors that he should be able to go home on a 3 weeks oral antibiotic treatment.
Dr. Nguyen 11:30 Methodist
•he stopped by to look over Kevin
•at this time he agrees with the other doctor that no ERCP is needed
•if bilirubin gets up in the 5’s again he might recommend it but for now longer home antibiotics and he should be able to be released today
•said at home antibiotic treatment is just as effective now
Brandi March 28 11:00 am Methodist
•Recalled his last visit and how long he took oral antibiotics.
•remembered if he was still having any diarrhea she was wanting to test for anything gastroenteritis
•noted he has to be careful with what he eats
•Bilirubin is 1.9 which is good for Kevin
•noted that his autoimmune hepatitis is still not quite controlled. We were/are scheduled for a follow up this Wednesday for the last hospital stay follow up. She wanted to be sure we checked the metabolites for one of his meds. Also she wanted him to have a standing order for labs.
•Dr. Nguyen should stop by. They called him to check in on Kevin
•possible Cholangitis but nothing remarkable and no need for the other test and procedures he’s had done before since he isn’t currently having pain
•she said she looked at his ct scan and commented to Kevin that his liver and spleen are huge. She drew a normal one. (I may insert a picture of the white board drawings)
•basically Kevin’s are almost touching to the point of like almost overlapping. So the tenderness is explained. They are beyond the protection of the rib cage she mentioned.
•normal for people with chronic liver disease to have enlarged spleen and liver
•whatever it is the antibiotics are working. He hasn’t had anymore fever.
•will send him home with 10-14 day broad spectrum antibiotics
•our question was how long do we wait after he has a fever to notify them. She replied that he has a lot going on and that we did good. Fever with him could be anything from blood stream infection, UTI, Cholangitis,… So we did perfect:)
•hoping for longer time between hospital visit!!!
•reminded us of protocol. During office hours they can direct admit to save going through the ER.
•I told her we declined the blood thinner belly shot and opted for walking and she said that is standard hospital protocol which Tiffany already said. I just forgot. Plus. I’m not a hospital protocol person. So when they walk in with stuff I am going to ask all the 5W’s and the H! (Thank you precept Bible studies!)
Dr. Galati and Phong Easter Sunday bedside visit:
•he will only need to be here a few days and possibly be released as early as tomorrow. He is getting IV antibiotics to help “clear the liver.”
•explained the bile ducts even further
•Kevin may have been under treated
•he may have needed more antibiotics
•possibly could be a situation where the Cholangitis recurs often enough that he may need to be put on a transplant list
•he explained the MELD score transplant number and for now this is not an option for Kevin but he continues to prepare and explain this because it is a possibility
•it could be Kevin will finally get over this infection and once it’s cleared he will be fine for a while
•it could be that the infection comes back no matter how much treatment simply because of the plumbing problem. It cannot drain. It is microscopic in those tiny bile ducts up in the liver
•it is a system that like fishing on bodies of water all fisherman in a boat should be able to travel between bodies of water. And the liver is set up that way. All the bile ducts communicate and bile flows throughout freely. But in Kevin’s case the way PSC works is that sometimes the bile cannot drain and the ducts are narrowed or form strictures all around deeply within the biliary tree of ducts so there is no way for the fisherman to get back. This would be an instance after many times with fever and infection to start the transplant request.
•he explained that a low MELD score can be petitioned with a letter from his office and they can ask for so many points based on Kevin’s history of being in and out of the hospital so much.
•it’s an anonymous review board and sometimes they come back with maybe a smaller number of points or grant the points for like 3 months.
•it sounds like it’s a complex system but at least we were introduced to it
•MELD score numbers: he drew a line. At one end is a normal score of 5 and the other end is a 40. Someone with a 40 has about one week left to live. They transplant at 30 +. He hasn’t officially calculated Kevin’s score but based on his bilirubin he is probably around a 9. He smiled and said no one will be talking to you at this number. You are not sick enough.
•we get that and don’t think we are ready for that yet. We definitely are praying for the antibiotic treatments to clear him.
•puss pockets: he explained that these start to form inside the bile ducts because of PSC causing blockage and the nature of this disease the puss pockets even though microscopic after time cannot be treated by antibiotic because nothing can get through. Thus creating an abscess. Once those are present this is communicated with the transplant board and that changes his MELD score.
•home IV vs oral antibiotic: he said Kevin can come into the hospital and get the IV antibiotic and then is sent home with another round. They can play with this scenario. Maybe he goes home with more. Or maybe he needs to be set up at home to have IV three times a week or something like that.
•basically different types of timing works differently for each patient
•PSC already makes it difficult by developing in those tiny recesses that are hard to reach no matter how small the fisherman is
•We asked is there a tiny fiber optic something that could enter those tiny recesses. He said there is something called a mother daughter scope but warned the more you enter the bile ducts the more things are kind of blown up into the deeper recesses so he doesn’t want to go in there too often using Any scope but he would love to invent a fiber optic something to clean it out and then we would never hear from him again! 🙂
•it is tiny up in there which is why Kevin tends to have so far this recurrence of Cholangitis
•we asked will getting a new liver take away the autoimmune hepatitis. He said it wouldn’t but the anti rejection treatment usually keeps it at bey.
•he did repeat if Kevin cannot clear the liver with antibiotics this is when the liver must come out.
•Protein drink has been added for his nutrition. It’s a clear flavored type because of his recent weight loss. He needs good nutrition for complete healing:)
•Albumin protein infusion is being given by IV as well because his protein levels or albumin level was low.
Happy Easter! Praising Him because He is risen and is our all powerful healer!!!
Sunday, March 27, 2016
Kevin is settled back in a room on the 7th floor. It’s after 1 am so his nurse said Happy Easter:)
Saturday, March 26,2016
Shreveport
We put a call into Kevin’s Doctor.
Dr. Galati wants labs to see if he needs to head back to Methodist.
Labs at urgent care in Shreveport Saturday the 26th showed an increased bilirubin 2.6 and another number I cannot recall that could show the biliary tracts are blocked again. (?)
The urgent care doctor and Dr. Galati conferenced called with all of us in the room to decide our options. They were both very concerned about Kevin taking a “quick” turn for the worse and played it safe by giving him 1 gram of IV Rocephin antibiotic as well as IV fluids. Then we zipped our bags because his doctor wanted him admitted back at Methodist in Houston. He is concerned that he is having a recurrence of Cholangitis. Both doctors were just so caring and wonderful. The doctor who never had seen Kevin at the urgent care clinic was remarkable and had such a caring staff. One nurse said as we left that she would be praying for us.
Friday, March 25, 2016
Fever 101.8 and nausea. We slept out on Mam Maw’s couches to keep a close eye on Kevin.
Thursday, March 24, 2016
Keith and Kevin flew to Knoxville to pack up Kevin’s dorm and drive his truck home. They had a good visit with his friends and Dr. Evans. Kevin actually had a rough Thursday night.
Wednesday March 23, 2016
Phong called with lab results. Bili is down to 2.2 She scheduled a follow up for next Wednesday. He took the last of the antibiotics.
Monday 21, 2016
Labs at Tomball
Hospital Stay 1 — 3/15/16-3/18/16
Friday, March 18, 2016
We are going home!!! It’s been a revolving door of doctors all morning:
12:00 pm
Dr. Seelbach
•his bilirubin is 2.4
•he was happy to see this
•he is sending him home with antibiotics to take care of biliary bacteria
•he wants to see Kevin’s liver enzymes and alkaline phosphates go down. He reminded us that when they are elevated that equals inflammation (which we knew but it was good to hear again.)
•along with that he said he knew Dr. Galati was “titrating” things and he hopes things will set at bey
•he said most of the patients he sees are older like 60 with poor liver from alcohol or Hepatitis C. He said it is rare to see autoimmune hepatitis. (Sooo does this mean we are on the party floor!? If so Kevin missed out on the party!!!)
•he did suggest to possibly see a rheumatologist (autoimmune specialist) if these flare ups continue. He did admit that Dr. Galati will figure it out. Talk to him about it. If a second opinion is needed for treatment. (I was like he was our second opinion in the grand scheme of things looking back from beginning)
•we are released to go home once the paper work is complete!!!
11:00 am
Brandi came in and went over a WEALTH of information. I completely chicken scratched up one page of my precept Bible study.
•good news he is getting released today!
•labs Monday or Tuesday
•clinic visit next week
•I did ask this: so what exactly has been going on. Like. If we were to be asked why are we here. I know we should know what we’ve been living but…(smiles)
•she gave this word: cholangitis (so an infection of his bile ducts. That improved with antibiotics.)
•while his body handled this at the same time it kind of was a bit much. Hence, the upward trend of the bilirubin. Anytime that is that high he will experience overall yuck (can you tell this bullet strayed from Brandi’s words to my chicken scratch)
•she recommends sometime this year a liver biopsy. Why: 1} the 2014 biopsy showed he was not Cirrhotic. His liver was stage 3. Stage 4 is the level once there that liver cancer screens need to take place every 6 months because of the risk for liver cancer at this stage. 2} she noticed “Sarcoidosis” in the 2014 biopsy results. (granuloma) I had her spell that word I’ve never heard it before so will have more questions answered later I’m sure about this.
•I could tell she really did some digging and exploring of Kevin’s file 🙂
•we went over dosage amounts for his routine medications since there have been some changes
•Ursodiol now 600 mg twice a day (2 pills 2 times a day with current script) we will get this followed up at clinic next week
•azathioprine keep the same for now. She and Dr. Galati are following his Thioporine Metabolite levels closely for this dosage.
•she is asking for a migraine medication
•I asked for normal headaches which one: Advil or Tylenol. She said Tylenol and only 2,000 milligrams a day. She admitted Advil is better for pain but more of a risk for GI bleeding. (I told her we pretty much overdose on Advil!!!!! She discussed this and actually the dose of Advil is fine. Just not often and there is a max per day. And especially NEVER on an empty stomach!)
10:00 am
Dr. Nguyen (ERCP) stopped in.
•he was happy to see/hear Kevin had a good night and morning
•glad he tolerated normal food
•said his liver enzymes are improving (?)
For sure the bilirubin is 2. ?
•he explained the stent removal because the bile duct was open
•he was able to open up a 4mm balloon and said he’s worried about it happening again but thinks he will be able to just use the balloon next time (if)
•he mentioned something about the stent interfering with the cystic duct. (Not clear on my part if this meant the stent itself interfered or if having the stent in period messed with it)
•I need to call his office to cancel the procedure that was scheduled for Wednesday
•we really like him! He is kind
8:15 am
Dr. Khan stopped in just to check on Kevin. No new information available to him yet. We had a few random questions he fielded but was glad to see Kevin feeling better. He looked over the stent removal papers with us explaining that procedure and answering questions we had about the images.
March 17, 2016
7:00 PM
He is just back in the room:) did great. They removed the stent. Other than that we will wait for morning report. He took nausea medicine. But is talking. We ordered real food. He wanted cheese quesadillas and a Coke. Then the siblings made an appearance at the perfect time again tonight! Kevin showered and was looking and feeling better. We streamed a movie Pirates of the Carribean of which Caleigh has never seen! Stuff like that use to not fit her movie standard of “more friendship and less death!”
So very thankful for answered prayers! So many have lifted Kevin up!
5:10 ERCP
Kevin is having the ERCP scope now. Pray for Dr. Nguyen to see clearly and have a good picture of what is going on. Earlier today one of the staff mentioned that Kevin is a complex case:) Thank you! Praise that he made it in this procedure today and didn’t have to be bumped!!!
10:30 am
•we finally met Brandi McCall, Dr. Galati’s acute care nurse practitioner, (she gave me her card or I am not sure what letters I might assign her!)
•she was very thorough
•we discussed his liver enzymes and his az. dosage (I was able to pull out Keith’s excel spread sheet of numbers and significant facts)
•it helped so much!!!
•she is ordering something for his migraine
•confirmed PSC even looking back to little things I remember them saying like beaded bile ducts and his MRCP and liver biopsies she was confident in this recent diagnosis
•waiting on what the ERCP finds later to tie all this together
•the bedside meeting was basically explaining the life of a PSC patient and what to expect.
•she did half mention Kevin may need to find an online college!
•also she said Dr. Nguyen will be his new best friend: needing a stent removing a stent …
•she went over the “protocol” for the future when Kevin has fever or chills especially a temperature over 101 to call them or if it’s after hours just get to this ER and they will be around to check on him soon.
•she also wanted to be sure we knew a liver transplant has been mentioned, and we have known that especially the latest clinic visit with Dr. Galati.
•mentioned how important it is to stay on top of symptoms so as not to increase the chance of really making him sicker thus putting him in transplant mode quicker. (Absolutely my words she said things more precise and clearly but I’m on rapid recall with Keith out of the room and Kevin asleep!!!)
•fabulous! Can’t say it enough! We are in the right place. I love her!!!!
Other than the way they have patients order food I am happy with his care here. (You have to call in your order. Maybe I’m old school but it’s just weird. So for example today I was up to call at 6:30, because that’s when they open, so he could receive his clear liquids breakfast before he went NPO for his ERCP procedure at 8:00am. And they said like yesterday he can’t have anything he is NPO. I replied but not until 8. Somehow the orders get in and maybe they see the time the order was placed and not the time actually on the order when it actually starts in real life??? So I press the nurse call and jolt out the door to FIND her because it’s a race against the clock. I have to get him not NPO so I can call and be on hold for 10 minutes then they have a 45 minute delivery time THEN it’s cutting it close! All I can say is Kevin was asleep. I think he would have slept through his nourishment had I not been here. And maybe it’s the mama in me that wants my boy to have his last broth!!! He’s been on clear liquids since we’ve been here so we gotta have em!!! At least this mama thinks so. Maybe it’s cutting edge food and nutrition and I’m just not there yet. I just think it’s weird.
10:00 am Dr. Seelbach the attending MD in the hospital stopped in:
•His bilirubin is lower 3.6 (from 4.8 yesterday and 5.1 before that)
•his alkaline phosphates he would like to see lower
March 16 6:00 pm
Dr. Nguyen (the doctor who placed Kevin’s stent 3 weeks ago) visited the room:
•MRI showed fluid around the gallbladder (acites?? Only I heard a form of this word)
•when he saw this he wanted the HIDA scan to see the function of the gallbladder
•initially the tracer wasn’t going into the gallbladder until he received the CCK and the morphine meds.
•the bile was flowing through the bile duct fine.
•He can’t see the stent except on an ERCP. Trying to get that scheduled tomorrow.
•it could be the stent is causing problems with the gall bladder.
March 16, 2016 Wednesday Methodist Hospital Day
The MRI showed an elongated gallbladder and right where the stent was that area was kind of fuzzy. Could be an occlusion. They would see this in the ERCP. Before doing the ERCP they ordered a HIDA scan to get a better image of the gallbladder. The HIDA scan is finished and he is back in the room. The ERCP could possibly be later or tomorrow so he is still on clear liquid diet.
March 15, 2016
Well, maybe it wasn’t a normal virus after all
Kevin was admitted to the hospital. They got him in for an office visit and the team decided to have him admitted for tests. He has not been feeling well off and on since Friday. Fever and chills along with pain and nausea came back Monday night. And to me, after the weekend we had, meant call the doctor in the morning.
They did blood work, an MRI, and the ERCP Doctor stopped by to check on Kevin. His bilirubin was high — 5.1 (I doubled over when I heard that number) So, something isn’t draining. Again. (?)
The ERCP procedure will be Wednesday. (This is moved up one week) The doctor wants to check to see if the stent is “occluded.” I missed seeing him but Cole and Keith gave me what he said. I was happy to know it will take place while he is in the hospital just because of the pain he experienced once we were home from the last one. I am calling the ERCP Doctor visit and the moved procedure one week early an answer to prayer!
And I am thankful for the insight the liver specialist team had to just look at him in the office visit and say they want to admit him. I wasn’t expecting it. But, will admit it’s a relief because I was running out of ideas at home. I mean. We drove to Bahama bucks to help cool him down. He was getting so hot. Not with fever. But just burning up and sweating through his shirt. He was sleeping in a recliner in our room so we could keep a close eye on him. I am calling him being admitted for tests an answer to prayer as well!
Late Macrh 12
He slept most of the day and the symptoms improved. He ate crackers and soup and is sipping 7 Up. I guess he is allowed to have a regular virus and I don’t have to go straight to google “complications with a stent!” The on call doctor did call late afternoon. He said take him to the ER if symptoms worsen and to try to get in Monday otherwise. These words were said to me too: did you know our office is closed on Saturdays! I’m guessing he had a very bad day too. But he definitely heard from me not as Kevin’s mom but as Kevin’s patient advocate! Very thankful Kevin turned a page and praying he stays on this one through the night.
March 12, 2016
Kevin woke us up at 5:30 am with pain, fever, chills, nausea. That is a phone call to the doctor. 5:54 am, 7:18 am, 8:43 am, 9:51 am I did just that. I’ve asked to please call a different on call doctor. The last call the answering service said that the on call doctor is aware of the problem. That he called at 9:43 to tell them just that. So, I can only imagine that perhaps he is consulting with Dr. Galati about what to do or say when he calls me back. All I know is they look you in the eye when you are leaving their office and say call us with any pain, fever, chills, vomit. I walk away from those words thinking oh I hope that never happens. Maybe it won’t! And it has. And again we will wait. At least for now, Kevin is resting with an ice pack on his head and a vomit bucket close by.
March 5, 2016
Mr. Bili Rubin
Well, as I think back on what I meant to post and never have, I have to write this quick one. Because I need the laugh in my thoughts! Caleigh walked through and asked us, “So, how is Billy? And who even is Billy? I thought Kevin was the one who was sick!!!” Littlest sweetie! We do walk around and have walked around talking about Bili. Bilirubin! And at one time in my life I remember not knowing what that even was! Now she knows. And we have a new code name for bilirubin level checks: Mr. Bili Rubin. I will let Cole tell the story one day of her realizing Donald Trump is not Donald Duck!
March 4, 2016
Dr. Galati Follow Up Visit from Kevin’s first ERCP
Dr. Galati asked Kevin how he was feeling. He replied much better especially his energy level. A lot more energy.
He asked if he was still taking his antibiotic. He has a couple more days of this med.
He mentioned since the ERCP Kevin’s numbers were coming down: bili at 2.2 which had maxed out at about 5.8. (Normal is below 1.0)
The doctor asked exactly what made him say he feels better specifically what is it that he feels better today than he did two weeks ago: Kevin said mostly not as tired no stomach upset.
He asked about his appetite along with commenting on Kevin’s weight loss. Kevin has lost some weight but his lowest since his return from college was 180. He weighed in at 185 and we joked about good ole home cooking! He said I could move in with him and his roommate to cook for him…he’s sure that’s what he would have done…we needed the laughterJ
He asked he is sleeping ok: Kevin said yes.
He asked what he is doing about school: Kevin told him he was taking this semester off. Dr. Galati was very supportive of this decision even off the cuff offering Kevin a job at the office. They talked about summer plans and he relayed since he has kids himself in college that a semester here and a year there in the grand scheme of things is not a big deal. It just really is not. And he shared that he took over two years off between college and medical school. He said he learned a lot and was in the work force and was able to travel.
Any pains at all: a little bit in the right side. We asked is this normal…to this he explained that they use to think patients couldn’t feel a stent that was left in. But then once the stent was removed they noticed the pain was gone. So, Kevin is having some discomfort from the remaining stent. Kevin was actually at a 5 today on the pain scale and took a pain pill.
He asked when we’ll see Dr. Nguyen again (did the ERCP procedure) We actually had just heard from that doctor’s office’s patient portal as we were waiting in the waiting room! This was the message: “Hi Kevin, Hope you are feeling better. The path result from your ercp was benign, no malignant cells seen. Please call my office to schedule for ercp/spyglass for further evaluation and stent removal/exchange in 4 weeks.”
Dr. Galati explained that Dr. Nguyen will do another ercp. He will remove the stent, shoot another cholangiogram, and just see that there’s no grunge or sludge in the liver. He reminded us if there is a fever day or night to give his office a call.
Kevin wanted to ask if he would be kept after this procedure since after the last one his body did not recover well at all. The pain was so intense we ended up spending the night in the ER to manage it. But Dr. Galati replied it was tough to tell. It’s a case by case.
WHAT THE ERCP SHOWED
- There is basically bile duct disease through the liver
- It is what he thought: Primary Sclerosing Cholangitis
- What the next chapter will be is unclear a little bit
- What we don’t want to have happen he said was for Kevin to get into this “cyclical bouts” of jaundice–pain–fever because eventually as the stricturing of the liver may progress and does not allow the bile to get out of the liver bilirubin goes up, it becomes a very simple plumbing problem: the liver isn’t draining.
- This is a perfect set up for infection which is called cholangitis.
- There are certainly antibiotics that he can take.
- There could be a situation where Kevin isn’t able to clear the infection.
- Then you’ve got this chronic infection. He will not feel well. And all sorts of different things.
- The one thing to bring up which is the biggest complication is the need for transplant.
- Now, he reminded us he is NOT at that point yet.
- But, it’s almost one of those things that’s worth mentioning every time they see him. Not to drill it into him or pummel him into submission saying “you will be getting a liver transplant at some time,” but he just wants us to know it is one of the options.
- It’s not an option like an elective option…they will not do it for the sake of doing it.
- There are criteria such as a high bilirubin where an ercp does not fix it or recurrent infections meaning you have a fever and take 7 to 10 days of antibiotic you sort of get better and your bilirubin sort of gets a little better and then a month later it’s instant replay: and you do your 10 to 14 days of antibiotic and you sort of get better and then 2 months later it’s the same thing.
- When you map this out over a year you will say, hey, Kevin has been here 4 or 5 times with infection and that would be grounds to think about transplant.
- What happens is the bile ducts: he draws a normal bile duct that has a stone and explains how the bile ducts communicate with one another. So, for example if there is a stone causing blockage and the stone is removed everything is going to drain. It opens up the channels.
-

- But with PSC what you have is these areas where the bile ducts are not communicating: you get a narrowing of the duct and with all these scaring areas he points out here is a stricture and here is a stricture and here is a stricture … so you cannot get a stent up there because it’s too small so everything behind a certain place in the stricture cannot drain.
- Drainage is the key. Oh and by the way there is a high stricture up here. Pointing to the different bile ducts that lace the liver. Nothing from here is able to drain.
- What happens is you get what they call lakes or pools of bile ducts that are isolated that do not communicate with the main bile ducts to drain.
- So that is where it becomes futile to put the stents in because the stent is draining here but it’s not draining all the way out in the periphery. This is where you have to say “game up” and the best solution is transplant.
- The other option with all of these bile duct diseases especially PSC is the risk of bile duct cancer called cholangiocarcinoma.
- One of the many dogmas (like an absolute) in medicine is that if you have Sclerosing cholangitis and if someone has it long enough and you live long enough you will get cholangiocarcinoma. You will get bile duct cancer. (He said this is similar to prostate cancer if a man lives long enough and is 93 years old he’s probably going to have a little cancer in there. It doesn’t matter it may not kill you but you’re going to have it there.)
- With these kinds of bile ducts problems he said they are in a sense always on the lookout for strictures and little tumors things like that that can develop in the liver and that would again be an indication for transplant.
- Now, he did say Kevin could clear up from this and do pretty ok.
- I, the mom, asked that obvious question: are you pretty sure this is Sclerosing cholangitis?
- He confirmed yes, based on the imaging, it’s Sclerosing.
- For now: labs every week
- At some point he will make it monthly and save Kevin’s arms
- He wants to see how fast he is coming down: the bilirubin
- Fever, chills, not feeling right call the office or come down
- Who knows he said his bilirubin may be 1.0 in one or two weeks
- We take the stent out, hold our breath, get labs every few weeks, we will see
- Are we good?
- What’s next…watch him…ercp…stent removal… after this we will get another set of plans
- No need to come back until after the ercp
- We were given lab orders for next week. Phong discussed with us after Dr. Galati stepped out what labs she needed. Mostly based on now she is wanting to just look at the liver. But we need to call if he isn’t feeling well or he is having any other symptoms so she can change the order if needed.
March 3, 2016
Dr. Galati’s office called. Kevin’s bilirubin is down! It’s at 2.2. They want to see him tomorrow. I will say I am looking forward to this appointment. And love that they called! You know they knew we were ready for his thoughts on all that’s taken place. Thankful for His caring hand and putting us in the hands of caring doctors.
This Too Shall Pass
March 1, 2016
As we left his lab place up in Tomball the technician who drew his blood who we have chatted with over these years said those exact words as we walked out of the office. “Kevin, this too shall pass.” She had asked him how school was going. We were honest with her because earlier today he officially withdrew from Crown or at least we officially told the Dean of Students that he will not return this semester. We have great peace about this. Kevin needs time to fully recover, heal, and rest. This semester will focus on getting him well. His timing is perfect. He had labs today. His bilirubin is being monitored closely. It was down to 2 ish before the ERCP last Wednesday. We noticed in the ER the night of the ERCP it was back up to a 4.4. Praying it will all settle out now that the stent is in place. We know the stent will have to be removed. I have to wonder out loud what do they do if the stent gets blocked? Kevin wants to know when they remove the stent can they just keep him overnight! I’m for that! And will ask. It couldn’t hurt. He is feeling ok. Staying home and resting. He is having a little pain and is still fatigued. We are hoping to hear good news from the cytology results where they brushed his bile ducts for samples to test. It is a 7-10 business day wait. And I cried leaving Lab Corp because the words were so precious to me from an almost complete stranger: this too shall pass. He has great things for Kevin. The dean spoke highly of him. And I don’t doubt how much he said he is missed. And I also know as our Pastor texted, “…This is all part of Rom. 8:28. We too have peace. When we cannot “track” our Lord, we will “trust” Him.”
5:00 am ER Released
We just got released w script for pain and naseau. Good news it’s not pancreatitis. It’s just pain from the procedure. His bili 4,4. Literally just got in car. Sleep much needed! Walgreens for pain meds comes first though:)
ER 2-25 16 4:00 am
4:00 am
So far they ruled out pancreatitis and the ER doctor thinks it’s pain from the procedure. He has a call into Dr. Nguyen to discuss these findings.
ER 2-24-16 10:00 PM
He’s experiencing pain so the doctor called ahead to have him admitted to the ER. He said he needs hydration and pain meds and he could be experiencing what is a normal but painful complication from the ERCP: pancreatitis.
Feb 24, 2016 Procedure Day
Kevin is in recovery now. Dr. Nguyen spoke to us and explained that indeed it was a longer stricture in the common bile duct. He “brushed” it (got tissue samples for testing) and put in a stent. It’s currently draining and that’s good. They will leave the stent in for 4-8 weeks. It is such a praise to have an answer.
Feb 22, 2016 part two
The ERCP Is this Wednesday Morning
We met with the ERCP Doctor. He and his entire staff are amazing. Dr. Nguyen asked Kevin questions and examined him and then explained very thoroughly what he will be looking for and described how the procedure will go. I cannot express enough how very impressed we were with him and all of his doctors helping us to do the next thing to get answers.
February 22, 2016
Today is a consultation for the ERCP
We will go today just for a physical exam and medical history consult with the doctor who will perform the ERCP on Kevin. We will find out today when they can schedule it.
ERCP February 19, 2016
His MRCP test last Friday did reveal that his bile ducts were changing and it is the beginning of something. Phong said it showed that he had a “mild irregularity of the something hepatic bile duct.” *something being I heard “impa” hepatic. I need to ask. I think she might have said extra hepatic. (Because I googled it after hanging up and couldn’t find an “impa” hepatic bile duct!) Anyway the procedure will be next week. She is hoping they can get him in on Monday. The ERCP will give us more answers. The procedure is an outpatient one. It will look for a number of things:
•they will go in with a scope and take a look around
•they will see the common bile duct
•is there a gallstone that was missed on the HIDA scan
•they can take biopsies and answer does he have a bile duct disease
•the doctor can look and see is it malignant or benign.
•he can see if the bile ducts need cleaning out…if so they place a stent to drain them. He would have to return in 3-4 weeks to have the stent removed
I reminded her he is taking Ursodiol and has been since his GGT was elevated back in the Texas Children’s Hospital days. She said that she was aware and even mentioned to the doctor should they increase it. He said no for now. It thins the bile to help it flow better.
I asked if he needs to continue on the antibiotic. He took the last one last night. I also asked if and when did they want more labs. She will call me back with Dr. G’s answer.
I asked will this procedure give us answers. She said yes. It will give us more clear picture of what it looks like. I asked will Kevin feel better after this procedure. She said he most definitely should and for example if his bile ducts need cleaned out he should feel better in about two days. I reminded her that he is missing school. She said she is constantly reminding Dr. Galati that we have to get this kid back to school!
His Gallbladder is Normal
This evening we heard that his HIDA scan showed a normal functioning gallbladder. So as excited as we were earlier that the test was completed successfully, I think I had a weak moment and cried about this news after hanging up the phone because I just wanted answers. I was really hoping today they would be revealed. More than anything my heart wanted Kevin back to normal. Piggybacking that news is the next step. They will schedule an ERCP. (This was mentioned in last Friday’s talk with Dr. Galati somewhere below the sketch in the posts after or below this one) I have googled it. It’s like an endoscopy but it also allows “other therapeutic interventions” to take place. (My words clean out his bile ducts)
The dean of students has been in constant contact with us. He has been a great encouragement to me and I’ve passed every thing he says along to Kevin. He said he is a great student and has friends there missing him. I know Kevin misses being at Crown. Especially after I asked him who did he want me to get to sit with him while we attended caleigh’s honor banquet tomorrow night! He might have been horrified at this suggestion! Well, he’s not himself. And I hate to leave him home alone! Keith was like: Beth, he drove himself to Knoxville to college. He will be fine. But seriously. He may be 18 but I would be fine getting someone to hang out! Lol! Maybe Cole can do the “online” thing and play some video games and sort of virtually keep an eye on him. What can I say. You come home to mom. You. Get. Mom!
Thursday Feb. 18, 2016
Take Two Took!
Today the technician said he was going to blame me if the tests weren’t clear because that means we didn’t give him enough fat to eat! Keith and I were like but we had a pizza party at midnight with wings! And precious friends brought by cookies (made with REAL butter!)
And we are happy to report that today’s second HIDA scan was clear! The gallbladder could be seen. So they were able to inject the CCK and do that function test to determine if there is a blockage. (My terms) We are waiting on his doctor to hear today’s report. Definitely praising Him for today’s clear images and for yesterday’s lab results that his bilirubin has lowered some. He is still tired and not feeling great. We are ready for some answers:)
I will leave today’s update with a verse a sweet friend at church sent right when we needed to read it: “This poor man cried, and the Lord heard him, and saved him out of all his troubles. The angel of the Lord encampeth round about them that fear him, and delivereth them.” Psalms 34:6-7
Buy One Get One
When we checked in we were informed that one of the HIDA scans was down and they would be about an hour and a half behind schedule. Once the scan was started it went for at least an hour. He let Keith and I stay in the room too. At some point the technician realized he wasn’t seeing the gallbladder function, so, he called the radiologist to look at the images. They called us in to conference with him and it was decided to redo today’s test Thursday morning. No matter what I know everyone is trying to get answers and for that we are thankful! Kevin was completely wiped out. By the time the test was over and we walked out of there, he had gone almost an entire day without eating plus had a headache on top of all of that.
February 16, 2016
Araceli called from Dr. Galati’s office to schedule Kevin’s HIDA Scan. It is today at 2:00 at Methodist Willowbrook. North Pavilion. She caught him before he ate since fasting before this scan is required. I’m very thankful it is happening today. Praising Him for answered prayers. I know He is in every detail.
February 15, 2016
We waited sooo patiently all day! I even looked at the clock at 4:57 and thought I better call now or never. Instead, they called us…sigh…Phong apologized for the lateness but also said they were deciding what to do next. I’m fine with that. That’s why I didn’t call them–yet!
They want to order a HIDA Scan with CCK. Also, they want more labs to keep an eye on things. They asked how he was feeling hoping the antibiotic helped. But, he is still hurting, tired, and yellow. Even the whites of his eyes are yellow. So we should expect calls in the next couple of days scheduling this. It will be downtown at Methodist.
In the conversation about the MRCP results, they said there was not a dominate stricture and nothing obvious going on. His bile ducts are irregular. (Which Keith says we knew.) She mentioned it could be early signing. But they want to see how the gallbladder is emptying.
So, wait for calls to schedule lab work and the HIDA scan. Continue to pray that the tests would reveal to the doctors what they need to know to get Kevin feeling better, and as they put it back to school!
In my Bible study this week this verse in Romans really spoke to my heart… “And not only so, but we glory in tribulations also: knowing that tribulation worketh patience; And patience, experience; and experience, hope: And hope maketh not ashamed; because the love of God is shed abroad in our hearts by the Holy Ghost which is given unto us.” Romans 5:3-5
If there is anyone I know that can stay standing under pressure this kid can! Our Pastor stopped by almost as soon as Kevin got home last week to pray with him and talk to him. He said Kevin is in “Suffering 101” then took it back and said no “Suffering 404!” Exactly! We are trusting Him with Kevin’s complete care.

Dr. Galati – Notes (February 12, 2016)
This entire post written by Keith after listening to the voice recording of today’s visit…hence the bullet points:)
• Pain – Yes, Stomach
• Pain that sent to ER – No, that pain was in the lower left back
• Fever – No
• Itching – No
• Feel same, worse, tired – Tired
• Chill sweats at night – No
• Keep you from keeping up with school, social events, life after class – pretty wasted after school
• Point to spot where belly hurts -?
• Gallbladder still in
• Pain while pressing where gallbladder is?
• How are bowels – Diarrhea
Overview Liver Disease Process (consensus)
• Kevin has Autoimmune hepatitis with an overlap of a bile duct problem
o Sclerosing cholangitis (PSC) – a systematic inflammation, destruction of the bile ducts
o Primary Biliary Cirrhosis (PBC) – a cousin of that
o Autoimmune Cholangiopathy – something similar
• Like Coke, Pepsi, Dr. Pepper lined up … all look similar with different flavors, but all colas
• Difficult to say which one it is, but it is a bile duct problem
• So, it is a tubing issue (drainage) along with the hepatitis part (inflammation of the liver)
• We have been watching the GGT and it has always sort of been elevated [something I could not hear 7:30] – That points towards a bile duct issue (one of the three above – not sure which-it’s a cola)
• So now the bilirubin jumps up … so now it comes down to – Do you have some sort of a blockage that is not allowing the bile to drain out?
o You may have some discomfort – it may be severe or it may be vague
o Sometimes you will have fever and sometimes not
o Sometimes it will mess with your bowels, other times it may not
• So these are very vague sort of complaints … the fact that you don’t have fever doesn’t necessarily make it better or worse, it is just that you don’t have fever which means no infection
• At the same time, we do know that any patient that has a bile duct problem is more prone to gall stones (actual little rocks that will form in your gall bladder)
• You are also at risk for something that we call sludge (sludge is sludge – thick, sticky bile that doesn’t allow for good flow through the liver. Things become obstructed. Sludge leads to sticky bile that can lead to stones or even more fine, almost like gravel, gritty, sandy type stuff)
• It could be:
o Do you have a stone?
o Do you have some sludge?
o Is it actually your gallbladder that is acting up? Is your gallbladder at the point now where it is becoming inflamed due to sludge, stones, obstruction, low grade infection even though there is not any fever?
• Another possibility is when you have this PSC, PBC, Autoimmune Cholangiopathy (whatever it is) … you do develop scaring in the bile duct. Bile ducts are just tubes. [Draws picture] Bile drains through the tubes.
• What we know is that with these different diseases, it causes scaring. Could it be that at this point in the disease, in the timeline, that you have developed strictures (narrowing). So it just got to the point now that it is narrowed, it was inflamed and now it has gotten to where it is not letting the bile flow. Or is there a narrowing a little higher up in the liver where it is not letting the bile down.
• That would be my first suggestion. That there is some sort of a blockage.
• So there are a couple of things that we can do:
o A variation of an MRI called an MRCP – It’s a regular MRI, but the software and the analysis looks just at the bile ducts. It looks at liver, too, but it focusses on the bile ducts to see if there is an area that is constricted.
▪ If the bile gets stagnant and it’s a little more possible to get an infection and that is called cholangitis (inflammation of the bile ducts). So it is not uncommon at any point … now, last year, 5 years from now or later. Can happen anytime. This may be your first episode of jaundice, first episode of cholangitis, maybe an infection that is just brewing below the point that you are going to get a fever and if we don’t do anything next week we are going to get a call that you have a temperature of 102, [Put on antibiotic (Levaquin) just to cover anything that may come and do the MRCP today.]
o Now the follow-up to this is
▪ the MRCP may come back and show this area looks a little narrowed (smoking gun)
▪ Or may come back with nothing
▪ We have a biopsy (gold standard)
o For the first time as a whole we can look at your whole liver and the bile ducts. It’s like a high altitude picture of all of the bile ducts to see if it is favoring autoimmune cholangiopathy, sclerosing cholangitis. It is tough to tell because you are quite young and you may not have developed all of the signs of what it really looks like. Like the full version. You are still in like the beta testing of what it is going to look like.
o If there is a suggestion that there may be an area of narrowing, the next thing we would do is called an ERCP (this is a scope test – that goes down into the first part of the small intestine, very easy to get into. We can put tiny catheters and inject contrast and it gives basically a cast of the inside of the liver. So we can see if there is a narrowing there, or if there is a well-placed stone there that is blocking the road.
o Or is there what we call no dominate stricture (meaning this is the guy that is causing the trouble) than we can then put a balloon in so that we can clean out the sludge, stone or grit. If this is the only issue, we can temporarily put a plastic stint in there to let it drain properly and clean up and heal an infection that is brewing and then remove it 4-6 weeks later take another picture, shoot more contrast pictures and see that it is draining well.
o Another possibility is that there is no dominate stricture and what we see is … things just happen at a certain time for no reason. It is not that you ate too much pizza, it is not that you didn’t do something or didn’t exercise enough. It’s just that we have this biologic clock and it said … Oh the first week in February, he is going to turn jaundice [gave examples of 12 year olds that this is happening to and 85 year olds that have had this for forty years and this is just now happening to them]. We might see in the ERCP that none of the bile ducts are blocked that they are just all kind of on the raggedy side, a little moth eaten, and it’s more a diffused problem and that there is not one single bile duct that you could put a stint in, or stretch, or take a stone out. It is just the whole thing is diffusely diseased. That would render a different discussion, a different plan, a different approach rather than BINGO, this is the guy, let’s just fix that and see what happens.
• Glossed over it earlier, but it could just be his gallbladder (if this is the case…delete all of the conversation above…) Might just be a gallbladder problem that anyone could have that has nothing to do with the liver, bile ducts, etc.
• He does have a Murphy sign (pain when you press on the gallbladder and take a deep breath) it tends to suggest gallbladder unhappiness
• He could be having a little bit of a gallbladder problem because he is not draining properly.
Wednesday February 10, 2016
Kevin called me and we were just catching up when he mentioned some things that got my attention. One, he missed class again yesterday because after he showered he was just so tired. He said he just didn’t have it in him. Two, he also said that over lunch some of his buddies told him he was looking yellow. And after that who is counting. It’s called send your mother a selfie now! Of which I sent to Dr. Galati. Those worlds collided finally. I think even without the selfie I was going to be hearing from them. And we did. I was trying to fit in a barre class to just keep doing something ordinary when I got the call. Araceli (my hero of the day today at the liver specialist of Texas) called and calmly gave me Kevin’s new bilirubin number of 4.8. Of which I just started silently sobbing. She was so calm and caring. She said Dr. Galati wants to see him this week. She set up a Friday morning appointment and sent orders for labs to be done between now and then. Then she mentioned in the same caring voice that Dr. G wanted him around until things were more “steady.” She mentioned some things that autoimmune patients go through that are perfectly normal. So even though we don’t know what is going on at this particular moment we know at least for now His plan is to bring Kevin home. It’s could be days or months. And really none of that matters. So, Keith secured Kevin a flight home. I was in contact with the Crown Dean of students and his RA. Both are completely wonderful and caring. They are personally seeing him to the plane in the morning. Even his roommate heard from me! Kevin didn’t answer for us to tell him all the doctor wanted so I creeped my own vault of pictures from the August drop off to college. I had taken a picture of the names and phone numbers of the room assignments. Well, it came in handy today anyway! Kevin was sleeping off a migraine but after hearing how elevated his bilirubin was and that he wouldn’t answer I just knew I had to find a physical hand to go check on him. Call me hysterical. I will own that!
Monday February 1 to Tuesday February 9
You can imagine I started the day out with a call in to Dr. Galati. They took the message. I then randomly got a call from the ER in Knoxville. So, I love how the Lord works. I could not ask for the records since Kevin is 18. But Dr. Galati’s office can. So I called them again. I did find out through all this and I mentioned it I know to some. If I had asked them to please tweet these records they would have been posted in an instant. And these are critical. Need now. No. Needed yesterday. And it took until Tuesday February 9 to get them. Both me and Abby (my hero at Liver Specialist of Texas) had done our best. She finally messaged us in the patient portal that they had all the ER visit records and were just waiting to consult with the Dr. G.
January 31, 2016 ER In Knoxville, TN
Kevin called me at 1:30 am on his way to the ER. His RA drove him and the dean of students met him there. He was having extreme pain in his lower back center and left side. They ran tests: CT scan, blood work and urinalysis. Pain and IV fluids were given. I prayed all night! He is back in his dorm feeling better as of 5:30 am they think it was a kidney stone, possible UTI, but his spleen is very very very enlarged. He sounded 100% better from the 1:30 am call to the 5:30 one! They gave him a steroid shot and pain pills and want him to check in with his dr here Monday. He missed classes last Wed and Fri but just over what he says was normal stuff getting use to the food again. I’m asking that He reveal whatever this is to the right medical staff and bring Kevin peace and healing.
“Fear them not therefore: for there is nothing covered, that shall not be revealed; and hid, that shall not be known.”
Mat.10:26
“Thus saith the Lord the maker thereof, the Lord that formed it, to establish it; the Lord is his name; Call unto me, and I will answer thee, and shew thee great and mighty things, which thou knowest not.
Behold, I will bring it health and cure, and I will cure them, and will reveal unto them the abundance of peace and truth.”
Jeremiah 33:2-3, 6 KJV
Not to mention I also heard this most beautiful hymn playing in my head and heart all night “I need thee every hour” … Very thankful for the tone of Kevin’s voice from the 1:30 to the 5:30 call. It was a difference in a plane ticket!
“My flesh and my heart faileth: but God is the strength of my heart, and my portion for ever.”
Psalms 73:2
January 9, 2016 Brown Spots
We noticed brown spots on Kevin’s stomach and back. He is my smooth skin toned child so after he whirled past me on the hover board classic Kevin style lifting his shirt to reveal his belly button to the world (!) I did a play back. And I know the spots were new! But after thinking it was a sign for something going on his doctor’s office said they were not concerned but to keep an eye on them. But I just want to know where did they come from. Google can’t even give me that. Stink!
Dr. Galati visit December 30, 2015
“Chasing the Numbers”
Kevin had an MRI on Christmas Eve. And the last set of labs was over thanksgiving. We saw Dr. Galati today and the first thing he said was when Kevin’s labs come over he gets a pain in his left eye!
He said the MRI results were good. No new issues. So that’s a praise!
He questioned him in areas of his general well being, like day to day fatigue and bowels, course load…
He also really wanted to be sure Kevin is taking his medications properly. He wants another set of labs and will decide what to do with Kevin early next week. He wants to think about it and listed to us these options:
•stay the course which is keep doing exactly what he is doing
•increase steroid and immunosuppressant
•change steroid and immunosuppressant (thinking about putting him back on prednisone. And/ or possibly changing azathioprine to cellcept
All in all he said he is “chasing the numbers.”
Please pray for specific wisdom and guidance for Dr. Galati over the next few days to make the right decision for Kevin’s treatment based on today’s visit and next labs.
Thanksgiving labs
The numbers are elevated and specifically concerning is the elevated bilirubin at 3.3.
July 22, 2015
I was waiting for this appointment with what I call “holy anticipation!” I hadn’t heard from the patient portal, and we had already been in contact so much over the medication that I didn’t mention labs. I knew it took two weeks for one of them, and I knew we were seeing him soon, so I just didn’t think I needed to mention it. But maybe should of. Because yet again. Who knew? Who knew that the labs in other states do not send the results without asking?? I mean Kevin walked in with paper copies of the “orders” and I even have a copy of the orders in case somewhere along the road trip his got lost. So now we really know nothing more about how the new dosage levels are working with his system but will soon enough.
Kevin has lost some weight. That’s a good thing. He hasn’t felt great and has had a decreased appetite so when relaying this to Dr. Galati he wasn’t too concerned. Kevin could pick something up easily and feel this way and eating wrong which was part of the picture due to road trip just is what it is.
The big thing besides getting to walk across the sky bridge and visit Paul was fielding the doctor’s questions about the upcoming men’s hike. I already had Cole and Caleigh since we visited Paul and was glad Cole could field the questions we were peppered with about the drinking water and all questions hike-wise. Part of me I guess was wanting him to say something like you can’t go on this hike! But he’s been hiking 40 years and even went off on some of his hiking stories. He was relieved to know Kevin would be in a group with experienced hikers and with a definite plan. He reminded me that most accidents that happen are due to uneducated and unprepared hikers. So, I guess I will not stress this. Kevin had me leaning on the side of stress because when he returned from the congress he simply said if he felt like he did then he wouldn’t go. So…I got it honest. But he is feeling great now.
We are keeping everything as it is for now since we are waiting on the labs. I do know they had to start a new patient portal and there were new faces in the office so there has been some transitioning just as a normal practice grows and adjusts to new technology. We did notice there were iMacs on the wall! He mentioned this at the last visit. He was awarded a grant for them and can face time Kevin or Keith…pretty cool. And what peace for me with Kevin in TN he said we could be in the office and face time Kevin:)
For now, waiting on labs and he we set an appointment for January over the break.
July 6, 2015
The Sargents dropped Kevin off at the labcorp in Knoxville and as best we could tell it went well. They waited at a chick fil a so its a win win as Christopher would say! He found his lab and a chick fil a!!!
July 3, 2015
Kevin needed labs 2 weeks before his July 22 visit so even though we tried to fit it in earlier we just didn’t get to. So got all the way to the lab. It was closed. 4th of July on Friday the 3rd. Who knew. So with him leaving for Youth Congress on the 4th he got to take his orders and find the lab he will use all next year anyway. So, a field trip with the teens and Sargents on the way to Powell:)
May 13, 2015
Dr. Galati visit. I recorded this one! Well voice recorded. He asked these questions:
When did Kevin take prednisone? How long?
August 2011 for 6 months
Why did they take him off?
We replied because his numbers were so good! He went a year or so with such good numbers. Of course he was still on azathioprine.
When did he start taking Budesonide? How long? Why did he stop?
He was on them from Dr. Walsh from about December 2013. He came off them for scopes all that fall of 2014. We transferred over to this practice in December 2014. Right before our spring break to Alaska Dr. Galati noticed at that March 3 visit (?date) that his numbers slipped back up a bit so he wanted him to add it.
When he started the visit he asked how Kevin felt, and this particular time he really had struggled with migraines. So Dr. Galati really “wondered” out loud. He wondered if the headaches could be from the steroids. We mentioned that Kevin has had migraines as far back as elementary school we remember canceling private lessons and missing baseball games due to bad headaches. We had seen Dr. Pope even about this.
Dr. Galati said the numbers have come down a small amount but not giant. He mentioned there may be some room to adjust the azathioprine. Like increase it a little bit. It’s not a one dose fits all kind of drug. It’s based on how Kevin’s body genetically processes the medicine.
He asked him what he wants to study. Kevin answered that he wants to be a pastor. (I personally will never forget this moment. Dr. Galati was examining him and listening to his chest and back and having him take deep breaths but when Kevin answered that, the doctor, to me, glanced over at me and had an expression of how proud I must be kind of look ??:)… It’s hard to explain but it was a good look. And we’ve gotten crazy looks and responses when he shares his major. So it was a blessing to not get a worldly response sitting in a medical office! That’s mom point of view. MPV)
He challenged him and said he did NOT want him to get up there and put on the freshman 20! I always heard freshman 15… So it’s increased 5 pounds!
He drilled us on the college:
What kind of dorm?
Can you cook for yourself?
Will he have a meal plan?
Is it a M-F with weekends off?
*We were honest. We had visited the school last summer. Kevin wasn’t as diet restricted as he is now. But this man wanted answers! {so much so that I called the school the next day to find out all this so the next visit I was ready for him!}
He discussed the problems with industrial food:)
•high in salt
•high in fat
•high in sugar
Reminded Kevin how tough. Tough. Tough. It will be. He compared it to a feeding frenzy! I threw out there is a salad bar! Kevin already informed me earlier that week that salad is not DINNER. Shared that thought with him. It’s funny but I could tell he was very concerned about what will Kevin eat!!! More so than I was! I actually hadn’t gotten there yet mentally! We have all summer:)
I loved his descriptions of what to stay away from! Like any sort of a pasta casserole…it’s super chalked with fat and calories. Instead stock up on vegetables and if they have a steak or pork chop even a hamburger without the roll baked chicken or pasta with olive oil and pepper. Fish baked over fried. Any thing is better than fried or battered. Grilled shrimp over popcorn shrimp.
Avoid the carbohydrates: breads cakes cookies
Anything casserole with breadcrumbs. He called that just a mess. ( and I thought Panko was healthy! Ssshhhhh not gonna tell him that!)
He related that earlier in his career he took care of all the pediatric liver transplant patients. Even though Kevin is an adult he reminded him he is still going to need some coaching.
He really opened up and shared the horror for all parents sending kids away to college is the same when it comes to a certain level of what are they doing and not doing. But he did remind Kevin that not all the other kids have this problem. He also reminded me not to drive him crazy…asking did he take his meds. (how did he know that was a struggle two years ago. Keith made me turn off my reminder alarm of Weird Al just eat it…(!) to remind me to remind Kevin! By that time it had been two years. Keith said he needs this responsibility so he can be ready to go away.) So I’m allowed to ask every once and a while the doctor said and Kevin should communicate some of that without our asking especially seeing that his refills are up to date and his blood work on schedule. Absolutely love that this was in the conversation! Absolutely!!!
He wants him to increase his azathioprine so from 3 pills to 4 which is 150 mg to 200 mg. The current level is “low normal” for the amount of drug in his system. I asked him if he was ok with the current numbers and he replied it’s not that he’s ok or not ok he is trying to figure out where Kevin lives best. He wants to see him before he leaves for college. So mid July and he wants a Prometheus and labs 2 weeks before that.
The nurse said to stay with local pharmacy for prescriptions because of how they will be playing with the dosage. {insert here the insane amount of times cvs and their office had to communicate to get the amount of pills correct. They just struggled here and who knows why. Something about the way it’s put in the system but let’s just say don’t drive away from the pharmacy or walk away from that counter until you open the bag, check the script, and count the pills. At one point they had only given him 30. I don’t do numbers but I know that isn’t enough or equal if he is taking 4 a day! Patience is the virtue here. It all got sorted out.}
March 13, 2015
Thank you for praying Kevin through yesterday. He started getting his “color back” last night about mid-evening. He even went to school this morning:) He is being carefully monitored. He has labs today and actually has weekly labs for now.
No real answers but definitely peace with a thankful heart and will give God the praise here! I’m going with we prayed that pain away!
He Looks Uncomfortable
Please pray for Kevin this morning. He was experiencing abnormal pain around his liver, went to the school nurse, they sent him home and his liver doctor wants to see him immediately downtown for an ultrasound. They may admit him if they see something on the image they don’t like. He was just “summoned” to this doctor Tuesday afternoon after his recent lab work showed extremely elevated liver enzymes and was put on a low dose long term steroid treatment to try to get his immune system suppressed.
We would greatly appreciate your prayers at this time. Pray for ease of pain for Kevin, safe travel downtown, wisdom and knowledge for the ultrasound technician and doctors looking at the images, and for complete peace about this situation.
A Walk Through the Numbers
March 3, 2015
February 11, 2015
Clean Up On Aisle Nine
That’s my take on this! Everybody in the store currently on aisle nine knows they are on aisle nine. And when the pickle jar drops out of someone’s hands everyone on aisle nine heard it and is stepping around it. Completely in the know. Except the person who needs to clean up the mess. And then You hear it: Clean Up On Aisle Nine! Blaring over the speaker. If you needed something off that aisle buddy you missed it. You’re not going anywhere near it now! I am that clean up! I felt like that after reading the dietary clarification below from Dr. Galati. I feel like after calling and calling to get clarification they went ahead and got on the loud speaker! Only this time saying: Attention All Liver Patients. Herein do we proclaim you have to eat this way! I claim it. I own that. Hopefully not every patient in his office knows why the proclamation was set forth! But when you don’t know…you DONT KNOW:) (That’s one for you Cole)
And when I start to explain this “clean up” you get the I don’t know what you’re talking about look, the I wouldn’t even know where to begin face, the glad it’s you and not me attitude. Hence, step away from the glass, the aisle, the entire aisle nine! It stinks:)
Thankfully we are supported by wonderful faithful friends who even before the proclamation was issued “officially” today have sent me pictures of food and doable recipes followed up with conversations answering questions for me like so what is a milligram? And how much is a 2 gram sodium diet? What exactly has fiber? We have a long way to go but we can do this!
And you know you’ve been there. Walking around. Hearing people talk about what they can and cannot eat. If you were me. You just listen but walk away. Now we are the ones who can’t walk away. So proud of Kevin. He may single handedly (I would say single liverly…) get it(?) may change many lives around him for the better just by eating better.
I use to say I never got that memo. How does everyone know how to eat what!? Well, we got the memo! I will paste it below:)
If you are reading this then you know me personally and we are open to recipes with high fiber and low sodium! You know how to reach me if you know something. Get in touch…I need help cleaning up aisle nine!
Here It Is:
Heard from Kevin’s dr today about his dietary expectations:
“Ms. Troutman
I hope this answer many of your questions going forwarded until you follow up in the office and thank you for your patience.
LOG NOTE
Date: 02/11/2015 01:52 PM
Patient: Troutman, Kevin DOB: 06/27/1997
Author: Galati, Joseph S
Sign Off Date: 02/11/2015 01:53 PM
Signed Off By: Galati, Joseph S
____________________________
For all of our patients with any sort of liver disease, especially those that may be taking immunosuppression, the basic guidelines should be followed:
1. We want all of our patients to maintain a low sodium diet, consuming no more than 2000 mg of sodium and her diet daily.
2. There needs to be the avoidance of process foods, including foods that come in a can, processed frozen foods, and all fast food.
3. Diet should consist of fresh fruits and vegetables, as well as fresh lean meat products
4. Dietary fiber should be consumed, and the target would be approximately 30 g of dietary fiber daily. Dietary fiber for the most part will come from fresh fruits and vegetables, as well as beans.”
February 6
Yeah…I called again. It’s killing me not to know. The MA was ill and out of the office. So, whew, life happens. She had a great talk with me. Mom to mom. She said this pretty much is his plan of care for liver patients. She was very friendly and caring. Completely understanding said we would hear from them next week.
January 29 afternoon
I did call and speak with a PA or NP who listened and answered some of my questions but said she would have Dr. Galati call. So we are still waiting for clarity on a few “underlined” observations.
January 29, 2015
This morning I am waiting to hear from someone at Texas Liver Specialists, Dr. Galati’s office. We walked out after seeing him yesterday and went straight to labs and even in the waiting room I typed the entry below and Kevin read over it. We get in from church and somewhere along the way there is an email from Dr. Galati in the patient portal that “recaps” the visit. I literally underlined everything that was new information to me in the email. I will be honest and say I am actually hoping they call and say that it was a bad cut and paste! I know they accidentally gave us the wrong standing orders as we left to go to the Smith tower for labs. So it could happen. I’m borderline horrified. But not. Like that makes any sense!
Jan 28, 2015
Dr. Galati
Based on the set of labs he ordered in Dec he said it was flagrant AIH. (Autoimmune Hepatitis) Flagrant markers.
The pathology department looked at the biopsies from 11 and 14. The 11 hinted at PBC or PSC and even now the numbers are hinting at something. He wants him to get labs today. Get labs every month then see him in May. He wants to get to know him that way. He cautioned Kevin on the Azathioprine sided effects such as lowered immune system so not to be a hypochondriac but definitely call quicker when he isn’t feeling well. Also be aware of pancreatitis. Just be aware. Long term side effect is liver cancer. He had a great conversation about how normal kids are worried about school and he has to worry about liver cancer. He said it was tough but all that to tell Kevin to live clean. No alcohol. No drugs.
He mentioned he is at grade 3 fibrosis. 0 is none then it stops at 4 with cirrhosis. (So he is one class away scar tissue wise from cirrhosis)
So by suppressing the inflammation caused by the immune system it is helping keep the scarring to minimum. (?)
He wants him to keep taking Azathioprine. Stay off steroids for now since he wants to get to know him. He mentioned about Ursodiol that he could take it as long as we could afford it. So we will keep up with that one until he says otherwise.
He chatted a bit about Kevin being responsible for taking meds. Keeping up with them. I could text once he is away with some reminders and refill help but he said for me like not to ask him to send videos of him taking his meds. He looked at Kev and said but to stop taking Azathioprine will send you to “hell in a handbag!” I did ask if he could ever outgrow this. Kevin said he said basically – no, it’s not very likely.
On a side note he did say that the Texas Children’s Pathologist is world renowned and I think I was picking up on how impressed he was with the pathologist “eye.” His pathologist agreed with the TCH pathologist so that is nice. He described them by saying when you look at the sky and say what color is it some will say blue while others may say blue gray…they both saw hints of PBC and or PSC.
The walk away is he doesn’t have to be labeled either way now. Whew! Yes something is happening but he is being watched. Kevin is feeling great. We will stay on top of this.
I know you can’t ask for more from a 17 year old boy who desires to serve the Lord with all his life than to live clean. We got this!
We were in an exam room that was covered in New York Yankees memorabilia. I was sitting in old stadium seats. Kevin took pictures of everything.
Again he said he would keep Dr. Olive and Dr. Walsh in the loop. Love that!
January 27, 2015
He Didn’t Even Pull Up The Covers!
We saw Dr. Walsh. She had a baby boy and named him Liam! She said she was so appreciative of the time off. He is 4 months old. She started after that by saying let me tell you what I know. Kevin, most of my patients stayed calm when I tuned in but you exploded! We all agreed. Remember her words before leaving were I want you all tucked in. So I said exactly…and he didn’t even pull the covers up! That would exactly describe his life since mid summer. He exploded. She said she received a letter from Dr. Galati so that eliminated the awkward but not awkward part of saying we are moving on. She was wonderful and discussed so much with us. She happened to mention in passing that she remembers Kevin because he was one of her first in-room assessments. Cute. (We have been with her as her name changed and now her family grew) She was realistic. She told Kevin he didn’t need 6 doctors but didn’t want to see him go but understood and gave us her email. She wants his senior picture…she said keep up. It was weird walking out of there. It was familiar.
January 22, 2015
Love Lexa!!
Wow! After thinking Monday that no one had Kevin on their mind Lexa called today with the best news. She said she was driving into the office this morning and it dawned on her that she still hadn’t received any slides from Texas Children’s. So she called again. She ended up asking for the manager and finally told them she was walking over to get the slides! She called to give me peace of mind!!! Neither of us have any idea why it took this long. I have no idea why they would want such incompetent employees! She said she has never had this much trouble ever getting slides. But she has them in her hands and is walking them to be viewed herself!
I am so absolutely relieved! Praising Him for following close behind and picking up the all the pieces! So so happy!
January 20, 2015
One More Phone Call
That is what came out when the office manager called and apologized and mentioned to me in all honestly that what I dealt with they are faced with every day. She said it is unbelievable what ‘one more phone call’ they have to keep making. She said they were out of the office Friday for training and much to their surprise the slides were still not received. She has documented how many calls they had over to TCH just for this request. She said she was speaking to me as an office manager, and mother, and a patient. She stated that Dr. Galati is the best and that she promised she would get Kevin, me, and Keith through this.
It is unfortunate and it hurts because I know really they need grace, mercy, forgiveness, for this perplexing mistake. Whoever is at fault. But it is hard to do when it’s Kevin I am fighting for. I love anything cancelled when it’s me! And when I spoke with Kevin he was like well…ok. And played basketball all day on his day off from school! I said Kevin, you totally need to answer these calls. Lexa would have loved receiving that response instead of maniac mama!
I inquired to Dee, the office manager, about several topics during our conversation over the phone:
~Why the appointment needed to be cancelled when they said there was no new information yet they dropped in our patient portal Kevin’s lab results within the hour after being cancelled that were taken 12/18/14 and sent to them 12/22/14. That out of all the numbers my eyes go straight to that GGT and it was at 158 from 124 from 110 (in the best order I could remember not having Keith’s spread sheet in front of me.) We need to know do we add the steroid back? He was taken off steroids so the scopes would not be masked. This was NEW information.
~What should I do about the TCH follow up with Dr. Walsh. We had hoped to have this opinion. She felt I should reschedule it.
~What to do about them saying I could NOT have access to his slides that they had to request them. I have a good friend who texted me saying she would do a fundraiser for me to bail me out of jail because she knows this mama’s heart and great day those slides will be delivered before our rescheduled appointment on Jan 28!:)
She said I do have every right to get them. It has been TCH who when I call pathology medical records “whoever” answers that phone tells me I have to have the doctor request them. Who knew!? Who ever knows!!!?? I did not have to. I could have requested the slides. *infuriated face*
~She said she would have someone call me about that GGT number but before she did she mentioned something about since it is his first labs…I stopped her. I said he has been having labs since August 2011. I am holding the copy of the medical release request that I sent TCH to have all records sent to Dr. Galati from TCH. She had some from Tomball hospital. (Hip hip Horray for them! Love Tomball!) but no others. So I gathered my thoughts. Said there was no need for anyone to call about the number because they have no history to see. And we will see Dr. Galati Jan 28. Next Wednesday. She instructed me to once again phone TCH. Send them a request with only labs checked. And interestingly enough when I did and I spoke to Stacey at TCH medical records she said the exact same thing. I gave her the brief history. The original request was October 22. She was super nice and informative. She offered great information. She said since my request said all records from Aug 2011 to present that that was too much for a fax. Here’s the kicker part: “so they chose to send what they thought was pertinent.” (!) *undeniably in disbelief face*
*crazy mad face*
I replied with well, my phone number is on the request and I didn’t receive a phone call telling me to please make separate and smaller request for records. I know I’m not in the medical field but if this is what people deal with every day we do need to send people to junior college for free for two years! Oh how America is declining in my eyes if this is an original thought to just me!
*hot face* She said to please make it attention Stacey and she would get it over to them today.
In my conversation with the office manager she let me know nicely who she was so I let her know who we were. I said we are the people who blog everything about Kevin, and put numbers and medications and procedures with dates in spreadsheets. When we get a phone call or test results we want to keep up with that information and although we may not know what to do with it we sure do want to know it. We know he is not critically ill but is chronically ill. She ended the call telling me that my faith would get me through this. That is true. And somehow even though I felt I was turned completely inside out with appall, somehow sprinkled in there was enough reference in my conversation that she knew she was speaking to a woman of faith. *bright face*
I am spent. I am determined. I am calling both offices now to simply follow up. That I have learned. I thought I followed up before. But today…I will follow up.
[Follow Up Call TCH Stacey Medical Records:
••• She remembered me. She sent 3 separate faxes to Dr. Galati’s office. 30 pages. She happened to state that she went as far back as November 2011. I said we really need all the way to August 2011. I said that is when he went from Tomball hospital in an ambulance to yall. Any labs done August to November are crucial. That is when the diagnosis was being made. Dr. Galati’s office needs those. She was very nice. Informative and was going to send those now. One follow up down:) And glad I did at that mind you…]
January 19, 2015
Shaking
Since Dec. 9th when I felt like an epic failure because the doctor looked me in the eye and said I need those slides, I have been waiting for today’s appointment. You can bet I called for the slides the very next morning. Know what? I’m not allowed to order them. The hospital said the doctor had to make that call. Well, that’s easy enough! So I just called the doctor’s office back who we just left not even 24 hours before and spoke to a different area of the office and they agreed. They said they would handle it.
Today is the 19th. Today is the follow up visit. I was emailed to confirm the appointment. I was Robo called to confirm the appointment. Yet this morning was awakened by Lexa telling me since they haven’t received Kevin’s slides they aren’t going to have anything new to discuss at today’s appointment. So she cancelled the appointment.
Uncontrollable shaking consumes me. With tears and barely a voice to be understood I asked about his labs. That is new information I am waiting for. I’ve checked the patient portal and nothing. She said they wait on those at the follow up. (Give me the GGT numbers or give me death lady!! That’s what I’m desperate to know!)
When you feel like for the second time in a row from Houston’s best medical centers your child fell through the cracks it’s what happens to you or at least to me.
Still shaking.
I said. I will go get the slides. I offered it 6 weeks ago. She replied I couldn’t. She kept repeating let me call TCH and see what went wrong. I asked her again through tears why this couldn’t have happened earlier. Why after December 10 when I called the day after his December 9th appointment and heard we will get the slides how I’m suppose to believe that now. I begged her. I said I will leave my house right now if you just give me the exact location in TCH where the slides are. She said they wouldn’t release them to me. I said what if I bring a lawyer!? She said they wouldn’t. I said what if I bring police. She again said no. (Which is good because I know both of these professionals but did I really want to make that call! If there’s an lol it would go here. If. Not feeling the lol)
She said she needed to call over to TCH and would call back. I did ask about how long until I could expect a return call and she said in less than 15 minutes. And it was. However, it takes 48-72 hours to receive the slides. So his appointment had to be moved to next week. January 28 at 1:00.
Shaking and crying I had to ask who was there when we left that office on December 9th walking around with a thought of Kevin or with Kevin on their heart? I asked from a mom’s perspective to be able to understand this just how does the office work? I am truly perplexed. Curious. Defeated even. I explained on how many levels this is disappointing. I am pretty sure she understood my disappointment. Kevin didn’t have to miss school today for this appointment because we are out today. Last semester we got “the letter” from the school district reminding us of that very thing. A Very Threatening kind of letter. “Stress the momma who can’t do anything but get a doctor’s note to try to clear some of them kind of letter.” I said we were to see his TCH doctor on the 27th and I wanted to be able to tell her what the expert decided. We fell through the cracks because she had something beautiful happen in her life: she had a baby. I cried to Lexa what do I do about that appointment? We will see her and have no new information. Should I cancel it? Let’s see. We fell through the crack with Dr. Walsh so we hopped across the street to Dr. Galati to slip through another. Kevin leaves for college this summer. It can’t keep taking this long between appointments. I know I’m a basket case. It’s how I handle disappointment on this scale when I know I have a chronically ill child who is close to an expert who has a specific treatment plan and a diagnosis and who in my opinion had plenty of time to get the slides to tell us this information at 2:00 today! The only question this mama’s heart needs answered is did they care enough? That is why I’m so upset. I feel as though they did not. I feel as though I am the only one who could and every place I turned my hands were tied. We were in Louisiana over the weekend saying goodbye to baby Reed, my niece’s 7 month old baby, and we didn’t have to rush back. Why didn’t the automated call tell me all this!? I pressed the right buttons?! Didn’t I!? I asked her where in the office was Kevin’s file? Like where do they put the cases that need follow up? I said I sure wouldn’t have waited until the day of the appointment to check and see?? Sobbing and shaking….and
yes, she apologized for dropping things (or something like that. I heard the word dropped) but said she would have the office manager call me later to explain things. Even in my shaking I am looking to Him. I know He knows me. He created me. I know He is my constant. He never changes. And I do take comfort in that. With deep deep breaths I will settle down. We expected new news today. We wanted answers.
My heart is broken…
December 9, 2014
One Of Those Dates
I have been waiting for this appointment all fall! We saw Dr. Galati of Liver Specialists Of Texas. He made a great first impression with us just with the pictures and letters hanging on his wall. He had a letter to Bush (41) and a signed photo of astronaut Alan Shepherd…golfer Arnold Palmer…in other words we weren’t in Kansas anymore Toto! (Children’s waiting and exam rooms covered with Toy Story and dinosaurs! Don’t even get me telling about what was on TV in the waiting room!)
He walked in and packed a punch. He examined (Kevin said he even examined him differently…he poked and didn’t just press) and asked questions engaging all of us in the conversation. Especially wanted to hear Kevin. He had an assistant type everything that was being said. He saw that I was taking notes and after hearing all of Kevin’s past three years of medical history he gave me this word to write down: Autoimmune cholangiopathy. You could tell he just had such a working knowledge on the treatments and diagnosis of everything Kevin has or is expected to have.
He wants to actually see the slides from Kevin’s two liver biopsies in the past three years. He ordered labs to be done in the next week or two. He asked a lot of questions. Explained the alphabet we are now familiar with:) AIH PSC PBC … And added the AC autoimmune cholangiopathy. We didn’t walk away with “so this is what he has” yet. But I love that he questioned the PBC liver biopsy result as Dr. Olive did. I told him it took Dr. Olive days and talks to the pathologist at TCH before he would tell us that news. So he’s not affirming any previous diagnosis yet. His daughter goes to school with Dr. Olive’s daughter so he said he would have a talk with him.
Had I written this last night it would have been with a much more “plummeting tone!” Because when he looked at me and said get me those slides, I was horrified because in my knowledge of medical records request I thought I had! I even called last week to make sure they had received the “medical records!” So I was frustrated within. I had unrealistic expectations about the visit. I just hoped it would all be solved! To quote Caleigh in another matter: a girl can hope can’t she?!
So this morning I jumped through all the hoops to get those slides to him. We see him again January 19 which is a school holiday so no missed school for Kevin! The actual slides were never a part of the initial request I thought I had made. They said he never asks for those for the first visit. Who knew?
He asked so many questions that we didn’t know the answers to that I felt like man…I was just not prepared for this visit! I have pages and pages of information on here. But can’t remember if his mitochondrial antibody (?) is positive??? Or if the surface of Kevin’s liver is scarred?? I vaguely remember hearing this information in the past and know it has been checked and looked at but couldn’t answer. None of us could…
I am the literal queen…so I take in information differently. Keith and Kevin were fine last night on the drive back home. I was just silent. Probably perplexed and plummeted and hungry and tired. Even earlier in the day when I tried to pick up Kevin’s refill for the meds he takes everyday the pharmacy said there is a shortage on it. They gave us a dozen. That is 4 days for Kevin. I drove away wiping tears because who is ready to hear that! Even the doctor didn’t know why but reassured us there are other meds available. Our pharmacy called while we were in the waiting room saying they found some and had a tech drive over to get it for us and it would be ready for pick up soon! They said the shortage should be over by the time of his next refill.
So, everything is better today. It will all get figured out. A good friend reminded me of just that in a text yesterday: “God knows what’s going on.”
November 21, 2014
Thankful for Normal!
We heard from Kevin’s doctor tonight. The results of his biopsies from the scopes earlier this week are normal too! Thankful for normal! We can do normal! He even released the pathology results so we would have them to take to the specialist on Dec 9.
Very Thankful mama here giving thanks with a grateful heart to the Holy one…(praise song lyrics filling my heart)
November 19, 2014
We Picked Up the Glasses

“He filled the room with upper cuts!”
November 18, 2014
We arrived really early for his procedures. He ended up going back around 9:30 and the doctor was out speaking to me in an hour and a half. He said everything looked normal and that he would call with the biopsy results in a few days. The nurse filled me in on the actual details during the procedure. Apparently Kevin filled that room up with upper cuts! He was trying to punch his anathesiologist! So shocking. I’d pay to see it!
November 17, 2014
Prep day wasn’t as fun as Kevin thought it would be! Down right no good! He did great drinking the prep or as Christopher calls it “juice poop” mixture!
November 16, 2014
I asked friends and family to send notes for Kevin’s prep day and me and Caleigh towered up toilet paper rolls outside of his door with the sticky notes of prep day encouragement on it!

November 14, 2014
Monday the 17th is “prep” day for him and Tuesday the 18th is scopes. Both kinds:0
He thinks it’s funny and great that a camera is going into “those” places! I try to ask if he’s ok or has any stress about it and he just giggles and says he GETS to poop all day!!!
It’s also Christopher’s birthday so I will have to get him over to give Kevin “juice poop day” advice and help in building a tower out of toilet paper rolls!
He’s feeling great. Keeping busy what’s new?! We have sent all the medical records to the liver specialist for his appointment on Dec 9. I’m reminded over and over that we are so blessed to be on this side of early detection.
Definitely asking for more prayers for him next week that those doctors will see what they need to in the scopes:) or see nothing at all:)
November 10, 2014
He is the Little Engine that Could!
Ok…recently we hopped back into Dr. Pope’s for Kevin to be seen mostly because of headaches. In the questions before they asked how long has he been having them or how many days or something like that. I know my response was well. It’s more like when does he not have one!
The nurse checked his vision and he came back afterwards and she said it was fine! Kevin whispered that it was blurry but he memorized the line from the first time she asked it. I said Kevin! Who does that! Who has room for that kind of detail! He said he just couldn’t help it! Anyway, I knew the official vision test would be today by his eye doctor. So we got the Big 8 listed on paper what causes and what types of headaches there are and he pretty much ruled out everything but stress and migraines.
So today when the eye doctor called me back to explain Kevin’s vision I was told from a year and a half ago when he was last seen he went from normal not really needing them to today having a double astigmatism which and I quote Dr. Norcini is “the number one cause of ocular headaches today.” He put it like this. People who really cannot see and aren’t in glasses yet walk into his office and say: I can’t see a thing. I need some help here. (Basically. Huge paraphrase) These people aren’t experiencing headaches because they don’t even try. They know they can’t. On the other hand. People like Kevin are 20/25 and 20/30 they can make it work. He said he’s like the little engine that could. He’s gonna keep going until he gets it done but afterward pay the price. Isn’t that good to know!? I mean I know migraines will still most likely be around but for being a senior with early release and one class as an office aid this kid still has been carrying a load of course work with his AP class and dual credit classes and usually every paper and project seem to be due on the same day. He has been cranking out the papers! And reading, reading, reading.
I have never been so happy to hear that there is something wrong with his vision! Umm…I will admit I might have been as happy after his third grade teacher called us in for a conference and she described Kevin after she said to start writing and he would look anywhere but his paper. She said she’d get his eyes tested above anything else. I thought maybe a spanking on the way:) I was like that is complete disobedience! Complete. Ended up he had convergence insufficiency. Otherwise known as double vision. No wonder he looked up when asked to look down and write. Those words were popping off the page he just wanted to see where they were! He wore prism type glasses for correction when doing seat work and such but over time his eyes strengthened. So to be able to tell his teacher that he really wasn’t disobeying and just needed glasses did make me happy!
I love that he described it as the little engine that could. If there is an engine that can it’s Kevin. Never seen a more determined, involved kid! He loves to say: the deed is done…well think how many deeds will be done without pain!
October 22, 2014
Wednesday
Where To Begin…(I started this Oct 22 and for the record it’s Nov 4!)
Ok…how about where I left off! (Only a month ago!) I do much better if I get to the update immediately. So much has happened that I hope I can get the details down.
Not long after Dr. Olive called did we begin having questions. So many it prompted a call into their office. That prompted a visit to see him on Oct 2.
That made me happy. (Because we went from seeing her before she had her baby with her wanting to check his labs. If they weren’t where they needed to be she said she’d want an MRI. If that didn’t look like she wanted it to look she would order a biopsy. We heard from her up until the new diagnosis after the biopsy. So after “the phone call” from Dr. Olive that he spoke with the pathologist we truly walked around with a lot on our minds. And on his end. He delivered the results and answered questions but then hung up. It’s the stuff that goes through your brain for days after the hang up. So, I picked up the phone to ask anyone that answered on the 11th floor at TCH what I had questions about. I truly received an Olaf on the other end. Warm hugs and all. They understood my questions enough to recommend us squeezing in a visit to see him. One side of me said it wasn’t necessary. While the other said get in there yesterday! I hate to take time away from sicker kids. But at the same time I wanted someone to look Kevin in the eye. Examine him. Poke and press his liver. Just an all around meet and greet and then some!
Here is my recap of that time in his office:
At the October 2 visit we went in with a list of questions. He weighed 202 and is 5’10”
-where is our best source for information on this overlapping syndrome PBC. How many can overlap? Is remission a possibility? Is this lifetime/chronic?
*He printed a sheet right there with the details of PBC and explained that this is partly due to his AIH in that it is an inflammation and the inflammation is spreading around the bile ducts…
[i need to scan that in plus Keith created a spreadsheet of just numbers and meds and tests ordered that I should see if it can be inserted. I blog. He creates excel spreadsheets. #ofcourse]
-I asked since she said the images of his bile ducts were beaded could they ever get unbeaded?
*He said yes. The liver heals itself.”
-he wants him to start Budesonide the low dose steroid that brought down the GGT previously. Then in 4 weeks get labs done. Start the steroid at 9mg for two weeks then taper to 6 mg then finally to 3 mg.
{actual Budesonide dates:
Sept. 24 started 9 mg
Oct. 8 went to 6 mg
Oct. 17 heard from Dr. Olive-after Kevin’s 4 week from starting steroid labs his GGT was only down to 122 from 124 and with a scope upcoming he didn’t want steroid use to mask anything they were looking for not to mention he has had severe migraines we think from a side effect of the steroid- so he said to taper to 3 mg then after 5 days stop. So as of Oct. 21 he took the last steroid. Currently his scopes are scheduled for Nov 18. Exactly 4 weeks from stopping. They have been now scheduled three different times. The first we changed due to band schedule. The second was rescheduled due to steroid use. Now the third I call tentative because I called and wanted to be sure since Dr. Olive pointed it out to begin with, that 4 weeks is enough to get the drug out of his system. So far they said it is.}
-We asked about the flu shot he gave Kevin his and I asked if Caleigh could get the mist. He thought about it. Said no. Then once he left the exam later he popped his head back in and said he looked it up and definitely do not let her get the flu mist since it is a live vaccination and Kevin cannot live “in house” with that.
-We said he has been having migraines and has noticed some blood only in his loose stools.
*Continue with the Sumatriptan and he was concerned about the blood in the stool so he asked if Kevin had ever been scoped. We said no. He wants to do scopes. We set the date for that based on Kevin’s crazy band schedule for October 29. *actual date 11/18 at 8:00 am. Arrive at 6:45 am. *they gave us lots of papers I haven’t read yet because they aren’t due! (Blood in a loose BM with his digestive and immune stuff sends flags for all things autoimmune. Irritial Bowel. Ulcerative Colitis. And sometime blood makes the d/loose BM happen. So it’s to peek inside. Not expecting anything. But highly recommended. So better now than when he is miles away.)
-I asked what age does Texas Children’s stop seeing patients.
*He replied for someone like Kevin it would be fine to go through college.”
-I asked do any of the doctors in this clinic have a practice outside of this hospital?
*He said no. They are all affiliated with Texas Children’s even though some may have offices off site.”
-I asked did he know of anyone who we would transfer to.
He mentioned Dr. Galati.
(This part is where I know the Lord is stepping us. As we look to Him he makes our path clear. I had already put these six letters in Google: AIH PBC and Dr. Galati’a name and practice showed up! Then a friend asked me questions and gave her testimony as to how her family handles health matters. She got his name.) *we now have even a fourth confirmation of Dr. Galati’s practice being recommended to us!
We had a very good visit with Dr. Olive. He was very thorough. I wanted him to mostly lay eyeballs and hands on Kevin since he took over our doctor’s cases while she is on maternity leave. Cannot even begin to tell you how much that 40 plus minute visit and talk with him helped me.
The nurse came in to schedule his scopes and give us labs. She gave us paper work and told me these are the labs that need to be done in 4 weeks:
1. Cholesterol
2. Mitochondrial
3. IGG
4. Smooth Muscle or Actin
5. Carbohydrate Antigen
CA-19-9 Cancer screenings
6. CEA
7. GGT
8. Liver Panel
9.CBC
10. Immunoglobulin
October 15, 2014
We went to lab corp to get the labs done. They drew 4 viles full. Kevin said he never even felt the needle go in. Either she was really good or he is very use to this. It’s a good thing they gave me the list and papers. Once again at first she looked and saw only two orders. So the lesson we learned months ago is still paying off! Ask what they are seeing. Tell them if it’s different. It worked! I pulled out my chicken scratched list of initials and tests I had no idea of most of them but counted at least 10. And it took some time but she found the orders. All of them.
10/16/14
Kevin wasn’t feeling well again. He had missed most of the entire week. We had seen Dr. Pope right after the biopsy and Kevin was coughing but normal and viral or allergy ridden. So we went in to see Dr. Pope again. Since all the labs were just there from the day before’s lab draw or at least most of them he told us some of them by trying to rule out what was wrong with Kevin. He explained many of the labs but some were still not available. He joked and said other than that elevated GGT number, Kevin really looks good on paper!
{numbers from him that is in even worse chicken scratch as I tried to write while Dr. Pope spoke:
GGT: 122
Hepatic panel (ALT & AST) he said looked good
Bilirubin: 0.6
Alkaline Phosphate: 161
CBC: normal 5.4 white
Hemoglobin: fine
LDL: 79
HDL: 54
Total Cholesterol: 144
*we didn’t know to fast so Kevin had a bowl of cereal before labs and Dr. Pope said that was fine.
Gamma globulin: ? He was honest. Said he didn’t know how to read it so he never orders it:)
IGA: 167
IGM: 101 normal
CEA: 3.2 normal
Carbo Antigen: 11 (0-35 is the range)
*like I said. I wrote what I thought I heard:)
–He gave us a script for nausea medicine that should help the nausea that accompanies the migraines called Zofran or odansetron.
When we walked into Dr. Pope’s they always weigh. He weighed 197. For whatever reason after the nurse left us alone in the room I couldn’t stop the tears. I know he needs to be losing weight but it just concerned me. We can work out with a trainer all summer and drop 5 all summer and he goes two weeks and drops 5. So he’s down 15 from his highest. I dried it up. Poor Kevin. Then after Dr. Pope said the GGT was 122 I remembered it was 124 pre MRI and along with taking a steroid and piled up missing days of school I was a bit emotional. Overwhelmed. As hard as I tried not to be. The harder I tried the more I cried. Needless to say: I walked out of there wiping tears and trying to look like I wasn’t. For Kevin’s sake. But Kevin loves me. He knows I cry over stuff. Yep. He would use just that word. Stuff. And we had a lot of stuff to contemplate.
Oct. 17 Dr. Olive called with the lab results and technically we heard some of them from Dr. Pope but definitely wanted to hear Dr. Olive’s take on them. I was keeping a friends kids and let me tell you. I forgot how quickly things go crazy once you have to take a phone call! I had to get in the office and close the door to hear. They could feel the seclusion! So even though I grabbed a notebook and started writing what I thought he said I am ify on these details.
–The GGT number wasn’t that much lower. He was open to letting him stay on the steroid a bit longer. But he also said since he’s had migraines and he wants to do the scopes that he might as well taper off the medication. He said something about the GGT could wax and wain? I wrote that the “auto antibody” was elevated and is elevated in 90% of PBC patients. He added as well that Kevin’s liver is stable. Love that!
He threw out “medical study” and the drug cellcept or anthro something(!) truly should have done this update sooner. He said he didn’t take that lightly. Said he is willing to give Budesonide more time. But wants to scope but to push them back to be steroid free.
I finally asked what I knew I wanted to ask about getting a second opinion. How do you ask this. I didn’t want to imply anything. We have had nothing but the best care at Texas Children’s but Dr. Galati’s name has been brought to our attention I feel in a most divine leading. So I asked him as we were winding down the conversation what he thought about getting a second opinion. I explained that we don’t doubt this diagnosis. We just know that what he said: Kevin has a rare thing going on. So rare they don’t see it at TCH. He said he would do the exact same thing! He said he was going to even talk to Dr. Galati himself about Kevin as a colleague of his. Can you say “peace that passes all understanding!?!” I can’t even type this without happy relief tears. It’s just so good to look to Him and know He is guiding us with His eyes and instructing us in the way we should go. Relief. Peace. New plan.
The very next day I was calling Dr. Galati’s office. I creeped their website enough between office hours I pretty much answered all my questions on how to go about getting this second opinion. But it was great to get it started. We have requested Kevin’s medical records…everything that has been done to him in the past three years to be sent to their practice. They called us back with a first available appointment on Dec 9. With his scopes on Nov 18 and Thanksgiving thrown in there that date will work out just perfectly.
***Ruth…there you go! I know you will be calling. And I’m sorry in advance for texting you that I am working on the update over and over, but I appreciate every click and refresh until I did. (Not that I know that’s what you did–it’s sure what I would have done!) You made me start this blog after all! It’s been just the perfect place to tuck the notes and chicken scratch away. I don’t know how people do it that don’t write things down!**
It’s Just So Good To Know
September 23, 2014
Dr. Olive said he would call. He also said he couldn’t promise what time. But close to 6 this evening he called after speaking to the pathologist who studied Kevin’s liver biopsy with this information:
•it does looks like PBC
(Primary biliary cirrhosis)
•he admitted he didn’t have a lot of experience in this or in treating it because he just doesn’t see it often enough.
•2 autoimmune processes are going on in his liver. Autoimmune Hepatitis and PBC
(Repeat: inflammation of the liver and inflammation of the bile ducts)
•he wants him to start Budesonide again. He was on this low dose steroid medication from December to March last year and noticed it effectively lowered his GGT number then, so he thinks it’s reasonable to start this again. (I asked if he knew what that number was going into the biopsy, and he gave me the August 26 number from the labs before the procedure and it was 102.)
•he wants him to repeat labs in 4 weeks.
He explained that it is an inflammation of the bile ducts which is PBC and not hardening of the bile ducts or PSC. Last week Mam Maw asked me if either one was worse than the other or which one did I want it to be:) I said neither, actually! But this relief came over me tonight after hearing his explanation. I don’t know why. Still, neither one is optimal…but I think of something inflamed as irritated and swollen, while hardened is well hardened! His body’s immune system needs to settle down and stop turning on him! I also haven’t clicked on too much stuff so my knowledge here is just what pops out of my own head and thoughts. I know he said it’s rare. It’s rare for him and his age. I did mention to him that Kevin looks great. Feels great. Acts great. That was his chance to say well maybe we have it all wrong. But he said instead that is exactly how a liver behaves. And that it is good that we know and can have that watchful eye on him.
Oh, he’s being watched alright! I remember well being taught this verse by our Pastor years ago:
“I will instruct thee and teach thee in the way which thou shalt go: I will guide thee with mine eye. (Psalms 32:8 KJV)” He gave a great illustration then about how much we can communicate with just our eyes and that made me then think of Big Daddy and all the instruction he could give with just a nod of his head. Our Lord wants us to look to Him. As we look His eyes guide us without ever really needing to hear a single word. He is watching us. I’m so thankful to know! Isn’t it just so good to know!
September 18, 2014
Call Me Diane…
Biopsy results expected. But none given…
I waited. Called. They weren’t available. I was upset.
(My attempt to be less wordy.)
Now for the cathartic words:
The doctor taking care of Dr. Walsh’s patients is Dr. Olive. The attendant who called me back said that he hasn’t looked at the results. Not the nurse. Not the doctor. The attendant just said the radiologist was out of town. I do not doubt this information but kind of thought that in the entire Texas Children’s hospital building and interventional radiology department there had to be someone who could read the results by now. The real problem was with me. I am as literal as the day is long. They said the results would be in 3-5 days. I was fine with that. Especially after seeing how crowded that biopsy room last week was. I felt like they were running kids through there like the double line wrapped around chick-fil-a drive-thru at lunch time. It’s mind boggling and completely disheartening to see so many kids in the hospital.
I even didn’t call until today. This morning. And not counting the weekend I actually thought I was patient giving them two more days, but honestly I felt like if I hadn’t of made the call when would “they” call? I know as Kevin would say nothing is pressing in the matter…only me. I’m pressed and stressed! And I’m a sympathizer, Dr Walsh had her baby! So happy for her but feel like if she were in the office we would have been contacted.
How does the system work? I’m just so curious. How do they keep up with all those kids? When Big Daddy was in MD Anderson I remember well them telling us that you are the best advocate for your family member. Do they know the trouble and torment we put ourselves through waiting? I’m a mind game maniac!
So I wait. Try to tell myself I’m not waiting but none the less it’s waiting. The furniture in the house is getting rearranged. And then I have to stop waiting and pretending not to wait and get on with my day. Today it just so happened that was grab Caleigh from school early to go get her cast off! No cell phones are allowed in the office where we sign them out. Of course the office manager from TCH calls me at that moment. Of course. I’m a rule follower too so it killed me to answer the phone in a no call zone. I had to. Then I’m like great, I’m now one of those people.
So now I’ve gotten an attendant and an office manager. I have the person who answers the phone and the person who is over the person who answers the phone and all I want is to speak to Dr. Walsh’s nurse or the doctor taking her patients while she is out. And both of these ladies told me it wouldn’t do any good because they don’t have the results. We actually had other questions for the nurse or doctor but once I heard it would be next Tuesday before the pathologist got back in town, well, I just couldn’t speak. I cracked. Why do we have to crack! I know we fell through the cracks! I told the office manager just that. I told her I realize Kevin’s doctor had her baby but I also know that at our last visit she wanted (and used these words) all her patients “tucked in” before going on maternity leave. We are not tucked in! And you could bet when we see her in January or February I would be telling her what has happened. She said she would speak to the doctor again between clinic visits and ask him to call me. She said to let her know if I hadn’t heard from him by morning.
Meanwhile, I am missing Keith. He’s out of town and the last few days had no phone or iPad charger because he left the charger with his laptop at the office while they did an off sight. Well, the home phone rang and I saw the number was a weird one so I answered thinking it would be the doctor. Instead I hear Keith’s voice and he calls me Diane! I’m like Keith? And he says something like he must have dialed the home number; He was trying to reach the office. So I say: well, let me hang up then so you can call Diane! I hung up. I wish I could insert a poll here to see just which way you would have taken that:) So I’m walking around thinking he is going to call me back. He never did. Not until after all the drama of my day and tears were settled. He calls and when he can tell I’m upset he actually can’t imagine why. So I might as well tell you. He hung up on me. And I was actually fine with that. I knew I needed to go unplug. I knew it was ridiculous! You know I was walking around with the woe is me attitude. Don’t hear from him in my darkest hour for days and then I hear from him…he can’t find a way to call me and yet finds a way to call Diane!? Oh, you know this just isn’t good. I knew we’d be laughing at it soon. Already are. But good grief the timing!
So we are in the cast office. I’m once again in an area where no cells signs are posted. And the doctor calls. We were close to being done. Just waiting on the school note, but I HAD to take that call. I felt so bad but I turned into one of those people. People. We need to not call those people those people. I have such a different outlook on this!
He explained the entire situation but better. He said the right things. He said yes the liver specialist pathologists (whatever their label is) are all out. He explained that he has questions about the notes from the pathologist that looked at Kevin’s biopsy and went into pretty specific details about them. He will call me next week after he has asked his questions. But he said I could walk away with knowing that he saw no new scarring or changes in the liver compared to the 2011 biopsy; his liver is working fine, functioning as it should; he feels there is no huge urgency for treatment; he wants us to take our time to make the right diagnosis. Autoimmune hepatitis and one of these two: PSC or PBC can coexist with his autoimmune disorder. And that’s where he got detailed. I was listening and understood but will wait on the specifics. I like what Kevin’s first nurse said before the biopsy last week when she accessed him. Her comment was something like basically you are a healthy young man! Praise the Lord!!
Now that was news worth fighting for! At the end of the day I think he would have never stopped and looked at Kevin at least not today. I brought it to his attention. I told Tiffany earlier I am even sick of hearing myself! But yet I look at Kevin and all he went through last week and find that strength and determination. Dr. Olive’s days are just like mine. There is so much to do that really you only can do what is due.
Made The Call
September 18, 2014
They said 3-5 days so I waited and even gave them a couple of more for good measure. Forget it. We are slammed here with Caleigh and the transition to middle school. Keith says we will make it. I say nay nay.
So at least I made the call to get the results of the biopsy he had last Tuesday. His doctor is on her maternity leave! So that is super exciting! The nurse said Dr. Olive’ (Oh•live•ay) is in the clinic today and will call me either between appointments or later this afternoon.
Waiting Still
Monday September 15, 2014
Even though tomorrow it’s a week there isn’t any news yet. We are in the “to” day. 3 “to” 5 days!
Recovery
September 10, 2014
Just a quick update. Kevin was in a lot of pain when he awakened from the biopsy yesterday. Especially his right side and shoulder. He said it felt like he just pitched an entire game! The pain subdued before leaving the hospital, but after 7 or so last night he had some unusual and unexpected bleeding at the site. We will keep him home today to keep an eye on things. Also he looked concerned and I just think he needs the rest.
He did grab some leaf samples for his 6 weeks project! That wasn’t on my radar but was good to see him out of the anesthesia fog:)
He has a note for no physical activity and is getting use to deep breathing so he said he has a “plan” for marching band this week:)
The results will not be available for 3-5 days at least so we will once again pray while we wait…
This morning I was trying to quickly get Caleigh to school early to finish her math test (pray for her transition to junior high) and fitting the French horn, back pack, lunch kit in my Mini Cooper I spilled an entire cup of coffee on (and it was a good tasting one!) her back pack and my precious mini! I did it. I quick dabbed it up with one of our many beach towels and on the way to school she said: my back pack smells like coffee. I will think of you all day:) That’s a good thing she was smiling when she said it because, people, around here I have been losing my marbles. {another blog post here entirely!}
May He be able to say the same of us…He is loving and smiling because of the sweet smells we offer Him in our time with Him each day in prayer.
Liver Biopsy
September 9, 2014
Kevin has his liver biopsy this morning at 10. We are praying for wisdom and guidance for the doctors and staff during the entire procedure. Also that He would show them through the results exactly what they need to see. We ask for complete healing if it is His will for Kevin’s liver and those pesky bile ducts! We know either way Kevin will glorify the Lord with his life.
It is a Tuesday people! He isn’t missing marching band practice…just an entire day of school….
Back to School News
August 25, 2014
We heard from Dr. Walsh for Kevin’s MRI results. He has to have a liver biopsy. They are calling to schedule it. She said the text book term for what his bile ducts look like is “beaded.” (Beads on a string) Normal bile ducts look like tubes.
She said there were definite changes old and new. These changes are consistent with Primary Sclerosing Cholangitis. He had inflammation of his liver. Since the MRI isn’t 100% she wants a biopsy for two reasons:
1- to confirm diagnosis
2- to see if there is progression in his active autoimmune
She can tell if there is scar tissue.
Random things I jotted down that she mentioned:
•Vancomiacin antibiotic she asked has he ever been on it. She has been reading about that. (Not sure if I spelled it correctly)
•she said keep the radar up for inflammatory bowel disease. And actually several others that sound like that but I didn’t write down.
[Note to self: If I haven’t heard from the DI dept I need to call them 832-826-5303 to schedule the biopsy.]
We discussed PSC somewhat. And she mentioned the next time we are in the office she would show us the images and mentioned that PSC can be slow and is chronic but it can go his entire life without any complications. But we need to be aware of it, keep an eye on it, and know he is already on all of the right treatment.
Kevin looks good. Feels good. And has the best schedule for his senior year! When I told Kevin I was crying but not really because of the news, and I told him not to take my tears as a sign of how good or bad anything was–he was like mom: you cry over everything. (And it’s back to school day here. Senior; New school for Caleigh; Two still away in college…Got Tears?) Then a little after he asked me when I do schedule the biopsy can I please schedule it on a Tuesday because that is the day marching band is off this year, and if he misses a day he doesn’t get to march in that week’s show! Really Kevin?! I will try, but I kind of think you will have some restrictions on lifting the heavy tuba/sousaphone after a biopsy but what do I know! I will try!
The Lord is answering some amazing prayers and recently my prayer life was strengthened when I was given a copy of a devotional book from a Moms in Prayer friend called Draw the Circle. Day 4 is titled “Don’t Pray Away” and key statements have stuck with me:
•”Sometimes the purpose of prayer is to get us out of circumstances, but more often than not, the purpose of prayer is to get us through them.”
•”Can our prayers change our circumstances? Absolutely! But when our circumstances don’t change, it’s often an indication that God is trying to change us. The primary purpose of prayer is not to change circumstances; the primary purpose of prayer is to change us! But either way, the chief objective remains the same: to glorify God in any and every situation.”
•”Jesus answered, Neither hath this man sinned, nor his parents: but that the works of God should be made manifest in him.” (John 9:3 KJV)
But even more key than these reminders is knowing that He is giving Kevin exactly what He knows he needs to in turn glorify Him. He is giving it! He knows. (In other words our back to school news is not news to God!)
We will glorify Him!
So Much for Trending
August 11, 2014
Dr Walsh called. She wants to do an MRI to see what his bile ducts are doing. That GGT number escalated based on the last labs. That’s the number that shows her if the bile ducts in his liver are hardening.
Kevin’s latest labs.
GGT: 124
AST: 36
ALT: 47
That GGT level is just not where it needs to be. She wants to take a peek inside to see if what the numbers are showing line up with what his bile ducts look like and depending on those images may or may not order a biopsy. She wants to be as noninvasive as possible. And only add the low dose steroid again to his meds if absolutely needed.
I’m like….so an MRI can show what the liver bile ducts look like?! You know she has got to be so patient. I’m mostly just taking it in. I’m a repeater. And a literal idiot! When they called to actually schedule the MRI I could hardly make it through the questions: Does he have metal anywhere on his body!? Well, I have metal military fillings and I know he has fillings…I don’t know!?! Has he ever had contrast? Can he be still or will he need sedation? They actually called it an MRCP. So I asked them: what is an MRCP! They had to look it up:) See how it feels!?!
I will admit. I wasn’t ready to hear that. I wanted it to just be the nurse calling. I wanted them to say we will repeat the labs. Even though it’s not what I wanted to hear I cannot tell you how very thankful I am for His watchful eye! A lot can happen between now and the peek inside and many are praying for His will in Kevin’s life. And for that I am forever grateful.
The Trending GGT
Dr. Walsh Summer Check Up 6-17
She is expecting! She is due mid September:) That’s a fun and exciting note!
She really thought Kevin looked great! Caleigh was with us today and when Dr. Walsh asked what was Kevin’s plans for the summer his baby sister replied: eating cheese. Yep. She just said that!
You can tell this doctor is a children’s doctor at Texas Children’s because she just rolled with it adding the many benefits of cheese! On the car ride home I asked Kevin if that mortified him and he said not at all. So I was mortified! We see her for 20 minutes every 6 months and we left her with a cheese eating impression!
Oh well…could be worse!
She hopped right up after asking Kevin if he understood any of what she spoke to me about over the phone last week and went all Dr. Pope on us drawing on the examining table paper explaining PSC (Primary Sclerosing Cholangitis.) She sketched out a liver, bile ducts, gall bladder, intestine, stomach,and quite possibly an esophagus!
Anyway she explained the path of food. It travels to the stomach. Then through the intestines. At the point where the bile ducts intersect the intestine she said it stops and asks the duct (or maybe the brain) for some bile to help with fat digestion. (On a side note she mentioned that bile is what turns urine yellow and stools brown) Anyway, she said almost everything you eat has some fat…however in Kevin’s case she compared his bile ducts to his immune system. His immune system was attacking his liver. That flare for now has settled down but the bile ducts are now NOT wanting to settle down or at least that is what the elevated GGT (bile duct number) is telling her and her colleagues. So his liver is doing better. But this PSC as she explained earlier to me is what they call an overlapping syndrome. She also explained that Ursodiol increases the bile flow or pushes it out which is a medication she added back in December.
What to do. She contemplated about putting him back on a low dose steroid he was on from January to March which helped get things on the AIH (Autoimmune Hepatitis with hepatitis simply meaning inflammation of the liver) side thankfully back under control. She decided to hold off on the steroid, Buedesonide, for now and even wait until two weeks after his wisdom teeth removal surgery to repeat labs. Depending on that result she may want to start up on that steroid. She definitely wants the labs repeated every 6-12 weeks. She apologized for being anal about the labs but said since she would be out to have her baby she wanted everyone “tucked in and doing fine.” I was fine with getting labs and would have totally asked for more if she hadn’t wanted them!
So that’s the plan. Labs after camp. Note to self: We need to schedule his 6 month check later too once her calendar opens after she returns from having her baby. She said February. Unless anything needs attending…
We need to let the anesthesiologist know to check the anesthesia and pick the one least harsh on the liver. When she was drawing the picture she did say that his liver was looking great!
I asked: will steroids mask the symptoms of PSC? Her reply was no if anything it will help reduce the inflammation in the bile ducts.
I asked: Can he feel it when the bile ducts are inflamed? She replied no. She said thankfully he has been keeping his appointments and his labs have been helpful in seeing the increased number in the GGT. Because PSC is slow going. She is not worried in the least. She is watching it. Is not expecting it to progress quickly if indeed that is what he has.
I asked: When she initially put him on Ursodiol I thought it was because he was possibly leaning towards primary biliary cirrhosis because I googled what does that medicine treat:) That is when she gave us the good information that she prescribed it to help increase the bile flow…(I think I knew it was for the GGT but that’s as far as it got)
He was 5’10 and 1/2″
So I think he grew a half inch. But he couldn’t tell me:)
All in all it was a very good visit. He is being watched and labs will be done frequently enough to see the trending GGT. (Maybe we should start a hashtag on that! I think twitter when I hear trending anyway!)
#GGTprayitdown!
Clicking
Stink:( I googled it. I call this update: if you give a mom a mouse she’s gonna google and click…this link seemed legit. I clicked my way through each step. Not gonna lie. Really wish I hadn’t. Where did it even come from. I had all kinds of explanations in my head. Talked about them with some of you! PSC–what!? Have they seen the kid they are even saying this about!!! There is just no way this is the next thing…he looks great. Seems to be feeling great. But I really cannot speak for those bile ducts…lol!
For the record he isn’t officially diagnosed with this yet:) so am drying up the sobs and trusting Him! And I will be ahead of myself at Tuesday afternoon’s appointment.
And pray his GGT number lower! And wisdom for Dr. Walsh and her “liver colleagues”…
The link I clicked away on:
http://www.mayoclinic.org/diseases-conditions/primary-sclerosing-cholangitis/basics/definition/con-20029446
June 13, 2014

Still sitting
Dr. Walsh called immediately after Kevin got the pie in the face today at VBS for being the mystery man and stealing prizes from the children!
His GGT was down to 96 from 110 so she said that is good news but it is still not where it needs to be.
The Anca Blood test she ordered was a marker for what she mentioned is called Primary Scolosing Colongitis: PSC (Haven’t looked it up just spelled it like it sounded!) She said it was an Over Lapping Syndrome. She isn’t completely diagnosing him with this yet but after consulting with her liver colleagues it is where they think he is headed. She said it cannot be totally confirmed without more imaging and another biopsy. She said it is too early for that yet but will repeat labs in a month and keep him on the current medications (Ursodiol and Azathioprine) She wanted to see more of a trend also in that GGT number. She actually said there is nothing that can be done about PSC anyway. We see her next week so will probably have plenty of questions on that front.
I asked: Can this possibly just be his initial autoimmune hepatitis just flaring itself. She replied: no because the AST and ALT numbers would be up as well. So it would need to be all three for that to be the case. (GGT ALT and AST)
I also asked: how does an increased GGT number have anything to do with weight. (During a previous call they mentioned he needed to lose some weight) She replied: a high GGT can be because of fat deposition in the liver. To that Kevin said: so, you calling me fat!:) lol!
I told her I completely emptied our pantry. Only put back worthy things. I said he would have to leave the house to find anything really unworthy:) He is also working out with a trainer in our fitness center in our neighborhood. So he is on an excellent path on that front. We think he has always looked great anyway!
He is very active…almost too active! The band auditions were recently posted for next year’s band placement, and he made the top band first chair tuba!!!!! It’s called Wind Ensemble. He was so cute when he got that news. He said, “I’m gonna be honest with you; I was a little surprised when I saw my name there!” I’m not so much surprised as I am SCARED! That band is intense! He takes the ACT in the morning, then gets to play in a showcase baseball tournament up in Tomball where college scouts will be present. So we are sitting, praying for healing in Kevin’s liver, and direction and guidance for his doctors and for his senior year and exact college placement. I love what more than one person has told me about Kevin: God has big plans for his life…I agree! We will keep praying He will use him for whatever purpose He has planned, and that He will reveal to us just enough to help keep him centered.
May 27, 2014
Sit
His labs were Monday, May 12. MONDAY MAY 19 I left a message with one nurse at Dr. Walsh’s office. I needed the results from labs as well as info for oral surgeon. (Kevin’s 3 wisdom teeth are scheduled to be surgically removed June 19) Dr. Walsh called us herself Tuesday the 20th. Note to self is call and tell the nurses we had the labs done so they can be watching for them. I think I call too much–not so.
She gave me these results:
AST same & ALT same but …
GGT 110 (!)–this was 38-45-40 in labs past. Dr Walsh said repeat in two weeks. (Which is actually next week) She put orders in at Labcorp. But also mentioned he could be working on another liver disease. Or fighting something viral. This is a phone conversation so I could cry pretty much unnoticed!
On Jan 2 of this year his GGT was up to 145 so she added Ursodiol to be taken twice a day along with the current low dose chemotherapy treatment he has been on since diagnosis in September 2011–Azathioprine. And I was hoping we could drop meds or at least one of them:) But I was for sure hoping that GGT was lowered. Not creeping back up! She said he needs to lose weight and take the meds everyday. We recently took his reminder off of our phones and had him take this over so even though we keep a close eye on it, it is his job. I told her this with my voice cracking because I had to ask if inconsistent taking of the daily meds could give us this number. She said it could but they would retest and can check those levels so wait and see then. Kevin does a good job remembering it’s me that is having the tough time letting go of that control. (Not to mention trying to find something easy to blame this on!)
Kevin is fine hearing the numbers, me?–not so much! But I don’t walk around with them long at all before I am comforted by Him. And hold on for a plug for Wednesday night prayer meeting: I wanted to put out an APB! Text. Email. Let my praying friends pray for that GGT number. I still am but in quietness and strength I am letting it sit with me. I didn’t have it in me but it was like he was telling me to sit on this a while. Those I immediately had contact with I shared but just felt the APB blitz could wait. He impressed that on me I know because when we got to church Wednesday night I am floored by His presence. (and it’s our first service that we didn’t have AWANA before so it’s a nice relaxing arrival:) and we even had guests visiting from West Coast Baptist College so it was a fun almost summer feel! Pastor let the group take over most of the service but still got up and said he would keep it short…and in that next 15 minutes the verses he led us to read JUMPED off the pages of scripture and into my heart. It was in Ruth too. Great book. Easy to read and adore. One I think I would say nope: nothing gonna be there for me. I zapped it through my mind thinking that then turned to the passage. But I heard Pastor reading them before I could even find them and things in my heart started spinning it all together. My mental conversation with myself. “Wait. I’m turning to Ruth 3:18. I know those chapters. Love them! Sit. Sit still?! He is telling me to sit still…” Then I found them:
Passages he referred to from Ruth and Isaiah:
“Then said she, Sit still, my daughter, until thou know how the matter will fall: for the man will not be in rest, until he have finished the thing this day. (Ruth 3:18 KJV)
For the Egyptians shall help in vain, and to no purpose: therefore have I cried concerning this, Their strength is to sit still.
For thus saith the Lord God, the Holy One of Israel; In returning and rest shall ye be saved; in quietness and in confidence shall be your strength: and ye would not. (Isaiah 30:7, 15 KJV)”
Absolutely comforting words. I was overwhelmed with this confirmation to sit. And may I add…sit until I know how the matter will fall…..smiles….smiles….smiles! I know He knows me but people HE KNOWS ME!
So, yes, I have been sitting with this. And I am asking all who read this obscure page on Kevin will pray while we sit! Pray specifically for his GGT number to be lowered in the next labs if it’s His will. Kevin is coughing and feels horrible and even missed school Thursday and Friday last week (which we surprised Keith with a birthday bay house Memorial Day unplugging so we all got to come instead of trickle in) but maybe his body is fighting something viral. We saw Dr. Pope Thursday. I told him the GGT number. He added of course the kid who has what no one has hardly heard of has his number going up! And to basically wait for the next numbers. Again I hear from both Popes in my life to sit & wait. Pray for that number! But also for direction if the number hasn’t changed that the doctors will have wisdom for the best method of healing his liver or diagnosing what else could be happening. Sit and pray with me while we wait…
March 20, 2014
Nurse Tiffany called today with his numbers. Kevin’s GGT is still slightly elevated but down from the last time. It was at a 40. So he went 40-44-38 the last three labs. They are letting him go 8 weeks before drawing them again. So the week of May 5-9.
March 17, 2014
We went to have his labs done in Tomball at the Quest there again. Things have settled down somewhat so we could stay close to home. That means he didn’t miss school but hopped up there after school. He even drove himself there and met me! We were in and out and he could hop back up for his band sectionals and I could grab Caleigh after school:) (beats that commute to Texas Children’s anyway!)
March 4, 2014
Got the numbers call twice today. First they called and said lower his steroid since his GGT was 44. It was slightly elevated but not too much. Then I reminded them he was already on the lowest of the taper down. So was taking 3 mg of the 9mg prescribed steroid from the end of December. So she said stay on that plan. Then called back after speaking to the doctor and said she wants him off the steroid. Horray for that especially since he was leaving for Disney World with the band and that meant less medicine bottles to send with them!
February 22, 2014
After a long break from baseball due to band and then basketball commitments Kevin was back on the mound tonight! Pastor Caleb got some great shots of him and I will upload them here soon. He had a great game. Got the win. I loved just being in this moment. Loved seeing him on the mound just doing what he likes to do–enjoying being there. It was no big deal really anymore to me if we won or what he threw. It was just wonderful seeing him loving where he was. He threw with power. I am forever thankful for that moment. Thankful for his continued strength. Thankful for his joy.


Kevin had been at an Impact Field Day having a blast with the teens then mentioned that he had a game later to his Youth Pastor. He showed up in New Caney to support Kevin. I was too cold to get up and snap a photo. Gotta love our YP for actually capturing this moment I have in my head!
February 19, 2014
We got the results from Kevin’s tests Monday today. Although nothing on her end regarding why he was lightheaded she actually wants him to see his PCP for that. He made it through school today so we will just see. It could be nothing.
His ultrasound showed a minimal or slightly enlarged spleen. Jocelyn is the nurse I spoke with this afternoon who said Dr. Walsh is not too concerned about the spleen at this time but will continue to monitor it. She also gave me his numbers:
ALT: 13
AST: 17
GGT: 38
He does get to drop another steroid so that puts him only at 3 mg. He stays at that until after the next labs in two weeks so March 3. (I need to call a day in advance to let them know which lab we will go to)
I wish I could say we know why his spleen is hurting but at least they are comfortable with what they saw. He will be great at determining what part of his innards are what since he has pretty much experienced all things digestive:) And I think I told her we would just keep trucking through it even though clearly I am doing none of the trucking! It’s all Kevin! That’s a “he-we!” And where did this trucking line come from anyway…
February 17, 2014
Kevin had another ultrasound done today. It was an easy go traffic wise because it was Presidents Day! No one on the Houston roads. We had a super great guy perform this ultrasound. Kevin responded after that he used really big words and had a deep voice. He needed this one since Dr. Walsh wanted to see what could be causing his side pain. The technician said nothing looked too scary.
February 5, 2014
What is up with Kevin? He has not felt great at all. Is actually really hurting. Not sleeping well. It was time for labs on Monday so down to TCH we went. To get the specific orders in our hands none of this quest only seeing so many and getting numbers and not getting numbers this way. At least until things settle down.
Maybe from the liver prospective they have settled down based on this weeks levels. Jocelyn the other nurse for Dr. Walsh called us back today. She said his levels are improving.
ALT: 9
AST: 16
GGT: 38 (it was at 147–normal is 9-31)
So with those numbers she still wants him to continue Azathioprine and Ursodiol but he can start to taper off the steroid Buedesonide from 9mg to 6mg beginning today. And she wants to repeat labs on the 17th. We have an appointment later today with Dr. Pope. Hopefully he will have some insight as to why he is walking around hurting. Especially his left side. Mostly stomach maybe intestine. What do I know?
I am very thankful his levels are returning to normal. Just a little concerned he doesn’t feel as normal as his levels are though:)
*saw Dr. Pope–he examined Kevin and as Kevin pointed to where his pain was Dr. Pope pinpointed that as his spleen. Since tests were just done he gave an explanation as to why nothing should be rerun at this moment but to monitor it. Once Dr. Walsh’s office touched bases with us about today’s PCP visit she had us schedule an ultrasound for the 17th. Not sure when she touched bases but it was about a week after seeing Dr. Pope. I had called them. They never returned my call. I assumed it was because they didn’t need to tell me anything. Actually, the message I left wasn’t delivered or just lost. So once they saw he was still hurting. Saw Dr. Pope. They then scheduled the ultrasound. Always follow up.
January 3, 2014
I totally saw this on a friend’s Facebook page and just had this image in my head all week. It is striking how much it pictures how much He loves us through His word! He is the living word. He is The Word:) We are loved.

Jan 2 cont…
He drank water from the rice field!
Tonight I had a “he drank water from the rice field!” moment. Or almost. And could still?? Once Mam Maw blurted this out during an MDAnderson doctor visit. She just knew it would help them with all Big B was dealing with. Mam Maw I don’t blame you!
I walked in tonight and saw Kevin drinking a Fresca. He loves flavored beverages. I was like. You are drinking Fresca? Doesn’t that have grapefruit juice in it? He’s like. I don’t know. So we picked it up and read the can. Yep. Grapefruit juice. Which Keith and Kevin said in passing it only reduces the effectiveness of the medicine. Boy oh boy. Had to fight tears. Enough came out that kev asked if I was ok and Caleigh sat beside me with her light up Lego set and we built until it was all better. But I wanted to call the doctor and scream: he’s drinking Fresca…funny. But not. Kevin said he wouldn’t drink it anymore and he’s maybe only had two. But he said maybe…:) and I said I wasn’t going to think about it:)
January 2, 2014
“Something is Going On”
Dr. Walsh called with the results of the ultrasound and the latest labs.
She said the ultrasound showed a smooth liver and no abnormalities. She said the spleen was slightly enlarged but not as much compared to the last images two years ago.
The lab that measures his dosage showed that his body is doing exactly what it should be with the dose he is taking. So he does not need an increase. She will check this again in about two to three months. (See previous explanation in post before this about PROMETHEUS® Thiopurine Metabolites)
However she did say “something is going on.” His bile duct number, GGT, and liver numbers, ALT AST, have bumped. I had my paper out w the initials ready to write exactly how much they bumped when she said she wanted to start him on Ursodiol today. He takes it twice a day. Along with everything else he is currently taking. She is always so nice and asking how he is feeling. Tell him she says hi. And to enjoy his break. He has been struggling with acid reflux / heartburn. She said it was a side effect of the steroid. I said he had been reading the paper it came with:) She replied “smart kid.” He is:) So she added another prescription to help with that just for as long as he is on the steroids.
She also wants to repeat the labs in a month. Note to self: go to TCH 11 th floor. Ask for Tiffany. She will have the stickers. Then head to the 3 rd floor for labs. After Feb 1. If the labs aren’t better then another biopsy may be needed.
I don’t know what to think so I won’t yet…I am ever so thankful for his doctors, nurses, TCH, lab people… Am blessed to have such a caring savior to keep His eye on Kevin with the wisdom He has given them all.
December 26, 2013
Kevin went for his scheduled ultrasound appointment today at 11:00. It was pretty uneventful. He couldn’t eat or drink 8 hours before and once we arrived to TCH it seemed to be the least crowded we’ve seen it. I don’t think the entire appointment even lasted 45 minutes. We had a very nice ultrasound technician. Keith and I were allowed in the room to watch. She pointed out everything she saw on the screen which was very interesting. The room was dark and quiet so I’m not gonna lie–I got pretty sleepy looking at Kevin’s innards! It was fascinating. I wish I could say I saw the surface of his liver. She said it looked smooth. She stepped out long enough to show the images to a doctor to make sure she got everything I guess. No real news for us yet. He is continuing his steroids along with his regular meds. No real side effects to speak of either. Which I’d say is all good…
December 20, 2013
#notgonnamissthis
I attended Caleigh’s last elementary Christmas party today! It was hotter than hot! We were melting in the classroom! I was also faithful to my Quest to Quest:) I phoned early today TCH just to check if the supervisor Don actually phoned Tiffany. I worked retail enough to know the phrases used to buy time; put off customers; redirect! Of course that is not what they did at all but honestly it’s in my mind. Keith’s motto: trust but verify. It’s all I was doing. Verifying trusty TCH:)
So I have my phone with me all day. Knowing since I left a message the return call would come….and it did. Terrific TCH Tiffany called only I was in Houston traffic. She explained wonderfully and so patiently and I will just put this out there repetitively what Quest filed. And what they needed that they haven’t filed but requested. What they need was Prometheus Thiopurine Metabolites. (Made her spell it. I googled it. Am pasting here. This is sent out to California)
“PROMETHEUS® Thiopurine Metabolites Cat. # 3200
PROMETHEUS® Thiopurine Metabolites testing assists physicians in optimizing ongoing dosing of thiopurine immunosuppressant therapy to reach and maintain therapeutic goal. Thiopurine metabolite testing also helps to identify drug metabolite levels that may lead to toxicity and some of the reasons for treatment failure.
• A quantitative evaluation of 6-TGN (thioguanine nucleotide) and 6-MMPN (methyl mercaptopurine nucleotide)
• PROMETHEUS Thiopurine Metabolites is only offered at Prometheus.
• Specimen Requirements – Whole blood, 5.0 mL; EDTA / Lavender Top Tube.
• Shipping and Handling – Refrigerate; Ship with cold pack (DO NOT FREEZE).
• Storage Conditions/Stability – 8 days refrigerated; 24 hours ambient.
• Turn Around Time – 3 business days from date of receipt.
• Therapeutic Range – 6-TGN: 235-400 pmole/8X108 RBC; 6-MMPN: <5,700 pmole/8X108 RBC.
• Prometheus is located in San Diego, CA. Tax ID# 33-0685754 NPI# 1073642641.
• Licensed in several states including New York and California.
• Prometheus Laboratories Inc. is CLIA certified and accredited by the College of American Pathologists. This test was
developed and its performance characteristics determined by Prometheus Laboratories Inc. It has not been cleared or approved by the U.S. Food and Drug Administration.
CPT Codes (as applied by Prometheus)
• 82491(X2), Quantitative HPLC (High Pressure Liquid Chromatography) for each nucleotide in peripheral RBC,
separate stationary and mobile phase.
• Dubinsky MC, Reyes E, Ofman J, et al. A cost-effective analysis of alternative disease management strategies in patients with Crohn’s disease treated with azathioprine or 6-mercaptopurine. Am J Gastroenterol. 2005;100(10):2239- 2247.
• Seidman EG, Clinical use and practical application of TPMT enzyme and 6-mercaptopurine metabolite monitoring in IBD. Rev Gastroterol Disord. 2003;3(suppl 1):S30-S38.
• Cuffari C, et al. Utilization of erythrocyte 6-thioguanine metabolite levels to optimize azathioprine therapy in patients with inflammatory bowel disease. Gut. 2001;48:642-646.
• Dubinsky MC, Lamothe S, Yang HY, et al. Pharmacogenomics and metabolite measurement for 6-mercaptopurine therapy in inflammatory bowel disease. Gastroenterology. 2000;118:705-713.”
It was not checked in what I thought under metabolic panel. (Now I know that. It isn’t even done at Quest:) see above googled and pasted info!)That is done for the doctor to see like chemistry different levels and I think she can tell if he’s taking his medicine. Some numbers help her to know where he is in relation to other numbers. So that made sense. She said they put in a complaint or spoke with Quest with where their system was failing. Which was good to know. I just didn’t know my part in this. I want Kevin to have the best care. I want to be as informed as I can be. Including being told all information whether I know what they are saying or not. It can just add a new wrinkle to my brain. So the next time I hear it it will sound more familiar!
I asked if there was a lab who allowed us to log in and see what they checked. She said no. Sometimes the dr will release them to my chart but so far they don’t have that. I just think there should be. Maybe because it is a way to check after this that what we leave the office thinking we will go and get tested for actually was done. Even if we have no idea what the test results mean we can see the completed information!
That test will be ready to read on the 26th. His ultrasound is that day. She also called me back once I got home which was an answer to prayer. No sooner was I telling Keith over dinner I just felt so perplexed. Lots if information. He said give it time. Then Tiffany called again. She had checked with Quest to be sure that this time they really did run that test. And they did. It was almost 7 pm. She made me happy cry telling me “Miss Beth I am the only one left in this building! I have been checking on you and she stayed until I got it!” Isn’t that just the best. She said she knows I am trying and only want what’s best for my son. Yep. Exactly. And I know they think we know more than we do because we are in there a lot but really I hear the buzz words and only do what they say. I can look and sound like a real idiot! I’m sooo literal! It is the biggest of my setbacks. I even try to figure out what I’m being literal about so I can give myself a heads up and then still get hit with the Amelia Bedelia award!
All that to say I am relieved to know that it feels like closure. As much as I want to give Quest what for I think they have. I also know I have learned to follow up! Somehow things got really layered with paperwork and the trail was fuzzy. It’s good. I’m good.
December 19, 2013
After Tiffany from TCH explained what to look for on the insurance claims I did just that. I saw several times a metabolic panel was ordered so thinking that was what was missing I called Quest. Very blessed to have an informative willing listener behind choice number 3! I think her name was Estella. She took my information and walked it to client services and said we should hear from them soon. Like within 30 minutes soon. And we did! Don one of the supervisors called. I explained as best I could what I thought was missing. He said he would call Tiffany at TCH. There are definitely some communication issues this company needs to work out but they were approachable and caring with what I call compassionate and attentive ear.
December 18, 2013
Inside Eyes
That seems to be my happy phrase for this update. We got the numbers call. Here are the numbers:
GGT: 147 normal is 31
ALT: 52 normal is 46
AST: 41 normal is 32
Thyprorine (?) metabolites will not be ready yet. One call they were throwing out all kinds of terms. Like 6mp and promethisis! She said it was just levels that they counted.
So the GGT doubled and the liver panels were on the rise. Dr. Walsh called me herself. Gave such good clear information. She prepped us well yesterday with the various plans. So she ruled out that it was a virus. She put him on a steroid called Budesonide 3 mg per capsule and wants him to take 9 mg each day. She said this one is different from the first one he was on and a lower dose. Such good news. She also ordered an ultrasound. We will have that done on the 26 th. It’s right downtown at TCH. And he cannot eat for 8 hours before.
It seemed like the calls were back to back with her office checking on us after we had time to take in the new news. Then scheduling an ultrasound. Then she knew I was on the quest case to find his missing numbers so she had a wonderful assistant (?) named Tiffany call and explain that. I get it. Not sure I can make anyone else get it. It still is somewhat frustrating and definitely a problem but my desire to hunt them down and just make them give us those numbers has all but diminished. As “orders” for labs are entered, the people drawing the blood really only see one at a time. Even if I say they need __________ checked. I can’t order it:) She gave me the best info. Always ask what they are drawing. We need to know what we are there for. Which sounds like a no brainer but if I say are you checking _______. They may just say what they see. Sometimes the code is off. Instead if they say what they see and I ask is this one there that we are for sure needing then if they say they cannot see the order we are to pick up the phone and call their office. They can remedy that situation easier than making numbers appear of lab work that was ordered but really never seen. Switching labs will not help.
I just want to help. I want justice done. We ordered these numbers three times. If they are out there I want them. But the thing of it is the actual orders are still out there. She could see that they were never followed based on other doctors submitting orders and the flawed system of them only being able to see the last order. It is ridiculous I admit but who knew!! When they say there is a standing order I figure they know what to check! She is turning this into her contact. I wish I knew who to turn it in to. Just as helpful info on what to expect and not expect at Quest!
She asked if I had questions. It is unbelievable that I actually asked her this but I did word my question to her this way: so with all you are seeing you feel sure he has autoimmune hepatitis. Just checking. Kevin asked how long he needed to take the steroids:) I’m like good question. I’m guessing as soon as his numbers start heading back within normal range:) We thought the numbers could be skewed since we never fasted before the routine lab work. But she did not think we needed to fast before those levels…
So many prayers and concerned family and friends. I know I’ve texted answers to how Kevin is actually feeling. He is feeling fine. Which is why I titled this invisible eyes. And I am praising Him for what the doctors can see in the blood work!!! They have caught this one before he knew he even had it! We are fearfully and wonderfully made. Ps 139 This thought got me back. Snapped out of my crying spell if you will. Inside eyes. They can tell so much from the blood work! I am praising Him for that and know He’s on top of this:) and so is TCH!
December 17, 2013
Bummer…I poured my heart out and the entire thing went away…horrifying yet a great reminder I forgot to save…plus maybe not the best idea to update on my old iphone! I feel better even though none of it is recorded for me to see!
Today was a check up with Dr. Walsh downtown Texas Children’s Hospital TCH. She is concerned about Kevin’s GGT level. (Explained it gives us insight into what the bile ducts are doing which lead out of the liver.) September it was at 44 and November it was up to 77. The post below was a wonderful 26! I’ll admit I teared up as it was hitting me that this was not the quick good news/normal numbers routine visit I was expecting but as she incitefully explained and mentioned they are on top of this…Keith reminded me of this exactly! Depending on today’s labs several options are available. Ultrasound. Biopsy. Steriods. Increased dosage of his daily medication or it could be nothing but a virus his body has been fighting…none of which we will even know until we get the numbers call. (self: you even sound better! Good job phone for deleting the wordy whiner!)
I do know it was very frustrating to her and me and Kevin that Quest Diagnostics has still not provided some levels that we know we are asking for yet they do not have. Keith said for me to call them since we have paid for lab work we either need to know where the numbers are or get a refund. And for the record to myself Kevin did get his flu shot on Oct 8 at the CVS. (Too bad we couldn’t remember that when we were being checked in!) She did ask how he was feeling of which we explained the migraine meds Dr Pope put him on as a back up to regular advil and the concern Dr. Tsai W had when we saw her for heartburn related issues since we couldn’t get ino Dr. Pope and that she too ordered labs and even hunted us down by phone because we hadn’t gotten in yet! So crazy that those numbers are nowhere! Dumbfounding! She said she would call us with the today’s numbers this week but the ones that tell us if he has out grown his dose (metabolytes?) will take a little longer…which is so frustrating since we have asked for them at least twice now! We should have something to compare to! And I guess I am shocked since the last visit we even discussed getting off meds in the future…she mentioned that she had been discussing Kevin’s case with colleagues but after seeing the latest labs was like…forget that for now lets figure out why that number is increasing. Dr. Walsh used this as a reminder to Kevin that no matter how he is feeling what he has is for a lifetime and he needs to keep his check ups and lab appointments:)
I am feeling frustrated yet confident and trusting with some weepy tears…love that when the tears started flowing in her office that she looked at Kevin and said…well, he seems to be use to it! Keith however gave me a once over over the phone that I shouldn’t be crying with Kevin right there! I love that he is looking out so for his boy that makes me weepy and for sure know that just maybe I shouldn’t be the one going to the check ups! One thing I know–my kids are use to my tears. And my precious Lord and Savior catches every one…He cares so much for us. I am just determined to keep calling on Him for healing and know He has a perfect purpose and plan for Kevin’s life.
June 18, 2013
The routine blood work numbers came in but we will just have to wait until next time for the metabolite check. The dr called and the orders just weren’t followed. No rush she said.
So here’s the routine:
AST:20 range (12-32)
ALT:13 range (7-33)
GGT:26 range (8-32)
June 11, 2013
We saw Dr. Mehta today. It was just a routine check up with labs. She is requesting labs today to check metabolites. I think here she mentioned to see if he has grown out of his dose. Also, she mentioned down the road … After college even, like that far down(!) that there is a chance he may can try coming off of his medicine. It would be our choice. So that is something to think about! She would be keeping close labs if we did. And it would involve another liver biopsy. Today we will draw labs. I just need to remember to put the 3 month lab on my calendar. I think we forgot to do one between 6 months visits! So we will do several labs while she is checking his dose levels but once that is determined we will be back to every 3 months.
November 16, 2012
Kevin and I saw Dr. Mehta on Election Day November 6! She said to pick the next holiday to have the check up so he wouldn’t miss any school. I actually took my camera with me since it was a “well” visit and we have come so far! I know I am becoming my mother now that I am taking pictures of our docotrs! Dr. Mehta or as we would refer to her earlier when we couldn’t keep all the doctor’s straight, Princess Jasmine, was fine with me taking one. I also have to include the picture of the “pigs” and I call them pigs everytime we pass them going into the hospital and up to that 11th floor but every time Kevin reminds me they are cows mom! I got the “numbers call” and for lack of having a better place to keep my notes I really have to post them here. The nurse said that when Dr. Mehta saw the numbers she told the nurse she had to call since they were the best ever! So, here goes:
- AST: 16 (12-32 normal range)
- ALT: 12 (7-32 normal range)
- GGT: 17 (8-32 normal range)
Such good news! He has come so far! So far that I have indeed fogotten how high his numbers originally were, and I am sure they are listed somewhere below but love that it is not a figure in my head. He is now compared to this time last year completely active! Band, Basketball, Baseball…and loads and loads of school work. Now to remember how to insert those photos:

July 12, 2012
Kevin is doing great! We visited Texas Children’s last month and he does not have to go again for months as long as all stays well. She said pick a holiday in the fall and schedule his check up so he doesn’t have to miss school. So i looked at the calendar and we will go in on election day! His labs are every 3 months so we will have one before seeing her and then one when we see her. They just opened a lab on that 11th floor of TX Children’s so it will be easy. She had a nutritionalists hop in and speak to us since I had seen a great one in February without Kevin but this one could speak straight to him about eating healthy. That helped me immensely. I am proud of the choices Kevin is making on his own. I am praying for continued strength and healing for him as well as a cure for his autoimmune disorder. Until then she is keeping him on his 150mg dosage of azathioprine (very low dose of chemo) to keep it in remission. She asked him how often in 3 weeks does he forget his meds and he said about once. I told her the story of seeing he forgot his meds and it was midnight so I took them up to him. Woke him. Said you forgot your meds and he took them and before I could get to bed he was in the shower! He thought it was time for school! She reminded him that taking the meds regularly keeps all the levels even and remission away. We stepped off the bus from church camp recently and he said all he remembered from last years camp was how much his stomach hurt. He would be hungry try to eat. Not be able to eat. Then the cycle would start over. I am so thankful with His help we were put in the right hands for healing to begin.
June 2012
I never really posted updates to visits between these two and that is probably due to one word: Geometry! Missing so much even after January from getting off steroids made for very rough days ahead in geometry! We found a wonderful tutor. He ended up making a commended score on 4 of 5 EOCs. Geometry was one of them! He missed commended by a smidge in English and we will take that! So ready for him to start this next school year with a clean slate.
Saturday December 31, 2011
I’m calling this post the “don’t take anything into the new year that you meant to do earlier post update on Kevin”. It will be all over the place but done!
The great news! Kevin took his last steroid Wednesday Dec 28! I have notes from doctor calls and visits tucked here and there that I need to get posted here! (it helps me to have a place i can go back and look) He did get all caught up with make up school work since the last update but it took every bit of that 2nd 6 weeks. The semester ends mid January so he is back on track in that area. Also we said we were going to do something big and we will but for now he plays that card everytime he thinks of it. We might get him a new video game or a subscription on mine quest and he will say remember all that make up work I did! I don’t think I could ever tell him no if he peppers it with that! (just don’t tell the Ezzios!)
We saw Dr. Mehta at Texas Childrens on Dec 6 for a routine check up. The next week which was the last week before Christmas break he “hit that brick wall!” We had to visit Dr. Pope and he did a “fatigue work up on him.” Basically ruled out a list of things he scribbled on the examining paper. The funny one was “burning the candle at both ends!” Yep…thats Kevin! He is manager of the basketball team and they went one night to Pasedena! The very next night was a wonderful band Christmas concert and homework and projects and Christmas parties sprinkled in to keep him up late. So Dr Pope ordered labs and gave him a school note since he missed 2 days. The quick results before we left his office showed that he was dropping bilirubin in his urine at a +1. Which “they say” normal kids don’t do but Kevin is not a normal kid. Can you believe that? Dr. Pope talking smack about my Kevin! Other than that it ruled out a lot that his pain and tiredness wasnt. The bummer was we were about to get to go 8 weeks between labs. So to back track on the numbers from the labs (some of my scribbled notes) he had these numbers:
November 9 Labs AST: 31 ALT: 35 GGT: 85 Such good numbers! 1of 3 in normal range and the other 2 super close. AST was the normal FYI.
December 14 Dr Pope Labs AST: 73 ALT: 64 GGT: 83
Dr. Pope’s office called and had us call Dr. Mehta to tell her his panel results were on the website for her to look at to determine what she wanted to do. So basically Kevin wasn’t experiencing anything new from “the list!” but he wanted her to take a look and touch bases with us on our next move. But he basically thought the AIH was “flaring up.” I don’t know the terminology. Tag. Your it. That is what pops in my head! So she did call and basically wasn’t too concerned about his levels but was if his symptoms did not improve. He was experiencing some pain but not “get to the ER for a work up pain.” He had started his tapering of steroids, was advised to stop taking the Prevacid since the steroid dose was so small and almost done but other than that no other changes to note. She felt his body may be just fighting a virus and depending how he felt through the weekend of the 16th she would either order labs early or later in the next week. She wanted us to call her with how his weekend went and once we did her office got back with us to say she wanted labs and that they have put in a “standing order” at our Quest. That was happy sad news. Happy cause I didn’t have to keep up with the orders and have them when we went! I like to say I’m organized but where I let the orders folder “float” and my mini were 2 different places! So now we can just walk in and they will stick a needle in his arm no questions asked! Yep. That’s the sad.
Labs from December 20:
AST: 64 ALT: 73
What can I say. I got this numbers call with Tiffany during a “gel-ish” mani so when she said they were basically about the same I didn’t ask GGT number. She is not concerned at all still but wants us to have more labs next week. Our original 8 week orders were for jan 4 so we will go around then. So much for making it 8 weeks without a lab.
Also on the back track front from when we saw Dr. Mehta on Dec 6 for a routine check up. Nothing was going on then of course! When Texas Children’s calls to remind you of your appointment they also say please don’t come if you are sick. Which Keith was, so Kevin and I had to go solo on that visit. And I have notes from that visit in my red “all things medical” folder but it is not floating near me now. So i will just go from memory. I do know she asked if we were able to get any of Keith’s dads medical records and we had not then. She is just very interested in seeing family history. But mam maw sent us a stack of them back after Christmas so we will have more than she ever needed at our next visit in 3 months. It will take me that long to scan or copy them. (This Feb 17 it will be 10 years since Big Daddy passed away.)
My memory from that office visit was how hard she tried to get Kevin to talk to her about anything and he would just look at me smiling with shoulders shrugging! And how hard I tried to not look like a controlling mother who never lets her kid speak! She was not concerned with his weight gain but said it should be down at the next visit since he will be off steroids. I was concerned that the high dose of steroids might have stunted his growth but he measured an inch taller at 5′ 9″ from his first visit to her. Of course he couldn’t stand at that visit so will we ever be sure:) She did say to this that usually it is not a concern but if he needs a second round sometimes at his age it could. Which is where we are currently. With his levels rising a little Dr. Pope and Dr. Mehta said he just may be one of those candidates who needs to be on steroids a little longer and maybe even a low dose long term. But for now they are just going to continue to watch him. So we are watching him:) She wanted his vision retested due to migraines just to rule that out so we saw his eye dr over the break and other than his pre existing convergence insufficiency…double vision…he has had since the 3rd grade he is fine. So we will keep monitoring his headaches and if needed take the next step.
So much since the last post and I was going to stop posting! But even though we are adjusting through it all I need this place to keep my sanity! My mind written down. Well, half of it anyway!
I will close this post with a verse I send to those who catch me at “a bad time”:
And my Bible opens to Joel… “Therefore also now, saith the Lord, turn ye even to me with all your heart, and with fasting, and with weeping, and with mourning: And rend your heart, and not your garments, and turn unto the Lord your God: for he is gracious and merciful, slow to anger, and of great kindness…(Joel 2:12, 13 KJV)
I have been a weeping-mourning-rent-hearted mommy who is probably in need of sleep more than anything else, as always, and laugh remembering years ago going to my family practitioner for how tired I was with toddlers that I had to have something wrong and he prescribed a cook, a maid, and a nap! We continue to trust Him for direction for Kevin’s healing and find great peace in doing so.
Wednesday November 2, 2011
One thing we have noticed is he is finally not as hungry as he has been! He actually can come in the door and do something besides forage for food. His steroid dose is now tapered from 60 mg per day down to 25 mg. We did take him to the dermatologist since the rash has not improved if anything it’s worse and the antibiotics he wanted to put him on to help with it he said he doubted our hepatologist would approve. I called down there just in case and instead of her nurse calling back she called and said he is to never ever ever take doxycycline monohydrate…guess that settles that:) So an over the counter soap bar and shower foam will do for now. He is like 7 weeks from being totally off them so maybe he can just keep dealing with it. Yikes! Poor Kevin. On the make up front who knew next week is the end of the 2nd 6 weeks. I thought we had 3 more weeks. So he is now on the geometry fast track. He made up 1 of 3 tests yesterday and will make up test 2 on Friday leaving just one more before next Friday and he will be officially caught up! We will do something big when that happens…really BIG!
Wednesday October 26, 2011
We got the numbers call again so this is a much better place for me to put them than whatever paper is in front of me when we get the call! Great news: ALT: 54, AST: 27, GGT: 99 !!!!! She still wants another lab draw in 2 weeks and for him to keep tapering down on the steroids. He is at 15mg twice a day now from 60 mg when he started. He did need to see Dr. Pope last week for a rash we thought first was laundry soap or shower soap then steroid reaction but Dr. Pope said he thought it looked viral and keep an eye on it and if in 2 weeks it hasn’t improved then get in to a dermatologist. He has had energy last week and this week and as band is tapering down now basketball picks up with tomorrow being the first after school practice. I think he hasn’t even officially made the team yet so hopefully he will know something soon:)
Wednesday October 12, 2011
We got great news this week! Monday he got the all clear from his surgeon and today we got the numbers call again. ALT: 118. AST: 45. GGT: 160. He has dropped another 10 mg of steroids too. We are on the taper paper and will be til 2012! He gets to start going every 2 weeks for lab draws instead of weekly. He has left his hall pass at home and if you saw him in the halls you’d see a normal boy with his real back pack walking to class with everyone else! His after school energy is increasing too. Basketball is keeping him sore since they are in the weight room and band is keeping him busy. He may never really march the routine but he is on the field playing and in the stands. I have started this and gotten sidetracked so many times then it goes away! So this is probably the last update on this page since life is really dare I say: back to normal. As normal as living with a SMTWTFS kid can be any how:)
Wednesday October 5, 2011
I got “the numbers call.” He went to the lab yesterday in Tomball they send the results to his doctor at Texas Children’s and we hear all within 24 hours. His labs are better. His AST is 80 from 143 last week; his ALT is 221 from 409 last week; his GGT is 203 from 263 last week and all that EQUALS taper down on the steroids starts today!!!! If all goes according to the taper plan on the paper he will finish his steroids and be completely off of them 12 weeks from today. And that means he will go into 2012 just taking the low dose chemo. I am ready for that. I picked up a dozen kolaches with Tiffany when she was here on fall break and said he can have them as an after school snack and I will freeze the remaining and they can be a yummy warm out the door and in the jeep breakfast for him and Cole. I went to freeze the remaining and there was only 6 left! He ate half a box of kolaches for an after school snack!!! But the taper paper plan begins today!
Friday September 30, 2011
Kevin made it the last 4 days of school this week:) Today he even stayed after and dressed out in band for the football game. He played in the stands and on the field but he did not march. He has to learn something–I over heard the tubas say–like 50 more sets! It is a very good feeling to see how far he has come. It was also very weird being in such a crowded football game and feeling like we didn’t belong because we didn’t know what to expect. We will get the routine down but felt like visitors at a home game. He also took some tests last week so he is feeling like he’s got this! Yes! I took a picture with my cannon rebel and not this phone but maybe soon I will do the old school thing and download the photos so I can upload them:)
Wednesday September 28,2011
Some good news about Kevin’s levels. Dr. Mehta’s nurse Melanie called with the results of the lab he just did yesterday. The numbers are still lower and she wanted to check next week which we originally were off for labs next week before she will start tapering the steroids. They are not in front of me but the key one was in the 400s. Down originally from 1800s. This is week 2 of meds too so it’s going in the right direction. She also wants him on a multi vitamin and a separate vitamin D supplement. She said just pick one and I begged her please give me a brand. There are too many to choose from. She said since he has so many pills that chewable or gummies are an option and I thought to myself. You don’t know my kevy. Gummies are always an option! Sure enough when I picked him up and told him all the scoop I asked what type of multi vitamin he wanted and he smiled that adorable smile and said “Gummies!” We may have to get him a bigger SMTWTFS or as Cole pronounces it “SMorTWiTIFS!” It really is impossible to say but everytime Mam Maw visits and needs her medicine box Cole always makes her call it that before he will give it to her!
Tuesday September 27, 2011
Kevin is going to school today! The 6 weeks shockingly ends this Friday and he went 3 days of the first week of school and 3 1/2 days last week and we are shooting for 4 days the rest of this week. (10.5 days out if 30 not bad) He will receive lots of “I’s” and can get them removed slowly and without stress each teacher is saying, and they each have a great plan for him and are so willing to work with him. Such a praise! Caleigh is home one more day and is feeling much better and Keith even overheard her say, “I didn’t know staying home could be so much fun!” I told her wait til the make up work only for her to tell me third graders at her school never have make up work! Oh to be so happy and clueless!
Monday September 26, 2011
He stayed home from school but it was because he is not sleeping well and getting up all through the night. 2 things that happened today in way of follow up that all things medical make me nuts!
1- Dr. Mehta (Princess Jasmine) his liver/GI doctor called this morning to hear about his trip to her ER since she was out Friday. After she looked over all that days numbers and tests she is pretty sure he could have had hopefully a one time episode of pancreatitis. And is thinking of some back up plans if it occurs again:) She did say for us to not wait around for them to return our call but to leave a message that we are headed to ER if he ever experiences that pain again. Never knew that. Good to know. Especially since watching him in pain and being able to do nothing but run in another room and cry was not a working option! I asked what pancreatitis was and she said like it sounds and like my bff on the way down told me it was…an inflamation of the pancreas…but Dr. Mehta said after tomorrows lab work if his numbers go down any they may start tapering his steroids off. Steroids can cause loss of sleep she mentioned but was concerned that the azathioprine, the low low dose chemo for aih, could be causing the pancreas to be inflamed. But she said there are other options and will be thinking of some in case it turns out to be that. So we left the ER Friday so glad to be going home but with no real answers only to get a better picture today.
2-another interesting thing that makes me nuts is Kevin left his urologist a urine sample last week because we were thinking, again bff input(!), maybe he is getting a uti type infection since he is not sleeping needing to use the bathroom a couple of times in the night. So we got him up there to Tomball where our hero doctor is who performed the original procedure and left that office with their “sample.” I called everyday just checking. Especially since we were seeing Dr. Mehta last Thursday for a regular check up. They said it takes several days. Then in ER they made him give a sample and just this afternoon the urologist called and said he is growing some bacteria and it can keep him up at night so they are calling in an antibiotic once the hepatologist approves it he can start taking to clear that up. So kind of good news but poor guy could he have anything else wrong:) But hooray if it will help him get a good nights rest!
I am worn out from preparing healthy food for him! It’s prep for food, make the food, he eats the food, then wants to prep for the next meal! It’s a good thing we made Jedi Juice pops yesterday. Caleigh so far must be viral with all the symptoms of strep so she has been ringing the bell ordering more pops all day. Tonight we will finally prepare the dark side salsa and he wants Obewan kabobs! For lunch today he helped me make my moms wonderful home made tomato soup and a salad. The salad dressing was a gift from Florida and it had a recipe for salad on it so we tossed that together and he engulfed it! I’m either going to need the secret recipe for that 1905 dressing or my Florida source will need to keep us in that like we keep barbecue sauce and ketchup around when my nephews come! Caleigh is trying to read her blue bonnet books this year and since she was sick I read aloud to her with Kevin listening in the living room…of course it was Origami Yoda:) Yep…it’s a genuine Texas bluebonnet book!
Sunday September 25, 2011

Jedi-Juice Pops:) Kevin is having a great day but Caleigh had to go to the cvs minute clinic. She has all the symptoms of strep throat except a positive strep test:) So she is quarantined from Kevin and waiting it out. If “they” call we get the magic bullets if not she is just viral and gets rest and Tylenol for temp:) So once again when Kevin is not eating he is looking through the star wars cookbook for food! He made Wookie Cookies and has the ingredients for Bosk Brownies. He had planned some Dark Side Salsa but since Caleigh threw us for a loop we came home from church and had good old mom’s Costco quesidillas….I learned how to make them in the isle of Costco in Alaska and was amazed it was so simple. I was sure that was an out to eat at papasitos food for sure!!!
Saturday September 24, 2011
It was a very long day in emergency room 9 yesterday. We were sent home last night after blood tests and an ultrasound gave the team enough peace that he was not experiencing appendicitis or pancreatitis. He rested between tests and Keith and I sat. Read. Waited. We are so thankful that they found nothing serious but in the back of our minds will always wonder just what was going on. Today he is back to his usual “Emeril” self. He and Keith made Oola-la French toast for all of us for breakfast and had me write out a list for Obewan-kabobs Ewok eats and Bobba Fett-ucinni:) We will make a great team. He loves finding the plan and I so dread making one!
Friday September 23, 2011 cont noon
By 10 we had heard from the nurse a couple of times and they wanted us to get him to Texas Children’s ER to be evaluated for pancreatitis. So that is where we are now just figuring out today’s random abnormal pain:)
Friday September 23, 2011
He was standing by my bedside at 5:30 am in an unusual and abnormal amount of pain. So we have calls into his doctor and are watching him until they call. He is resting and did shower but I think he may have just hit a brick wall. It has been a good week for him but alot to take in too. The pain has substantially subsided but I just don’t think he thinks he would want this at school. So for now he is staying home. Getting rest. And waiting to hear from her.
Thursday September 22, 2011
The word of the week is “embedded!” We have been embedded in back to school with Kevin and make up work. Each day a different plan is revealed that makes the job that much more do-able. Geometry seems unending but he is getting it. English should be caught up after he writes a descriptive essay and we now have a skype Latin tutor to help get him through Latin:) He touched on biology tonight cause Keith was at a deacons meeting and I’m not allowed to ever help the kids with math. So we spent our time on biology vocabulary. Give me English and essays any day.
His check up downtown was today with his liver doctor and she spent alot of time with us. Clearly it is as I pictured. The white knights of the liver are fighting those red ninjas of the immune system. He doesn’t have a liver problem but an immune system problem. And that is causing the liver to be inflamed as well as his spleen. The lifestyle change we fretted and kept waiting for the list of what nots was not even a lifestyle change for us…alcohol and drugs are dangerous for him even in the smallest of quantities. That’s it! Well alright! We definitely got that covered so bring on the twinkies:) However he even has to be careful with Tylenol and ibuprofen. His numbers went from the 1800s when they found him to 700s and once they get to a normal range he can start tapering off the steroid but the very very low dose chemo he will take for life. We had a list of questions and she answered them plus so much more. She even handed him some reading material on everything. This was his first visit with her that he wasn’t lying down but sitting up…and she noticed. He continues blood lab work drawn on a schedule that finally tapers off to every 4 weeks. She monitors everything through those results and will let us know even when he can get his flu shot which he must get but once all is normal. He did not test positive for the Epstein Barr virus which she mentioned in an earlier phone call that would have been a double hit to the liver. Instead he has what he has and as so typical of most of her cases the autoimmune hepatitis was discovered on a separate issue pre-surgery routine lab and again thankfully so. He has been making it through school days! I just keep thinking that I’ll get a call from the nurse that he is asleep in their office but he comes in strong. He is looking so much better and he even drove out to get haircuts with us! Caleigh got bangs! I will finish this when I’m more awake! I keep nodding off:) Plus I dont have the notes in front of me and I am tapering off:)
Monday September 19, 2011 4:00PM

If you really know Kevin then you remember when he was a toddler my good friend called him “Emeril” because he loved playing with Tiffany’s little tykes kitchen and has been known to ask for a blender and even a toaster oven for Christmas and be excited to get it!! (and I must add if you know me I asked her, “who is Emeril!?) So as much as it goes against me to open a cookbook for a recipe Kevin had been looking through them over the last couple of weeks helping me out with what to make! I knew when they dismissed him from the hospital and realized how much he did enjoy circling the menu choices for the next day’s meals I’d have to shed my pantry style cooking and write out ingredients AND go on that frustrating scavenger hunt up and down isles and back up and down isles….some of you call that grocery shopping but I say nay nay!!! So these were the last things he wanted that we didn’t get to…Skywalker Smoothie, TIE Fighter Ties, and tonight hopefully those Greedo’s Burritos! So I headed to the store once I realized the phone was not going to ring for me to go pick him up:) And, the nurse, who sent me an email that he hadn’t come to her yet and stated that it looked like he was going to make it through the day. (And I promise I didn’t pay her to do this!) So it does feel like a first day of school where you try to be mother if the year! And the best compliment came from Cole that they weren’t a “stinker!” Another great moment was the carpool line. I haven’t been in a high school carpool in forever since Tiffany and Cole are both drivers but today I got in that line and waited to see him standing on the curb and his English teacher (who he has like 2nd period) was with him! She walked him out and motioned me to pull over then gave me the best explanation of his make up work including copies of what she wants and when to have it done. She said she does not want him stressing over her class and it can all be done by the middle if next week easily. So pretty soon I get to go back into “fun sucker” mode and crack the whip for homework and make up work to begin. I knew he needed to get this day behind him and am so thankful for the many prayers he received for strength….he was strengthened:) Now if they could find it in their hearts to save their daddy one of the fighters!
Monday September 19, 2011
Kevin is back at school and I am missing him!!! I hated that he was home and all that happened that he went through but it has been a sweet time with him and I cannot tell you how much I miss him:) He looked great and is equipped with notes from the nurse for a pass to her anytime and to leave class early to get to the next class until his next surgeon urologist visit October 10 and hopefully he gets fully cleared. He has blood drawn tomorrow after school, and we have a follow up liver doctor appointment this Thursday down at Texas Children’s. I am praying for Him to give Kevin strength to get through this new back to school transition from Phil 4:13 “I can do all things through Christ which strengtheneth me.”
Thursday September 15, 2011

I finally remembered to ask him if I could post this picture of him playing Pentago back in my room with his daddy a couple of nights ago. He had played Caleigh me and Cole earlier and needed someone else to whoop up on! He started the medicines on Tuesday night. I feel like I took a big hit of confusion with all that but it now has settled out and all is well. Keith and I divided and conquered Oak open house Tuesday night then snuck in a date to report what the other learned:) It kills me not to get around to both boys teachers but when 2 are at one school and it’s the bell schedule open house you have no choice but divide and conquer. I battled tears here and there because everyone was so concerned for Kevin. I thought I’d be fine walking the halls of the largest school this year in the Klein district of 4,132 students knowing I would not possibly really have time to bump into anyone I really knew. But precious caring friends were out there and around every corner. Even his teachers were so understanding and some mentioned how they were praying for him. Yeah…more tears. He is doing great! Today another subway meatball sub was delivered by a different friend and this one was a footlong! I had a six inch. He finished his footlong before I ate my last veggie bite!!! We got Kevin back:) He hasn’t had an appetite for that big of one in a long long time. And at open house in his English class I saw all they had read–short stories! And I remember doing my student teaching in 9th grade English and almost every short story listed was one of my favorites. So we read together yesterday and today great short stories. He has been re-listening to the entire narnia series on cd up to this point. So why not!? I even had fun turning pages in his book and reread some favorite poems. He also took notes on his tablet while watching a short story powerpoint. Keith and Cole have been helping him get started on geometry too so our prayers again are being answered! I love the picture of Him going behind us and picking up the pieces and have been praying especially for Kevin in the overwhelming amount of missing 3 1/2 weeks of school make up work for Him to do just that. And He is and will continue until all the grades are in. And every teacher said Oak is a paperless campus so Cole will have to show him how to navigate the online teacher drop boxes to turn stuff in. What I am wishing I had now, and we see his liver doctor one week from today to consult with her all we have just been officially given and maybe she will have some of it, is just a better visual of what is going on in his body. I know the definition of hepatitis—an inflammation of the liver and his is autoimmune hep—so his own immune system is fighting his liver or liver cells and causing scarring which ultimately leads to liver failure. But like when we had the lightning/fire 2 years ago and I needed to imagine Keebler Elves all in our walls drying out the wires I am wanting an animated picture! I hear clanking swords when I look at him and think of what his body is doing. And I asked Keith what he heard and he hears nothing! I explained to him it’s like that old school house rocks animation but the “I’m just a bill” is a medieval night type figure with swords and there are good ones and bad ones just fighting away! Only I see the protective white knights of the liver on the liver because after the liver biopsy I have a clear picture right where that organ is but the immune system bad nights, like modern red ninjas, and I think they are popping out everywhere he has blood flowing?!? So someone should alert our doctor I am expecting great things next week! I do know she mentioned there will be some lifestyle changes. Who mentions that and doesn’t give an immediate list. So here we are coming up with our own. Kevin asked for a Big Mac yesterday and we joked and said especially since he hasn’t even wanted one in so long that we better get it now before we get that lifestyle change list! We speculated that of course it will be eat fresher foods. So I told Kevin the meds he is taking will encourage hunger so pick fresh. He came to me later asking if he should throw away our baby carrots since there is black stuff on them and the bag was stamped September 5th! Yes! And wash your hands!!! So we are that house where not a carb goes bad but the fruits and veggies grow fuzz! I also saw on his chemo meds to wash your hands thoroughly after touching. So I said that will be another lifestyle change. We might have to become germaphobes. Or pretend germaphobes! He is a nail biter and one time we offered after trying everything else $10.00 for each nail he would need to cut with clippers. He got his hundred dollars and has been biting ever since! But I have been noticing he is getting fingernails again. I also am having him learn what pill he takes how many and when. Then give him oral quizzes. So again…lifestyle change! We are trying to figure em out before we go so we don’t walk away all gloom and doomed! Another one is frequent lab visits. I have one picked out close to us that he can go to without missing school. We are shooting for him to return to school this Monday. After walking Oak with a different perspective I can say he is going to be worn out. The 9th grade principal and AP and staff have emailed me telling me the nurse will have a note for him to be able to have extra time to get to classes so I guess no Segway will be needed! We will cancel that order:) And lastly we have been watching alot of movies and the clear play version of The Patriot is where we are. I am feeling finally some rest and retreat! But for most of the past few weeks felt like we were that lined up militia just waiting for and taking every thing shot at us! The past day or 2 have been restful and I would like to say I heard the “Retreat!!” sounded…there is no white flag of surrender waving here but we are feeling the retreat:) Gotta love a retreat.
Tuesday September 13, 2011
The question I keep getting is how is Kevin taking this all in? Its just like his baseball pitching days when he was given the nickname “the ice on the mound!” He could have just walked 5 players and be sitting waiting for the next inning to go out again but call me or Keith over to the fence and ask could he go bowling with this kid after the game he just invited him or maybe that he was hungry so would ask what are we eating later:) Then step on the mound the next inning and strike out 3! He works like this. He takes it all in and is so calm and collective. He’s known to strike out watching pitch after pitch go by and not even swing the bat because he didn’t like any of the pitches! One game I had had it and hollered from the bleachers, “I’ll stop feeding you if you go down looking! Swing That Bat!!!” So I remind mostly myself that right now he is just looking….watching every pitch go by these doctors and nurses and tests results can throw his way. I see the Lord protecting him in all of it. And with Caleigh one upping my prayer last night at tuck in he has the entire stands on his side:) I was praying with her and mentioned how thankful I was for medicines he can take everyday for life to make his liver better and in her prayer she said she “wanted that bumped down to 3 years.” I came down and told Kevin that, and it made him laugh. Then he has his brother Cole who I watched yesterday while I was taking phone calls and lots of notes come stand by me listening and reading and whispering to me it was all going to be fine. He then whether he knew it or not went on a self appointed mission of the evening as if he were called up. Operation Distraction. At one point I couldn’t find them even in the house. He had Kevin out on the trampoline! He’s asked him everyday when he came in from school to go jump with him–smiling. And yesterday when I got out there in my best I’m-the-mother-and-I-somehow-cannot-but-speak-the-obvious tone—said he cannot be on that! He had a biopsy and can have no physical activity from that alone for 2 weeks….and I was stopped at that with, mom, we are just walking around on it he needed some outside time. And I was like well yeah. It was a great idea as long as no real jumping was gonna happen! After that Cole set him up in the study and they did some LOTRO until dinner. He played him in Pentago and just pretty much stayed by his side not letting him think much about it. Then we have Tiffany who let the record show that before we even knew anything she was coming home this weekend and of course most importantly changed her profile picture to a brother one! True dedication! When I tucked Kevin in last night we had a good good long chat. Prayer. Hugs. Tears–all on my part:) And I would say I saw in him some actual relief. A big relief now knowing what it all is. And his doctor did a perfect job last week explaining what she was looking for from the biopsy so he has had a week of Ifs and can now just know it is what it is. He likes listening to KSBJ the Christian radio station and we both know when this one song comes on we joke and say there’s your song! I will try to paste below Mandisa’s “Stronger” lyrics below:
“Hey, heard you were up all night
Thinking about how your world ain’t right
And you wonder if things will ever get better
And you’re asking why is it always raining on you
When all you want is just a little good news
Instead of standing there stuck out in the weather
Oh, don’t hang your head
It’s gonna end
God’s right there
Even if it’s hard to see Him
I promise you that He still cares
When the waves are taking you under
Hold on just a little bit longer
He knows that this is gonna make you stronger, stronger
The pain ain’t gonna last forever
And things can only get better
Believe me
This is gonna make you stronger
Gonna make you stronger, stronger, stronger
Believe me, this is gonna make you …
Try and do the best you can
Hold on and let Him hold your hand
And go on and fall into the arms of Jesus
Oh, lift your head it’s gonna end
God’s right there
Even when you just can’t feel Him
I promise you that He still cares
‘Cause if He started this work in your life
He will be faithful to complete it
If only you believe it
He knows how much it hurts
And I’m sure that He’s gonna help you get through this
When the waves are taking you under
Hold on just a little bit longer
He knows that this is gonna make you stronger, stronger
The pain ain’t gonna last forever
In time it’s gonna get better
Believe me
This is gonna make you stronger”
Monday September 12, 2011
First, Kevin had a pretty good weekend. He wasn’t feeling great from the biopsy and of course what we now know officially as autoimmune hepatitis but he was coming along. I will say sometimes I see a sick little boy who looks weak and tired and skinny just not feeling his best then other times he is getting up by himself to get a drink and sitting at the table to eat! Last night for the first time in almost 3 weeks he climbed the stairs and slept in his bed! Today he got the all clear from the wonderful urologist we love and are so thankful for — that he should be ready to return to school once his liver doctor says he can. He’s the one who got Kevin on the next bus to Texas Children’s hospital to see the liver team down there because he knew something was not right with his liver:) And sure enough something is not exactly right. His liver doctor did call today after 4:30 with the news that he does have autoimmune hepatitis and that he has had it for quite some time:( So that means there is some damage–fibrosis/scarring. But the liver she said once treatment begins, tomorrow, and after time it starts healing itself from the damage if treated correctly and as long as his body accepts the treatment. She does not anticipate any problems. She got the number for our cvs and is calling the medicine in. He will take as mentioned last week at our visit with her a steroid coupled with the low dose chemotherapy Imuran. He will slowly come off the steroid but will take the Imuran for life. She is waiting on one more test from the biopsy that she said could show another thing going on with the liver that would be a double hit. She will call me tomorrow with that detail and for now it doesn’t change his course of treatment. It got foggy there too so once she said she is calling tomorrow again I stopped trying to figure it out in case it isn’t anything! Who am I kidding! But we got this:) She didn’t want to start treatment until the urologist approved it would not hinder any healing from the surgery he had almost 3 weeks ago. So by the time we finished talking his office was closed but I left a message with his answering service thinking we could talk in the morning and he called me back himself within 15 minutes! He gave the go ahead so tomorrow he will start the treatment and will be feeling better she said in a week or two. He can go to school after we see how he handles the meds and has more strength back:) We are thinking later this week and for sure early next week. He cannot participate in any physical activity for one month but after that should be able to surgery wise and A.H. (autoimmune hepatitis) wise too. She wants to visit with us again at out convenience to give us more information about it all and to see and speak with Kevin. She mentioned there will be some lifestyle changes but said we would talk of those later. Part of them are the many lab visits. They have his baseline and will watch him very closely doing labs every 2 weeks then bump it to every 4 weeks then bump it to every 8 weeks and will see him through out the process of his treatment. I did mention his headaches and she reversed the information we had on Tylenol and advil from the hospital stay. Kevin was on the pediatric floor and they said to not take Tylenol. But she said he could take Tylenol but stay away from ibuprofen especially as a recurring daily medicine. But if that is what works for his headaches then it is fine for those. We will have to ask later but she wanted him to be seen while he is having a bad headache to determine if it is a ??pressure condition build up??? I don’t know how to do that? Who will see you at the drop of a hat when you have a headache. Will ask her that. Kevin asked if she mentioned why his spleen is enlarged too and I forgot to ask that as well. I got teary eyed only when she started discussing the side effects of the meds and that meds can be toxic to your liver. But we sure do not desire the alternative…liver failure if we do not administer them:) The picture is coming together and we see God’s hand all over it. We are so thankful for so much! We know He was letting us know it was time to find this out before Kevin got any sicker. I have felt all along of His protection. I know it doesn’t seem like protection when you see the pain and all he has been through in the past 3 weeks but really he is being protected:)
Saturday September 10, 2011
Just been watching videos and resting yesterday and today. And the only call on the home phone was yesterday and of course I answer every call and it was a telemarketer:( He sees the surgeon again Monday afternoon and we are hoping to get the results of his biopsy sometime Monday too. Cole brought home Kevin’s laptop and textbooks Friday so we can start to develop a plan on make up work….when he is ready. I was so excited to see him get up and just go open the fridge and grab a Gatorade that I exclaimed, “look at you being normal!” Then realized I slipped into accidentally aggravating him:)
Thursday September 8, 2011 1:40 pm
The doctor who performed the biopsy stepped out and told us that all went well. She was able to go in where she wanted and the entire procedure was 30 minutes. We are with him while he sleeps in and out and has to stay for at least 4 hours. My phone is not getting great service which is a first for me as a Verizon person but keiths AT&T is so of course I took over his to post this but need to get it back to him so he can get back to more serious matters…words with friends! Thank you for praying. We will know results as early as tomorrow and as late as Monday.
Thursday September 8, 2011
He is having the biopsy today. The nurse called us back yesterday after we handled up on his headache and she wasn’t warm and fuzzy and understanding but said try not to give him anything else. Even when I told her she just didn’t know how horrible it was.
We are strengthened by each of your prayers and emails, texts, calls, visits and comments. We know He is protecting Kevin and has him in His perfect will. He chose to just reach down while Kevin was sitting in church and touch him starting this entire process. We know He was like…it’s time because we were thinking how else would we have ever known:) We see His hand working and have peace and strength that does surpass all understanding.
Wednesday September 7, 2011
He had a horrible night. He had little bit of a headache yesterday after the trip downtown but since he is having a biopsy tomorrow he cannot take any ibuprofen. They said and the paper said only Tylenol. Well he was already taken off that so I gave him a Dr. Pepper and a smile:) Unfortunately after midnight his headache had intensified so much. I was already trying to massage it away. So I woke up Keith and asked should I give Tylenol. The paper says Tylenol. He said yes. Then I woke him again cause all we had was extra strength Tylenol. 500 mg a pill. Kevin was taking 3 ibuprofen at 200mg a pill so I couldn’t figure out if there was a difference being so tired but Keith said give him 2. For the next 2 1/2 hours I was up and down with him trying to massage that headache away and praying and turning off any light he could see then he said the lights on the fridge were even too much so since I couldn’t find tape anywhere in the dark I stumbled on a sticky notepad and sticky noted the blue lights on the fridge, microwave and oven! Finally at 2:30 am after he begged for ibuprofen I woke up Keith! He said go ahead and give it to him. So that stuff finally worked or we have totally overdosed our kid with liver problems! (and that is a “we” we not an “I” we wether Keith remembers any of it or not!) I do know he needed codeine at the hospital yesterday and as much as we didn’t want to give it did anyway so I am calling it a kickback headache from codeine. And I get to call TCH today and see if we need to postpone the biopsy because of the meds he took. And hopefully they won’t like think we are absolute idiots and cannot follow directions. Then I have old hop-a-long Caleigh who fell out of bed (she has been sleeping in tiffanys room and not much sleeping is going on cause she comes out every morning with a new treasure!) and was hobbling along (which she has been having all sorts of clumsy falls and bumps and really dramatizing them lately even frequenting the school nurse…I want to say look I’m on to you, your fine, but at some point in the day something “distracts” her and she gets back to normal.) So this morning she hobbled and missed her bus which on any other day would have been fine had Keith’s car decided not to quit running and block my mini in (loaner mini at that mine is in the shop)! He was late for work and meetings and we were going to push the dinosaur expedition out of the driveway but he found some tool in the garage and clamped it on the battery connector that didn’t look like it was having a good life anymore and since it started just drove it to work like that and said it never sounded better! All this and Kevin is sleeping soundly…and I am so thankful!
Tuesday September 6, 2011 2:15pm
Dr. Mehta explained to us very clearly that Kevin has indications from his lab work that he could have autoimmune hepatitis. They can positively identify autoimmune hepatitis with a liver biopsy. He has one scheduled for this Thursday morning. She will read the results as early as Friday but it could be Monday. He needed blood drawn for the biopsy so we just did that before leaving the hospital. It is not 100% sure yet but IF the biopsy results prove that it is he will be treated with 2 meds first a steroid and then Imuran which is a low dose chemotherapy drug. He will take them for life. Stuff got fuzzy here but I figured we have time on the treatment front to ask more questions because he just may not have it or need the treatment. Cross that bridge when we need to. He will still be able to lead a very normal life but will be closely monitored with labs if he needs to go on the meds. She explained everything very thoroughly including what he is experiencing now which is active inflamation>;;>;;>;;next comes attacking of the liver>;;>;;>;;then scarring>;;>;;>;;then cirrhosis. (the biopsy will show how much of the previous mentioned steps he has experienced) She then stepped out to allow us to take it in then she came back in to answer questions.
Questions we asked:
~Autoimmune what?
Autoimmune hepatitis.
~What was the chemo drug?
She even spelled out the generic of Imuran which is azathioprine
~Kevin weighed 161 pounds. He is also 5’9.8″ 🙂 Kevin asked since all he has been doing is sitting around eating you think he’d gain weight?
She said after surgery your body uses alot of calories to heal. Healing takes priority. She did point out that IF his bilirubin numbers are up after today’s labs then that can cause weight loss because of poor absorption. But the lab results in the past have been normal for that level.
~We asked her to look at the color of his belly. It has been looking yellow to us. She said it did not look yellow to her that when she first walked in she would say he is bronze:)
~Keith said not to ask this next one but I did. I asked her should we test our other 3 kids’ liver enzymes? She said no:) She said she would understand if we did but she does not encourage it.
~Of course we asked how did he get it IF this is it?
She replied that no one knows. Autoimmune diseases(?if that was the word?) are still being studied and it is not anything we did wrong or something he ate…they just know that for some reason your immune system starts turning on you and attacks different organs/glands. She named several that are familiar sounding but I don’t know how to spell:). (like lupus and hashimotos)
She reminded us we are not sure but if so it will be detected very early. And they will know more on how far its progressed after the biopsy.
He will not be able to take any medications until 2 weeks after the biopsy like Motrin and stuff like that. He did need codeine this morning after the trip there and elevator ride to the 11th floor but we did not know at that time a biopsy was so near in his future:)
~We did ask how would we have known this again IF it is autoimmune hepatitis?
She said his liver would have gotten very sick, he probably would be yellow… And that most people who come see them are caught by something else happening. So Keith chimed in saying…”So the torsion was good!” We laughed because that would be the only good thing out of that awful painful experience!
~We also asked what IF it is not autoimmune hepatitis and she said first she would expect today’s labs to be very good at all normal levels:) and basically we will talk after the biopsy results are in. There would be a lot more questions.
That’s all I can think of for now! While writing this they already called verifying our insurance for Thursday’s biopsy. I’m feeling a nap:)
Tuesday September 6, 2011
Kevin has had a pretty good long weekend. Fever free and yesterday no pain meds. This morning we head to TCH for his appointment with GI Liver doctors at 11:30. Thank you for your prayers!
Friday September 2, 2011
It was visitor day:) Kevin got such fun stuff too! Get well popcorn, Starbucks white hot chocolate, a beautiful orchid that only requires 3 ice cubes a week to keep alive (can we do it?!) and RJ Goodies treats:) He is still managing the pain but so far today no fever! That is a first since all this started! His Liver doctor phoned yesterday and said she hopes all the test results will be in so Tuesday she can put the picture together for us. So we are looking forward to a restful weekend and no doctor visits or blood draws. He is totally bummed to not be marching in tomorrow night’s first home game. Please pray that those looking at his liver blood tests will have as one friend prayed “super Nancy Drew eyes!” and that He would give them wisdom and discernment and clarity of thought.
Thursday September 1, 2011
Kevin had a good check up with the surgeon. He said Kevin is getting better just not fantastic. He wants to see him in 10 days and will not release him to return to school until then and that is pending anything the GI/Liver doctor says next week. He wants him to start an antibiotic but that too is pending being filled based on GI/Liver doctor approval. It seemed like everyone in their knew Kevin or of him. The doctor, who has performed robotics kidney surgery and whose father in law use to head TCH for 35 years, told us that of the thousands of times he has performed this surgery he has never seen anything like what happened to Kevin. So as I told Kevin he is much better off than he was one week ago! So definitely a praise!
Wednesday August 31, 2011
Last night I fell asleep after 12:30 and at 1:00am he was crying standing over me and at an 8! He said he was throwing pillows at me and hollering my name:( so I gave him 2 codeine poor guy! Had to get up by himself! I switched my head closer to him so he could bang on me with the back scratcher, and I told him to ring that bell! I grew up with 7 siblings and can sleep through a train wreck! Keith threatened to fire me from my night job! Dr. Popes nurse called and said that his liver enzymes were still elevated but a little lower than when he was in the hospital. They are faxing them to TCH for our appointment Tuesday. He has had horrible hiccups today and we googled ways to get rid of them and tried at least 13 before he fell asleep with a hiccup headache! His school principal also called to check on “her boy:)” We are both having pretty wild dreams:) But getting rest.
Tuesday August 30, 2011 11:30pm

He said I could post this:) Table for eating, playing on the laptop, and building hour long Lego star wars projects to keep his mind off the pain. He is surrounded by the basics: broom for a cane, radio to listen to KSBJ, zen garden from Aunt She-o and Uncle Ro to rake rocks but Cole has taken over:) and bamboo plant from Pastor and our church. Today was a much better day and he was able to stay put and get a lot of rest. After yesterday’s terrible horrible no good very bad day we needed it:)
Monday August 29, 2011 5:15
Today was off to a super rough start! We had a doctor’s appointment to get to and his pain was a 7 with codeine at wake up. We used the office chair to get him to the door then once at the office they had a wheelchair that he basically used as a walker since he would have had to squeeze into it but one does not squeeze after such surgery. We survived it all. They drew more blood and Dr. Pope replied when I commented on his hygiene that as long as you can breathe in the room and he is not reeking it’s good. Once you cannot then take him out back and hose him off! We needed the laugh:) tiff was able to help so much before heading back to school. Such good timing. On the way home I was driving so slowly and carefully and Kevin noticed a firetruck pass us not in an emergency and said they were all staring at me:) I said it’s either because I’m so good looking or they were shocked to see someone so young driving so slow! Either way I am complimented! I said so what do they want: me to hold up a sign saying slow driver son recovering from torsion on board! After the morning we had it’s a wonder an ambulance didn’t come get us both! I was truly thinking why are we home! But we got good information for pain and fever management and he is back settled down now and the best part we both napped:) The surgeon finally contacted us and had been following him through the TCH drs and we see him Thursday and one week from tomorrow we are back down at the TCH clinic to see the GI and hopefully get the scoop on what’s up with his liver!
Sunday August 28, 2011 4:00
I had an update written and it went away. And since then he has just had a good day in some ways as well as a bad day in others. Still managing pain and fever. We will have several appointments over the next week. But we did get home around 5 pm last night! I think he is loving it!? He asked for a make shift table to set up around him to use like the one at the hospital. So he can now use the lap top…build legos that Keith got for him and eat. We are set:) I am so thankful for the many prayers, comments, emails, texts and good information. Not to mention all the food and treats sent our way. We are blessed. I don’t have nearly as much down time and the stuff I can write down are facts like blood pressure temperature and when I gave meds.
Saturday August 27, 2011 1:15
He gets to go home!! Dr. Lo just came in and said that the GI and urologist agreed that he could go home. They want us to see Dr. Pope Monday to draw more labs and make a follow up appointment with the GI dr for one week. He is a little overwhelmed with the news but I reminded him that when Paw Paw had his liver transplant I was the one who went up intending to be hospital watch and they sent him home on my watch;) I have previous experience:) I think he is just concerned home means back to work! But I assured him he will still be a patient just at home. For now we are waiting for discharge and they said before dinner:) We will see.
Saturday August 27, 2011 10:40
Ok…I hit send real quick on the paragraph below because the team of doctors came in.
~his hematocrit levels were just a bit low
~one reason he was kept overnight was the blood was not clotting and now those numbers are better
~his liver enzyme levels are a bit higher than yesterday but not much
~ruled out all the hepatitis A B C as mentioned. Ruled out Epstein-Barr Virus aka type of mono but showed he has had it before. We never knew that and they said it is very common and people have the non full blown version all the time without knowing.
~want a urologist to check him today
~as mentioned to us yesterday they may possibly just transfer him to that team of GI doctors that visited us yesterday. And with that if urologist and GI agree he can go home and be handled as an outpatient.
~regarding his migraines they want him to be taking Motrin and not Excedrin Migraine as we’ve treated before at home because Excedrin has acetaminophen (Tylenol) and is processed in the liver. Motrin is processed through the kidney. I stopped them here and asked is that on the label?! Who remembers this in 3 days:) I will now cause I’m writing it down.
~their goal is (1)to get his liver enzymes stable and (2)for him to have better pain control. So far the last morphine was 10:30 last night. Only Tylenol at 9 this morning for migraine so far. I know I know he is not supposed to have it now but we didn’t know that then:) and (3)to complete the work up the GI doctors ordered or be treated as outpatient.
~reminded Kevin the procedure he had is one of the most painful thing a body can go through and not to be afraid to ask for meds. (no tears that time)
I called Keith to tell him all of the above hence the bullet style of writing. My ah ha moment. When the urologist saw Kevin the next morning after surgery and remembered the liver enzymes elevated it was like ok…because of that (which could be just nothing he just happened to have torsion when his liver was doing it’s everyday job) he is having extra bleeding which causes swelling which causes pain. So even though I mentioned they were 2 separate things the one actually caused the other post surgically speaking …maybe. All I know is even though I’m not at Dr. Popes office for a normal pediatric visit I can hear him saying when sometimes I ask him why about a particular issue he says it’s just dumb luck! Another thing if I can remember the wording specifically he says is…if you are hearing hoofs then don’t look for zebras! Keith reminded me that the urologist that did the surgery said if something is going on with the liver you can bleed more. Which is a clotting issue. When he saw the swelling and the bleeding (and bruising) it triggered to him(surgeon urologist) that the liver enzymes were elevated and was the cause of this. If liver enzymes weren’t elevated he would have had a much more normal recovery! Got it!!! I get it! She gets it;) So that all led us to TCH. I am slow at comprehending medical terms but getting there:)
Saturday August 27, 2011 9:00
Kevin slept for 5 hours last night! The slew of blood draws came at 7 am. (He did awaken with a migraine which is a preexisting condition.) Dr. Rose came in and talked a little more to me about his ultrasound results mentioning the spleen was enlarged which I remembered and the liver was. Keith and I both missed that yesterday and were wondering so it was good to get clarification. It was just me so I am asking how can you tell that from an ultrasound? She said it’s just like a wound on your arm when it’s inflamed and sore. We can see on the ultrasound that his liver and spleen are inflamed. That made little tears trickle and Kevin was asleep so she just sat and re explained it because the first time around I was too busy focusing on not crying that I didn’t really listen. So I asked her if she could just retell that part about the liver. (I couldn’t remember the word “inflamed” just like on ER night i couldn’t remember “torsion.”) So the sweet dr–if your allowed to refer to them that way:) sat while Kevin was sleeping and let me hear her again. And I joke about Caleigh being clueless! Then another doctor followed close behind and checked him and in passing mentioned that torsion is one of the most painful things a body can experience and yep you think an inflamed liver brought tears she brought me a paper towel:) But it’s all good. They both reassured me that the body works like this. We may never have known his body is doing just what it’s supposed to be doing when fighting an infection which is what it’s doing when things are inflamed (my reasoning) so 2 separate things are going on and one because of the other is now being thoroughly examined in case their is something that like early detection can help. Really I am putting my thoughts here to so I can keep things settled in my head. I should turn it over to “bullet point Keith” but when he is around for the next dr visits I will have him recap and I will just type:)
Friday August 26, 2011 11:45
They call him “the tan one.” Kevin already has a nick name on the floor Keith told me and it’s the tan man! We have been asked by almost everyone who walks in… So this is his skin color? He has always been my tanned one. Beautiful squishy soft skin. He is just so touchable! ( I actually checked him into doerre one day while he was there and for some reason reached over and touched his arm and instead of saying good bye get to class I said what I was thinking out loud– “squishy squishy!” I couldn’t even believe it myself but hey… What’s done is done!) I am staying the night tonight. Keith pulled a double header so will hop up in the morning. He has had a much better day. His pain levels have been 5-2 and had a headache that reached a 5 when the pain was at it’s lowest. I still as the mom doc think he just doesn’t look good. He has that look in his eyes that just says he doesn’t feel good. It is so good to see him eating and drinking more and the nurse was “psyched” when she saw him actually playing a video game. Yesterday was a very bad day. The last time the nurse popped in she gave us a heads up that the liver doctors have ordered a slew of labs for tomorrow then repeated a slew. I said more than 12? And she pulled out her paper and we looked at them and yes…the list was more than 12. Don’t even know if I’m spelling slew correctly! Keith called once he made it home with news that Kevin’s surgeon left several messages on our machine checking on him. He knew we were being transferred quickly so just wanted to check. That just made me happy:) I was having a bit of tears at dinner with Keith in the cafeteria just taking it all in. And I know my Pastor came and had us rolling with laughter and praying and am trusting Philipians 4:4-6 that he shared. But I loved that surgeon. And yesterday we both thought we don’t even know his name. So we had the nurse find it in the paper work because we think he wanted to follow up with Kevin in a week at least he said he did. I kind of felt lost and out of a loop that we weren’t really in long enough to be in the loop! So it was good to know he hadn’t forgotten Kevin:) Just so good to know:)
Friday, August 26, 2011 4:30 PM
Two liver specialists just left and updated us with the following:
~he does not have hepatitis A, B or C. However his HepB vaccine is needing a boost. There were no antibodies found in his blood.
~there still trying to figure out why the spleen is enlarged.
~examining the blood work and will do more tests tomorrow. They are looking for an infection of some type or an autoimmune type of infection because something is fighting the liver right now.
~there is a chance he will be released tomorrow it just depends on the results.
~whatever is fighting the liver could also be making the spleen enlarged.
~he has a fever of 101.1
Friday August 26, 2011 2:00PM
So far this morning my plan was a happy one. Don’t even try to park just do the valet! $11 to park in the garage $11 for valet…you choose valet. Until it’s full! And every garage around the place was too! I think I know why St. Luke’s heart hospital does so well…wanting to get to your child and it taking an hour puts some stress on your body!! But Keith will forever be my “on star!” I just dial him up and he always gets me in the right direction and sounds so calm in the entire process:) I just knew the team of doctors was meeting by 10 and I would miss it all. He was supposed to have his ultrasound at 8:30 but it was delayed until after 12. So then were the team of doctors delayed as well. He has had a pretty good day pain wise. So far he has not gotten above a 5. He was able to get a record amount of sleep–4 hours. Such a praise! He has had lots of blood drawn and we are just waiting. Happily I might add eating cookies from cookie bouquet sweet people had delivered:) his left arm was really hurting him and he kept it still most of yesterday and was told today he needed to move it around. Aka–hit the nurses station and pick out a ps2 game. So I grabbed him up Lego star wars and he is following the doctors orders and moving the hand and arm. The GI dr was in assessing him and will return since the ultrasound tech came for him. Kevin was told at 4am not to eat or drink until after the ultrasound so when he was finished there he came back to the lunch he ordered. Cheese pizza, fruit, mashed potatoes, corn and strawberry milk. He was given morphine for the pain not long ago and is gaming but I suspect he will be snoozing very soon.
Thursday August 25, 2011
We have had a crazy 24 hours. Last night while at church just sitting in the pew Kevin leaned over to me and said that his right side was hurting. I sent him out to walk it off but it became clear on the ride home that the pain had intensified. It wasn’t a matter of not taking him in but rather let’s get the kids home to dad and find out where he thinks we should head. So guessing it was appendicitis territory he said go to Tomball hospital instead of one of those quick clinics which we frequent alot. He ended up needing a procedure done in emergency surgery and all seemed fine. The surgeon even said if it weren’t midnight we’d send him home. So Keith stayed the night with him and I went home to get Cole and Caleigh out the door for school. I really was tired and practically nauseous so I called Keith and told him he gets to wait on the tag team since I knew I needed a tiny bit of sleep. Kevin had been in a lot of pain and I found out that when I joke and say I don’t do pain…I really don’t do pain! I can’t even watch someone else not doing pain. English teacher was the perfect profession for me:) I maybe got 30 minutes sleep when Keith called saying that they discovered “by chance” from his labs that his liver enzymes were elevated and after checking with the doctors at Tomball they wanted him transferred by ambulance to Texas Children’s hospital. I ended up riding in the transfer ambulance with him and we got checked in around 4 this afternoon. Keith followed behind. We have seen different doctors and they have ordered labs and will test his liver function. It could just be his enzymes were high and it was randomly found during his stay at Tomball or it could be something else. The team of doctors will meet in the morning, Friday, and then will get with us about the results. Keith stayed the night again but funny thing about riding to a hospital in an ambulance…you don’t really know where the car is parked no matter how good of directions he gave us! So me and Cole and Caleigh wandered in the halls and elevators that after hours let you shut the doors and push buttons but took you no where for almost an hour! I called, texted and emailed Keith time and time again to help! He had fallen asleep! Im thinking he must have sneaked pain meds! He had to walk to us then get us to where he parked. They probably have an app for that. I didn’t want Keith to have to leave Kevin’s side because of the action that happens in that room and sure enough the labs were being drawn and a pediatrician was attending to Kevin by the time he got back up to him. But it’s all good. I have heard what good hands he will be in at TCH but know the hands he is in that matters so much more. I appreciate all your thoughts and prayers and will probably post news here as we get updates. Hopefully like one of the doctors mentioned–once his pain is handled from the Tomball procedure most of the liver tests can be done out of the hospital. He went from pain that was off the charts to tonight when I left 3-5 but With medication. And with a temp of 100. Also as much as I want to stay I told Keith somehow I keep accidentally aggravating him! I am just over doing the mom thing on my 14 year old boy and it ain’t working! At least I recognize my faults but just can’t help myself! I even spoke with Cole about it and he said tiff would eat it up just not he or Kevin. So I will take the line of advice from Andy in the toy story movie and “back off.” So Keith took the night shift again and Kevin gets a break from me! Oh, but I’ll be back:) And I might even find time to pick up a cookie bouquet!!!
August 25, 2011 2:30am
I left Keith and Kevin all tucked in at the hospital. So what started out with Kevin whispering to me on the church pew that his right side was hurting ended up requiring emergency surgery at Tomball hospital. I cannot tell you how hard it was seeing Kevin in so much pain and being able to do nothing. Nothing but pray that is. One er nurse said the pain meds she was giving him was 10 times that of morphine and it took the pain away for a tiny bit but by the time she came back to check on him he was back at a 9. And in no time what I thought was going to be an ultrasound was escalated to surgery and of course understandably so. With what he had time was not on his side.
What I want to tell is that when I was leaned over that bed wanting to find time to pray out loud over him and seeing the pain and thinking wow…really…I’m going to pray… Pain killer is not taking an edge off of it. But even though I was interrupted here and there I did pray and had already asked him if I could ask others too and when I was talking with him before I left I told him I just couldn’t believe the pain he was in and that the meds were not helping and he looked at me and said, “nothing helped the pain until after you prayed.” Such a precious testimony and to think I almost talked myself out of praying! And I know we were praying in one accord because I saw the texts later of y’all responding and just know they were answered tonight:)
He is our shepherd and our MIT group prayed that this past Monday morning and I have to say I was calling on the shepherd again:)
It is not such a specific medical update but I wanted to wind down before getting some sleep and share how good God is! Thank you for praying! He should come home tomorrow. Beth
August 24, 2011 Wednesday after 930pm
Kevin was admitted to Tomball Hospital ER and was immediately taken back for emergency surgery for testicular torsion.


So sorry to hear of Kevin’s problem, but the Lord is in control and we pray that the doctors will get wisdom to know what and how to treat Kevin. Keep looking up!! We love you and will be praying all will be better real soon. God bless , Bro.Rudy & Helen
Hey Beth. Just wanted to drop you a note and say we’re praying. Hope things are looking up soon. ❤
Thank you for the update, Beth. Just want you all to know we are praying.
Love you!
Gary, Ruth, and boys
praying, praying, praying. May God continue to give him relief from the pain….
Dear Keith & Beth,
I’m just now learning all about Kevin and please know that we are keeping you all in our prayers. I know this has been difficult for everyone. We certainly understand how hard it is being in the hospital and watching your child struggle. Praying he feels better soon!!
Love to you all,
Natalie & Ken Furman
Praying for all of you, Beth. As your one friend said, praying for “super Nancy Drew eyes,” especially as they perform and analyze the liver biopsy. Praying for God’s miraculous healing!
Finally got to read all the updates…..I am praying for him, Beth…..
Beth,
You have been on my mind for several days. I have thought of calling you but time seems to get away from me. I woke up and was wide awake…decided to check up on your via FB. I am so sad and my heart is heavy for Kevin, you, Keith…our family. I know God was wanting me to start praying. I am praying for the precious healing blood of Jesus to cover Kevin inside and out…from the top of his head to the bottom of his feet. Comfort and strength for you and Keith. Wisdom and discernment for his doctors and anyone who has any decision making over Kevin. Let me know if you need anything.
Love and hugs dear friends,
Tracy
give me the name of that nurse who was not warm and fuzzy and i’ll have some words for her.
Good nurses make all the difference…tell him to hang in there..this too shall pass… 🙂
So glad you are all able to rest….it feels so good to see them normal after being that sick…. 🙂
Beth ~ It is just like YOU to encourage US in your blog posts! What a blessing to read your post this morning (Tues. 9/13) of your interactions with Kevin, Caleigh, Cole and Tiffany! I’ll pray with Caleigh and seek that it be “bumped down to three years”! Your children are embodying the love of Christ that you and Keith have always demonstrated. Praying for daily peace and strength for all of you. You are all a treasure! ❤
Jim and I are praying for Kevin. For you, Keith, Cole and Tiffany. Know I love you and yours.